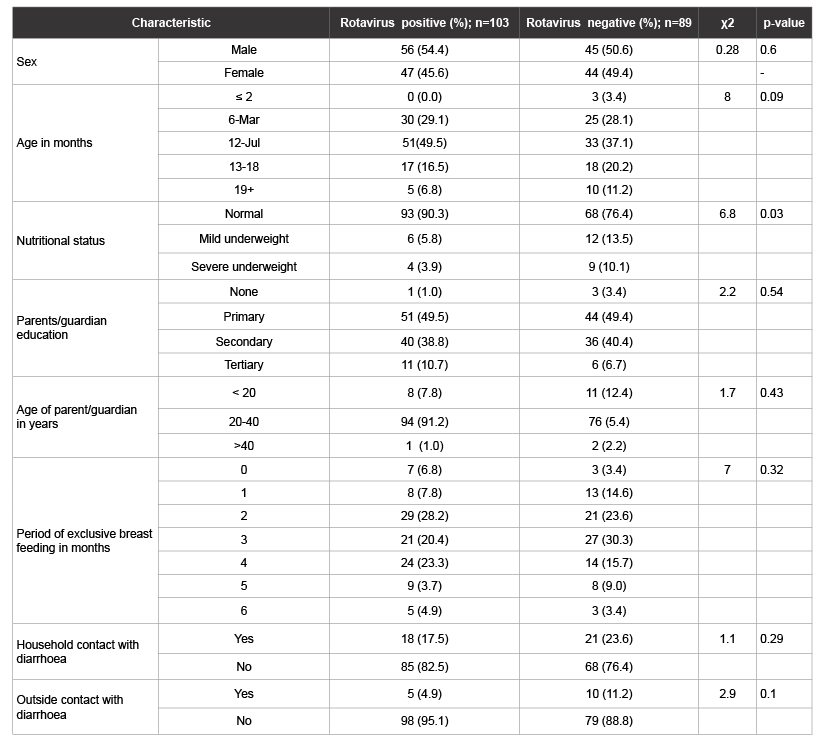
Table 1: Comparative demographic characteristics between rotavirus positive and rotavirus negative children (<5 years old) presenting with acute diarrhoea at Kenyatta National Hospital from June to August 2006
Gatinu BW1 Kiulia NM2 Nyachieo A2 Macharia W1 Nyangao JO3 Irimu G1*
1Department of Paediatrics, University of Nairobi, Nairobi, Kenya*Corresponding author: Grace Irimu, Department of Paediatrics, School of Medicine, University of Nairobi, P.O. Box 19676, Nairobi, Kenya, E-mail: girimu2014@gmail.com
Background: Worldwide rotavirus (RV) infection is a major cause of diarrhea in children <5 years of age. Continual monitoring of RV prevalence and its associated clinical characteristics is necessary to estimate the burden of the disease. In this study, we evaluated the clinical features associated with RV diarrhea such as dehydration and levels of electrolytes, urea and creatinine at Kenyatta National Hospital, Nairobi, Kenya.
Methods: A total of 192 diarrheic stool samples were collected from children under 5 years of age and tested for presence of RV using enzyme immunoassay (EIA). A further 92 blood samples collected from the same cohort but only targeting severely dehydrated children, were used for the analysis of electrolytes (Potassium and Sodium ions), urea and creatinine.
Results: Rotavirus was detected in 53.4% (103/192) of stool specimens. Dehydration was common in most of the children who presented with diarrhea regardless of RV status (172/192; 89.6%). However, RV patients had increased duration and frequency of vomiting compared with non rotavirus patients but levels of dehydration were similar in both groups. There was loss of electrolytes and elevated levels of both urea (>7.5mmol/l) and creatinine (>80μmol/l) in all severely dehydrated cases.
