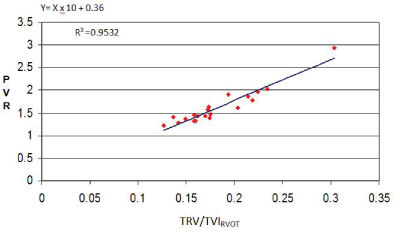
Figure 1: Linear regression analysis between PVR by right catheterization and the ratio TRV/TVIRVOT obtained by Doppler echocardiography.

Tania T Muñoz-Hernández* Elizabeth Hirschhaut-Schor Simon F Tovar-Blanco Guillermo J Lara-Boada
Department of Cardiology, Military Hospital “Dr. Carlos Arvelo”, Caracas, Venezuela*Corresponding author: Tania T Muñoz-Hernández, Echocardiography Unit, Department of Cardiology, University Hospital “Dr. Carlos Arvelo”, Av. Jose Angel Lamas, San Juan Parish, Caracas, Venezuela, E-mail: electroshock_2010@hotmail.com
Introduction and objectives: Right Heart Catheterization (RHC) is a gold method to perform the Pulmonary Vascular Reactivity Test (PVRT), however echocardiography has proven effective in estimating different hemodynamic variables. This study to demonstrate that with the Doppler echocardiographic index: Tricuspid Regurgitation Maximum Velocity (TRV)/Time-Velocity Integral of the Right Ventricle Outflow Tract (TVIrvot) we will obtain a Pulmonary Vascular Resistance Value (PVR) comparable to the invasive method. We evaluate its applicability in the PVRT.
Methods: Prospective, double-blind, observational study in 30 patients, performed in 2 stages: A) We obtained simultaneous measurements of PVR by invasive method and echocardiography. TRV/TVIrovt index measurements were correlated with invasive PVR using the analysis of linear regression. An equation was modeled to calculate PVR in Wood Units (WU) by echocardiography; the results were compared with invasive RVP measurements using the Bland-Altman analysis. B) TRVP was performed by simultaneous measurement of PVR and Pulmonary Arterial Mean Pressure (MPAP) with the echocardiographic and invasive method. We use the equation formulated by Abbas (RVPa) and another modified one proposed in this study (RVPt).
Results: In the first stage, the TRV/TVIrotv ratio correlated well with invasive PVR measurements (R2 =0.92). The Bland Altman analysis using RVP=10 × VRT/TVIrvot+0.36 showed satisfactory agreement limits (mean ± 0.36, L: 0.12-0.61). In the TRVP there was a high correlation of PVR between the two methods using the two equations. We also found high correlation with MPAP.
Conclusions: The Doppler echocardiogram offers a reliable and non-invasive method to measure the PVR and MPAP in the PVRT.
Right heart catheterization; Wood units; Doppler echocardiography; Pulmonary vascular reactivity test
TRV-Peak Tricuspid Regurgitant Velocity; TVI rvot-Right Ventricular Outflow Tract Time-Velocity Integral; PVRTPulmonary Vascular Reactivy Test; MPAP-Mean Pulmonary Arterial Pressure; PH-Pulmonary Hypertension; PVR (SG)-Pulmonar Vascular Resistence (Swan Ganz)
Pulmonary vascular resistance is a hemodynamic variable very useful for the management of patients with advanced pathologies cardiovascular and pulmonary, to evaluate the therapeutic response in patients with congestive heart failure [1,2]. Evaluation of patients candidates for cardiac and liver transplant [3-7], is a prognostic parameter for patients with congenital diseases [8], is considered a critical parameter for evaluating PH independent of etiology [9]. The PVR is calculated invasively by the relation of the pressure gradient and the flow transpulmonar [10], Abbas and collaborators [11,12] proposed to estimate the measurement echocardiographic of the PVR by the relation TRV/TVIrvot representing the method most used currently, among others proposed for its calculation [13-18]. On the other hand, the PVRT has very precise indications according to the European Society Cardiology guidelines [9] for the diagnosis, treatment and prognosis of the PH. Right catheterization is considered as the gold standard for the definitive diagnosis of PAH and the method of choice for PVRT [19]. There aren’t reports of studies comparing in the PVRT simultaneous measurements of PVR and MPAP with the invasive method and the Echocardiography Doppler. In this investigation we raised 3 objectives: 1) Revalidate Abbas’s equation in a group of patients [20] with indication of Right Heart Catheterization (RHC) diagnosis. 2) Compare the invasive and non-invasive measurements of MPAP and PVR in a group of patients who underwent the PVRT and verify the effectiveness of the echocardiographic measurements. 3) Demonstrate in this group of patients the utility and efficiency of a novel Echocardiographic equation to calculate the PVR when compared with the Abbas’s equation [10] and the RHC.
