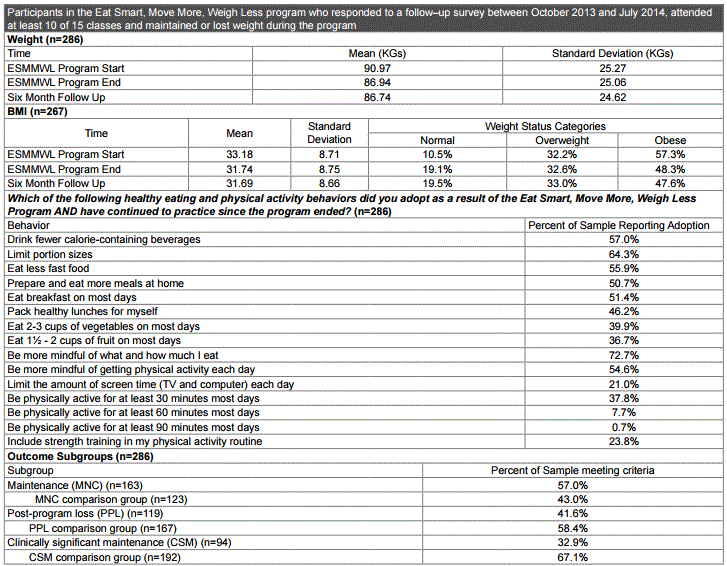
Table 1: Descriptive statistics for weight loss maintenance study sample.


Sam Thompson1* Carolyn Dunn2 Surabhi Aggarwal2 Samuel Tchwenko1 Alice Wang3 Jill Rushing1 Cathy Thomas1 Kelly Nordby2 Christine Allison4
1North Carolina Division of Public Health, Raleigh, North Carolina, USA*Corresponding author: Sam Thompson, North Carolina Division of Public Health, Raleigh, North Carolina 27699-1915, USA, Tel: (919) 707-5238; E-mail: sam.thompson@dhhs.nc.gov
Introduction: The study identifies behaviors associated with weight loss maintenance six months after completing an online weight management program. The findings have potential to inform the promotion and ongoing support of behaviors that foster weight loss maintenance.
Methods: A retrospective cohort design was employed for responses submitted between October 2013 and July 2014 to a follow-up survey of participants in an online weight management program. Participants’ weights at the start of the program (W1), at the end of the program (W2) and six months after the program (W3) were used to create three outcome subgroups: Maintenance (W3 ≤ W2 ≤ W1), Post-program loss (W3<.05) between these outcome subgroups and behaviors adopted and continued as a result of the program.
Results: Eight of 15 weight management behaviors assessed were associated with one or more outcome subgroups while four behaviors (limiting portion sizes, eating vegetables, and mindfulness of healthy eating and physical activity) were associated with all three outcome subgroups.
Conclusion: Study findings identify behaviors that should be fostered as part of a sustained response to overweight and obesity. The identified mindfulness and healthy eating behaviors should be emphasized throughout a weight management curriculum to encourage participants to adopt behaviors that will contribute to their sustained success.
Weight loss maintenance; Weight management; Mindfulness; Obesity; Nutrition; Physical activity; Internet
Behaviors associated with weight loss maintenance six months after completing an online weight management program were identified from responses to a follow-up survey of participants in Eat Smart, Move More, Weigh Less (ESMMWL), a 15-week, evidence-based adult weight management program [1]. This inquiry contributes to existing literature on behaviors that support weight loss maintenance, particularly after online interventions. These findings have potential to inform intervention curricula regarding the promotion of behaviors that support weight loss maintenance, as well as further investigation into the relationships between specific behaviors and weight loss maintenance. These findings may also help public health practitioners identify obesity prevention strategies that support behaviors proven to foster weight loss maintenance.
Online interactive technology interventions have been demonstrated to help participants lose or maintain weight, including maintaining clinically significant weight loss ( ≥ 5% of bodyweight) for a large proportion of participants [2,3]. Participants who completed ESMMWL lost significantly more weight than those in the wait-list control group and had a greater reduction in BMI [4]. Reductions in BMI, weight, and waist circumference were greater for online ESMMWL participants than those attending in-person classes [5]. Internet-based programs reach large numbers of participants in dispersed work settings and lead to improvements in eating habits, as well as moving individuals into the normal weight category [2]. However, the long-term effectiveness of web based weight loss interventions is uncertain [6]. A systematic review of web-based weight loss programs could not reach conclusions on their long-term effectiveness [7]. Computer-delivered interventions have demonstrated sustained improvements in health behaviors outcomes at the first post-intervention assessment [8]. However, the long-term effect of these behaviors on participants’ weight is unknown [8].
