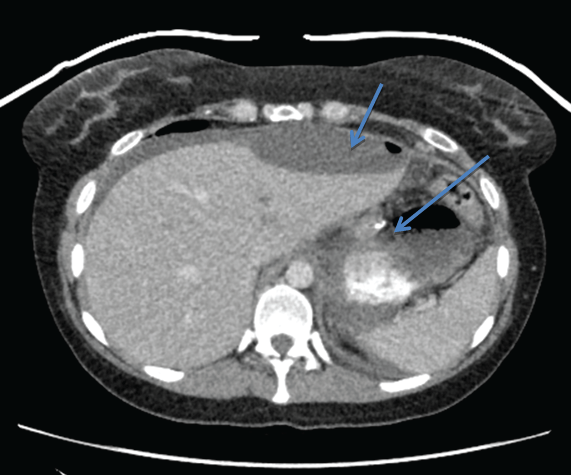
Figure 1: Free sleeve gastrectomy leak.


Ruth Blackham1 Jeff Hamdorf1 Jeremy Tan1*
Western Surgical Health, Broadway, Nedlands, Western Australia, Australia*Corresponding author: Jeremy Tan, Western Surgical Health, Broadway, Nedlands, Western Australia 6009, Australia, Tel: +65 6220 9323; E-mail: jthtan1@gmail.com
The management of staple line disruption following sleeve gastrectomy is a controversial area. We propose a novel method of converting a leaking sleeve gastrectomy to a Roux-en-Y gastric bypass in the acute setting, regardless of whether the defect is able to be visualized. Our proposed method of undertaking a major surgical reconstructive procedure is seemingly counter to traditional surgical dogma, requiring two anastomoses within a potentially septic field. We present three cases of sleeve leak where the conversion to a gastric bypass acutely was completed successfully. Additionally the potential length of stay and number of procedures is decreased in a Roux-en-Y conversion compared to endoscopic therapeutic measures in the same setting.
Gastric bypass; Laparoscopic; Leaks; Sleeve gastrectomy; Complication
Sleeve gastrectomy leaks are amongst the most challenging of complications after this increasingly popular bariatric procedure [1]. Until recently the accepted methods of treatment involved a combination of laparotomy, laparoscopy, endoscopic covered stenting or double pigtail stents, percutaneous radiologically guided drainage, jejunal enteric feeding and total parenteral nutrition [2]. Several algorithms have been proposed as to how to manage these sleeve gastrectomy leaks [2-6]. However none to-date have suggested conversion to a Roux-en-Y gastric bypass at the initial washout and drainage procedure in an early sleeve gastrectomy leak. To our knowledge there is only a single case report to date which has suggested this approach [7].
We present a series of three cases where this relatively counter-intuitive strategy was followed with positive outcomes.
The first patient was a 43 year old female who underwent elective sleeve gastrectomy after gastric band removal three months prior. After an uneventful procedure the patient developed left upper quadrant pain with abdominal distension on the second day postoperatively. A CT scan (Figure 1), suggested a proximal staple line disruption (Figure 1)

Figure 1: Free sleeve gastrectomy leak.
She was taken to theatre for a laparoscopy and this was converted to laparotomy to allow better visualization of the proximal staple line leak. At surgery an out-pouching of the gastric pouch was seen at the proximal end of the sleeve with a perforation at the “tip” of the pouch. The pouch, including the site of the leak was excised and a Roux-en-Y gastric bypass was performed (Figure 2). A feeding gastrostomy was inserted into the distal stomach remnant (Figure 2).
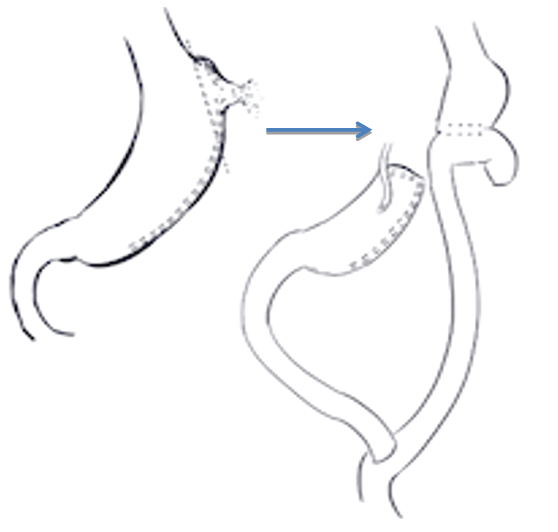
Figure 2: Excision of leak and conversion to Roux-en-Ygastric bypass.
