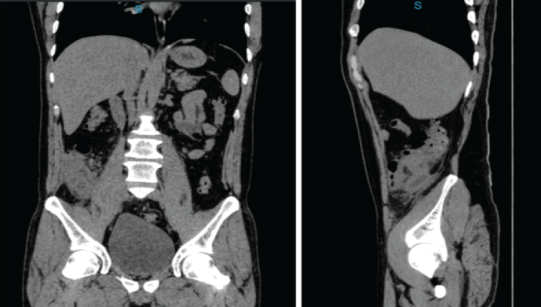
Image 1: Abdominal CT scan, coronal and sagittal view, appendicular area with abundant striation of mesenteric fat with appendicular thickening.

Hidalgo-Delgado Jesús Nicolás1* Bizueto-Rosas Héctor2 Zárraga-Rodríguez José Luis2 Reyes-Quijano Luis Antonio3 GómezCuevas Carlos Fernando4 Magaña-Salcedo Jaime Roberto1 Echeverry-Fernández Camilo Andrés1 Valdés-González Tayde Teresa1 Díaz-Cupa Brenda5 Vera-Salinas Agustín Ignacio1 Maldonado-Perdomo Jorge Emmanuel1 Tego-Ortiz Gabriel Yamil1 Bizueto-Blancas Noelly Noemí6 García-Solís Mario7 Pompa de La Rosa Cayetano8 Torrejón-Hernández Carlos Adrián1
1General Surgery Resident, Dr. Darío Fernández Fierro, General Hospital, ISSSTE, Mexico City, Mexico*Corresponding author: Hidalgo-Delgado Jesús Nicolás, General Surgery Resident, Dr. Darío Fernández Fierro General Hospital, Instituto de Seguridad Social de los Trabajadores del Estado (ISSSTE), Mexico City, Mexico, Tel: +52 7331357737; E-mail: nickolhd24@hotmail.com
Objective: Presentation of an acute appendicitis and non-Hodgkin lymphoma of lymphoid tissue associated with extranodal mucosa from the cecum clinical case.
Introduction: The cecal appendix can be affected by Non-Hodgkin Lymphomas (NHL) by extension of the neoplasm; however primary appendicular lymphoproliferative processes are uncommon. The NHL of Mucosal-Associated Lymphoid Tissue (MALT) is exceptional. To establish the diagnosis of MALT, a morphological, molecular and immunohistochemical diagnosis is required, including molecular techniques that reflect B cell clones, PCR analysis or the identification of chromosomal abnormalities.
Methods: 40 year old male, with 15 days of evolution of abdominal pain located in Right Lower Quadrant (RLQ) and associated symptoms like decreased appetite, nausea, and adynamia, who was firstly diagnosticated as an urinary tract infection treated as outpatient; upon his readmission, he was performed CT scan evidencing mesenteric panniculitis and thickening of the appendicular wall; he was surgically intervened finding edematous and congestive vermiform appendix with lower third perforation, and indurated cecum with 2 cm perforation from the appendicular base, performing right hemicolectomy with ileo-transverse mechanical anastomosis; he was discharged home 7 days after the postoperative period; the histopathological study and immunohistochemistry panel was compatible with MALT-type lymphoma, with lesion-free edges. Extension CT scans with no evidence of distant disease. He was sent to oncology for follow-up.
Conclusion: It is important to get an established diagnosis in this rare pathology with molecular techniques and not only with histopathological cuts, since 30% of patients relapse.
Extranodal lymphoma; Cecum; Acute appendicitis
Mucosal-Associated Lymphoid Tissue Lymphomas (MALTs) are a subtype of non-Hodgkin lymphomas, classified by the World Health Organization (WHO), as B-cell lymphomas that are in extranodal areas, which lack of organized lymphoid tissue. They most often affect the stomach, followed by the small intestine and colon, but can affect other parts of the gastrointestinal tract. It accounts for about 5% of all Non-Hodgkin Lymphomas (NHL) [1-4].
The term MALT-like lymphoma was introduced in 1983 by Isaacson P, et al. [5]; it is believed to be due to chronic antigenic stimulation caused by persistent infection and/or autoimmune processes [3,4]. Histologically it is classified as a lymphoepithelial lesion with invasion of the lymphoplasmic epithelium [1].
Non-gastric MALT is the third NHL in frequency (6-8%); it is asymptomatic, chronic, with a long survival, however, contrary to other lymphomas, it is incurable. For the diagnosis of MALT, as in all lymphomas, an excisional lymph node sample must be taken, in the search for neoplastic cells in the marginal area of the node, with a behavior of interfollicular expansion in layers and cytoplasmic eosinophilia, which have the appearance of clusters (degenerated cells), together with the use of microscopic and immunohistochemical techniques where it is necessary, to have pathological expertise.
Lymphomas, both Hodgkin and non-Hodgkin lymphomas, can affect the cecal appendix secondarily after the extension of the neoplasm from another location. The involvement of the gastrointestinal tract by extranodal lymphomas represents between 30-45% of the total [6] and 1 to 4% of gastrointestinal malignancies [1]. MALT-type NHL accounts for 7% of all NHL in Europe. Within NHL, primary appendicular lymphoproliferative processes are very rare; they are usually B-cell NHL such as the Burkitt type or the diffuse large B-cell [1]; as for MALT-type NHL, they are considered exceptional cases [7,8].
