
Full Text
Psychological Health and Overweight and Obesity Among High Stressed Work Environments
Pouran D Faghri 1*, Christina Mignano2, Tania B Huedo-Medina3, Martin Cherniack4
1 Professor of Health Promotion Sciences, Department of Allied Health Sciences and Professor of Community Medicine and Health Care, School of Medicine, University of Connecticut, USA2Graduate Research Assistant at the Center for the Promotion of Health in the New England Workplace, USA
3Assistant Professor of Biostatistics, University of Connecticut, USA
4Professor of Medicine, School of Medicine, University of Connecticut, USA
*Corresponding author: Pouran D Faghri, Professor of Health Promotion Sciences, Department of Allied Health Sciences and Professor of Community Medicine and Health Care, School of Medicine, University of Connecticut, USA, Tel: 860-486-0018; Fax: 860-486-5375; E-mail: Pouran.faghri@uconn.edu
Abstract
Correctional employees are recognized to underreport stress and stress symptoms and are known to have a culture that discourages appearing “weak” and seeking psychiatric help. This study assesses underreporting of stress and emotions. Additionally, it evaluates the relationships between stress and emotions on health behaviors. Correctional employees (n=317) completed physical assessments to measure body mass index (BMI), and surveys to assess perceived stress, emotions, and health behavior (diet, exercise, and sleep quality). Stress and emotion survey items were evaluated for under-reporting via skewness, kurtosis, and visual assessment of histograms. Structural equation modeling evaluated relationships between stress/emotion and health behaviors. Responses to stress and negatively worded emotions were non-normally distributed whereas responses to positively-worded emotions were normally distributed. Emotion predicted diet, exercise, and sleep quality whereas stress predicted only sleep quality. As stress was a poor predictor of health behaviors and responses to stress and negatively worded emotions were non-normally distributed it may suggests correctional employees are under-reporting stress and negative emotions.
Keywords
Stress; Emotion; Health behavior; Correctional employees; Structural equation modeling
Introduction
Almost 69% of U.S. adults are considered overweight or obese [1]. Obesity predicts increased risks of morbidity and mortality [2-5] and elevated medical costs [6]. Health behaviors have been identified as key determinants of bodyweight (e.g. diet and exercise) [5,7-9]. Stress and poor psychological health such as negative emotions, depression, and anxiety may also be risk factors for obesity by promoting poor health behaviors. Emotional characteristics have been related to both body weight and health behaviors. Multiple studies also suggest that negative emotions (e.g. negative mood) may negatively affect eating patterns [10-12]. In addition, elevated stress is related to poor sleep quality and duration [13]. Furthermore, poor sleep quality has been related to psychosocial health including negative mood state, depression [14], anger, hostility, and aggression [15-17].
Work stress also has been associated with unhealthy lifestyle behaviors such as poor dietary practices [18] and low levels of physical activity [19,20], thus contributing to weight gain, abdominal obesity [21,22], and metabolic syndrome [23]. Chronic work stress has serious adverse implications on employee health and well-being [24-27] and has been significantly associated with rises in plasma cortisol level, coronary heart disease [25], high blood pressure, high blood sugar [28], and psychological issues such as anxiety and depression [29-32]. Furthermore, occupations characterized with high job strain (high work demands and low decision control) have been associated with increased risk of depressive symptoms, and those characterized with high job strain coupled with low social support are associated with psychological distress, job dissatisfaction, and negative emotions [31,33]. Additionally, chronic psychological distress and negative work experiences may negatively impact an individual’s personality, resulting in a persistently negative outlook [34].
Law enforcement personnel are an occupational group with higher health risks compared to working adults in other occupations [35]. Correctional employees have elevated rates of overweight and obesity when compared to national U.S. averages (86.6% and 55.8%, respectively), vs. (69% and 32%, respectively) [36]. Likewise, correctional employees report poor health behaviors including poor diet, snacking on low nutrient foods [37], low physical activity, sedentary behaviors, and poor sleep patterns [29]. Correctional employees are also recognized for high rates of occupational stress and depression [34]. Unfortunately, the poor psychological health profiles of correctional employees appear to perpetuate poor health behaviors and ultimately contribute to overweight/obesity. For example, in a focus group study correctional employees reported that job related stress was a major contributor to poor dietary practices [29].
The contributing effect of work stress on health in correctional employees rests on the presence of multiple sources of daily stress including the hierarchical structure, work environment (poor staff to inmate ratios, required overtime, and shift work), contact with incarcerated inmates, low social support, negative public image, work overload, role ambiguity, low skill discretion, job-demands-control imbalance and effort-to-reward imbalance [34,37,38-42]. The constant sense of personal endangerment effects correctional employees health behavior [24,43]. Correctional work is associated with high levels of adverse emotions and elevated prevalence of mental health issues [44] that include perception of a short life expectancy, high suicide rates [45], and high rates of depression [46,47].
The term emotional labor describes the management or modification of emotions when one’s occupation requires expression of certain feelings while concealing other emotions [48.49] This may take the form of faking, enhancing, or suppressing certain expression to achieve the desired emotional anterior [50]. Emotional labor has been associated with adverse psychosocial states and measures, including burnout [51,52], job stress and self-alienation [49,52], depression, cynicism, role alienation [53], emotional numbness [54], and job tensions [51,55]. When emotional labor results in a conflict between required emotions and true emotions, the result has been termed as ‘emotional dissonance’. The larger the gap between required emotions and true emotions, the more likely an employee is to experience stress, job burnout, and psychological separation from one’s self [56,57].
Although law enforcement, including work in corrections, is noted to be a high-stress occupation, law enforcement personnel commonly under-report stress levels and stress symptoms [35,58-60]. This reported phenomenon provides a basis for testing the emotional labor construct and hypothesis [35,60]. The resulting emotional detachment from both self and other is associated with poor family relationships (e.g. marital disruption and divorce) [35,61,62] and has been observed in police officers [63], military personnel [64] and correctional officers [24,65]. These occupations all require the display of a detached attitude during emotionally challenging situations (e.g. conflict, aggression, manipulation) while refraining from displaying actual feelings [63]. For example, military personnel are characterized as “macho” and being immune to the challenges and traumas that are “just part of the job”. Individuals who do not keep up this “macho” description are identified as “lacking in moral fiber”. Seeking psychiatric help is viewed with a negative stigma and therefore, military members generally do not seek such help for fear of appearing weak [64]. Furthermore, exposure to life-threatening events, a common experience for law enforcement personnel, can also result in feelings of detachment, emotional numbness, and interfere with an individual’s ability to function as they used to [66].
Correctional officers need to display various emotional fronts in specific situations (e.g. friendly/supporting, anger/toughness, and/or concealing distress and weakness) [67]. In corrections work, expression of emotions and feelings has been characterized as an occupational hazard and low-status “women’s work” [68]. Although confronted with many stressful situations, correctional officers have are limited in coping by the primacy of security and procedures. Therefore, correctional employees have few tools to decompress when faced with stressful situations and must internally cope with intense and negative emotions while requiring to appear calm and emotionally detached [69]. Among correctional officers, this emotional dissonance has been noted as a source of stress [63]. Denial of occupational stress and its consequences have been cited as sources of feelings of helplessness and alienation [70].
