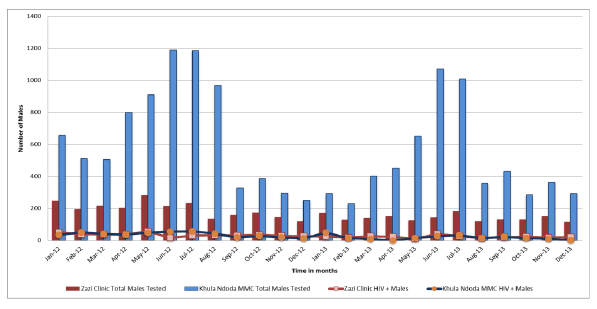
Figure 1: Total males tested vs HIV-positive males at Zazi HCT clinic and KhulaNdoda VMMC clinic

Lebina L1* Milovanovic M1 Essien T1 Martinson N1,2
1Perinatal and HIV Research Unit, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, South Africa*Corresponding author: Dr. Limakatso Lebina, Perinatal and HIV Research Unit, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, PO Box 114, Diepkloof 1864, South Africa, E-mail: limakatsol@phru.co.za
Background: Early detection of HIV status is an important step in ensuring that HIV-infected individuals receive appropriate care and treatment. HIV testing and counselling (HCT) sites at clinics, the workplace, and campaigns are often the primary channel for HIV testing. Circumcision clinics also provide testing and counselling services to large numbers of men of all ages requesting voluntary medical male circumcision (VMMC). The objective of this study was to report HIV positivity in people testing at a stand-alone HCT clinic and a VMMC clinic.
Method: A retrospective data review done over two years across two clinics at the Chris Hani Baragwanath Academic Hospital in Soweto: KhulaNdoda a voluntary medical male circumcision clinic and Zazi HCT clinic. Both sites offer a walk-in, free-of-charge HIV testing and counselling service. The results of all men over the age of 10 years, who attended either of the clinics and were HIV-tested, are included in this paper.
Results: A total of 17,761 (13,801 VMMC clinic and 3,960 HCT clinic) males were tested. At the VMMC clinic all the people tested were males while the HCT clinic tested 45% (3960/8736) males and 55% (4,776/8,736) females. Overall 7.8% (CI: 7.4-8.2%; 1,385/17,761) of the males tested were newly diagnosed with HIV across both sites: 4.8% (CI: 4.4-5.2%; 670/13,801) at the VMMC clinic and 18% (CI: 16.8-19.2%;715/3,960) at HCT clinic (p<0.05). Among the females that tested at the HCT clinic 29.8% (CI: 28.5-31.1%; 1423/4776) were newly diagnosed with HIV. The overall (both males and females) HIV positivity at the HCT clinic was 24.5% (CI: 23.6-25.4%; 2138/8736).
Conclusion: HCT and circumcision sites detect similar numbers but different HIV positivity. Circumcision programs provide an additional platform for young males, who might not go to a HCT clinic to know their HIV status and thus access care and treatment of HIV positive.
HIV; Circumcision; HCT; HIV testing
The HIV prevalence in South Africa is 12.2% according to the latest National Survey [1] however it varies by age with the most affected age group being 15-49 years (19%) [1]. Although there is a slight decrease in HIV incidence, the numbers are still concurringly high with 370000 new infections recorded in 2012 [2]. HIV Counselling and Testing (HCT) has been scaled-up and provided across various settings (healthcare facilities, mobile sites, workplaces and traditional healers) in order to increase the number of people who know their status and access appropriate care [1]. Between 2010 and 2012, 3.7 million people in South Africa had tested for HIV [1].