This study hypothesizes that ESMMWL online participants who adopted specific healthy eating and physical activity behaviors and continued them after the program ended will be more likely to have
at six-month follow-up when compared against their counterparts who did not adhere to the same behaviors.
The study uses a retrospective cohort design. Responses to follow-up surveys completed between October 2013 and July 2014 were analyzed to identify behaviors that respondents reported adopting and continuing as a result of ESMMWL that were associated with weight loss maintenance six months after the program ended. Study participants were members of the North Carolina State Health Plan for Teachers and State Employees. Though the follow-up survey did not collect demographic data, ESMMWL evaluation data through November of 2015 (n=2,191) suggest that the same population, State Health Plan participants, is 90.8% female, 18.6% African American and 77.5% white, with an average age of 50 years.
ESMMWL was promoted to the study participants through wellness committee leaders and key contacts at state worksites and public schools. Classes were offered monthly and participants enrolled using an online registration form that allowed them to opt-in to the follow-up survey. Participants were provided access to 15 weekly, online, real time sessions with the same classmates and instructor, at the day and time they signed up for during registration. Sessions focused on evidence-based healthy eating and physical activity strategies. Participants set a healthy weight goal for themselves at the beginning of the program, which could be a steady loss of weight or maintenance of current weight. Each week, participants reported their weight, minutes of aerobic activity and minutes of strength training and received personalized feedback from their instructor though an online portal [5].
Participants who opted in were e-mailed the 24-question survey via Survey Monkey (Palo Alto, CA) six months after the program ended. The survey asked participants about: program attendance, height, current weight and weight at the start and end of the program, behaviors adopted and continued as a result of the program, changes in medications for conditions associated with overweight and obesity and general comments about the program. The survey remained active for two weeks. Participants received reminder e-mails one week after they received the survey and two days before the survey closed. No incentive was provided for completing the survey.
Participants (n=1,450) received a follow-up survey between October 2013 and July 2014; 461 (31.8%) responded. Respondents who gained weight during the program were not considered to have achieved positive program outcomes and therefore were excluded from the study sample. Respondents who did not complete the program (attended fewer than 10 of the 15 program classes) or had missing weight values were also excluded, resulting in a final study sample of 286. The North Carolina State University Institutional Review Board approved the study
Responses to questions about behaviors adopted and continued as a result of ESMMWL were analyzed, as well as weight at the time of survey completion and at the start and end of the program. Those questions were asked as follows:
Participants’ weights at the start of the program (W1), at the end of the program (W2) and six months after the program (W3) were used to create three outcome subgroups:
These subgroups are indicators of participant maintenance of positive program outcomes. Indicator rigor increases in the order presented above.

Table 1: Descriptive statistics for weight loss maintenance study sample.
Univariate analysis consisted of descriptive and summary statistics including: the percentage of the study sample that met inclusion criteria for each outcome subgroup, the percentage of the study sample that reported adopting and continuing each weight management behavior, and means for respondents’ weights and BMIs at the start and end of the program, and at the time they completed the survey (Table 1). Bivariate analysis used chi-squared tests to determine associations between behaviors and outcome subgroups (Table 2). Associations between outcome subgroups and behaviors were considered significant if they had a p value of less than .05. Analyses were performed using Stata version 13.0 (StataCorp LP).
The following criteria were applied to the sample (n=286) to place respondents either in or out of three outcome subgroups:
Analyses identified behaviors that respondents, who met criteria for outcome subgroups, adopted at significantly higher rates than respondents in the respective comparison group.