Due to emotional detachment, correctional officers may not realize detrimental consequences (e.g. negative behavioral patterns and emotional instability) traumatic events. Alarmingly, this inability to express negative emotions and inhibition of emotions are strong predictors of poor physical health and illness (e.g. high blood pressure & cancer) [50,63].
Overall, occupational stress in law enforcement personnel is seen as a problem for employers by adversely affecting the psychological, emotional, and behavioral health of employees [43,71-72]. Emotional dissonance has many detrimental effects on employee health including increased stress. Therefore, both emotional dissonance and the acute and chronic stressors of these high stress occupations must be effectively understood and addressed. Many studies note these populations to underreport stress and stress related symptoms [24,31,60]. Therefore, addressing stress and emotions within corrections may enhance healthpromoting efforts. Hence, the purpose of this study was to examine the prevalence of reported stress, negatively worded emotions (e.g. feeling blue or worthless), and positively-worded emotions (e.g. feeling calm or happy) amongst a group of correctional employees and compare responses to assess for under-reporting and possible evidence of emotional labor and emotional dissonance. Further, researchers examined if reported stress and overall emotion had an effect on reported health behaviors (diet, exercise, and sleep quality). Drawing attention to emotional labor and dissonance experienced by correctional employees and the effects of employee stress and emotions on health behaviors will bring better awareness to understanding the determinants of health among employees.
Materials and Methods
Design
This was a cross-sectional observational study.
Participants
Data collection was conducted at two correctional institutions in the same Northeastern state. Prior to data collection, members of the research team met with Wardens and Union representatives on multiple occasions to discuss best practices and procedures for encouraging participation. All employees of these facilities were invited for voluntary participation. Volunteers were recruited with flyers posted in the facilities and roll call announcements conducted by research staff and supervisory lieutenants. After being informed about study requirements and having time to discuss questions with research staff, participants signed a consent form approved by the Institutional Review Board. Health Risk Assessment (HRA) survey and physical assessments were conducted in secure locations within each facility. Participants were financially compensated for each portion of the assessment they participated in (survey and physical assessment) for a maximum of $50. Research staff spent approximately two months at each site. Administration was fully informed of all study procedures and gave their support and encouragement to employees for participation. Three hundred and seventeen employees completed the Health Risk Assessment (HRA) and the physical assessment.
Measurements
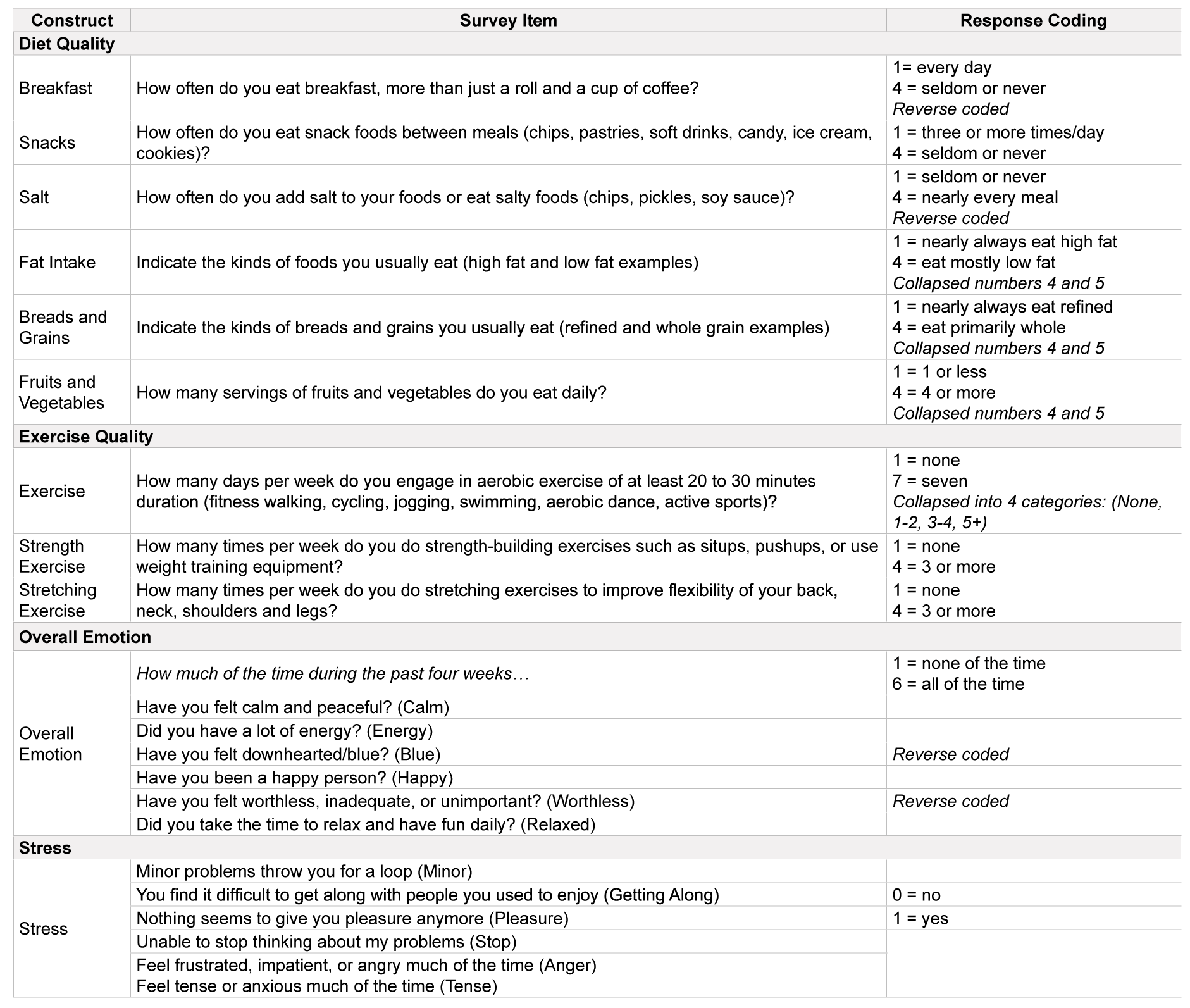
Data from the Health Risk Assessment (HRA) survey and a physical assessment were utilized (variables further discussed below). The HRA tool is commonly used in workplace wellness programs and has been certified by the National Committee for Quality Assurance [73]. All survey items used are listed in Table 1
Physical assessment: Trained research staff measured height and weight with a calibrated Seca 700 physician balance beam scale, measuring weight to the nearest 0.1 kilogram and height to the nearest millimeter. Height and weight measures were used to calculate body mass index (BMI) (weight in kilograms divided by height in meters squared) and classified based on Centers for Disease Control and Prevention (CDC) recommendations [74,75].
Health risk assessment: This study used the Wellsource® HRA- The Personal Wellness Profile™, a survey utilizing 39 questions in Likert scale form to assess multiple dimensions of participant’s self-reported health. For this study, responses to nutrition, physical activity, stress, and emotions were assessed. Survey items were used to create an overall latent variable score for each health behavior, stress, and overall emotion.
Health behaviors: Th ree health behaviors were assessed based on selfreported answers to HRA questions (diet, exercise, and sleep quality).
