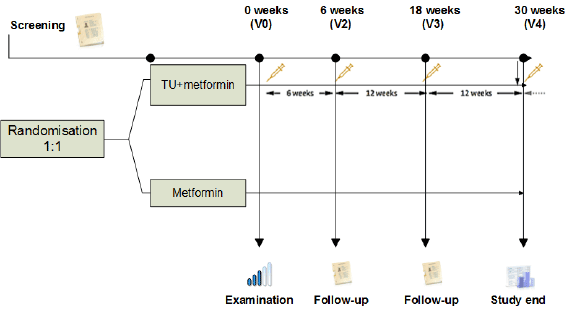
Figure 1: Trial design TU – testosterone undecanoate


Sergey V Nedogoda Irina N Barykina Alla S Salasyuk* Viktoria O Smirnova Viktoria J Khripaeva
Department of Therapy and Endocrinology FUV, Volgograd State Medical University, Russia*Corresponding author: Alla Salasyuk, Department of Therapy and Endocrinology FUV, Volgograd State Medical University, Russia, Tel: +79023803131; E-mail: solarheart7@gmail.com
Background and objectives: Metabolic syndrome (MS), characterized by central obesity, insulin resistance, dyslipidemia and hypertension is a well-known risk factor for the development of cardiovascular disorders. Globally, obese patients have a higher risk of morbidity and mortality, development of type 2 diabetes and cardiovascular disease. In addition, obesity leads to a decrease in serum testosterone and vice versa. We conducted randomized open-label trial, evaluating the effects of normalizing testosterone levels in obese hypogonadal men with metabolic syndrome.
Methods: It was a prospective, open-label, randomized, and parallel group study. 60 patients (mean age 45,3 ± 2,4 years ) with MS and total testosterone levels less than 12.0 nmol/L were enrolled and randomized 1:1 to receive testosterone undecanoate (TU) injections and metformin, or only metformin for 30 weeks. Lifestyle modification was recommended in both groups. The groups were well balanced at baseline. Primary endpoints were variations from baseline of cardiovascular (blood pressure (BP), arterial stiffness, endothelial function, carotid intima-media thickness) and body composition (body mass index (BMI), waist circumflex, percent of adipose tissue) parameters. Secondary endpoints were variations from baseline of hormonal (levels of total testosterone (TT), free testosterone (FT)) and metabolic (fasting glucose, lipids, uric acid) parameters.
Results: In our study, a continuous decline of body weight, body mass index and waist circumference was observed in combination therapy group. Triglyceride, total and LDL cholesterol levels, uric acid and C-peptide level were decreased, and HDL cholesterol level was increased (P<0.05 for all) in testosterone with metformin group more than in metformin only group at 30 weeks. The positive impact on the cardiovascular parameters (arterial stiffness, endothelial function, carotid intima-media thickness) revealed during the study was more pronounced in the combination treatment group. No significant changes in safety parameters were detected in both groups. No serious adverse event with causal relationship was reported during the study.
Conclusions: Study showed favorable effects of testosterone replacement in aging patients with low testosterone levels. TU effectively provides consistent TT concentrations within the normal range, improves cardio-metabolic and hormonal parameters, and has a positive impact on patient body weight, favorable safety profile and high level of patient tolerability.
Metabolic syndrome; Obesity; Male hypogonadism; Testosterone replacement therapy; Endothelial function; Insulin resistance; Testosterone
It is well known and documented that obesity may cause hypogonadism, and that hypogonadism may cause obesity. [1-4]
It has generated disputes about what condition comes first; obesity or hypogonadism? And what must be the first point of intervention? It was proved that obesity and hypogonadism create a self-perpetuating vicious cycle. After the vicious circle has been created, it does not matter where interfering. We can either treat obesity or hypogonadism first. The most important issue is to break the vicious circle as soon as possible, before it will be a threat to the health. Treating hypogonadism first may prove more effective in that it to a large extent “automatically” takes care of the excess body fat and metabolic derangements, and also confers psychological benefits that will help obese men become more physically active [4]. Thereby, restoring testosterone levels in hypogonadal obese men will relatively quickly break the self-perpetuating vicious circle, and transform it into a “health promoting circle.” Long-term testosterone replacement therapy in men with hypogonadism improves body composition, metabolic syndrome components and quality of life, and thereby can help break the vicious cycle [5].