It’s a prospective, double-blind, observational study that was divided into two stages, the first part was selected 20 patients. 10 patients with admission to Intensive Care Unit (ICU) and placement of Swan Ganz catheter for presenting medical pathologies that merited measurement of hemodynamic variables; 10 patients in the Center’s cardiology department consultation or hospitalization, with indication of right catheterization to confirm diagnosis clinical and echocardiographic of PH. No distinction was made for age group, sex, comorbidity, or medication was omitted (Table 1). All patients entered our center in the period from February to August 2008.
| SEX (M/F) | 15/5 |
| AGE mean (RANGE) years | 48 (21-78) |
| Ejection fraction mean (RANGE) | 55 (30-75) |
| MPAP mean (RANGE) mmHg | 20 (13-30) |
| Pulmonary capillary pressure | |
| Mean (RANGE) | 12 (6-20) |
| 12 mmHg | 12 |
| 13-19 mmHg | 7 |
| ≥ 20 mmHg | 1 |
| PVR (cat) mean (RANGE) (WU) | 1.5 (1.22-2.02) |
| PVR S.G mean (RANGE) | 1.7 (1.28-2.95) |
| Diagnostics | |
| Aortic valve replacement+revascularization | 1 |
| Mitral valve replacement | 1 |
| Resection of Myxoma+revascularization | 1 |
| Myocardial revascularization | 6 |
| Aorticaneurysm correction | 1 |
| Ventricular septal defect | 3 |
| Interatrial Communication | 6 |
| Dilatation of the pulmonary artery trunk | 1 |
Table 1: Clinical, hemodynamic and demographic characteristics of patients (group 1).
Regurgitation tricuspid >2+. The clinical, hemodynamic and demographic characteristics are shown in table 1.
In the second part of the study were included 11 patients referred to the medical consultation, of pneumonology, pediatric cardiology and adult cardiology of the same center with presumptive diagnosis of pH, of different etiology, degree of severity and echocardiographic criteria for Perform the pulmonary vascular reactivity test. These patients were studied from July to December 2009 (Table 2).
| SEX (M/F) | 5/5 |
| AGE mean (RANGE) years | 47 (27-63) |
| Ejection fractions mean (RANGE) (%) | 55 (30-75) |
| MPAP mean (RANGE) mmHg | 27 (17-62) |
| Pulmonary capillary pressure | |
| Mean (RANGE) mmHg | 12 (8-31) |
| ≤ 12 mmHg | 8 |
| 13-19 mmHg | 0 |
| ≥ 20 mmHg | 2 |
| PVR (cat) Mean (RANGE) (WU) | 6.29 (1.25-16.4) |
| PVR (echo) mean (RANGE) (WU) | 3.20 (1.64-8.16)* |
| CO (Lt/min) mean (RANGE) | 4 (3.2-5.2) |
| RVD mean(RANGO) mm | 34 (22-55) |
| TVIrvot Mean(RANGE) cm | 13.72 (6-22) |
| Diagnostics | |
| Interatrial Communication | 2 |
| Valvular heart disease type severe mitral insuffi ncy | 2 |
| COPD+ PH severe | 3 |
| Aortic and mitral valve heart disease, double lesion type, both mild |
1 |
| Ventricular septal defect | 1 |
| Dilatation of the pulmonary artery trunk | 1 |
Table 2: Clinical, hemodynamic and demographic characteristics of
patients (group 2).
COPD=Chronic Obstructive Pulmonary Disease; PAH=Pulmonary Arterial Hypertension; PH=Pulmonal Hypertension; PVRcat=Pulmonary Vascular Resistance by Catheterization; PVReco=Pulmonary Vascular Resistance by Echocardiographic; RVD=Right Ventricular Diameter; WU=Wood Units *Calculation obtained by the equation proposed by Abbas: PVRecho=TVR/ TVIrvot x 10+0.16.
Exclusion criterion: Patients with hemodynamic instability, chronic or acute hypoxemia, coagulation disorders.