Post-operatively the patient sustained a wound infection as a result of some subcutaneous cross-contamination of leakage from around the gastrostomy tube. The wound was re-opened on the ward and managed with a negative-pressure (VAC) wound dressing.
Otherwise, the patient made a good recovery and was discharged after a total hospital stay of 21postoperative days.
The patient was a 67 year old woman who underwent gastric band removal three years previously. The laparoscopic sleeve gastrectomy required substantial adhesiolysis with a staple device misfire at the distal end of the sleeve. This was secured and reinforced with a further deployment of the stapler and large bore drain placed adjacent to the area. Four days postoperatively she developed left upper quadrant pain, fever and became tachycardic. A CT scan showed a localised collection in the left upper quadrant (Figure 3).
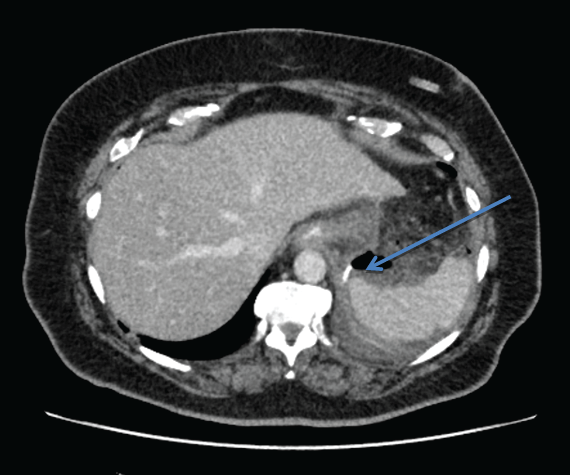
Figure 3: Contained sleeve gastrectomy leak.
At laparoscopy, there was a 3 cm × 4 cm abscess located in the left upper quadrant adjacent to the uppermost part of the staple line. There was no identifiable disruption of the staple line, but there appeared to be a slight twist in the region of the angularis incisura such that the passage of a 40 Fr bougie passed trans-orally was impeded just above this point. The abscess was drained and a laparoscopic Roux-en-Y gastric bypass was performed. The gastro-jejunostomy was fashioned just proximal to the point of impaction of the bougie. (Figure 4) A feeding gastrostomy was inserted laparoscopically into the distal (excluded) stomach. A 28 Fr bore drain was left adjacent to the staple line in the left upper quadrant (LUQ) (Figure 4).
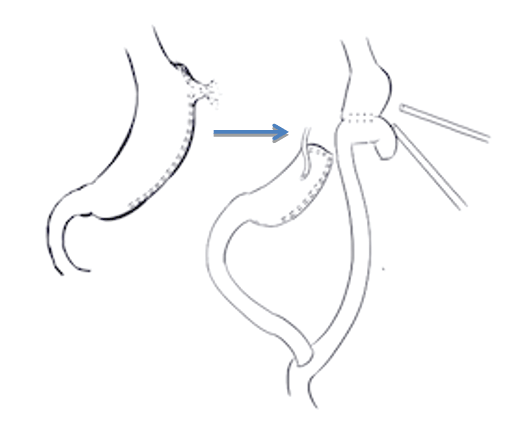
Figure 4: Roux-en-Y gastric bypass with gastro-jejunal anastomosis below presumptive leak site.
The patient developed quite extensive cellulitis around the gastrostomy tube exit site and was treated with intravenous antibiotics. She otherwise remained systemically well throughout the post-operative period.
Although no leak was seen at surgery, oral contrast swallow studies at days 7 and 14 following the bypass surgery showed a persistent small leak of contrast from the upper gastric pouch to the bore drain (Figure 5). However, as the daily output from the drain was <5 mL, the patient was allowed oral intake and she was discharged at day 31 with drain insitu. This was removed after six weeks without the need for additional procedures (Figure 5).
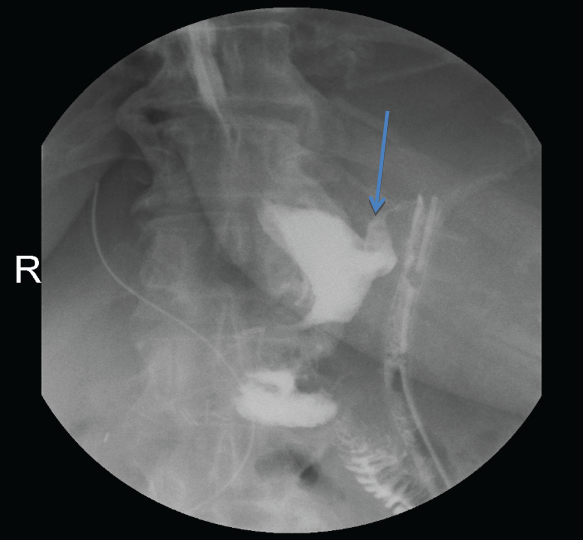
Figure 5: Oral contrast swallow study showing persistent leak into drain.