In addition, large amounts of modern data accumulated over the last two decades has demonstrated that a low testosterone level is associated with increased risk of development of cardiovascular risk factors, atherosclerosis and mortality, and that testosterone therapy has beneficial effects on multiple risk factors and risk biomarkers related to these clinical conditions [6].
A plenty meta-analysis showed that weight loss (diet, physical exercise, bariatric surgery) reverts the obesity-associated hypogonadotropic hypogonadism [7]. Diet and exercise may have short-term beneficial effects on obesity, but, unfortunately, in the long term, most of the patients returned to the original weight [8]. In view of the serious negative effects of obesity on health, new approaches to managing obesity are needed [9]. Our study focused on the effects of normalizing serum testosterone in hypogonadal men with metabolic syndrome on body composition and cardiovascular risk factors.
We conducted an open-label, prospective, randomized, parallel group study. Patients included in the study in compliance with the rules of GCP (Good clinical practice), provided written informed consent and compliance with the inclusion criteria, as well as the absence of exclusion criteria.
The study included 60 patients with metabolic syndrome according IDF 2005 criteria, normo- or hypogonadotropic secondary hypogonadism (level of total testosterone <12 nmol/L on two early morning separate days (between 8:00 and 11:00 a.m.)) and arterial hypertension on stable antihypertensive therapy.
Patients were excluded if they were aged ≤ 18 years or had known hypersensitivity, intolerance or contraindications to study treatment; PSA level above 4 ng/ml, suspicion or known history of prostate cancer, breast cancer; primary hypogonadism, anti-androgens or glucocorticoids treatment; diseases that lead to a decrease in testosterone secretion (hypothyroidism, hyperprolactinemia, pituitary tumor); severe cardiovascular disease; renal or hepatic insufficiency; or a serious illness affecting their prognosis.
Concomitant medications (lipid-lowering therapies, antihypertensives) were continued if doses had remained stable for ≥ 3 months before randomization.
Primary endpoints were variations from baseline of cardiovascular (blood pressure (BP), arterial stiffness, endothelial function, carotid intima-media thickness) and body composition (body mass index (BMI), waist circumflex, percent of adipose tissue) parameters. Secondary endpoints were variations from baseline of hormonal (levels of total testosterone (TT), free testosterone (FT)) and metabolic (fasting glucose, lipids, uric acid) parameters.
Patients were randomly allocated into two groups:
Group 1 (mean age 45,1 ± 6,4 years) received testosterone undecanoate 1000 mg at baseline, after 6 and 18 weeks (Nebido, Bayer Pharma AG) and metformin 1000 mg BID for entire study period (Glucophage, Merck Sante).
Group 2 (average age 45,5 ± 2,4 years) received metformin 1000 mg BID for the entire study period (Glucophage, Merck Sante).
Lifestyle modification (diet, physical activity) was recommended in both groups. On the first visit for each patient was estimated the correct caloric intake and given instructions for count calories, and observance of the principles of a balanced diet for weight loss. Weight loss drugs were not allowed and were given recommendation to develop at least 150 min/ week of aerobic exercise of moderate intensity (50-70% of maximum heart rate) and/or at least 90 min / week of vigorous exercise (70% of maximum heart rate). Physical activity should have been distributed in at least 3 days/week, with no more than two consecutive days without activity.
The study design is shown in Figure 1.
Clinical and demographic characteristics of the groups were assessed at baseline. At baseline and every visit, the following options were assessed: general physical examination and anthropometric parameters, i.e., weight, height, body mass index (BMI), waist circumference, systolic and diastolic blood pressure, heart rate, blood samples. Pulse pressure was calculated by arithmetic difference between systolic and diastolic blood pressure. Hormonal assessment included total T and sex hormone binding globulin (SHBG) measured by immunochemiluminescence (Immulite 2000 Siemens). Blood sampling was carried out in the morning. Because testosterone secretion is pulsatile, to avoid false readings blood sampling was performed three times at intervals of 20 minutes, each sample was determined by the level of T, as the true considered the lowest level. The level and percent of free and bioavailable testosterone was determined by calculation using the Vermeulen equation (online calculator available at http://issam.ch/freetesto.htm).