Diet quality score was calculated from 6 survey items assessing how often the participant ate from each food groupparentheses (snacks, high salt foods whole grains), and frequency of eating breakfast. Because survey roots used either 4- or 5-point Likert scale, all questions were normalized to a 4-point scale prior to analysis. Answers ranged from (1) ‘almost never eat the healthier options’ to (4) ‘almost always eat the healthier options’. Higher latent diet quality scores represent better overall diet.

Exercise quality score was based on 3 survey items assessing frequency of aerobic, strength building, and stretching exercise on 4- or 7-point Likert scales, with all items normalized to a 4-point scale. Answers ranged from (1) ‘never’ to (4) ‘three or more days/week’, with higher latent exercise quality scores indicating better exercise habits.
Sleep quality was based on a single question asking, “how often do you get 7 to 8 hours of sleep”. Answers on a 4-point Likert scale ranged from (1) ‘always’ to (4) ‘seldom or never’. This item was reverse coded so a higher latent score represented better sleep quality.
Stress
A perceived stress latent variable was created from 6 survey items with “yes” or “no” responses. Higher latent scores indicate higher stress levels.
Overall emotion
Overall emotion latent variable was created from 6 survey items. Two questions were considered negatively worded emotions (feeling blue and feeling worthless) and four were considered positively worded emotions (feeling energy, calm, happy, and relaxed). Answers were on a 6-point Likert scale and ranged from (1) ‘none of the time’ to (6) ‘all of the time’. Responses were reverse coded as needed so that a higher latent overall emotion score represented more positive overall emotion.
Data Analyses
Data from HRAs and physical assessments were transferred to Microsoft Excel and IBM SPSS™ version 21.0 software [76]. Frequencies and histograms were used to assess the prevalence of each stress signal and emotion. To assess under-reporting of stress and emotions each was evaluated for non-normality in responses. Determination of nonnormality was based on recommendations by Kim et al. who states that for samples of n>300 histograms and the absolute value of skewness and kurtosis should be utilized. An absolute skew of >2 or an absolute kurtosis >7 is a reference value to determine substantial non-normality [77]. Analyses were conducted on dependent variables with and without outliers evaluated as +3 standard deviations from the mean [78]. To create latent variable (explained below) all binary variables were coded as 0 and 1, variables on Likert scales were reverse coded if needed, and categories of variable survey items were normalized. Variables were assessed for missing values. All variables had 100% response rate besides 3 emotions questions, which had 3 missing responses. Therefore, these individuals were not used in analyses involving emotions.
Latent variables and structural equation models
Next, we used Structural Equation Modeling (SEM) [79-81] to make latent variables (stress, overall emotion, diet quality, and exercise quality) and test for relationships between these variables. Latent variable indicators are listed in Table 2. All analyses for latent variables and structural models were conducted using Mplus version 7.11 [82]. The SEM procedure used was based on recommendations by Buhi 2007 [83]. Latent constructs that could not be directly measured were represented by directly measured survey items (indicators), by assessing the shared variance between correlations/ covariances of the indicators. Measurement models used to create these latent constructs increased statistical accuracy by capturing measurement error [84]. After creating latent constructs, structural models were created to assess the relationships between the various latent constructs (stress, overall emotion, diet quality, and exercise quality) and directly reported or observed constructs (sleep quality and BMI). All measurements and structural models were assessed based on model fit to the data (how well the data fits the hypothesized relationships) as represented by the root mean square error of approximation (RMSEA), the comparative fit index (CFI), and the Tucker Lewis Index (TLI). Rejection criteria was: >0.06 for RMSEA, <0.95 for CFI, <0.90, and <&0.95 for TLI [85]. In cases of inadequate model fit, latent variables were altered by either co-varying indicators or removing non-meaningful indicators (determined by factor loads and p-value), see Table 3.
Results
Participant characteristics
Descriptive analyses indicated that a majority of corrections employees reported no/few stress signals, with the percent reporting no stress signals ranging from 81.4 - 91.2% depending on the signal. Of the 6 stress signals, percentage of participants who reported not having the signal were; 81.4%, 85.8%, 88.3%, 87.1%, 87.1%, and 91.2% (Table 4). All 6 stress signals had a large skewness (1.621 to 2.915), with 5 of the 6 survey items being above the reference value for non-normality. Please refer to the histogram in Figure 1 for the distribution of all stress signals.
The 6 responses to emotion survey items, as listed in Table 5, were coalesced from 6 responses to 3 (all or most of the time, some of the time, little or none of the time). When comparing responses to negatively worded emotions (worthless, blue) vs. positively-worded emotions (happy, calm, energetic, taking time to relax) a smaller percentage of participants reported having a negative feeling. Both negative emotions had a large skew (skewness of -0.924 to -2.060) indicating a non-normal distribution with a majority of participants reporting rarely having the negative emotion. In contrast, reporting of the 4 positive emotions was more evenly distributed with a more proportionate distribution of participants responding to having the given emotion all of the time, some of the time and little or none of the time, skewness of 0.169 to -0.556 (Figure 2). For the negatively worded emotion of feeling downhearted/blue only 2.8% of individuals reported feeling the negative emotion a majority of the time. In comparison, for the positively-worded emotion of feeling happy, 10.4% of individuals report not feeling happy a majority of the time. The implication is that responses to positively-worded questions differ from negatively worded questions, even when the construct is similar.
SEM analysis results are depicted in Table 6. These show that higher self-reported stress had no effect on diet or exercise quality, but negatively effected sleep quality (β=-0.23, p=0.001). Overall emotion directly effected all three health behaviors; diet (β =0.163, p=0.006), exercise (β=0.163, p=0.006), and sleep quality (β =0.318, p<0.001), with positive emotion resulting in better health behaviors. These results suggest that reported overall emotion might be more meaningful in predicting health behaviors than reported stress
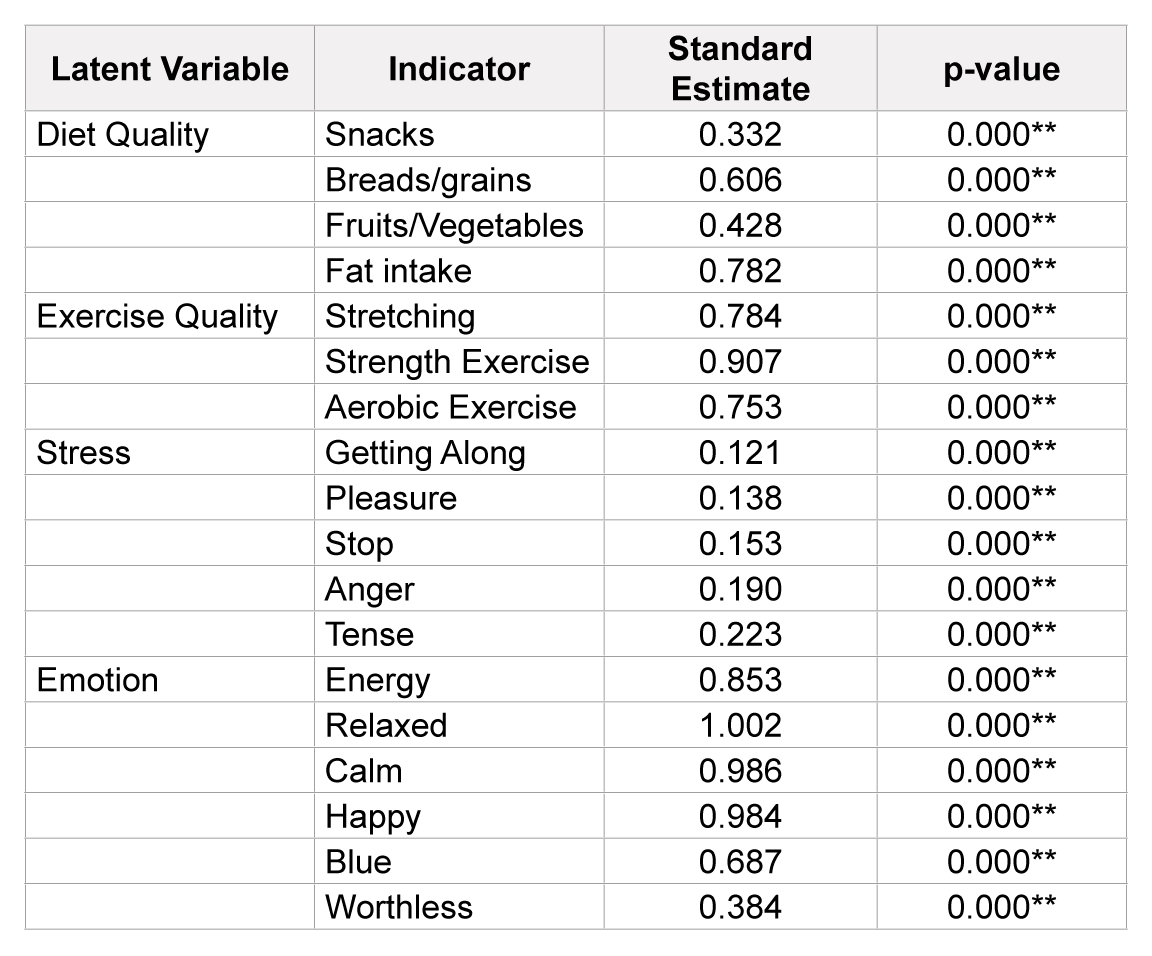
*p<0.05.; **pp<0.01; Please refer to Table 1 for more detailed description of response answers.