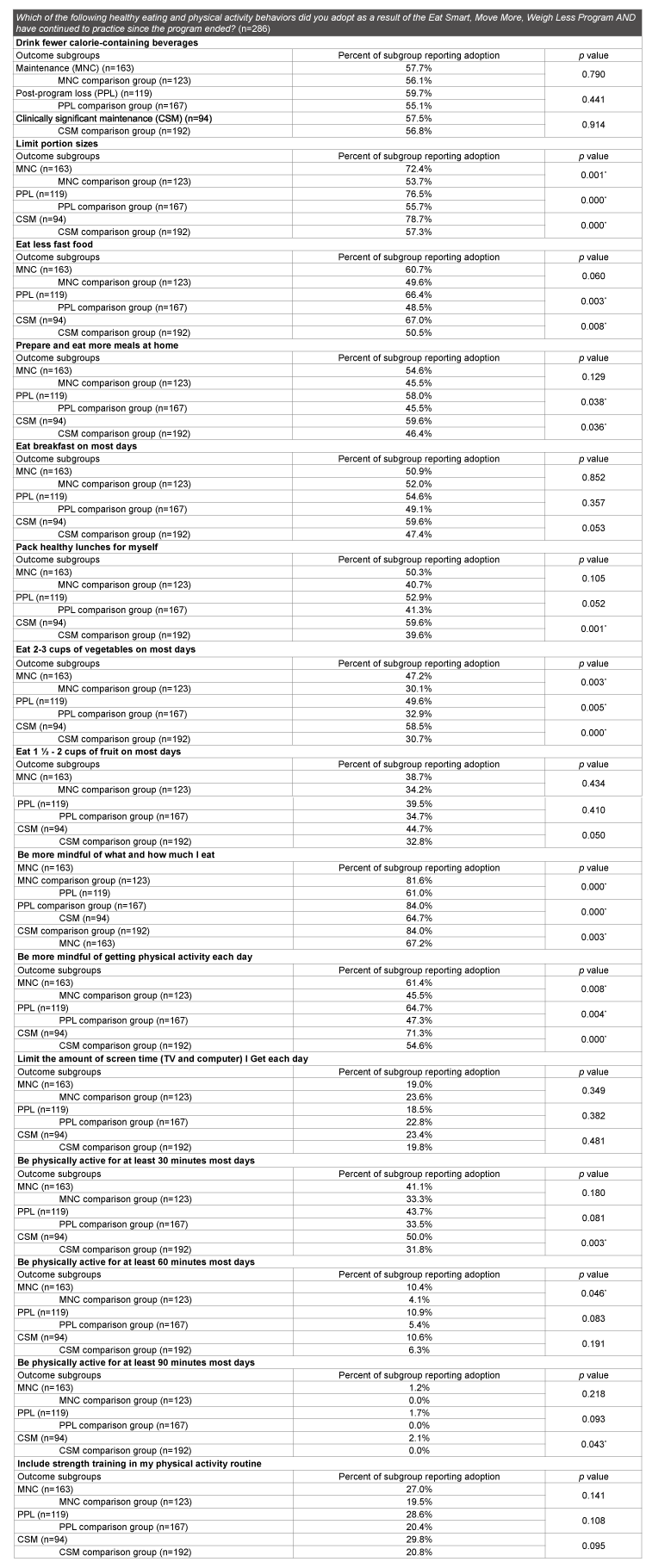
Table 2: Results of chi-squared tests to determine associations between outcome subgroups and behaviors reported.
*p value indicates statistical significance
“Being more mindful of what and how much I eat” was significantly associated with all outcome subgroups. Eighty-two percent of individuals that met MNC criteria reported adopting and continuing this behavior (compared to 61.0% of respondents that did not meet MNC criteria, p<0.001), as did 84.0% of PPL (compared to 64.7%, p<0.001) and 84.0% of CSM (compared to 67.2%, p=0.003). Table 1 presents the number of participants that fell in each outcome subgroup and the respective comparison group.
“Being more mindful of getting physical activity each day” was significantly associated with all outcome subgroups. Sixty-one percent of individuals that met MNC criteria reported adopting and continuing this behavior (compared to 45.5% of respondents that did not meet MNC criteria, p=0.008), as did 64.7% of PPL (compared to 47.3%, p=0.004), and 71.3% of CSM (compared to 54.6%, p<0.001).
Limiting portion sizes was significantly associated with all outcome subgroups. Seventy-two percent of individuals that met MNC criteria reported adopting and continuing to limit portion sizes as a result of the program (compared to 53.7% that did not meet MNC criteria, p=0.001), as did 76.5% of PPL (compared to 55.7%, p<0.001), and 78.7% of CSM (compared to 57.3%, p<0.001).
Preparing and eating more meals at home was reported at significantly higher rates by respondents meeting PPL (58.0% compared to 45.5%, p=0.038) and CSM criteria (59.6% compared to 46.4%, p=0.036). Another behavior related to planning and portion control, packing healthy lunches was reported at significantly higher rate in the CSM subgroup (59.6% compared to 39.6%, p=0.001).