Figure 1: Trial design TU – testosterone undecanoate
Fasting blood samples were collected for evaluation metabolic and safety parameters included plasma total cholesterol, HDL and triglycerides, PSA, blood glucose, hemoglobin and hematocrit, liver and kidney functions, serum bilirubin, serum transaminases, creatinine and uric acid according to previously published procedures [10]. C-peptide levels were measured using a C-peptide immunoluminometric assay. Percentage of adipose tissue was determined by bioimbedance method, using Omron BF306 device (OMRON Healthcare Inc., Lake Forest, IL, USA). An AlokaProsound L7 Premier device (Hitachi Aloka Medical Ltd., Tokyo, Japan) was used to determine intima/media thickness and flowdependent vasodilatation. Pulse wave velocity (PWV), augmentation index and central aortic BP were determined using a SphygmoCor device (AtCor Medical Pty Ltd., West Ryde, NSW, Australia).
Treatment tolerability was assessed at each follow-up visit.
Patients with the following clinical laboratory parameters were withdrawn either at baseline or during the course of study if hematocrit level ≥ 52%; PSA level increased >1.0 ng/mL above the baseline PSA if baseline PSA was <2.0 ng/mL; PSA level increase >50% of the baseline PSA if baseline PSA was >2.0 ng/mL.
Data are presented as means ± standard deviations or numbers and percentages. A paired student’s t test was used to detect significant changes with treatment; p<0.05 was considered statistically significant.
Continuous quantitative baseline and demographic features were tested using a simple t test on independent samples. A nonstandard distribution of values was analyzed using a Mann–Whitney test, while qualitative traits were assessed using a Fisher’s exact test or χ2 test, depending on the number of observations in each cell of the contingency table. Comparison of the intergroup effectiveness of various treatments was performed using Dunnett’s test, which assessed changes in the rate of improvement, compared with baseline, and standardized them (α=5%). Differences between measurements obtained after active treatment and the corresponding baseline values were expressed as means ± standard deviations and were compared through analysis of variance (ANOVA), with allowance for the treatment order and subject. If the p value associated with the main factor (treatment) fell below 0.05, single contrasts between the four treatments were tested with the Newman–Keuls test. p values <0.05 were considered statistically significant. Statistical processing was performed using BMDP statistics software (Statistical Solutions, Saugus, MA, USA).
The baseline characteristics of the patients are shown in Table 1. As can be seen from the data, the differences between the groups did not reach statistical significance, making the possibility of further comparison.
It should be noted, that in groups were no diabetic patients, but 5 patients in the testosterone\metformin group and 6 patients in metformin group by anamnesis had impaired fasting glucose, and 4 patients in each group had impaired glucose tolerance.
All 60 patients in both groups complete the study. Any serious side effects or intolerance to therapies that could require discontinuation of testosterone undecanoate is not registered during the study period.
The effects on anthropometric and metabolic parameters of different treatment options are presented in the Table 2.
There were significant decreases in weight, BMI, WC and WHR in the group receiving combination therapy of metformin and testosterone compared with the metformin group (Figure 2).
Pronounced and statistically significant reduction in waist circumference in the testosterone + metformin group demonstrates that the compensation of testosterone deficiency in patients with MS and androgen deficiency plays an important role in the correction of visceral obesity.
Furthermore, in the group treated with testosterone, the patients noticed a decrease in appetite and increased motivation to reduce weight and increase physical activity. Unfortunately, these data are based on spontaneous patient’s reporting; no questionnaires were used in this study to evaluate effect of treatment on this parameter. Further investigations are needed in this field to clarify the data.
In testosterone + metformin group dynamics of reducing the concentration of total cholesterol was 11,2% (p<0.05), the content of TG and LDL -13.07% to 12.00%, respectively (p<0.05). The impact of the combination of the state of lipid profile has done apparently, mainly due to the antiatherogenic actions of testosterone.
In the investigation of HDL level statistically significant changes were observed in the group of TU+ metformin, the dynamics of this parameter accounted 34,5% (p<0.05). The group of patients is statistically different between the level of HDL after treatment (p=0.02).
In our study, we examined the dynamics of Triglyceride/HDL Cholesterol Ratio, as one of the simplest markers of insulin resistance [11]. The dynamics of this indicator is reflected in the figure 3.
Reduction of C-peptide in both treatment groups was clinically apparent and statistically significant (p<0,05).
Assessing the impact on the level of uric acid was found significant differences. In the group testosterone + metformin showed a reduction of uric acid level of 18.3% (p>0,05). In Metformin group statistically significant changes is not revealed.