Table 2:Latent variables and survey item indicators
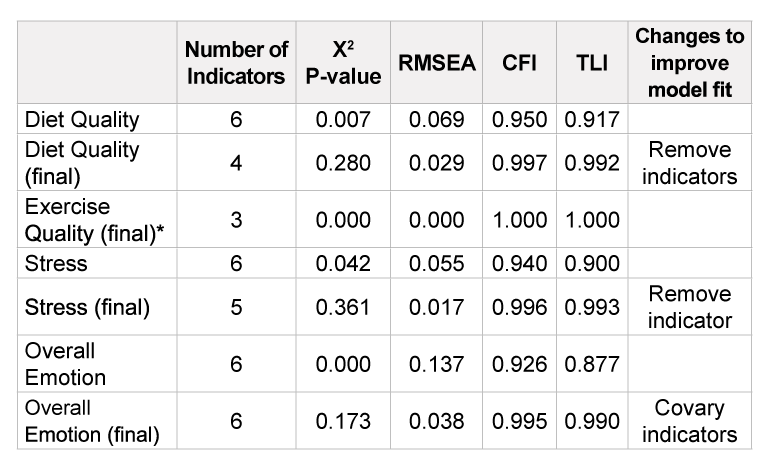
*Identified models do not have accurate model fit information and modifications were not possible
Table 3:Latent Variable Model Fit with comparison of model fit before and after improvements were made
Discussion
The use of SEM assessed if stress and/or overall emotion were predictive of health behaviors. Results suggest a relationship between emotions and health behaviors, with a more positive mood or better overall emotion related to better diet, exercise, and sleep quality. On the other hand, stress was related only to sleep quality but not diet and exercise quality. These results indicate that overall emotion was a more meaningful predictor of health behaviors than stress in this population. One inference is that rather than relying on self-reported stress alone as a predictive variable, it may be useful to assess multiple stress and emotion related variables since the suitability for a particular population cannot be assumed. The importance of understanding the study population before administering surveys is implicit. Previous studies also have found a positive relationship
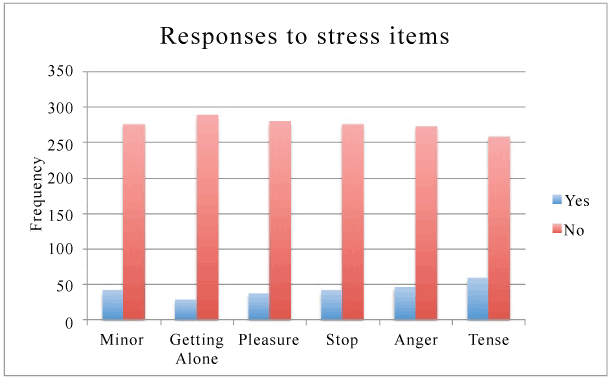
Figure 1: Distribution of responses to stress survey items

Figure 2: Distribution of responses to positively and negatively worded emotions
between emotions and health behaviors [10,11,86]. Gibson (2006) [87] found mood can alter food choices and suggested that eating may calm stressed “nerves” through hedonic sensory qualities that elicit pleasure. In human laboratory research, negative mood states have been related to altered preferences for highly-palatable foods [88] and to a disinhibiting effect on eating [89,90]. Udo found non-obese participants had less resistance to eating during negative mood induction than positive mood induction [12]. A meta-analysis by Knottinen examined relationships between depression/depressive symptoms and obesity [91]. Higher levels of depression were related to a tendency to eat during negative- emotions lower self-efficacy for physical activity when facing barriers, lower reported physical activity, and higher levels of adiposity [91]. Finally, the link between emotions and sleep quality has been noted in previous research. Stewart (2011) found adults with higher reported negative affect had poorer sleep quality [92]. Furthermore, poor sleep quality has been associated with depression [14], anger, hostility, and aggression [15-17].
The relationship between stress and health behaviors is controversial [93,94]. Some studies have found certain types of stress including work stress to be associated with obesity-related behaviors among adults (e.g. diet and exercise quality) [95-98]. However, other studies have failed to show a relationship between stress and dietary changes, similar to our own study [99-101]. This may be due in part to the differences in responses to stress. A meta-analysis captured this ambiguity with approximately 40% of individuals increasing their intake, 40% decreasing their intake, and 20% reporting no change their intake and eating behaviors in response to perceived stress [102]. Interestingly, individuals who were in the higher range of normal weight or who were overweight generally increased their intake with stress, whereas those who are underweight or in the lower end of normal weight typically did not increase their intake or decreased their intake [103]. Additionally, those individuals who were “emotional eaters” tended to have cravings for and increase their intake of high-fat/sweet and rewarding/comfort foods in response to stress. There is evidence that individuals who use food as a reward in stressful times or negative mood states tend to decrease awareness of calorie intake and food restriction in the presence of stress [98]. Women’s dietary practices may be more influenced by stress than men [87,98]. As our study population was largely male, this may be a reason for not finding a significant relationship. Our study failed to find an association between the effect of stress and exercise. Similarly, Conroy (2007) found only a modest association between leisure physical activity and stress levels [104].