The patient was a 38 year old man who had a laparoscopic adjustable gastric band removed one year previously as a result of persistent dysphagia. He developed a fever of 38.9 degrees on the third day after undergoing a routine sleeve gastrectomy. The CRP was elevated to over 200 mg/L. A CT scan showed a collection contiguous with the proximal gastric remnant and left lobe of liver.
At laparoscopy he had gross contamination of the left supracolic compartment. After drainage of the pus and despite methylene blue testing, no leak was identified. A 38 Fr bougie passed trans-orally appeared to impact at a fold adjacent to the angularis incisura of the stomach. As such, the decision was made to perform a laparoscopic acute conversion to a Roux-en-Y gastric bypass with insertion of a feeding jejunostomy. The gastric remnant was divided and gastro-jejunostomy formed just proximal to the point of impaction of the bougie. A 28 Fr bore drain was placed adjacent to the gastric remnant staple line.
A CT-swallow performed five days later showed an air-filled collection with a small amount of contrast extravasation. The bore drain was withdrawn by approximately 8 cm and following this drained 100-200 mL daily for several days before tapering off.
A repeat CT swallow performed on day 11 post-op showed a small sliver of air adjacent to the gastric staple line without further extravasation of contrast (Figure 6).
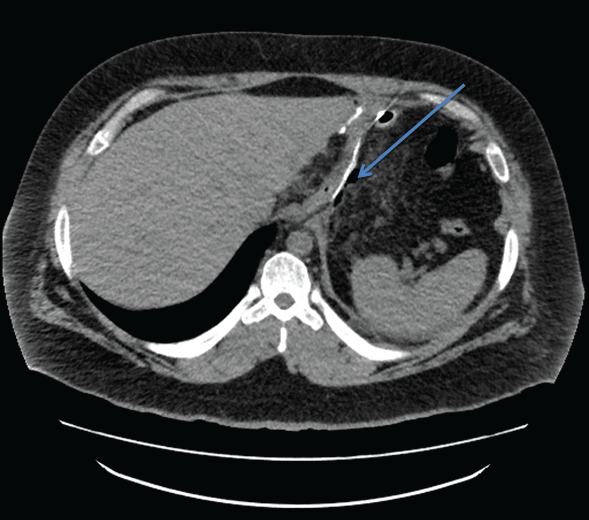
Figure 6: Resolving leak following Roux-en-Y gastric bypass.
The drain output fell to less than 10 mL a day, and accordingly, the patient was allowed to commence oral fluid intake. The drain output remained low and the patient discharged home after a total hospital stay of 16 days, without the need for jejunostomy feeds. The drain was left in for a further week and removed.
The current management of leaks following sleeve gastrectomy is based upon the consensus guidelines of the ASMBS [8]. These state that operative management for acute gastro-intestinal leaks follows the arguably somewhat traditional goals of drainage and placement of drains for controlled fistula formation. They also note that definitive surgical management of non-healing fistulas is technically challenging without favouring one procedure over another. Current surgical algorithms include early over sewing, drainage, endoscopic stenting or use of a Roux limb. For sleeve gastrectomy leaks with free perforation, a “damage control” approach with laparoscopic washout and drainage has been used, followed by endoscopic intervention [8-10]. Despite this traditional approach, there remains a number of patients who develop a chronic fistula requiring delayed definitive salvage surgery, usually in the form of fistula excision then Roux-en-Y oesophago-jejunostomy [5,11,12].
The three patients presented similarly in terms of: clinical status, inflammatory and infectious biology, cardiac and general constants. All three patients were haemodynamically stable, had been operated on within the previous 5 days and as such represented early sleeve gastrectomy leaks. Microbiological culture of specimens taken intra-operatively grew a combination of enteric bacteria and fungi. Intra-operative endoscopy is not routinely undertaken at our Centre as endoscopy is almost exclusively performed by gastroenterologists and not surgeons in our health care setting. Furthermore, expertise for interventional endoscopy for the deployment of long covered stents and/or balloon dilatation of the incisura, as well as insertion of double pig-tail stents for the management of sleeve leaks resides in another hospital, namely the public tertiary referral centre, and patient transfer with the inevitable delay in treatment would ensue if interventional endoscopy was desired.