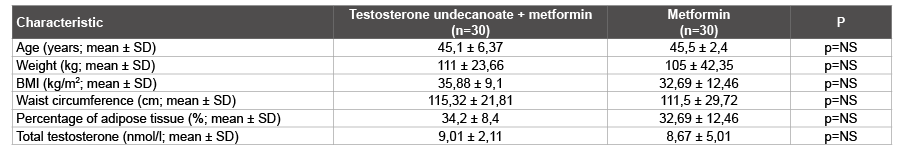
Table 1: Clinical and demographic characteristics of the study subjects
BMI: Body mass index
NS: Not significant
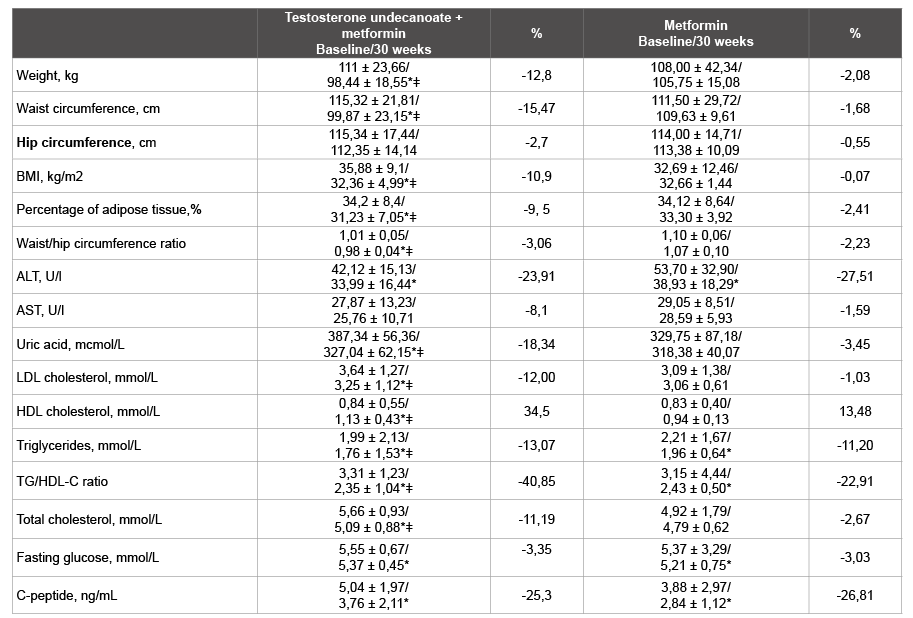
Table 2: Blood biochemistry and anthropometric parametersa
a All data are expressed as means ± SDs
SD, standard deviation;BMI, body mass index; ALT, Alanine aminotransferase; AST, Aspartate aminotransferase; TG/HDL-C, Triglyceride/HDL Cholesterol Ratio;HDL, high-density lipoprotein;TG,triglycerides;
*p<0.05 versus baseline
ǂ p<0.05 differences between groups
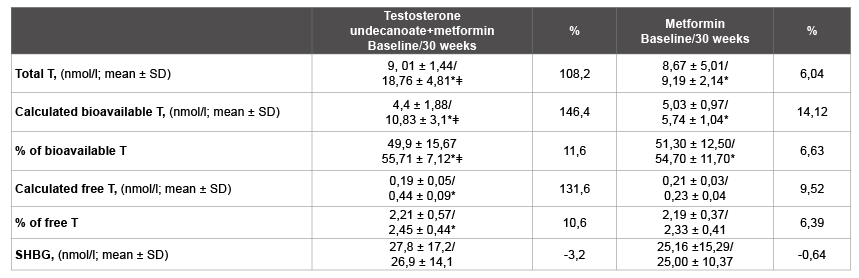
Table 3: Androgen metabolism parametersa
a All data are expressed as means ± SDs
T, testosterone; SHBG, sex hormone-binding globulin; SD standard deviation
*p<0.05 versus baseline
ǂ p<0.05 differences between groups
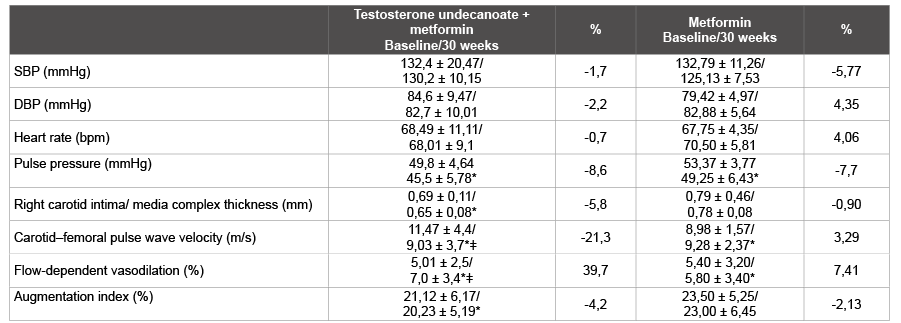
Table 4: Changes in systolic and diastolic blood pressure, heart rate and vascular structure parametersa
