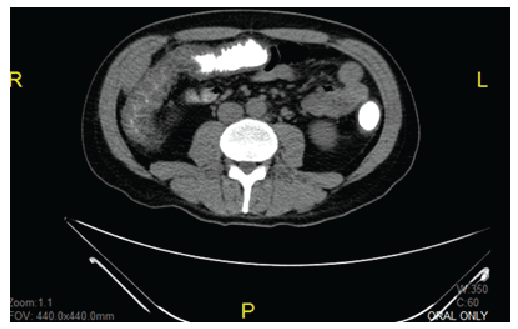
Figure 1: CT scan of patient’s colitis, showing colon wall thickening
Céline Pascheles1* Nicolae Bizeta2
1Stony Brook University School of Medicine, Stony Brook, NY, USA*Corresponding author: Céline Pascheles, Stony Brook University School of Medicine, Stony Brook, NY, USA, E-mail: Celine.pascheles@stonybrookmedicine.edu
Background: About 500,000 people are annually infected with Shigella species in the United States, with an average annual incidence of 4.82 cases per 100,000 individuals. While most reported cases have previously been described in children under the age of 10, Shigellosis has now been recognized as a sexually transmitted disease among men who have sex with men, with direct oral-anal contact posing as major risk factor.
Methodology: In this abstract we describe a rare case presentation of sepsis due to Shigella colitis in a previously healthy individual that led to a new diagnosis of HIV/AIDS. What makes this case unique is that the patient’s hospital course was soon complicated by hypoxic respiratory failure and recurrent sepsis associated with bilateral Pneumocystis jiroveci pneumonia confirmed with bronchoalveolar lavage.
Results: With appropriate antibiotic therapy and supportive measures the patient made a remarkable recovery leading to discharge at a rehabilitation facility. In addition, the patient was followed at an HIV clinic and within six weeks of anti-retroviral treatment, his viral load decreased by three logs and he had an appropriate immunologic response.
Conclusion:Shigellosis is a sexually transmitted disease that is prevalent in men who have sex with men, requiring a high index of suspicion in those who engage in oral-anal contact. To the best of our knowledge, this is the first case describing a previously healthy patient presenting with both Shigella and Pneumocystis jiroveci pneumonia, leading to a diagnosis of AIDS.
HIV; AIDS; Shigella; Pneumocystis jiroveci pneumonia; Case report; Sexually transmitted disease
Bacillary dysentery caused by Shigella bacteria is an intestinal bacterial infection that causes severe watery diarrhea [1]. The infection is highly contagious, spreading from person to person via food, drinking water and from oral-fecal transmission. Today, 500,000 people per year are infected with Shigella species in the United States, [1] with an average annual incidence of 4.82 cases per 100,000 individuals [2]. While most reported cases have previously been described in children under the age of 10, [3] shigellosis is now recognized as a sexually transmitted disease among men who have sex with men (MSM), with direct oral-anal contact posing as major risk factor [4]. MSM engage in direct oral-anal contact, thereby allowing for the transmission of Shigella, a now recognized sexually transmitted disease.
Internationally, men who have sex with men are almost 20 times more likely than the general population to acquire HIV, with numbers continuing to rise in certain geographical locations. In 2011, 41% of newly diagnosed HIV infections in Western Europe were found in men who had sex with men, and 63% in the United States of America [5].
Men who have sex with men are especially vulnerable to HIV because of the higher risk of viral transmission during unprotected anal sex in comparison to vaginal intercourse [6]. This is particularly significant because the men who have sex with men who acquire the HIV virus are subsequently at higher risk of further developing the opportunistic infections commonly seen with HIV/AIDS, including Shigellosis, as described above, as well as Pneumocystis jiroveci (PJP), a lung diseases seen in immunocompromised individuals with CD4 counts of less than 200 cells/µL [7].
In this report, we describe a unique presentation of Shigella colitis in a previously healthy individual that led to a new diagnosis of HIV/AIDS patient.
A 43 year old Caucasian male with no prior medical history presented with complaints of unintentional weight loss and anorexia over the past six months. Within the past five days he developed acute, progressively worsening diarrhea associated with diffuse abdominal cramps, fevers and progressive shortness of breath. Initial laboratory results showed lymphopenia and acute kidney injury, and his urine toxicology screen was positive for cocaine. Initial chest X-ray (CXR) was clear, but computed tomography (CT) scan abdomen showed pan colitis (Figure 1). He was started on empiric Ciprofloxacin and Metronidazole pending work up. Blood cultures remained negative, but stool cultures were positive for Shigella flexneri, which is rare considering the most common form of Shigella species in the United States is Shigella sonnei [1]. In the interim, he tested positive for HIV, with a CD4 count of 29 (7%) and a viral load of 253,910. He was then started on oral (PO) Trimethoprim/sulfamethoxazole (TMP-SMX) and weekly Azithromycin for opportunistic infection prophylaxis. Highly active anti-retroviral therapy (HAART) was deferred at this time. His hospital course was then complicated by respiratory failure and sepsis associated with bilateral pneumonia evident on CXR following intravenous (IV) hydration. He was empirically started on vancomycin and Piperacillin/Tazobactam for healthcare-associated (HCAP) but continued to be febrile, with an arterial blood gas (ABG) showing a PaO2 <70. Bronchoscopy was positive for Pneumocystis jiroveci pneumonia (PJP) on Broncho-alveolar lavage (BAL) and he was immediately started on IV TMP-SMX along with a 21 day course of Prednisone. After a brief clinical response, supported by CXR improvement, fevers recurred. Sulfa drug allergy was suspected and IV TMP-SMX was changed to IV Clindamycin and PO Primaquine to complete the 21 day treatment for PJP. He ultimately responded to this regimen and was sent to rehab.

