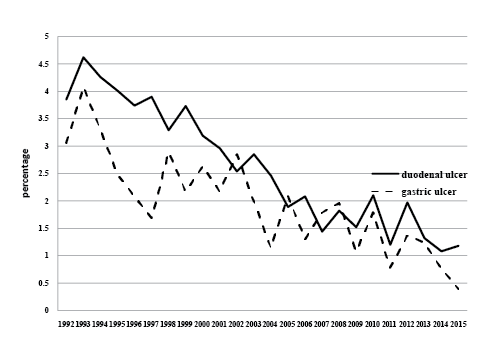
Figure 1: The yearly incidence of peptic ulcers as percentage of the total number of yearly upper gastrointestinal endoscopies.
Loffeld RJLF* Liberov B Dekkers PEP
Department of Internal Medicine and Gastroenterology, ZaansMedisch Centrum, Zaandam, The Netherlands*Corresponding author: Loffeld RJLF, Department of Internal Medicine and Gastroenterology, ZaansMedisch Centrum, Zaandam, The Netherlands, Tel: 31-75-6502779; Fax: 31-75-6502379; E-mail: loffeld.r@zaansmc.nl
Background: It was noticed that the incidence of peptic ulcer disease is decreasing in patients undergoing upper gastrointestinal endoscopy.
Aim: The yearly incidence of peptic ulcer disease and peptic ulcer bleeding is described.
Materials and Methods: A prospectively collected database of consecutive upper gastrointestinal endoscopies (1992-2016) was used.
Results: In the study period a duodenal ulcer was seen in 919 patients and, gastric ulcer 683. Two hundred twenty two patients (24.2%) had a bleeding duodenal ulcer; this was 125 patients (18.3%) with a gastric ulcer. Duodenal ulcers had significantly more often a presentation with bleeding than gastric ulcers (p=0.004). The yearly incidence of peptic ulcers significantly decreased in the study period. However, no decrease was noted in the number of patients with bleeding.
Conclusion: The incidence of peptic ulcers significantly decreases making the disease truly a vanishing disease.
Peptic ulcer; Epidemiology; Duodenal ulcer; Gastric ulcer
Peptic ulcer disease once was a condition with great morbidity and even mortality [1,2]. In the past operation was the only curative treatment option. This changed dramatically since the introduction of medical therapy [3,4]. In the late seventies of the twenties century with H2 -receptor antagonists, and later on with proton pump inhibitors. The most important step forwards in the treatment of this chronic recurrent disease was the discovery of H.pylori and the acceptance of its pathogenetic properties [5-7]. With anti-H.pylori therapy peptic ulcer disease could be cured definitely [8,9].
In daily practice it was noticed that the incidence and prevalence of peptic ulcer disease is decreasing in patients undergoing upper gastrointestinal endoscopy [10]. For this reason the earlier study was extended over a very long period of time in order to study the yearly incidence of peptic ulcer disease and peptic ulcer bleeding.
A large prospectively collected database of consecutive upper gastrointestinal endoscopies done in the endoscopy department of the ZaansMedisch Centrum, was used in order to identify patients with ulcers in duodenum or stomach. The study period was 1992 until 2016. Only patients with the first incident duodenal or gastric ulcer were included. Endoscopies done because of follow-up after prior diagnosed ulcer disease, especially in cases of gastric ulcer or complicated duodenal ulcer, were excluded. Endoscopy reports of patients with ulcers were studied for concurrent abnormalities in the upper gastrointestinal tract.
Statistical analysis was done with chi-square test for contingency tables. A value below 0.05 was considered significant.
In the study period a total of 34396 upper gastrointestinal endoscopies were done. A duodenal ulcer was seen in 919 patients (547 men, 377 women), while a gastric ulcer was diagnosed in 683 patients (381 men, 302 women). Two hundred twenty two patients (24.2%) with a duodenal ulcer had complicated ulcer disease in the sense that they had a bleeding ulcer, while this was the case in 125 patients (18.3%) with a gastric ulcer. Duodenal ulcers had significantly more often a presentation with bleeding than gastric ulcers (p=0.004). Figure 1 shows the yearly incidence of peptic ulcer in percentage of yield of the total number of yearly endoscopies. Figure 2 shows the absolute yearly numbers of peptic ulcers as well as the number of patients with a bleeding ulcer. As clearly can be seen a significant decrease in incidence in the period of 24 years is noted. However, no change was noted in the number of patients with bleeding. In fact, the yearly number of patients with a bleeding ulcer remained rather constant. Table 1 shows the concomitant endoscopic diagnoses. In 31 patients a concomitant malignancy was present (4 cases of oesophageal cancer, one cardia cancer, 26 cases of distal gastric cancer), in 37 cases the gastric ulcer appeared to be a malignant ulcer. Unfortunately the dataset did not include the macroscopic appearance of the ulcer. Hence it is not known whether the endoscopist already suspected the ulcer to be malignant.