a All data are expressed as means ± SDs
bpm beats/minute, DBP diastolic blood pressure, SBP systolic blood pressure, SD standard deviation
*p<0.05 versus baseline
ǂp<0.05 differences between groups
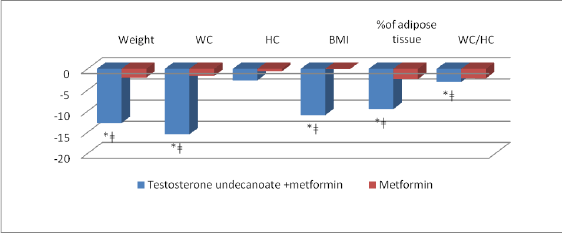
Figure 2: The dynamics of weight, BMI, WC, HC and WHR *p<0.05 versus baseline ǂp<0.05 differences between groups
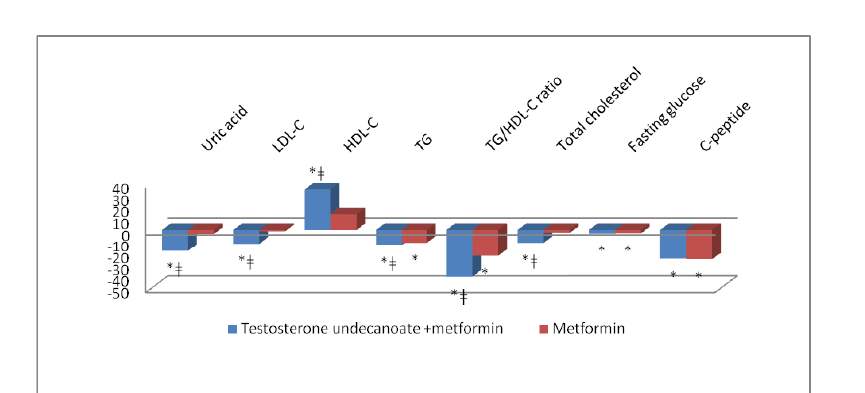
Figure 3: The dynamics of the metabolic parameters *p<0.05 versus baseline ǂp<0.05 differences between groupsa
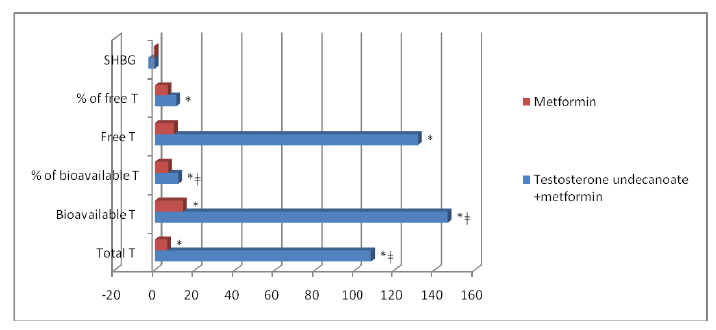
Figure 4: The dynamics of androgen metabolism parameters *p<0.05 versus baseline ǂp<0.05 differences between groups
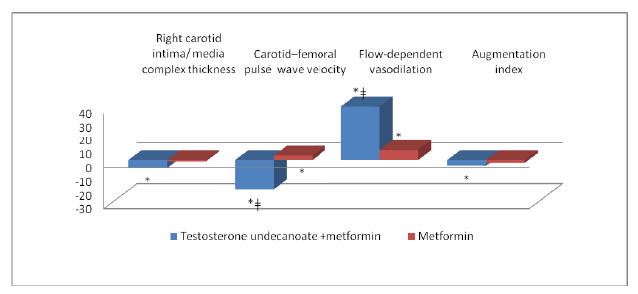
Figure 5: Changes in vascular structure after 30 weeks of treatment, %. *p<0.05 versus baseline ǂp<0.05 differences between groups
In both clinical groups statistically significant, but clinically unexpressed decrease of fasting glucose levels was observed (p<0.05).