Voluntary Medical Male Circumcision (VMMC) was shown to reduce the risk of acquiring HIV in heterosexual males by 60% [3-5] and has been recommended by the World Health Organisation to be integrated into the biomedical HIV prevention interventions in 14 Eastern and Southern African countries [6]. As part of South African government’s strategies to curb the HIV epidemic VMMC services were scaled-up resulting in 1.8 million (43% of target) men have been circumcised in South Africa over a 6 year period [7]. Part of the VMMC programme is that all men must know their HIV status and receive HIV risk reduction counselling prior to the circumcision procedure [6]. Household members survey in four provinces in South Africa showed that among the youth (18-24 years), only 52.2% had ever tested for HIV, and of those tested, 39.9% were males and 60.1% females [8]. Some of the barriers for HIV testing include: fear of knowing and living with an HIV-positive status, stigma and discrimination. Some of the approaches that have been recommended by the WHO to increase uptake of HIV testing (especially in adolescents) include: provider initiated testing and counselling (PICT) and community based HCT [9]. Late HCT delays diagnosis and entry into care and treatment, therefore every prospect to increase HCT should be evaluated. Therefore, it is important to review and report on HIV positivity among people testing in a standalone HCT site and a VMMC clinic.
A retrospective data review was conducted using routinely collected data over two years (2012-2013) across two clinics at the Chris Hani Baragwanath Academic Hospital (CHBAH) in Soweto.
Khula Ndoda is a voluntary medical male circumcision site and Zazi HCT clinic is at the CHBAH. According to the most recent Census of South Africa [10] there are approximately 1 272 000 people living in Soweto of whom 49.6% are men. Khula Ndoda is a high volume Male Circumcision clinic opened in December 2010, and by end December 2014 it had completed 32962 circumcisions. Khula Ndoda provides free VMMC services to males >10 years of age as well as HIV counselling and testing and symptomatic TB screening. The WHO has recommended that an increase of VMMC services be offered to men who are about to be or are already sexually active [7]. In winter the demand for circumcision services is very high with an average of 1500 men requesting VMMC while in summer the demand is less with approximately 600 VMMC performed. Zazi HCT clinic was started in November 2008 and provides comprehensive and free of charge HIV HCT services such as good quality pre-test and post-counselling and testing for all age groups and genders. Zazi clinic is a walk in facility, no scheduling is necessary. Clients that test HIV-positive at the two clinics are offered a CD4 count test and referred for care. Both clinics use a single rapid HIV test with a confirmatory sequential test for reactive or difficult to interpret results. All tests are provided by the Department of Health and vary depending on stock availability. The main difference between the two sites is that one offers VMMC services, but HIV testing, TB screening, CD4 count testing and referrals were done according to similar protocols at both sites. Furthermore, in both clinics basic health screening of diabetes, hypertension and anaemia are also provided.
HIV testing services are provided by trained counsellors and are supervised by social workers (counselling aspects) and professional nurses (HIV testing). The VMMC and HCT clinics do not provide any treatment, clients with newly diagnosed medical conditions are referred for further treatment and care in other facilities. The National Health Laboratory Services (NHLS) provides quality assurance monitoring of HIV testing for both clinics by verifying the test kits and test kit storage.
We chose to review data from two (2012 and 2013) years during which time the two clinics were fully functional and under the same management team. All participants at the HCT clinic (irrespective of age) that received HCT services during this time period were considered eligible for inclusion in the review. Participants at the VMMC clinic who were ≥ 10 years old and received VMMC and HCT services were considered eligible. The data was collected from routinely submitted monthly reports for program monitoring and evaluation. The routinely collected data included: number of HIV tests performed, number of HIV positive and negative cases across various age categories.
This study used aggregated, routinely collected data with no individual level data; therefore ethics approval was not required for this analysis.
The continuous variables in the data were analysed descriptively to determine the medians and interquartile ranges. Chi-squared tests were used to compare proportions. A significance level of 5% was used in the analysis. Analyses were done using Statistical Analysis software version 9.2 (SAS Institute, Inc. Cary NC).
From January 2012 to December 2013 a total of 22,537 (13,801 at VMMC clinic and 8,736 at HCT clinic) people were tested for HIV at the two clinics (Table 1). All the people tested at the VMMC clinic were males while the HCT clinic tested 45% (3,960/8,736) males and 55% (4,776/8,736) females. Overall 7.8% (CI: 7.4-8.2%; 1,385/17,761) of the males tested were newly diagnosed with HIV across both sites: 4.8% (CI: 4.4-5.2%; 670/13,801) at the VMMC clinic and 18% (CI: 16.8- 19.2%;715/3,960) at the HCT clinic (p<0.05). Among the females that tested at the HCT clinic, 29.8% (CI: 28.5-31.1%; 1423/4776) were newly diagnosed with HIV. The overall (both males and females) HIV positivity at the HCT clinic was 24.5% (CI: 23.6-25.4%; 2,138/8,736).