Figure 1: The yearly incidence of peptic ulcers as percentage of the total number of yearly upper gastrointestinal endoscopies.
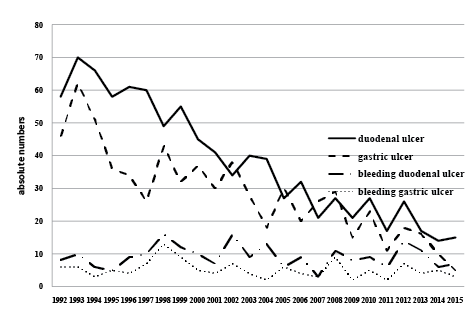
Figure 2: The yearly incidence of peptic ulcers in absolute numbers. In addition the yearly number of patients presenting with bleeding is noted.
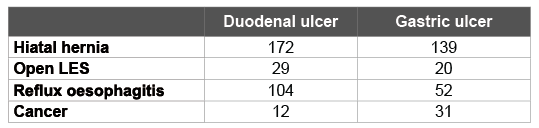
Table 1: Concomitant diagnoses in patients with peptic ulcer disease
The present study clearly shows an ongoing decrease in incidence of peptic ulcer disease. This is in accordance with reports from different countries all over the world [10-12]. Carli et al. [13] studied peptic ulcer disease in two different time periods. They reported on a decrease of peptic ulcer disease related to H.pylori. However, ulcers due to NSAID use showed a clear rise. Xia et al. [14] studied patients in Hong Kong sent for endoscopy because of dyspepsia and also found a decrease in mainly duodenal ulcer disease. The prevalence of ulcers also decreased in a 19- year observation period in Italy [15].
Since all ulcers diagnosed in the present study are new ulcers this decrease cannot be explained by installment of anti-H.pylori therapy. The only plausible reason is the decreasing acquisition of the bacterium in the population. The known risk factors for infection with H.pylori are a low standard of living, poor education, and reduced life span. Prevalence of H.pylori infection increases with rising age [16]. This phenomenon does not reflect an increasing acquisition when people get older, but merely is an age cohort effect [17]. H.pylori is acquired at young age and causes a life time inflammation of the stomach [18]. After being high in childhood the acquisition rate exponentially slows down with age in all age cohorts [19]. Change in H.pylori infection status with time is rare [20].The prevalence of infection in developed countries is falling [21]. Nowadays, gastric and duodenal ulcers tend to occur in older people, who were more likely to have been exposed to H pylori in their childhood than recently born generations [22]. It is well-known form several epidemiological studies that acquisition indeed is decreasing in the last decennia [14,23]. Since the Second World War the prevalence of H.pylori is decreasing, at least in the Western World. This is mainly due to improvement in living standard with better hygienic circumstances.
A possible flaw of the study is the fact that all patients underwent endoscopy, and that use of NSAID’s or acid suppressive therapy is not known. Many patients are treated because of dyspepsia by their general practitioner. Some undergo endoscopy; some are treated blindly with anti-H.pylori therapy without proper diagnosis. All these patients will not ever develop peptic ulcers if H.pylori is eradicated.
Not all ulcers are the consequence of an infection with H.pylori. Use of NSAID’s is also a risk factor. However, in the Netherlands, patients on NSAID therapy receive stomach protective therapy. Arents et al. [24] studied the prevalence of H.pylori-negative peptic ulcer disease in a period of eight years and detected a decrease in ulcer disease. Hence, it is to be expected that the occurrence of this type of ulcers also decreases.
An important observation is the fact the number of patients presenting with a bleeding ulcer did not decrease in the period of more than twenty years. In a large Danish study it appeared that despite the improved medical treatment of peptic ulcers this has not been associated with decreasing hospitalization or death from complicated peptic ulcers [25]. Bleeding ulcers also remain a problem in the United States of America. The number of patients treated endoscopically even increased [26]. There only can be speculation on the reason why the number of patients presenting a bleeding ulcer did not decrease. A possible explanation could be that many patients have cardiovascular disease and are treated with anticoagulant therapy.
From the present study it can be conclude that peptic ulcer disease is truly a vanishing disease.
Download Provisional PDF Here
Article Type: Research Article
Citation: Loffeld RJLF, Liberov B, Dekkers PEP (2016) Peptic Ulcer Disease: A Vanishing Disease! J Gastric Disord Ther 2(4): doi http://dx.doi.org/10.16966/2381- 8689.123
Copyright: © 2016 Loffeld RJLF, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access