
Figure 1: CT scan without injection of contrast product shows the lesion (the right temporo-polar hypodensity is badly limited and is encircled by an oedema in shape of thimble.

Sondo KA1* Zabsonré DS2 Diallo I3 Bambara TA4 Ouédraogo SM5 Ouédraogo GA1 Kyélem C5 Yaméogo NV6 Ouédraogo A7 Lamien A7 Drabo YJ3
1Department of Infectious Diseases, University Hospital Yalgado Ouédraogo, Ouagadougou, Burkina Faso*Corresponding author: Apoline K Sondo, Department of Infectious Diseases, University Hospital Yalgado Ouédraogo, 01BP 815 Ouagadougou 01 Burkina Faso, Tel: 0022670077198; E-mail: sondoapoline@Yahoo.fr
Introduction: During HIV infection, immunity deficiency promotes the development of some tumors such as glioblastomas witch are central nervous system malignant tumors with a high astrocytary differentiation. Their prognosis is poor with an average survival ranged between 12 and 15 months.
Objective: To report a case of glioblastoma in an HIV infected patient with more than 24 months of survival.
Methodology: We achieved a document review of patient that is followed up in our department for HIV infection and who developed a glioblastoma.
Case: A 41 year-old HIV1 infected black man, treated presented some encephalic signs (headaches, mental confusion, nauseas and vomiting) without neurological localization. He was treated by the highly active antiretroviral therapy (HAART) two years ago, and had an immunovirological success six months after the beginning of the HAART. CD4 rate was 315 cells/mm3 with undetectable viral load. Cerebral CT scan founded a right temporo-polar expensive process and right cerebral parenchyma edema. The anatomo-pathological examination of the tumor biopsy concluded of glioblastoma. The surgical tumorectomy associated with chemotherapy and radiotherapy has been realized. Result is excellent because thirty months after the diagnosis, the patient is still alive with good clinical presentation (normal clinical examination) and normal CT scan control.
Conclusion: Glioblastoma should be suspected in HIV infected people with neurological signs even if they are minimal; because with an early diagnosis and an adequate treatment, it is possible to increase the survival, despite the high malignancy of the glioblastoma. In Burkina Faso, the imagery should be accessible and available to the population and the medical and technical equipments should be reinforced.
Glioblastoma; HIV1; Early diagnosis; Good prognosis; Burkina Faso
Antiretroviral therapy of the people infected by Human Immunodeficiency Virus (HIV) increased their survival. One of the consequences of this situation is the incidence of some cancers. According to a study undertaken in Great Britain, 40% of the patients at acquired immunodeficiency Syndrome (AIDS) stage, contract a cancer at the advanced level of their disease [1]. Gliomas are the most frequent forms of brain primitive tumors and the glioblastoma which is a high rank tumor is the most malignant form of these tumors [2]. The incidence of glioblastomas in France is estimated at 2,000 new cases per year [3]. In Africa and particularly in Democratic Republic of Congo, this affection reaches 41% of the cerebral tumors [4]. In Burkina Faso, according to Lompo-Goumbri et al. [5], the glioblastoma is probably under diagnosed, because it represents 0.02% of the histologically confirmed cancers, from 1986 to 2006. The means of diagnosis are neither available, nor always easily accessible for the population. The initial examination is based on the imagery and the confirmation, on the histological examination of the tumor sample [6]. Significant scientific progress on gliomas and their treatment improved the patient’s survival: thus the tumor resection is supplemented by the combination of concomitant and complementary radiotherapy and chemotherapy (through the temozolomide) [7,8]. But this treatment is palliative and the fatal evolution in a short term is foreseeable with many relapses. Indeed, glioblastomas have bad prognosis with average survival varying between 12 and 15 months [3]. The combination of glioblastoma –HIV infection is rare, apart from some cases reported in the developed countries, where the authors report some delays in diagnosis, associated with a raised mortality; even in these developed countries, the diagnosis is made in post-mortem [9-15]. Hall et al. [13] had inventoried 21 cases of glioblastomas in HIV infected people between 1987 and 2009; he did a research on PUBMED about the issue, and in this study 3 cases over 4 mentioned between 2005 and 2007 died; more often, the diagnosis is made in post-mortem [11,13,16]. We report the case of an HIV-1 infected patient whose survival is more than two years after the diagnosis of a glioblastoma.