The therapy in all patients of group testosterone + metformin normalized values of total and bioavailable testosterone (p<0,05 for both), respectively. Patients in metformin group also recorded small, but statistical significant increases in the total and bioavailable testosterone, which is associated with a change in androgen metabolism while reducing weight of visceral fat during metformin therapy (Table 3).
Results confirm the effectiveness of testosterone undecanoate in compensation androgen deficiency and suggest adequate dose of therapy (Figure 4).
Changes of systolic and diastolic blood pressure, heart rate and vascular structure parameters are presented in the Table 4.
Vascular structure parameters improved significantly with testosterone +metformin (Figure 5). It is shown that combination therapy with testosterone drugs to a greater extent than traditional therapy, helped to improve the vascular elasticity, which showed a decrease in carotidfemoral PWV in the relevant mode of therapy. Augmentation index and IMT was significantly improved only in the treatment of testosterone + metformin.
Pulse pressure, which reflects arterial stiffness and has been suggested to be an independent cardiovascular risk factor, decrease in both groups with no significant intergroup differences.
In testosterone + metformin group flow-dependent vasodilation was significantly improved after a month of therapy, and has shown a permanent positive trend (39.7% at 30 weeks, p<0.05). Patients on metformin monotherapy also had a slight, but statistically significant improvement in endothelial function in the brachial artery after 30 weeks of starting treatment -7.4% (p<0.05).
Levels of Hemoglobin (mg/dL) and hematocrit (%) rose significantly, but values did not exceed the upper limit of the reference range during period of observation. Increasing hematocrit above 54%, which would require discontinuation of testosterone undecanoate, was not observed in any patient. In both groups values of PSA did not rise significantly.
We obtained data supporting the efficacy and safety of androgen therapy in patients with MS and androgen deficiency. Although differing views about the necessity, effectiveness and duration of androgen therapy, the results of most recent studies coincide with ours, and show a positive effect of testosterone therapy on all components of MS [5,12].
Compensation of androgen deficiency causes a decrease in a key component of MS - abdominal obesity, which is proven reduces the risk of cardiovascular morbidity and mortality in MS [9,13,14,15].
In our study a continuous decline of body weight, body mass index and waist circumference was observed. Fasting glucose, serum total cholesterol, LDL cholesterol and triglycerides declined significantly during testosterone therapy. HDL increased slightly but significantly.
Marked decrease of Triglyceride/HDL Cholesterol Ratio in the group receiving combination therapy with testosterone, compared with monotherapy with metformin, suggests a pathogenetic substantiation of the combined therapy in terms of impact on the basic mechanism of onset and progression of MS – insulin resistance [11]. Effect of therapy on the C-peptide level supports previous conclusions about the positive impact of androgen therapy and metformin to reduce insulin resistance in patients with MS.
The results of our study are in agreement with earlier studies confirming a positive effect of normalizing serum testosterone on variables of the metabolic syndrome [10,16,17].
The administered therapy resulted in a reduction or normalization of serum aminotransferase levels, comparable in both groups observation. On this basis, we can conclude an independent effect of metformin on this indicator, which is confirmed by data from studies conducted before [18]. So, metformin can be considered as a method of prevention and treatment of NAFLD in MS.
Also in the group of patients undergoing androgen therapy has been revealed a significant decrease in the level of uric acid. In recent studies showed, that androgen deficiency can be a trigger for the development of hyperuricemia [19]. This suggests that one way of correcting hyperuricemia in MS may be androgen replacement, which is expected to result in a partial normalization of uric acid levels. It is important because proven that the high level of uric acid is an independent significant risk factor for developing cardiovascular complications [20].
We obtained results demonstrating that the combination therapy with testosterone more so than conventional therapy, substantiated from the point of correction of vascular stiffness, which showed a decrease in carotidfemoral PWV in the relevant mode of therapy. Positive improvements were found in pulse pressure levels also. In earlier studies was shown, that PP strongly associated with androgen deficiency [21]. So, correction of testosterone level and metformin supplementation may affect on this parameter via decrease of insulin resistance. Insulin, at physiological concentrations in healthy subjects, has acute vasodilatory effects that lead to increased arterial distensibility. Furthermore, testosterone exerts a favorable effect upon vascular reactivity, inflammation, cytokine production, adhesion molecule expression, as well as on serum lipid concentration and hemostatic factors, suggesting a protective role against the vascular changes.