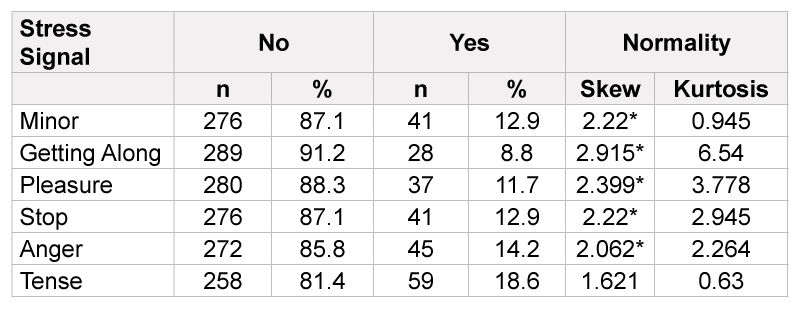
*Non-normality base on: absolute skew >2 or absolute Kurtosis >7; Please refer to Table 1 for more detailed description of response answers.
Table 4: Participant Report of Stress Signals
Another reason for not finding a significant relationship between stress, diet and exercise quality in our study may be the small range of the responses to perceived stress. In one worksite obesity prevention study it was hypothesized that stress would affect risk for obesity through biobehavioral processes. The authors found a relationship between higher stress levels and lower levels of eating awareness, physical activity, and walking, but no relationship between stress levels and BMI or diet quality were seen. The authors suggested that this might be because the range of reported stress scores in the sample was too small to detect associations. The average stress scores were not consistent with the expected highly stressed population [98]. Future studies should address possible moderators of the perceived stress-health behavior relationship (e.g. overweight and obesity, sex, eating behavior domains) [98,105].
Our study did find a relationship between stress and sleep quality. The link between stress and sleep quality was also seen in a study by Kashani (2012) who found that higher levels of stress were correlated with significant disturbances in sleep duration and quality [106]. Hemmingsson (2014) stated that sleep patterns are adversely affected by chronic exposure to stress [107].
Although correctional work is recognized as a high stress occupation, in our study self-reports of stress and negatively worded emotions were very low. These findings would imply that this is a population that is rather unstressed. However, this conflicts with the well-supported idea that corrections are a high stress occupation [34,35,65]. Previous studies also reported such conflicts [29,108], suggesting that correctional employees under-report stress and emotions (particularly negatively worded emotions). In contrast, in our study, responses to positivelyworded emotions had a more uniform distribution, possibly signifying more accurate reporting. Although they are asking very similar questions more participants admit to not feeling happy (possibly because it is a positively-worded emotion) whereas a much smaller percentage of participants admit to feeling downhearted hearted/blue (possibly because it is a negatively worded emotion). Interestingly, correctional employees may more accurately report positively-worded emotions, but are less likely to report negatively worded emotions.
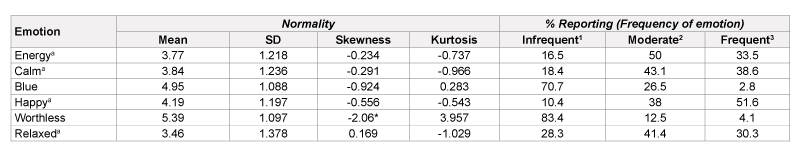
*Non-normality base on: absolute skew >2 or absolute Kurtosis >7;
aReverse coded so that higher values represent better overall emotion for data analyses
1Little or none of the time (1-2); 2Some of the time (3-4); 3All or most of the time (5-6).
Please refer to Table 1 for more detailed description of response answers.
Table 5: Participant Report of Emotions
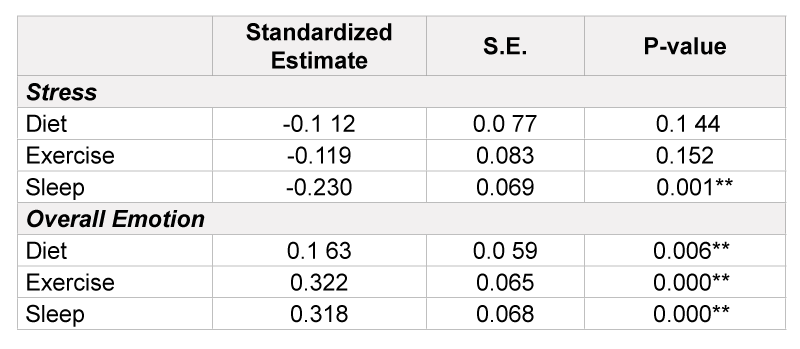
*p>0.05.; **p>0.01.
Table 6: Stress & Overall Emotion’s Effects on Health Behaviors
These results suggest that correctional employees may be underreporting stress and negatively worded emotions. This may conceivably be the result of job prescribed emotional labor in which employees are expected to refrain from displaying stress and emotions to prevent the appearance of weakness. Correctional employees are often expected to display certain emotions while on the job such as appearing strong and tough in stressful situations, even if these emotions are at odds with their true emotions [67]. This may be a reason why correctional employees, and law enforcement employees in general, have been noted to underreport signs of weakness of stress and stress-related symptoms.
Under-reporting has been reported in other studies as discrepancies between reported levels of stress and physiological levels of stress. Given the reliance of many investigators on surveys and psychosocial assessment, the discrepancy is a potential serious barrier to valid results. Cheek (1983) found that objective stress measures (e.g. physical illness and high divorce rates) in correctional officers suggest high job stress. In contrast, correctional officers reported they were not especially stressed or tense. Although corrections officers denied their stress and its consequences (physical, emotional, interpersonal, and occupational), they readily reported stress-related problems in their colleagues, noting that correctional work is indeed stressful yet reporting that they themselves did not feel the effects of this stress. The authors concluded that correctional officers attempt to hold in their emotions and deny their weaknesses [108]. Morse et al. (2011) found that correctional officers’ surveys indicated high levels of stress-related symptoms (hypertension, alcohol consumption) and that a majority of employees were concerned about their personal safety (almost 66%). However, these same employees reported confidence in managing the demands of the job. The authors concluded that the conflict between stress-related symptoms and reported stress may have resulted from a false perception of adequately managing stress [29]. McCarty (2009) found similar discrepancies between physiological and self-reported levels of stress, and suggested that when assessing correctional employee stress, physiological measures should be utilized if possible (e.g. cortisol, dehydroepiandrosterone (DHEA), cholesterol, triglycerides, fasting glucose levels, 10-min resting electrocardiogram, heart rate variability, and blood pressure) [24,109].
Conclusion
Law enforcement personnel face difficult situations in which they on stress reduction skills to regain psychological and physiological equilibrium [35], and may refrain from expressing true emotions. Seeking psychiatric assistance can be seen as a weakness [64]. Due to the negative physical affects, experience negative emotions and may have little trainingbehavioral outcomes, and mental health implications, it is important to address occupational stress and negative emotions in law enforcement personnel. Particularly, efforts to educate law enforcement employees on the risks of stress and withheld emotions and on effective ways to cope may be helpful in alleviating emotional turmoil. Training employees in managing their emotions has been recommended [63]. Lourel advised that high stress occupations such as law enforcement should have counseling and psychological support, and that employees should be provided with regular debriefing support to prevent psychological disturbances and promote overall health and wellbeing [110]. Moreover, health care professionals should pay extra attention to the physiological and physical health of patients who work in high stress occupations. Finally, emotions have been noted as central to decision making [111] and can be highly predictive of health behaviors [112,113], however, they are rarely addressed in social-cognitive interventions [114]. Future interventions would benefit from considering the influence of stress and emotions on participant health behaviors, and understanding the unique stressors that may be inhibiting healthy behaviors. Incorporating occupational health psychology in health promotion effort should be considered to help achieve sustainable outcomes in employee health behavior change.