Eating less fast food was reported at significantly higher rates by respondents meeting PPL (66.4% compared to 48.5%, p=0.003) and CSM criteria (67.0% compared to 50.5%, p=0.008). Eating 2-3 cups of vegetables on most days had significant associations with all outcome subgroups. Forty-seven percent of respondents that met criteria for the MNC subgroup reported eating 2-3 cups of vegetables on most days, while only 30.1% of respondents that did not meet MNC criteria reported vegetable consumption at this level (p=0.003). Findings were similar for PPL (49.6% compared to 32.9%, p=0.005), and CSM (58.5% compared to 30.7%, p<0.000). However, eating 1 ½ -2 cups of fruit on most days (MNC, p=0.434; PPL, p=0.410; CSM, p=0.050) and eating breakfast on most days (MNC, p=0.852; PPL, p=0.357; CSM, p=0.053) were not associated with any outcome subgroup.
CSM was associated with being physically active for at least 30 minutes (50.0% compared to 31.8%, p=0.003) and 90 minutes (2.1% compared to 0.0%, p=0.043) on most days. Physical activity for at least 60 minutes a day was reported at a significantly higher rate by respondents that met MNC criteria (10.4% compared to 4.1%, p=0.046). Including strength training in physical activity routines (MNC, p=0.141; PPL, p=0.108; CSM, p=0.095) and limiting screen time (MNC, p=0.349; PPL, p=0.382; CSM, p=0.481) were not associated with any outcome subgroup.
Analyses strongly suggest that being more mindful of what and how much one eats and of getting physical activity each day can support weight loss maintenance in the six months following a weight management intervention. Significant associations were found between all three outcome subgroups and the surveyed behaviors, “be more mindful of what and how much I eat” (MNC, p=0.000; PPL, p=0.000; CSM, p=0.003) and “be more mindful of getting physical activity each day” (MNC, p=0.008; PPL, p=0.004; CSM, p=0.000). These findings are consistent with existing evidence that weight loss maintenance is associated with the personal decision to lose weight and that weight management interventions should stress the importance of being more mindful [9-11].
Findings derived from questions on the follow-up survey about participants’ eating behaviors fell into three categories: portion control, eating healthier and time regularity in eating. Results strongly suggest that limiting portion sizes supports weight loss maintenance (MNC, p=0.001; PPL, p=0.000; CSM, p=0.000). Planning as it relates to decreasing portions, “portion distortion,” (the normalization of large serving sizes) and poor food choices may explain why preparing and eating more meals at home was reported at a significantly higher rate by respondents that met PPL (p=0.038) and CSM (p=0.036) criteria. Planning food choices can facilitate portion control and may decrease the potential to make poor food choices from easily available foods that are energy dense but nutrient poor (i.e. vending machines, office candy jars, and fast-food restaurants) [12]. Packing healthy lunches, a behavior that is also related to planning, was reported at a significantly higher rate by CSM respondents (p=0.001).
Eating less fast food was reported at a significantly higher rate by respondents that met PPL (p=0.003) and CSM (p=0.008) criteria. Results in this area resemble those from another study which found that weight decrease was significant at six-month follow-up when there was a 20% decrease in junk foods [2]. Eating 2-3 cups of vegetables on most days was reported at significantly higher rate by respondents in all outcome subgroups (MNC, p=0.003; PPL, p=0.005; CSM, p=0.000).
However, analyses did not find associations between some eating behaviors, generally regarded as healthy, and the outcome subgroups. For example, eating 1 ½ -2 cups of fruit on most days was not reported at a significantly higher rate by any outcome subgroup, confirming recent literature that has not found associations between fruit intake and body weight [13,14]. Rather than overall increases in fruit intake, further inquiry should address determinants related to fruit consumption such as energy density, energy content and preparation methods. While sufficient evidence exists for public health strategies that discourage consumption of sugary drinks as a part of a healthy lifestyle [15], “drinking fewer calorie-containing beverages” was not associated with any outcome subgroup. Eating breakfast on most days was not associated with any outcome subgroups.
Physical activity has previously been shown to correlate positively with sustained weight-loss [7-12,16]. The follow-up survey asked if, as a result of the program, respondents began and continued to be physical activity for at least 30, 60, and 90 minutes on most days, if they engaged in strength training and if they limited their screen time.