At the VMMC clinic 81% (542/670) and at the HCT clinic 86% (614/715) of males testing HIV-positive were between the ages 25-49 years. Among these HIV-positive males, 4% (27/670) at the VMMC clinic and 3.4% (24/715) at the HCT clinic were between the ages of 15-19 years.
At the VMMC clinic, an average of 575 circumcision were done per month over the two year period however, there was seasonal variability in June-July (winter months) related to circumcision services demand. For example, in June-July 2012 and 2013 a total of 2,372 and 2,079 HIV tests were performed respectively compared to November-December 2012 and 2013 (541 and 656 respectively) (Figure 1). On average, a total of 364 HIV tests (165 males and 199 females), were performed on a monthly basis at the HCT clinic (Figure 1).

Figure 1: Total males tested vs HIV-positive males at Zazi HCT clinic and KhulaNdoda VMMC clinic
This routinely collected data review shows that: more males are tested through the circumcision programme compared to the HCT clinic and the overall proportion of HIV-positive males is higher in the HCT clinic. Circumcision programmes provide an additional setting through which to reach a large number of men and youth. The uptake of HCT services and transmission into HIV treatment is still low despite improvements in HIV treatment and prognosis [1,9]. Women (71.9%) and adults aged 25-49 (78.2%) are more likely to test compared to men (59%) and youth aged 15-24 (50.5%) according to the most recent HIV survey in South Africa [1]. One of the influencing factors of whether or not people seek HIV testing and treatment is fear of stigma [11]. Although much has been done to create awareness and promote acceptance of people living with HIV, stigma in families and communities, continues to be observed [11]. The advantage of receiving a free medical male circumcision might appeal to the youth and men who want to reduce their risk of contracting HIV as previous research has shown, circumcision decreases the risk of HIV infection acquisition in men [3]. In a study on acceptability of VMMC devices most men who request circumcision indicated that they chose VMMC because it is safe, clean, and healthy and will prevent them from getting diseases (Unpublished Observation).
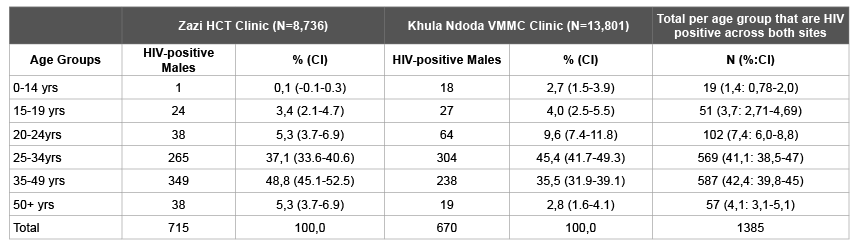
Table 1: Newly diagnosed males with HIV per age category at a VMMC and an HCT clinic
Retrospective review of routinely collected data for reporting, with no individual data making the analysis limited the study to only a few variables. Another limitation is that there was no record of referrals between the two sites and that we did not follow-up participants to assess linkage to care.
In conclusion, our data review highlights that HCT and circumcision sites detect similar numbers but different HIV positivity with more men accessing HCT services through circumcision sites. Circumcision programs provide an additional platform for young males, who might not go to a HCT clinic to know their HIV status. Scale-up of VMMC programmes will increase the number of men who know their HIV status and are accessing appropriate treatment.
The staff members at the two clinics who assisted with data collection and all the clinic clients whose information were used in this data review.
All authors declare no conflict of interest.
Download Provisional PDF Here
Article Type: Research Article
Citation: Lebina L, Milovanovic M, Essien T, Martinson N (2016) Circumcision Programmes as a Platform for HIV Testing. J HIV AIDS 2(1): doi http://dx.doi.org/10.16966/2380-5536.116
Copyright: © 2016 Lebina L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access