Figure 1: CT scan of patient’s colitis, showing colon wall thickening
In this case report, we describe a case of HIV/AIDS presenting as Shigella colitis. Even more remarkably, the patient presented with Shigella colitis with coexistent Pneumocystis jiroveci pneumonia in the setting of newly diagnosed AIDS. Though PJP is the most common presenting manifestation of AIDS and has always been a major opportunistic infection since the beginning of the HIV/AIDS epidemic, [8] what makes this case so unique is the co-infection of PJP with Shigellosis. To the best of our knowledge and after an extensive literature review of the epidemiology, the simultaneous presentation of the two opportunistic infections in a previously healthy patient has never been described.
The high rates of shigellosis found in HIV infected patients can be explained by the compromised immunity found in those with HIV, making them more prone to infection [6]. This is significant because it complicates management and treatment of this patient population. In our patient, hospital course was complicated with PJP, a respiratory infection commonly found in those with CD4 counts <200 [8]. This required TMPSMX antibiotic treatment, the recommended medical therapy for PJP in HIV-infected patients. After a brief clinical response, however, the patient became febrile. Sulfa allergy was suspected, as allergic reactions to TMPSMX in AIDS patients are not uncommon, with rates as high as 30-40% [9]. In fact, the side effect profile of TMP-SMX is considerably greater in AIDS patients as compared to the general population, with a reported rate of 24–83% vs. 8% [10].
In the majority of cases, allergic reactions occur within the first two weeks of treatment, although delayed reaction can also be seen [11]. As such, about half of patients require a change in treatment. In our patient, antibiotic therapy was ultimately changed to IV clindamycin and PO Primaquine with favorable results and the patient was sent to rehab [9]. The patient was followed in outpatient clinic for 3 months, until he was lost to follow up.
Although the precise mechanism of how antimicrobial sulfonamides cause adverse drug reactions in HIV/AIDS patients still remains uncertain, it is possible that reactive metabolites may be involved.
Given the chemical reactivity of hydroxylamine and nitroso metabolites of sulfamethoxazole, covalent binding to proteins is likely, leading to the induction of specific immune responses. Therefore, it appears that changes in metabolism and detoxification are associated with an increased risk for developing allergic reactions to sulfonamides, with a more frequent allergy to sulfonamides in the AIDS patient population [9].
Given the acute drug reaction (ADR), our patient was started on Dapsone for PJP prophylaxis and HAART therapy as an outpatient. At the time of hospitalization, HAART therapy was withheld in attempt to avoid immune reconstitution inflammatory syndrome (IRIS) and adverse drug reactions [12].
Though there have been other reports of HIV/AIDS presenting as Shigella colitis or PJP, what is most remarkable in this case is that this patient presented with Shigella colitis with coexistent PJP, and was only subsequently found to have HIV/AIDS. To the best of our knowledge, this is the first paper describing the case of a previously healthy patient presenting with both Shigella colitis and PJP in the setting of newly diagnosed AIDS. Patient’s risk factors for HIV was unprotected sex with men and women in addition to illicit drug use. He denied injection drug use and had never had a blood transfusion. Interestingly, at the time of presentation he had not been sexually active for two years, yet he presented with these symptoms at this time.
With appropriate antibiotic therapy and supportive measures the patient made a remarkable recovery leading to discharge at a rehabilitation facility. In addition, the patient was followed at an HIV clinic and within six weeks of antiretroviral treatment, his viral load decreased by three logs and he had an appropriate immunologic response. His viral load decreased from 253,910 to less than 20, and his CD4 count increased from 29 to 365. Unfortunately, after 3 months of routine check ups, he was ultimately lost to follow up.
Download Provisional PDF Here
Article Type: Case Report
Citation: Pascheles C, Bizeta N (2016) AIDS presenting as Shigella colitis and Pneumocystis jiroveci pneumonia in a forty-three years old male. J Emerg Dis Virol 2(2): doi http://dx.doi.org/10.16966/ 2473-1846.115
Copyright: © 2016 Pascheles C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access