Respondents that met CSM criteria were significantly more likely to report being physically active for at least 30 minutes (p=0.003) and for at least 90 minutes on most days (p=0.043). Additionally, respondents that met MNC criteria were significantly more likely to report being physically active for at least 60 minutes on most days (p=0.046). The fact that all the three durations of daily physical activity asked about were only significantly associated with one outcome subgroup suggests that analyses were inconclusive regarding this relationship. Moreover, relatively few respondents reported adoption of physical activity compared to other surveyed behaviors. Thirty-eight percent (n=108) of the study sample reported being physically active for 30 minutes, 7.7% (n=22) reported 60 minutes and only 0.7% (n=2) reported engaging in 90 minutes on most days. However, as covered above, being mindful of getting daily physical activity was reported at a significantly higher rate in all outcome subgroups. These analyses will be run again after more participants respond to the follow-up survey. Eventually, there will be sufficient adoption reported on this question-set, both overall and within outcome subgroups, to draw more conclusive findings.
No association was found between the adoption of strength training and any outcome subgroup (MNC, p=0.141; PPL, p=0.108; CSM, p=0.095). Previous literature has found that strength training in combination with dietary energy restriction may be beneficial for weight loss maintenance [17]. No timeline was specified for the aforementioned findings, however, so it is possible that a follow-up period longer than six months may be necessary to observe the relationship between strength training and weight loss maintenance. Limiting screen time also was not associated with any outcome subgroup.
Overweight and obesity put millions of Americans at increased risk for multiple chronic diseases and cost the country billions of dollars in healthcare and lost productivity [18]. The literature suggests that only about 20% of individuals who lose weight will succeed in keeping it off [19]. Public health strategies that promote behaviors known to support weight loss maintenance could help increase that 20% and, in turn, contribute to efforts to reduce obesity at the population-level. Study findings identify behaviors that can be fostered to address overweight and obesity. The identified mindfulness and healthy eating behaviors should be reemphasized towards the end of a weight management curriculum to make participants aware of factors that will contribute to their sustained success. While these findings are for a real time, online intervention, the behaviors the study identifies as being related to weight maintenance may have application to other weight loss interventions or self-directed weight management.
Collecting respondents’ weight data through physical examination instead of self-report might solidify these findings. However, there was no incentive for participants to report erroneous weight measures. Moreover, principal measures employed weight as a continuous variable in order to examine weight change over time, the suggested practice for minimizing issues typically associated with self-report [20].
Elements of the follow-up survey data, including participants’ weights at the beginning and end of the program, were reported retrospectively. While limited bias has been observed in retrospectively reported weight data, the associated recall period was much longer than in this study; 10 years compared to six months [21]. Additionally, there is reason to believe that the weight data reported retrospectively in the follow-up survey would be remembered. These weights represent the beginning and end of, and progress made during, a program that respondents made a significant investment to complete.
Collecting responses to the same questions at 12, 18, 24 months or even further would enable analyses to observe the effect of time on; 1) relationships between behaviors and maintenance, and 2) participants’ adherence to specific weight management behaviors. The study’s strong findings related to mindfulness suggest additional questions that could be asked about the relationship between mindfulness and weight loss maintenance. Monitoring food consumption and weight, including weighing in more than once per week, has been demonstrated to be a successful strategy for ongoing weight loss [22]. Monitoring makes individuals working to maintain their weight more mindful of decisions regarding food selection and other weight-related behaviors [9]. Adding questions about monitoring to the follow-up survey will enable the analysis of relationships between the adoption of tracking behaviors and weight loss maintenance, as well as how frequently participants have to engage in tracking behaviors (dose-response) for them to be impactful. Another potential area of inquiry is how mindfulness can be effectively fostered through community-level obesity prevention strategies. Examples of related findings to-date include, menu-labeling policies can affect peoples’ choices when ordering at restaurants and signs placed near stairwells, elevators and escalators increase stair use by reminding individuals about opportunities for physical activity [23,24]. However, more study should be conducted to identify other community-level interventions that support behaviors associated with weight loss maintenance.
Based on this analysis, the behaviors most likely to support weight loss maintenance are: being more mindful of what and how much one eats; being mindful of getting physical activity; limiting portion sizes; and, eating 2-3 cups of vegetables on most days. At the individual level, these behaviors can be promoted to enhance the effectiveness of weight management programs. At the systems level, ways to foster these behaviors should be considered in the design of interventions intended to address obesity.
Financial support for the Eat Smart, Move More, Weigh Less program, where data for this study was collected, was provided by the North Carolina State Health Plan for Teachers and State Employees.
Download Provisional PDF Here
Article Type: Research Article
Citation: Thompson S, Dunn C, Aggarwal S, Tchwenko S, Wang A, et al. (2016) Behaviors Predictive of Weight Loss Maintenance: SixMonth Follow up of an Online Weight Management Program. Obes Open Access 2(3): doi http:// dx.doi.org/10.16966/2380-5528.124
Copyright: © 2016 Thompson S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access