References
- Center for Disease Control and Prevention National Center for Disease Statistics (2013) Health, United States, 2012: With special feature on emergency care. Hyattsville, MD. [Ref.]
- National Institutes of Health (1998) Clinical guidelines on the identification, evaluation, and treatment of overweight and obesity in adults—The evidence report. NIH Publication, Tech Rep, 98-4083. [Ref.]
- Jensen MD, Ryan DH, Apovian CM, Ard JD, Comuzzie AG, et al. (2013) 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: A report of the American College of Cardiology/ American Heart Association Task Force on Practice Guidelines and the Obesity Society. Circulation 129: S102-S138. [Ref.]
- National Task Force on the Prevention and Treatment of Obesity (2000) Overweight, obesity, and health risk. Arch Intern Med 160: 898-904. [Ref.]
- U.S. Department of Health and Human Services (2010) The surgeon general’s vision for a healthy and fit nation. Department of Health and Human Services, Office of the Surgeon General, Rockville, MD: U.S. [Ref.]
- Trogdon JG, Finkelstein EA, Feagan CW, Cohen JW (2012) State- and payer-specific estimates of annual medical expenditures attributable to obesity. Obesity (Silver Spring) 20: 214-220. [Ref.]
- Drapeau V, Hetherington M, Tremblay A (2011) Impact of eating and lifestyle behaviors on body weight: Beyond energy value. In: Handbook of Behavior, Food, and Nutrition, Preedy VR, Watson RR, Martin CR (eds), Springer New York 693-706. [Ref.]
- Demark-Wahnefried W, Morey MC, Sloane R, Snyder DC, Miller PE, et al. (2012) Reach out to enhance wellness home-based dietexercise intervention promotes reproducible and sustainable longterm improvements in health behaviors, body weight, and physical functioning in older, overweight/obese cancer survivors. J Clin Oncol 30: 2354-2361. [Ref.]
- Mozaffarian D, Hao T, Rimm EB, Willett WC, Hu FB (2011) Changes in diet and lifestyle and long-term weight gain in women and men. N Engl J Med 364: 2392-2404. [Ref.]
- Loxton NJ, Dawe S, Cahill A (2011) Does negative mood drive the urge to eat? The contribution of negative mood, exposure to food cues and eating style. Appetite 56: 368-374. [Ref.]
- Macht M (2008) How emotions affect eating: a five-way model. Appetite 50: 1-11. [Ref.]
- Udo T, Grilo CM, Brownell KD, Weinberger AH, Dileone RJ, et al. (2013) Modeling the effects of positive and negative mood on the ability to resist eating in obese and non-obese individuals. Eat Behav 14: 40-46. [Ref.]
- Akerstedt T (2006) Psychosocial stress and impaired sleep. Scand J Work Environ Health 32: 493-501. [Ref.]
- Tsuno N, Besset A, Ritchie K (2005) Sleep and depression. J Clin Psychiatry 66: 1254-1269. [Ref.]
- Shin C, Kim J, Yi H, Lee H, Lee J, et al. (2005) Relationship between trait-anger and sleep disturbances in middle-aged men and women. J Psychosom Res 58: 183-189. [Ref.]
- Caska CM, Hendrickson BE, Wong MH, Ali S, Neylan T, et al. (2009) Anger expression and sleep quality in patients with coronary heart disease: findings from the Heart and Soul Study. Psychosom Med 71: 280-285. [Ref.]
- Taylor ND, Fireman GD, Levin R (2013) Trait Hostility, Perceived Stress, and Sleep Quality in a Sample of Normal Sleepers. Sleep Disord 2013: 735812. [Ref.]
- Wardle J, Steptoe A, Oliver G, Lipsey Z (2000) Stress, dietary restraint and food intake. J Psychosom Res 48: 195-202. [Ref.]
- Kirk MA, Rhodes RE (2011) Occupation correlates of adults’ participation in leisure-time physical activity: a systematic review. Am J Prev Med 40: 476-485. [Ref.]
- Twisk JW, Snel J, Kemper HC, van Mechelen W (1999) Changes in daily hassles and life events and the relationship with coronary heart disease risk factors: a 2-year longitudinal study in 27-29-year-old males and females. J Psychosom Res 46: 229-240. [Ref.]
- Wardle J, Chida Y, Gibson EL, Whitaker KL, Steptoe A (2011) Stress and adiposity: a meta-analysis of longitudinal studies. Obesity (Silver Spring) 19: 771-778. [Ref.]
- Caban AJ, Lee DJ, Fleming LE, Gómez-Marín O, LeBlanc W, et al. (2005) Obesity in US workers: The National Health Interview Survey, 1986 to 2002. Am J Public Health 95: 1614-1622. [Ref.]
- Chandola T, Brunner E, Marmot M (2006) Chronic stress at work and the metabolic syndrome: prospective study. BMJ 332: 521-525. [Ref.]
- McCraty R, Atkinson M, Lipsenthal L, Arguelles L (2009) New hope for correctional officers: an innovative program for reducing stress and health risks. Appl Psychophysiol Biofeedback 34: 251-272. [Ref.]
- Chandola T, Britton A, Brunner E, Hemingway H, Malik M, et al. (2008) Work stress and coronary heart disease: what are the mechanisms? Eur Heart J 29: 640-648. [Ref.]
- Cooper CL, Davidson MJ, Robinson P (1982) Stress in the police service. J Occup Med 24: 30-36. [Ref.]
- Kirkcaldy B1, Cooper CL, Ruffalo P (1995) Work stress and health in a sample of U.S. police. Psychol Rep 76: 700-702. [Ref.]
- Karasek RA (1992) Healthy Work: Stress, Productivity and the Reconstruction of Working Life.Basic Books, New York.[Ref.]
- Morse T, Dussetschleger J, Warren N, Cherniack M (2011) Talking about health: correction employees’ assessments of obstacles to healthy living. J Occup Environ Med 53: 1037-1045. [Ref.]
- Melchior M, Caspi A, Milne BJ, Danese A, Poulton R, et al. (2007) Work stress precipitates depression and anxiety in young, working women and men. Psychol Med 37: 1119-1129. [Ref.]
- Blackmore ER, Stansfeld SA, Weller I, Munce S, Zagorski BM, et al. (2007) Major depressive episodes and work stress: results from a national population survey. Am J Public Health 97: 2088-2093. [Ref.]
- Paterniti S, Niedhammer I, Lang T, Consoli SM (2002) Psychosocial factors at work, personality traits and depressive symptoms. Longitudinal results from the GAZEL Study. Br J Psychiatry 181: 111- 117. [Ref.]
- Mausner-Dorsch H, Eaton WW (2000) Psychosocial work environment and depression: epidemiologic assessment of the demand-control model. Am J Public Health 90: 1765-1770. [Ref.]
- Denhof MD, Spinaris CG (2013) Depression, PTSD, and comorbidity in United States corrections professionals: Prevalence and impact on helath and functioning. Desert Waters Correctional Outreach, Florence [Ref.]