Appendicular involvement is an extremely unusual location for a primary lymphoproliferative process and represents according to some series 0.015% [7]; it develops in men in the sixth decade of life, so it is mentioned that with the increase in life expectancy, this entity must be considered as a differential diagnosis of acute abdomen in geriatric patients [8].
For the diagnosis, which is usually late, it is necessary to perform a complete immunohistochemical battery of CD20, CD79a and CD43, in addition to extension imaging studies. As CT findings, the presence of retroperitoneal nodular adenopathies with necrotic appearance and tumor lesion of pseudo nodular appearance in RLQ of cecal origin is suggestive of localized primary appendicular tumor, with adjacent fat respected [9]. The appendicular affection is due to the intravascular invasion of the tumor that conditions ischemia and inflammation of the appendix. The behavior of MALT-like NHL is usually aggressive [8].
MALT colon lymphoma rarely causes abdominal pain, perforation, obstruction or intussusceptions; is commonly asymptomatic or associated with mild to severe gastrointestinal bleeding. In the colonic MALT lymphoma, there is usually simultaneous involvement in other areas of gastrointestinal tract [10].
For the treatment after evaluation by hematology, chemotherapy (rituximab, cyclophosphamide, hydroxydaunorubicin, vincristine, prednisone [R-CHOP]) and/or radiotherapy is recommended, depending on whether the extension study is negative or positive.
According to the location, cecostomy and appendectomy can be curative [8-13].
In the case of gastric MALT lymphoma, the prognosis is less favorable in the presence of diffuse B-cell lymphoma, usually coupled with H. pylori antibiotic resistant and the existence of mutations (Bcl10 or NFκB), which worsen the response to treatment [14]; however, it is important to mention that H. pylori does not play a role in the development of extragastric MALT lymphomas [9].
In colorectal MALT lymphoma, surgical resection is mandatory when there is no response to eradication therapy or chemotherapy and if it is localized without spread. On the other hand, other authors report that surgery is the procedure of choice for colorectal MALT lymphoma, because its pathogenesis and therapeutic strategy are not well established [9].
40 year old male, with history of smoking, began his condition fifteen days before its admission, with abdominal pain in RLQ with stinging characteristic, intensity 7/10 on EVA scale, accompanied with fever (38°C); it was diagnosed as a complicated urinary tract infection, prescribing a third generation cephalosporin and analgesics as outpatient treatment; he returns to the emergency department, referring persistence of pain, adding loss of appetite, nausea, asthenia and adynamia; to the physical examination with decreased peristalsis, intense abdominal pain on deep palpation in RLQ without peritoneal irritation data. Laboratory studies are within normal parameters. CT scan is requested in which intestinal loops are observed at cecum level and appendicular area with mesenteric panniculitis and thickening of the appendicular wall (Images 1 and 2).

Image 1: Abdominal CT scan, coronal and sagittal view, appendicular area with abundant striation of mesenteric fat with appendicular thickening.
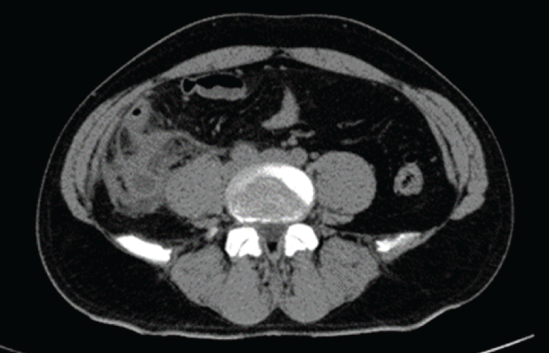
Image 2: Abdominal CT scan, axial view, Intestinal loops attached at cecum level and appendicular area with striation of mesenteric fat.
It is decided to intervene surgically with an exploratory laparotomy, finding purulent free fluid at the pelvis, inflammatory plastron and adhesions at peri cecal level with edematous and congestive vermiform appendix with a lower third perforation, indurated cecum with multiple adhesions to retroperitoneum, and perforation 2 cm from the appendicular base, therefore, extended right hemicolectomy is performed with mechanical lateral ileotransverse anastomosis; Penrose drainage is placed in the pelvis; The surgical piece is sent for definitive anatomopathological study.
The patient evolves properly, being managed with antimicrobial and analgesic treatment for 7 days; diet was started 3 days postoperatively and it is discharged from the hospital 8 days after.
The definitive macroscopic and histopathological report was an acute appendicitis with findings of chronic and acute intense periappendicitis (Image 3), cecum with a tumor lesion measuring 2.2 × 2.1 × 1.7 cm; histopathological reports and the immunohistochemistry panel (Immunohistochemical pattern: BCL2++, BCL6+, Kappa+light chains, Lambda+light chains) was compatible with MALT-type lymphoma; malignant free surgical margins. Contrasted CT was performed without evidence of distant disease, sending the patient to medical oncology service for follow-up and clinical surveillance.