An HIV-1 infected 41 year-old black man on antiretroviral therapy (ART) since July 2011, without associated medical antecedents was admitted. At the beginning of ART, CD4 rate was 144 cells per milliliter, and viral load at 2.388 copies per millimeter (3.38 log). Six months after ART beginning, viral load was undetectable and CD4 rate at 493 cells/ml. In March 2013 (18 months after ART beginning), the patient presented some encephalic signs (such as intense headaches, a mental confusion, nauseas and vomitings), without any sign of neurological localization, nor fever. The physical examination was normal. The immunological and virological assessment carried out showed an always undetectable viral load but a reduction in CD4 rate (315 cells/ml) despite a well therapeutic observance. The cerebral CT scan showed a right temporo-parietal cerebral abscess and a right parenchyma edema. The patient has chosen to go to another country for his treatment where the cerebral CT scan showed a right temporo-polar expansive process which occupies the entire temporal pit, with a peri-lesional edema and mass effect on median structures (Figures 1 and 2). The anatomo-pathological examination of the tumor sample found a necrosis mitotic glial tumor confirmed by immuno-histochemistry, and richly vascularized lesions with high proliferation factor suggesting glioblastoma. The patient underwent surgical tumorectomy associated with chemotherapy and radiotherapy according to guidelines [7]. CT scan magnetic resonance imaging six months after the surgery showed the disappearance of the lesion without any sign of relapses (Figures 3 and 4). Moreover the encephalic syndrome had disappeared, and no anomaly was found in cerebral angiogram, thoraco-pulmonary CT scan, echocardiography and cephalorachidian liquid culture. Thirty months later, the patient’s clinical examination is normal and HIV immuno-virological control showed undetectable viral load and CD4 rate raised to 553 cells/ml.
The incidence of cerebral primitive tumors is to 8-10/100,000 per year in France. In patients of more than 85 year-old, the incidence increased from 5.4 in 1975 to 15.7 in 1991 [15]. This increase is probably due to the improvement diagnostic tools such as CT scan and MRI and to the increase in life expectancy [15].
The malignant glial tumors that occur in young adult (25 to 34 yearold) are anaplasic astrocytome kind. They affect nearly 3,000 people per year in France. Glioblastomas represent 65% of gliomas and are the most frequent of primitive cerebral tumors that constantly increase in most of European countries [15]. The etiology is unknown in most cases (95%) except for rare cases of radio-induced gliomas or the exceptional genetic forms which were well identified [17,8]. In most of countries in Africa, particularly in Burkina Faso, cerebral tumors in general are underdiagnosed, because diagnostic tools are lacking.

Figure 1: CT scan without injection of contrast product shows the lesion (the right temporo-polar hypodensity is badly limited and is encircled by an oedema in shape of thimble.
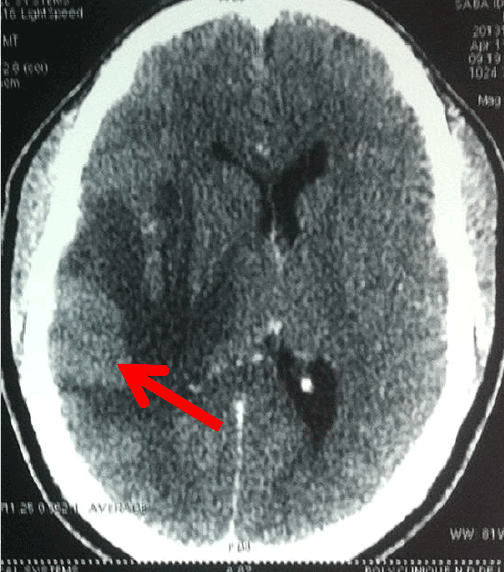
Figure 2: CT scan with injection of contrast product. We can notice a catch of contrast by the lesion which is better visible and is encircled at any time by the oedema in shape of thimble.

Figure 3: CT scan control during the 6th month (with contrast product) shows the disappearance of the lesion. That is to say there no lesion that takes the contrast product and is encircled by an oedema in shape of thimble; Furthermore, we can notice the initial surgical marks.
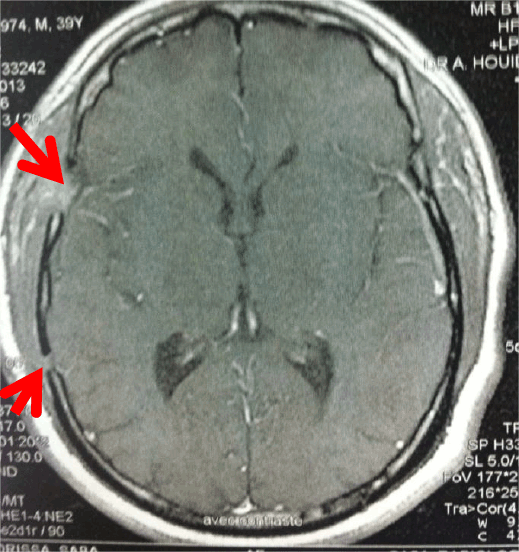
Figure 4: MRI control during the 6th month in T1 weighted sequences after injection of gadolinium. We can notice a lack of the lesion. That is to say there no lesion that takes the product of contrast and is encircled by an oedema in shape of thimble; furthermore, we can notice the initial surgical marks.