Conclusion: Rotavirus was associated with increased duration and frequency of vomiting, but loss of electrolytes and elevated levels of both urea and creatinine were similar among severely dehydrated RV positive and negative children. This study provides useful information to policy makers on RV that could, together with other studies in Kenya on RV, aid in understanding the disease burden, earlier clinical diagnosis and evaluation of cost benefit analysis for RV vaccines in Kenya.
Rotavirus; Children; Clinical features; Diarrhea; Electrolytes
Rotavirus (RV) is the most common cause of acute gastroenteritis in young children and is associated with substantial morbidity and mortality. It is also the leading cause of severe dehydrating diarrhea in infants and young children less than 5 years of age worldwide [1,2]. In sub-Saharan Africa, estimations show that RV infection is responsible for the death of approximately 300,000 children under 5 years old annually [3]. In other diarrhoeal diseases, improvement of hygiene and sanitation may reduce the incidence, but these measures are unlikely sufficient for RV control. Vaccination is considered to be the best control measure likely to have a significant impact on the incidence of severely dehydrating RV disease [4]. Since RV vaccine is yet to be introduced in many less developed countries due to cost burden, early detection and clinical management of RV cases remains the most practical way of decreasing child morbidity and mortality in these countries. In addition, due to limited data available in less developed countries, active continual surveillance of RV is required to estimate the true burden of the disease to serve as a basis for policy makers to determine where and when they can introduce the vaccines.
In Kenya, several studies have documented the prevalence of RV in young children in different hospitals [5,6]. Based on these reports, the prevalence of RV infection varies widely underscoring the importance of hospital-based surveillance [7]. For instance, one study of clinics in Nairobi including Kenyatta National Hospital, where our present study focused, found a RV prevalence of 11% during 2001-2002 surveillance [8] which on follow-up in 2006-2008 increased to 40% [7]. However, none of these studies documented clinical features or profiles of electrolytes, urea and creatinine. Such clinical data is important for the diagnosis and management of the disease. To address this issue, we postulated that severely dehydrated RV positive cases are more likely to have unusual levels of electrolytes, urea and creatinine as compared to other nonrotavirus diarrhoea cases.
This cross sectional study was carried out at the Pediatric Emergency Unit and the general pediatric wards of Kenyatta National Hospital (KNH) Nairobi, Kenya. Kenyatta National Hospital is the largest public hospital in Kenya. It is located in Nairobi, the capital city. It is both a referral centre for pediatric cases (defined as up to 12 years of age), as well as a primary health facility for sick children mostly serving the residents of Nairobi, and a good number of children from the bordering districts.
Fecal samples were collected between 1st June to 31st August 2006 from consecutive children aged <5 years old presenting with diarrhea in KNH. Only those children who had experienced an episode of 3 looser than normal or watery stools in a 24-hour period lasting for ≤ 7 days were enrolled. The inclusion and exclusion criteria were based on the WHO’s Generic Protocol for Hospital based Surveillance of Rotavirus Gastroenteritis in children under 5 years of age [9].
A focused clinical history and physical examination was undertaken by the physician and the details entered in the study questionnaire. The level of dehydration was classified using the WHO guidelines as no dehydration, some dehydration, severe dehydration without shock and severe dehydration with shock [10]. The level of dehydration was based on clinical parameters such as skin turgor, sunken eyes, ability to drink, peripheral pulses character, and level of mental consciousness.
Fecal samples (about 5 g) were collected in sterile specimen collecting bottles (poly pots) and stored at 4°C until analyzed by enzyme immunoassay (EIA) for detection of RV and then transferred to -20°C for long term storage. Blood samples were also collected for analysis of electrolytes, urea and creatinine.
A ten percent suspension of fresh stool in sample diluent (phosphate buffered saline (pH 7.4) was made and tested for the presence of group A rotavirus antigen by using a commercial rotavirus antigen-detection enzyme immunoassay (EIA) (IDEIATM kit, Dako Diagnostics Ltd, Cambridgeshire, UK) according to the manufacturer’s instructions and as also described in detail elsewhere [11].