One patient was removed from the study because of the inability to perform measurements with the catheter and in 2 patients only one measurement was made. All patients in the Department of Cardiology (both stages) signed informed consent. Table 3 shows the values obtained in the 10 patients of the PVRT of the TRV/TVIrvot index, the first Abbas equation, applying the Abbas algorithm and RHC. Table 4 shows the values obtained from MPAP calculated with the Chemla equation and RHC at times 0 (t0), 30 minutes, (t30) and recovery (tR) of the test.
TRV/TVIrvot BASAL |
PVR (eco) BASAL* |
PVR (algorithm) |
PVR (cat) BASAL |
| 0.14 | 1.56 | 1.56 | 1.25 |
| 0.16 | 1.76 | 1.76 | 1.8 |
| 0.22 | 2.36 | 2.36 | 2.16 |
| 0.23 | 2.46 | 2.46 | 3.8 |
| 0.24 | 2.56 | 2.56 | 4.18 |
| 0.25 | 2.66 | 2.66 | 4.2 |
| 0.36 | 3.76 | 8.9 | 11.5 |
| 0.38 | 3.96 | 7.36 | 16.4 |
| 0.53 | 5.46 | 10 | 10.5 |
| 0.8 | 8.16 | 13.33 | 14.37 |
Table 3: Invasive and non-invasive measurements of Pulmonary Vascular
Resistance in the pulmonary vascular reactivity test.
*Obtained from the Abbas equation PVRecho=10 × TRV/TVIrvot+0.16.
| MPAPecho* t0 | MPAP Ct t0 | MPAPecho t30 | MPAP Ct t30 | MPAPecho R | MPAPCt R |
| 25 | 17 | ||||
| 30 | 23 | ||||
| 61 | 62 | 56 | 57 | 56 | 57 |
| 49 | 61 | 57 | 60 | 53 | 54 |
| 64 | 54 | 47 | 48 | 47 | 48 |
| 34 | 33 | 26 | 27 | 28 | 30 |
| 33 | 32 | 28 | 30 | 27 | 33 |
| 21 | 18 | 16 | 16 | 15 | 14 |
| 35 | 27 | 25 | 22 | 25 | 22 |
| 50 | 54 | 50 | 51 | 63 | 64 |
Table 4: Invasive and non-invasive measurements of MPAP during stages t0, t3 and recovery (tR) from PVRT.
*MPAPecho=0.61 × SPAP+1.95.
The study was approved by the Bioethics and Medical Ethics Committee of the medical institution.
The Doppler and two-dimensional measurements were performed with the Philips Sonos 7500 S3 and Philips IE33 SE1 equipment According to American Society Cardiology guidelines [20]. The TRV/TVIrvot index was determined by Doppler echocardiography using the view of the short parasternal axis at the level of large vessels. The TVIrvot (cm) was obtained with pulsed Doppler by placing the sample volume at a level of the proximal 5 mm of the pulmonary valve just before the beginning of the closing [20], and the TRV (m/s) was obtained with continuous Doppler placed in the regurgitating flow tricuspid at the valve level. It was also determined this variable in the view 4 cameras with the intention of getting the maximum velocity possible. With this and the Right Atrial Pressure (RAP), using the modified Bernoulli equation were obtained values of Systolic Pulmonary Arterial Pressure (SPAP) [21,22] to then calculate the MPAP with the equation proposed by Chemla D, et al. [23].
In both parts of the work, measurements were performed 3 times and averaged. The measurement of the Ejection Fraction (EF) was determined by the method of Simpson [20]. Measurement of the Right Ventricle Diameter (RVD) was done in the long parasternal axis by evaluating the proximal or subvalvular RVOT measured from the angle formed by the junction of the aortic ring with the basal septum and the free wall of the RV at the end of the diastole [20].
In the intensive care unit, patients in the first group [10] were placed Swan Ganz catheters arrow, 6 or 7 French (F) to obtain pulmonary pressure and flow measurements. The Seldinger technique was used to approach the Internal Jugular Vein (IJV) or Subclavia [24]. Cardiac Output (CO) was determined by the technique of thermodilution and PVR with the equation: PVR: MPAP-PCP/CO [24-27]. In the Hemodynamics laboratory, Judkins catheter 6 F was used in all patients, with femoral venous approach, guided by fluoroscopy. The PVRT was performed in the hemodynamics laboratory with central venous approach and placing, Swan Ganz catheter. 20 micrograms of inhaled illoprost were administered with simultaneous measurements of the variables of TRV, TVIrvot, MPAP. CO and Pulmonary Capillary Pressure (PCP) were obtained by thermodilution and wedging respectively. Measurements were performed at 0, 5, 10, 15, 30 minutes and recovery [28,29].