- McCraty R, Atkinson M, Lipsenthal L, Arguelles L (2003) Impact of the power to change performance program on stress and health risks in correctional officers. HeartMath Research Center, Institute of HeartMath, Tech. Rep. 03-014, Boulder Creek, CA. [Ref.]
- Ferraro L, Faghri PD, Henning R, Cherniack M (2013) Workplacebased participatory approach to weight loss for correctional employees. J Occup Environ Med 55: 147-155. [Ref.]
- Kivimäki M, Head J, Ferrie JE, Shipley MJ, Brunner E, et al. (2006) Work stress, weight gain and weight loss: evidence for bidirectional effects of job strain on body mass index in the Whitehall II study. Int J Obes (Lond) 30: 982-987. [Ref.]
- Dignam JT, Barrera M Jr, West SG (1986) Occupational stress, social support, and burnout among correctional officers. Am J Community Psychol 14: 177-193. [Ref.]
- Hannerz H, Albertsen K, Nielsen ML, Tuchsen F, Burr H (2004) Occupational factors and 5-year weight change among men in a danish national cohort. Health Psychol 23: 283-288. [Ref.]
- Oginska-Bulik N (2005) Emotional intelligence in the workplace: exploring its effects on occupational stress and health outcomes in human service workers. Int J Occup Med Environ Health 18: 167-175. [Ref.]
- Ramey SL, Downing NR, Franke WD (2009) Milwaukee police department retirees: cardiovascular disease risk and morbidity among aging law enforcement officers. AAOHN J 57: 448-453. [Ref.]
- Schaufeli WB, Peeters MCW (2000) Job Stress And Burnout Among Correctional Officers: A Literature Review. International Journal of Stress Management 7: 19-48. [Ref.]
- Burke RJ (1994) Stressful events, work-family conflict, coping, psychological burnout, and well-being among police officers. Psychol Rep 75: 787-800. [Ref.]
- Ghaddar A, Mateo I, Sanchez P (2008) Occupational stress and mental health among correctional officers: a cross-sectional study. J Occup Health 50: 92-98. [Ref.]
- Stack SJ, Tsoudisa O (1997) Suicide risk among correctional officers: a logistic regression analysis. Archives of Suicide Research 183-186. [Ref.]
- Agid O, Kohn Y, Lerer B (2000) Environmental stress and psychiatric illness. Biomed Pharmacother 54: 135-141. [Ref.]
- Obidoa C, Reeves D, Warren N, Reisine S, Cherniack M (2011) Depression and work family conflict among corrections officers. J Occup Environ Med 53: 1294-1301. [Ref.]
- Brotheridge CM, Grandey AA (2002) Emotional labor and burnout: comparing two perspectives of “people work”. Journal of Vocational Behavior 60: 17-39. [Ref.]
- Hochschild AR (1983) The Managed Heart: Commercialization of Human Feeling. University of California Press, Berkley 1983. [Ref.]
- Grandey AA (2000) Emotion regulation in the workplace: a new way to conceptualize emotional labor. J Occup Health Psychol 5: 95-110.s [Ref.]
- Wharton AS (1999) The psychosocial consequences of emotional labor. Annals of the American Academy of Political and Social Science 158-176. [Ref.]
- de Castro AB, Agnew J, Fitzgerald ST (2004) Emotional labor: relevant theory for occupational health practice in post-industrial America. AAOHN J 52: 109-115. [Ref.]
- Ashforth B, Humphrey R (1993) Emotional Labor in Service Roles: The Influence of Identity. Academy of Management Executive 18: 88-115. [Ref.]
- Van Maanen J, Kunda G (1989) Real feelings: Emotional expression and organizational culture. Research in Organizational Behavior 11: 43-103. [Ref.]
- Abraham R (1999) Emotional Intelligence in Organizations: A Conceptualization. Genetic, Social & General Psychology Monographs 125: 209-224. [Ref.]
- Pugh SD, Groth M, Hennig-Thurau T (2011) Willing and able to fake emotions: a closer examination of the link between emotional dissonance and employee well-being. J Appl Psychol 96: 377-390.[Ref.]
- Robins SP, Judge TA (2012) Organizational Behavior. 15th edition, Pearson Education.[Ref.]
- McCraty R, Tomasino D, Atkinson M, Sundram J (1999) Impact of the HeartMath self-management skills program on physiological and psychological stress in police officers. HeartMath Research Center, Institute of HeartMath, Tech Rep 99-075. [Ref.]
- McLaren S, Gollan W, Horwell C (1998) Perceived stress as a function of occupation. Psychol Rep 82: 794. [Ref.]
- Coman G, Evans B (1991) Stressors facing Australian police in the 1990s. Police Studies 14: 153-165. [Ref.]
- Gaines J, Jermier J (1983) Emotional exhaustion in a high stress organization. Acad Manag J 26: 567-586. [Ref.]
- Jackson S, Malasch C (1982) After-effects of job-related stress: Families as victims. Journal of Occupational Behavior 3: 63-77. [Ref.]
- Bakker AB, Heuven E (2006) Emotional Dissonance, Burnout, and InRole Performance Among Nurses and Police Officers. International Journal of Stress Management 13: 423-440. [Ref.]
- MacDonald CM (2003) Evaluation of stress debriefing interventions with military populations. Mil Med 168: 961-968. [Ref.]
- Micieli J (2008) Stress and the effects of working in a high security prison. National Institute of Justice, Rockville, MD, Tech Rep 224105. [Ref.]
- Center for Substance Abuse Treatment (US) (2014) Chapter 3, understanding the impact of trauma. In: Trauma-Informed Care in Behavioral Health Services, 57th edition, Centre for Substance Abuse and Mental Health Services Administration (US), Rockville, MD [Ref.]
- Tracy SJ (2005) Locking up emotion: Moving beyond dissonance and understanding emotion labor discomfort. Communication Monographs 72: 261-283. [Ref.]
- Pogrebin MR, Poole ED (1991) Police and tragic events: The management of emotion. Journal of Criminal Justice 19: 395-403. [Ref.]
- Zapf D, Vogt C, Seifert C, Mertini H, Isic A (1999) Emotion Work as a Source of Stress: The Concept and Development of an Instrument. European Journal of Work and Organizational Psychology 8: 371-400. [Ref.]
- Veneziano C (1984) Occupational Stress and the line correctional officer. Southern Journal of Criminal Justice 8: 214-231. [Ref.]
- Brown JM, Campbell EA (1994) Stress and policing: Sources and strategies. John Wiley & Sons, Chichester. [Ref.]
- Sewell J (1981) Police stress. FBI law enforcement bulletin 50: 7-11. [Ref.]
- Faghri PD, Blozie E, Gustavesen S, Kotejoshyer R (2008) The role of tailored consultation following health-risk appraisals in employees’ health behavior. J Occup Environ Med 50: 1378-1385. [Ref.]
- Wellsource I (2011) Personal Wellness Profile. Advantage Health Risk Assessment. [Ref.]
- National Heart Lung and Blood Institute (2012) What are Overweight and Obesity? NIH. [Ref.]
- IBM Corp (2012) IBM SPSS Statistics for Windows, Version 21.0. [Ref.]
- Kim HY (2013) Statistical notes for clinical researchers: assessing normal distribution using skewness and kurtosis. Restor Dent Endod 38: 52-54. [Ref.]
- SPSS Inc (2008) Chapter 5: Outliers and Anomalous Data. In: Introduction to clementine and data mining, Chicago, IL, 5-1-5-27. [Ref.]