In fact the CT scan which is the initial examination that allows suspecting cerebral tumors is not always available. But even though it is available, it is not accessible for the most part of the population because it is expensive. Tumor malignity degree cannot be shown by CT scan which cannot often make the difference between high degree glial tumor and metastatic lesion or abscess. We need to use MRI and especially cerebral biopsy, with anatomopathologic analysis for diagnosis. Indeed, some authors such as Psimaras [8] and Wolff et al. [12] pointed out in their studies, some cases of glioblastomas, which were treated as a neurotoxoplasmosis. But due to clinical deterioration of patient brain biopsy allowed the diagnosis of glioblastoma. During HIV infection, the most frequent cerebral tumors are the non-hodgkinians cerebral lymphomas, which raise some diagnostic difficulties with the glioblastoma, as a consequence of frequent mislaying diagnoses [11].
Our patient had no glioblastoma risk factors such as the risk of chemical carcinogenesis related to the professional environment (rubber, lead, cerebral irradiation). The known medical history was immune suppression linked to HIV infection [8,17].
Although some viruses (JC, simian virus 40) are known to be etiologic in some cases of some cerebral tumors, to our knowledge, no study has showed the link between HIV and glioblastoma yet, unlike some cancers that have been identified since 1993, as associated with HIV infection [18,19]. However, Moullignier et al. [9] in France had already reported a case of glioblastoma in a homosexual infected by the HIV since 1992. In 1994, in a retrospective study on 70 patients infected by HIV, he discovered four glials tumors among which one was a glioblastoma [10]. Since then, this association was frequently observed, with some delays of diagnosis found and often associated with a fatal evolution; the diagnosis of glioblastoma is often done through an autopsy: a case which was previously diagnosed and treated like a neuro-toxoplasmosis in the study of Oliveira et al. [16], and another case in the study of Vannemreddy et al. [11], previously treated like a primitive lymphoma of the central nervous system.
In 2009, Hall et al. [13] noticed an increase in the frequency of the glioblastomas in HIV infected people. So the question that some authors ask to themselves nowadays is the probable oncogenic influence of the HIV on the glial cells [11].
Primitive cerebral toxoplasmosis and lymphoma are the most frequent neurological pathologies during HIV infection. But nowadays, we must look for glioblastoma that frequency is increasing in HIV infected people. The objective as far as glioblastoma is concerned, is to carry out an early diagnosis and treatment for better prognosis because according to Hall, survival depends on tumor and not immune depression [13]. For this intention, it is fundamental to have available and accessible medical, technical and therapeutic tools. However, even in developed countries with available high medical and therapeutic tools, gliobastoma diagnosis in HIV infected person has been done in post mortem or with some delays in diagnosis as shown Hall and other authors’ review of literature [9-14,16]. In our study survival is approximately 30 months after the diagnosis. In the literature, some authors found an average survival of 12- 15 months. In Hall et al. [13] survey, the average survival was about 8 months (ranges 0-26 months after the diagnosis) [3]. We think that the particularity of the long life of our patient is the fact that the diagnosis was early. The tumor was discovered fortuitously by cerebral imaging as well as the histological confirmation of the glioblastoma, which was not expected. Treatment was early and complete: tumorectomy was followed by a concomitant and complementary chemotherapy and radiotherapy. This treatment was possible in a country where radiotherapy was available unlike in Burkina Faso. The early diagnosis associated with an early and entire surgical and medical treatment would probably be accountable for the survival without any relapse of our patient up to now. Any other explanations? Has survival any link with HIV? Or with the ART? Or with the patient himself? Or a simple coincidence? Waiting for some answers in other studies, we had to suspect the glioblastoma and look for it in HIV infected people with any minimal neurological manifestations, and prescribe easily cerebral imaging.
The glioblastoma is increasing in HIV infected people. We should think about it, in an HIV infected person that has neurological manifestations even if they are minimal, because the prolonged survival of the patient will depend on the precocity of the diagnosis and treatment. In Burkina Faso, the reinforcement of the technical and therapeutic equipments for the cancers care is a strong recommendation.
Download Provisional PDF Here
Article Type: Case Report
Citation: Sondo KA, Zabsonré DS, Diallo I, Bambara TA, Ouédraogo SM, et al. (2015) A Rare Case of Co-Morbidity: Glioblastoma on HIV Infected Patient with more than Two-Year Survival. J HIV AIDS 1(3): http://dx.doi.org/10.16966/2380- 5536.112
Copyright: © 2015 Sondo KA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access