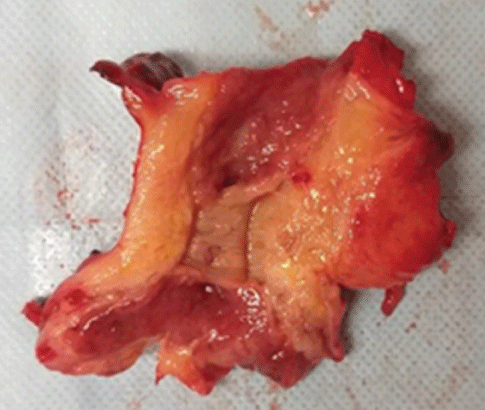
Image 3: Cecal appendage measuring 12 × 6 × 4 cm of smooth, opaque surface, with fibrin-purulent deposits, meso adipose appendage, yellow, wall of 2 cm, appendiceal lumen occupied by material.
We are facing a dilemma, the longer-living population that entails longer exposure to carcinogenic factors (Pan American Health Organization, PAHO); such as environmental factors, water and air pollution, are risk factors for some types of cancer, including colon; 57% of new cases of cancer and 47% of cancer deaths were in patients over 69 years of age; the WHO estimates that by 2030, new cases will exceed 20 million annually; It also mentions that in Mexico (being cancer the third cause of death and colon cancer, the third most frequent) in the last 20 years since 1990, there has been an increase of oncologic patients due to the growth and aging of the population [15].
We will have more and more pathologies such as MALT lymphoma, which although they are very rare diseases, the increase in survival of the population, makes the time of exposure to external factors, cellular degenerations and a chronic antigenic stimulation caused by a persistent infection and/or autoimmune processes (autoimmune thrombocytopenic purpura) long enough to let these lesions develop [3,4,16]. Which means, we have to suspect and take into account these conditions in the diagnosis, no matter how rare they are, and the management must be multidisciplinary.
We cannot establish definitive treatment guidelines, because they are emerging diseases and just a few cases have been reported.
H. pylori infection is currently considered a public health problem, since 50% of the world’s population suffers from it and is related to gastric MALT lymphoma; the indiscriminate use of antimicrobial therapy has caused the emergence of antibiotic resistance, leading to a public health problem [16]. In Mexico the prevalence goes from 30 to 90% [17] and worldwide 50% [18,19].
We mention all of this because it has been related to emerging pathologies such as our case; and since gastric, colon, and lung cancer [10] are among the main causes of death in our country, we should take it into account, like other pathologies that can affect us.
It is noteworthy that hereditary factors could be related, and this can be suspected when most cases occur in regions such as Japan, Korea and Taiwan, that could be due to the age of its population, dietary risk factors or the timely detection of the pathology [20].
Although many studies have suggested so far that colorectal MALT lymphoma is not related to H. pylori infection, it would be necessary to perform or clarify in the future with immunohistochemical tests, that over time will be improved and the development of new tests (such as qualitative immunochromatographic tests based on the detection of the peroxydoxine antigen, present in pathogenic germs) will allow us to identify factors associated with immune regulation disorders or identify new pathogenic mechanisms; it should also not be forgotten that its interpretation requires well-trained personnel.
It is also described that colorectal cáncer results from chromosome instability with mutations that compromise not only the coli gene of adenomatous polyposis, but also the tumor suppressor gene p53 and the K-ras oncogene in 85% of cases, and the remaining 15%, is due to the loss of genes involved in the repair of DNA imbalances (microsatellite instability), that increase the incidence of MALT lymphoma, together with prolonged exposure to potentially triggers of the longer-living population [21].
Although it is described that most MALT lymphomas of the colon can manifest with mild or massive gastrointestinal hemorrhage, the findings in colonoscopy are nonspecific and can be confused with a polypoid lesion, an ulcer, a nodule or even be reported as normallooking mucosa [10].
MALT lymphoma being a rare pathology, treatment is not yet standardized.
Faced with new scenarios as a longer-living population, we must bear in mind pathologies that are uncommon, the confirmation diagnosis must be histopathological, which requires immunohistochemical tests, diagnostic expertise, but most important, is the early suspicion of rare diseases either by environmental, dietary, and personal risk factors, since making a timely diagnosis, survival can be satisfactory
It is better to suspect it than make an incorrect diagnosis that can fall into the realm of medical negligence. “The doctor and the confessor, the older the better.”
The authors declare that there is no conflict of interest.
Right to privacy, confidentiality of data and informed consent.
The authors state that they have followed their workplace’s protocols on publication of patient data and that no patient data appear in this article.
This research has not received any specific grants from public sector agencies.
Download Provisional PDF Here
Article Type: CASE REPORT
Citation: Nicolás HDJ, Héctor BR, Luis ZRJ, Antonio RQL, Fernando GCC, et al. (2022) Non-hodgkin Lymphoma of Lymphoid Tissue Associated with Extranodal Mucosa of the Cecum and Acute Appendicitis. Report of a Case. J Surg Open Access 8(1): dx.doi.org/10.16966/2470- 0991.259
Copyright: © 2022 Nicolás HDJ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access