Table 1: Comparative demographic characteristics between rotavirus positive and rotavirus negative children (<5 years old) presenting with acute diarrhoea at Kenyatta National Hospital from June to August 2006
Blood samples of children with severe dehydration were assessed for electrolytes by assays for potassium and sodium ions, urea and creatinine on sera. To obtain sera, whole blood was kept at room temperature (24-25ºC) for 2-3 hours then centrifuged at 1400 rpm which was then aliquoted into 2 ml vials and kept at -20ºC until use. The biochemical analysis were done at the Kenyatta National Hospital biochemistry laboratories on automated instrument (CE6600 Multimode Computing UV Spectrophotometer, Cambridge, England) by use of commercial kits specific for each analyte (Human, Gesellschaft für Biochemica und Diagnostica mbH, Wiesbaden Germany). The reference values used were provided by the manufacturer.
The prevalence of dehydration among RV positive and RV negative patients was compared using Chi-square test; median levels of electrolytes, urea and creatinine between RV positive and RV negative cases were compared using Student’s t-test. All statistical calculations were conducted using StatView software (SAS Institute, USA). Differences with p-values <0.05 were considered significant.
This study was approved by the Kenyatta National Hospital Ethics and Research Committee and informed consent was obtained from children’s guardians/parents before enrolment into the study.
A total of 192 children with diarrhoea were recruited for the study with 103 (53.4%, 95% CI: 46.3-60.9) being positive for RV infection. Demographic characteristics for the children including nutritional status, parents’ education, parent’s age, duration of breastfeeding, and having a household contact with diarrhea were similar between rotavirus positive and negative cases (Table 1). Classification of RV positive cases according to age showed that the majority of RV disease occurred in children ≤ 18 months of age (98/103; 95%, Table 1). Most (89.6%; 172/192) of the diarrhoea cases were accompanied by dehydration (Table 2). The frequency and duration of vomiting were both significantly higher in RV positive cases as compared to non-rotavirus cases (p=0.0065 and p=0.004, respectively; Table 2). However, there was no significant difference in dehydration status between RV positive and negative cases.
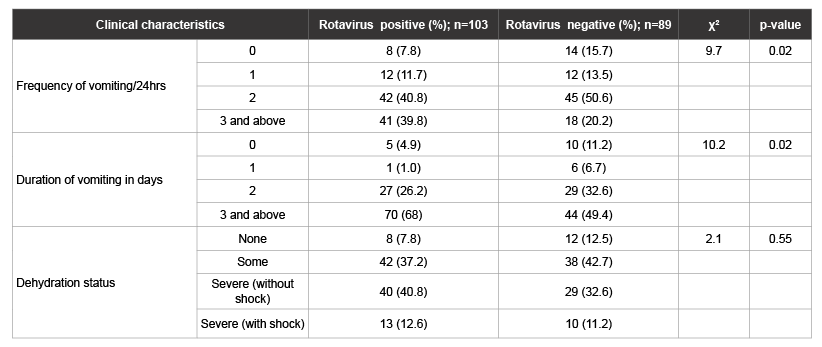
Table 2: Comparative clinical characteristics between rotavirus positive and rotavirus negative children (<5 years old) presenting with acute diarrhoea at Kenyatta National Hospital from June to August 2006.
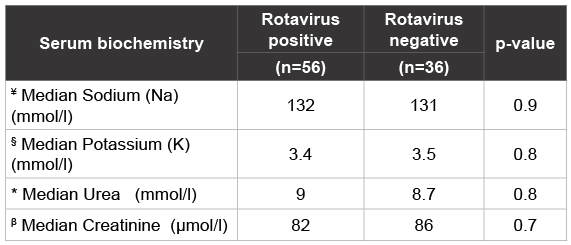
Table 3: Levels of serum electrolytes, urea and creatinine among rotavirus
positive and rotavirus negative children of <5 years old with severe
dehydration (n=92) at Kenyatta National Hospital from June to August 2006.