We thus propose that the surgical approach of direct conversion to bypass leads to quicker leak resolution, decreased inpatient stay and a lower number of procedures overall, as most reports on endoscopic management specify a median of 3-6 endoscopic procedures in leaking sleeve gastrectomies before leak resolution is effected [13]. Risk of stent migration is high, up to 50% after bariatric surgery [14]. Resolution of the leak also often takes up to 6 weeks or more [15] in comparison to 30 days following Roux-en-Y gastric bypass [16]. There are multiple controversies in treatment associated with the inability to perform prospective randomised trials in this setting.
The aetiology of sleeve leaks is highly dependent upon the relative pressure gradient from proximal to distal. Whether the initial insult is due to mechanical causes such as stapler misfire or thermal injury, or a later ischaemic event, the leak is likely to be proximal. The propensity for leaks to occur at the upper end of the staple line may be potentiated by relative ischaemia at the angle of His coupled with relative stenosis of the sleeve, either due to twisting or folding of the sleeved stomach, often in the region of the angularis incisura [17]. This leads to a high pressure in the proximal remnant stomach, which then succumbs at the weakest spot.
There is substantial merit in the principle of forming a Roux-en-Y gastric bypass in the setting of an early, proximal leak. Often such patients have an element of sepsis which justifies prompt surgical intervention. However, limiting surgical intervention to washout, drainage and suturing of the defect, when possible, does not mitigate the high pressure area of the proximal stomach, leaving the patient liable to a secondary leak by failure of the repair. The construction of a bypass allows the pouch to form a low pressure field allowing for healing of the leak site. Ideally the defect is visualized allowing it to be excluded with a stapling device, however as shown above it can be used in the setting where the defect is not seen despite efforts such as methylene blue, air leak testing or intraoperative gastroscopy. The use of a 28 Fr bore drain adjacent to the presumptive site of leakage is also important as the stiffness of this drain ensures a lower likelihood of dislodgement away from the staple line, in addition to its preferentially large lumen.
The sleeve gastrectomy leaks discussed in the patients above were detected early and underwent emergent surgical management prior to potential septic shock with inotrope requirement. The option of gastric bypass is attractive in the more haemodynamically stable patient and potentially in hospitals where interventional endoscopy expertise may not be available. If, despite the Roux-en-Y gastric bypass, the leak is not healing, the option for an endoscopic intervention is still available [18].
There are reports of anastomosing a Roux loop to the defect in the staple line but this presupposes the defect is visible in the first place [19- 22]. We postulate that oedema secondary to inflammation from leak causes difficulty in visualizing a small leak at the time of surgery. When the oedema reduces after 3-5 days, the leak reopens and is often visible on radiological studies with oral contrast. This leak does not heal readily in the high pressure context of a sleeve whereas it behaves more like controlled fistulas elsewhere in the gastro-intestinal tract in the context of a Roux-en-Y gastric bypass.
Our group performs about 300-400 bariatric surgical operations a year and it is important to note that the first two patients were referred to us from another surgeon, and are not from within our Practice. One of the authors also has a public hospital appointment where interventional endoscopy expertise resides and where 10-14 sleeve leaks are managed per year [2,23]. We have published previously regarding the management of sleeve leaks [2], and one of the authors has another article in press [23], pertaining to the management of sleeve leaks where the average time to healing in patients undergoing endoscopic management was 85 days. These patients were endoscopically treated with a combination of long fully covered metal stents, double pigtail stents for internal drainage with balloon dilatation to the incisura angularis, and endoscopic clipping of a small residual mucosal defect.
Our experience thus far has indicated that the relatively novel approach of early conversion from leaking sleeve gastrectomy to Roux-en-Y gastric bypass in the acute setting is safe and effective in appropriate patients. It may be especially useful in centres where interventional endoscopic expertise is not readily available. It is preferable to manage a leaking gastric pouch in a low pressure system within a gastric bypass than it is to manage a leaking sleeve within a high pressure system caused by distal obstruction. Such a surgical algorithm may decrease length of stay and overall morbidity, in addition to obviating the need for further surgical or endoscopic measures.
Credit for diagrams to Dr Jonathon Foo Fellow, Upper Gastro-Intestinal Surgery Unit, at Sir Charles Gairdner Hospital, Western Australia.
Download Provisional PDF Here
Article Type: Case Series
Citation: Blackham R, Hamdorf J, Tan J (2017) Acute Conversion of Early Sleeve Gastrectomy Leak to Roux-en-Y Gastric Bypass. Obes Open Access 3(1): doi http://dx.doi.org/10.16966/2380-5528.128
Copyright: © 2017 Blackham R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access