- Wiley DE (1973) Identification problem for structural equation models with unmeasured variables. In: Structural Equation Models in the Social Sciences. Academic Press, New York 66-83. [Ref.]
- Keesling JW (1972) Maximum likelihood approaches to causal analysis. [Ref.]
- Joreskog KG (1973) A general method for estimating a linear structural equation system. In: Structural Equation Models in the Social Sciences, Goldberger AS, Duncan OD (eds), Academic Press, New York 85-112. [Ref.]
- Muthén LK, Muthén BO (2010) Mplus User’s Guide. Los Angeles, CA. [Ref.]
- Buhi ER, Goodson P, Neilands TB (2007) Structural equation modeling: a primer for health behavior researchers. Am J Health Behav 31: 74- 85. [Ref.]
- Muthén BO (2002) Beyond SEM: General Latent Variable Modeling. Behaviormetrika 29: 81-117. [Ref.]
- Hu L, Bentler PM (1999) Cutoff criteria for fit indexes in covariance structure analysis: conventional criteria versus new alternatives. Structural Equation Modeling: A Multidisciplinary Journal 6: 1-55. [Ref.]
- Stice E, Presnell K, Shaw H, Rohde P (2005) Psychological and behavioral risk factors for obesity onset in adolescent girls: a prospective study. J Consult Clin Psychol 73: 195-202. [Ref.]
- Gibson EL (2006) Emotional influences on food choice: sensory, physiological and psychological pathways. Physiol Behav 89: 53-61. [Ref.]
- Oliver G, Wardle J, Gibson EL (2000) Stress and food choice: a laboratory study. Psychosom Med 62: 853-865. [Ref.]
- Habhab S, Sheldon JP, Loeb RC (2009) The relationship between stress, dietary restraint, and food preferences in women. Appetite 52: 437-444. [Ref.]
- Lattimore P, Caswell N (2004) Differential effects of active and passive stress on food intake in restrained and unrestrained eaters. Appetite 42: 167-173. [Ref.]
- Konttinen H, Silventoinen K, Sarlio-Lahteenkorva S, Mannisto S, Haukkala A (2010) Emotional eating and physical activity self-efficacy as pathways in the association between depressive symptoms and adiposity indicators. Am J Clin Nutr 92: 1031-1039. [Ref.]
- Stewart JC, Rand KL, Hawkins MA, Stines JA (2011) Associations of the shared and unique of positive and negetive emotional factors with sleep quality. Personality and Individual Differences 50: 609-614. [Ref.]
- Trost SG, Owen N, Bauman AE, Sallis JF, Brown W (2002) Correlates of adults’ participation in physical activity: review and update. Med Sci Sports Exerc 34: 1996-2001. [Ref.]
- Rhodes RE, Nigg CR (2011) Advancing physical activity theory: a review and future directions. Exerc Sport Sci Rev 39: 113-119. [Ref.]
- Tamers SL, Beresford SA, Cheadle AD, Zheng Y, Bishop SK, et al. (2011) The association between worksite social support, diet, physical activity and body mass index. Prev Med 53: 53-56. [Ref.]
- Cash SW, Beresford SA, Henderson JA, McTiernan A, Xiao L, et al. (2012) Dietary and physical activity behaviors related to obesityspecific quality of life and work productivity: baseline results from a worksite trial. Br J Nutr 108: 1134-1142. [Ref.]
- Choi B, Schnall PL, Yang H, Dobson M, Landsbergis P, et al. (2010) Psychosocial working conditions and active leisure-time physical activity in middle-aged us workers. Int J Occup Med Environ Health 23: 239-253. [Ref.]
- Barrington WE, Ceballos RM, Bishop SK, McGregor BA, Beresford SAA (2012) Perceived stress, behavior, and body mass index among adults participating in a worksite obesity prevention program, Seattle, 2005-2007. Prev Chronic Dis 9: 120001. [Ref.]
- Griffin KW, Friend R, Eitel P, Lobel M (1993) Effects of environmental demands, stress, and mood on health practices. J Behav Med 16: 643- 661. [Ref.]
- Macht M, Haupt C, Ellgring H (2005) The perceived function of eating is changed during examination stress: a field study. Eat Behav 6: 109-112. [Ref.]
- Pollard TM, Steptoe A, Canaan L, Davies GJ, Wardle J (1995) Effects of academic examination stress on eating behavior and blood lipid levels. Int J Behav Med 2: 299-320. [Ref.]
- Dallman MF (2010) Stress-induced obesity and the emotional nervous system. Trends Endocrinol Metab 21: 159-165. [Ref.]
- Brunner EJ, Chandola T, Marmot MG (2007) Prospective effect of job strain on general and central obesity in the Whitehall II Study. Am J Epidemiol 165: 828-837. [Ref.]
- Conroy MB, Simkin-Silverman LR, Pettee KK, Hess R, Kuller LH, et al. (2007) Lapses and psychosocial factors related to physical activity in early postmenopause. Med Sci Sports Exerc 39: 1858-1866. [Ref.]
- Oliver G, Wardle J (1999) Perceived effects of stress on food choice. Physiol Behav 66: 511-515. [Ref.]
- Kashani M, Eliasson A, Vernalis M (2012) Perceived stress correlates with disturbed sleep: a link connecting stress and cardiovascular disease. Stress 15: 45-51. [Ref.]
- Hemmingsson E (2014) A new model of the role of psychological and emotional distress in promoting obesity: conceptual review with implications for treatment and prevention. Obes Rev 15: 769-779. [Ref.]
- Cheek FE (1984) Stress Management for Correctional Officers and their Families. American Correctional Association, Alexandria, VA. [Ref.]
- Torres SJ, Nowson CA (2007) Relationship between stress, eating behavior, and obesity. Nutrition 23: 887-894. [Ref.]
- Lourel M, Abdellaoui S, Chevaleyre S, Paltrier M, Gana K (2008) Relationships Between Psychological Job Demands, Job Control and Burnout Among Firefighters. North American Journal of Psychology 10: 489-496. [Ref.]
- Loewenstein G, Lerner J (2003) The role of emotion in decision making. In: The Handbook of Affective Science, Davidson RJ, Goldsmith HH, Scherer KR (eds), Oxford University Press, Oxford, England. [Ref.]
- Lawton R, Conner M, McEachan R (2009) Desire or reason: predicting health behaviors from affective and cognitive attitudes. Health Psychol 28: 56-65.[Ref.]
- Norton TR, Bogart LM, Cecil H, Pinkerton SD (2005) Primacy of affect over cognition in determining adult men’s condom-use behavior. Journal of Applied Social Psychology 35: 2493-2534. [Ref.]
- Ferrer RA, Fisher JD, Buck R, Amico KR (2011) Pilot test of an emotional education intervention component for sexual risk reduction. Health Psychol 30: 656-660. [Ref.]
Download Provisional PDF Here
Article Information
Article Type: Research Article
Citation: Faghri PD, Mignano C, Cherniack M and Huedo-Medina TB (2015) Psychological Health and Overweight and Obesity Among High Stressed Work Environments. Obes Open Access Volume1.1: http://dx.doi.org/10.16966/2380-5528.101
Copyright: © 2015 Faghri PD, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
SCI FORSCHEN JOURNALS
All Sci Forschen Journals are Open Access