Augmentation index and carotid intima-media thickness was significantly improved only in the treatment of testosterone and metformin. This is consistent with previous studies, which had examined the association between endogenous testosterone levels and carotid intima-media thickness (CIMT), a surrogate measure of atherosclerosis. All studies documented an inverse relationship of CIMT with total testosterone, free testosterone, or bioavailable testosterone, meaning that higher testosterone levels are associated with lower CIMT (i.e. less atherosclerosis) [22-31]. It is notable that no study has reported a significant relationship between higher testosterone levels and increased carotid intima-media thickness.
Furthermore patients showed significant improvement in endothelial function. In combination therapy group percent increase in flowdepended vasodilatation of the brachial artery was significantly improved after a month of therapy, and displays a constant positive trend. Patients on metformin monotherapy also had a statistically significant improvement of endothelial function in the brachial artery, but the extent of improvement was clinically pronounced a little. This indirectly confirms the previously obtained data about vasodilating properties of androgen therapy [32].
It should be noted that all the patients in the observation group were initially marked by low levels of post compression changes in brachial artery diameter compared with reference values. This indicates systemic violations of endothelial function in MS.
Since based current knowledge improvement in the elastic properties of the main arteries and normalization of endothelial function - the main target of medical intervention in patients with high cardiovascular risk, the positive effect of androgen replacement therapy on these parameters is another argument for early start of androgen therapy in men with MS.
It is well known that overweight and obese men with metabolic syndrome at baseline have higher risks to regain weight (odds ratio=2.8, p=0.015) after initial weight loss [33].
To our knowledge, it is the first study to compare traditional therapy of MS with metformin and combining metformin and testosterone therapy.
Combination therapy with metformin and testosterone allowed to potentiate the effect of these drugs on patients anthropometric, metabolic and cardiovascular characteristics. The synergism actions of components expressed in a more intensive weight loss, rather than by simple summation of the potential effects of the individual drugs.
It is of utmost interest that in contrast to the U-shaped curve for weight loss seen with traditional obesity treatments, which are characterized by weight loss and weight regain, treatment with testosterone replacement therapy results in a continuous reduction in obesity parameters (waist circumference, weight and BMI) for >5 years, or until metabolic abnormalities return to healthy ranges [5,33-36].
So this mode of therapy may be considered reasonable in the pathogenetic therapy of patients with MS. It should be underscored that the contribution of testosterone replacement therapy to combating obesity remains largely unknown to medical professionals [24]. It is therefore important to highlight the promising research on the anti-obesity effects of testosterone replacement therapy and help implement its research findings into clinical practice, for the benefit of a growing population of suffering hypogonadal obese men.
It should be noted some study limitations, which potentially could affect the results. The study was not placebo-controlled, the number of subjects was relatively small, and that the duration was short. However at the moment we continue to monitoring the group of patients treated with testosterone, to assess the long-term results of therapy. Another study limitation is represented by the impossibility to ascertain patient’s adherence to diet and physical activity plan throughout the study period. We had prescribed life style changes on first visit, and checked results obtained by interview ingeach patient at different time points of the study.
In conclusion, study showed favorable effects of testosterone replacement in patients with low testosterone levels and metabolic syndrome. TU effectively provides consistent TT concentrations within the normal range, improves cardio-metabolic and hormonal parameters, and has a positive impact on body weight, a favorable safety profile and high level of patient tolerability.
Testosterone replacement therapy has been proposed to be a new potential obesity treatment modality in hypogonadal men with excessive body fat mass and metabolic derangements. Further observation for patients participating in the study will more accurately ascertain specific points of application of this therapy.
No funding was provided for this study. Authors have no conflicts of interest to declare. The authors have no other relevant affiliations or financial involvement with any organization or entity in conflict with the subject matter or materials discussed in the manuscript, apart from those disclosed.
Download Provisional PDF Here
Aritcle Type: Research article
Citation: Nedogoda SV, Barykina IN, Salasyuk AS, Smirnova VO, Khripaeva VJ (2015) Effects of Testosterone Replacement Therapy on Cardio-Metabolic, Hormonal and Anthropometric Parameters in Obese Hypogonadal Men with Metabolic Syndrome. Obes Open Access 1(2): doi http://dx.doi. org/10.16966/2380-5528.108
Copyright: © 2015 Nedogoda SV, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access