Normal values (range)
¥ Serum Sodium (Na) mmol/l = 135.0-155.0
§ Serum Potassium (K) (mmol/l) = 3.6-5.5
* Serum Urea (mmol/l) = 1.7-8.3
β Serum Creatinine (µmol/l) = 44.0-80.0
Fifty-six (56/103, 54.4%) of RV positive patients and 36 (36/89, 40.4%) of RV negative patients had blood biochemistry done. Analysis of serum electrolytes (Potassium and Sodium), creatinine and urea among those severely dehydrated showed that in both RV positive cases and negative cases there was a slight hyponatremia and hypokalemia and slightly elevated levels of both urea and creatinine. These differences between RV positive and negative cases were not statistically significant (Table 3).
The prevalence of RV diarrhea among the children aged less than 5 years who presented to Kenyatta National Hospital between June to August 2006 was 53.4% (95% CI; 46.3%-60.9%). The majority (about 90%) of RV positive cases occurred among children ≤ 18 months. The findings were similar to studies carried out elsewhere in Africa [12, 13] The proportion of RV declined after 18 months of age possibly due to immunity conferred by prior RV infections [14]. Children above this age group were less likely to seek medical care in hospital. This study indicates that RV infection in developing countries peaks during early life (< 2 years) similar to RV infection in developed countries [12, 15, 16].
Our data indicated that RV patients had increased duration and frequency of vomiting compared with non-rotavirus patients but the levels of dehydration were similar. Similar data has been reported elsewhere [17- 22]. The frequency of vomiting (>3 per 24 hrs) of vomiting at the initial stages of disease (usually preceding loose stools) as observed in our study could be useful information during diagnosis of possible RV.
Analysis of serum electrolytes showed that in severely dehydrated cases there was a slight hyponatremia and hypokalaemia and slightly elevated levels, above normal, of both urea (>8.3 mmol/l) and creatinine (>80 µmol/l) though no significant differences between RV positive and negative cases. The study did not obtain adequate information to determine the cause of the electrolyte derangements. Nevertheless, it is possible that all the children who visited the Kenyatta National Hospital may have had some form of fluid management prior to presenting to Kenyatta National Hospital with either plain water, home-made solutions, oral rehydration salts at home or intravenous fluids for those referred from other hospitals but further studies are required to investigate this concept.
There are several limitations of the present study. First, because of short duration (3 months) of the study, these data may not be fully representative of actual burden of RV disease in Kenya. The shortened study period also limits determining the annual prevalence of RV comparability of the prevalence of RV observed in this study with other studies. Additionally, we also only collected data from a single hospital and children with RV diarrhea treated at this hospital may not be representative of all children with RV diarrhea in Kenya. We did not collect data about treatment for dehydration prior to receiving care at Kenyatta National Hospital which may have influenced the levels of dehydration observed in our study.
Group A RV is a common cause of diarrhoea associated with severe dehydration in Kenya. However, there was no difference in levels of electrolytes, urea, or creatinine among severely dehydrated RV positive and RV negative children. This study, together with other studies in Kenya on RV, could aid in understanding the disease burden and evaluation of cost benefit analysis of RV vaccines introduction in Kenya.
GBW acknowledges partial funding from GlaxoSmithKline Biologicals for his Master of Medicine studies.
The authors declare no conflict of interest. Kiulia NM and Nyangao JO are members of the African Rotavirus Surveillance Network. None of the authors have associations that could pose conflicts of interest.
Download Provisional PDF Here
Article Type: Research Article
Citation: Gatinu BW, Kiulia NM, Nyachieo A, Macharia W, et al. (2016) Clinical Features Associated with Group A Rotavirus in Children Presenting with Acute Diarrhoea at Kenyatta National Hospital, Nairobi, Kenya. J Emerg Dis Virol 2 (1): doi http://dx.doi.org/10.16966/2473-1846.112
Copyright: © 2016 Gatinu BW, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access