We take as a criterion of positivity of the PVRT a decrease >20% of the MPAP and the PVR without diminishing the CO [30].
We used software MedCalc statitic 2019 version 18.11.3/14.0 SPSS and Real statistics Excel. Performed linear regression analysis between the invasive method PVR measured in Woods Units (WU), and noninvasive TRV/TVIrvot in both parts of the study. This analysis was also used between the values of PVR obtained by echocardiography using the algorithm of Abbas AE, et al. [12] and the equation proposed in this work. The Pearson correlation coefficient was determined in all cases, and a regression equation was derived. The calculated values were then studied using the Bland-Altman analysis. Using the ROC curve, a cutting value was obtained for TRV/TVIrvot and PVR (catheterization) to predict high values of PVR>4.5 WU with balanced values of sensitivity and specificity [31].
The images were reassessed to quantify the reliability of the intraobserver and interobserver. The Intraclass Correlation Coefficient (ICC) was determined for variability inter and intraobservers; the relationship between the force of agreement and ICC were analyzed. The Kappa coefficient was also estimated to assess the degree of interobserver concordance.
The first group found analyzed a PCP greater than 12 mmHg was found in 7 patients. 10 patients presented left heart disease of different etiology (Table 1). The linear correlation analysis between PVRcath and TRV/TVIrvot, showed high correlation (R2 =0.95.95% CI). The equation derived from linear regression was PVRecho=10 × TRV/TVIrvot+0.36 (Figure 1).

Figure 1: Linear regression analysis between PVR by right catheterization and the ratio TRV/TVIRVOT obtained by Doppler echocardiography.
Applying the analysis of Bland-Altman, the values of PVR of this equation showed satisfactory limits in accordance with the PVRcath, with average value 0.36 (SD: 0.13-0.6) (Figure 2).
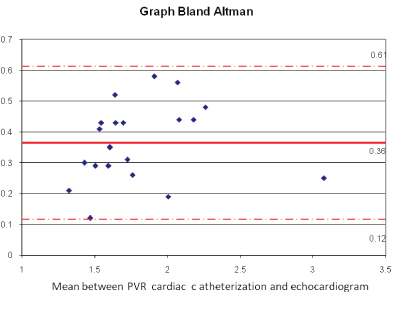
Figure 2: Analysis of Bland-Almant showing the limits of agreement between PVRCATH and PVRECHO.
In the second group analyzed (Table 2), 8 of them presented PCP equal or less than 12 mmHg, being varied the subgroups within the classification of PH accepted by ESC: 1.4.4. Congenital heart disease: interatrial communication [2], Interventricular communication [1], 2.3. Valvular: Mitral valvulopathy type severe insufficiency [2], Aortic and mitral valvulopathy type double lesion, both mild [1]. 3.1. Severe COPD+Severe PH [3] and 3.5 Diseases of pulmonary development: Dilation of the pulmonary artery trunk [1]; unlike the first group, most patients reported high PVR values for being candidate patients of the PVRT (Table 2).
In the second stage of the study, the analysis of linear correlation between PVRcath and TRV/TVIrvot basal showed good correlation (R2=0.70, 95% CI) that was exceeded by excluding the highest values of PVRcath (R2 =0.92, 95% CI) (Figures 3 and 4).
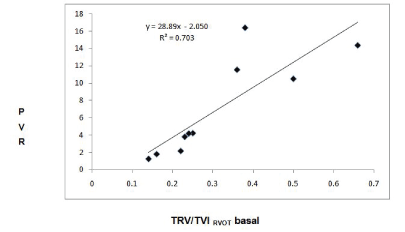
Figure 3: Linear regression analysis between the PVRCATH and the TRV/ TVIRVOT relation at the beginning of the PVRT.
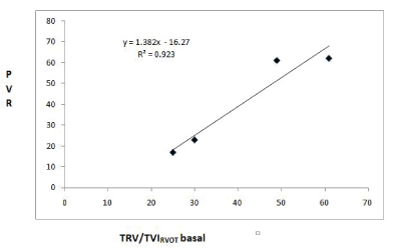
Figure 4: Linear regression analysis between the PVRCATH and the baseline TRV/TVIRVOT ratio after excluding the 4 highest values obtained by catheterization.
There was also a report of high correlation between the two methods by excluding the 3 highest values at 30 minutes of the test and in the recovery stage (R2=0.89 in both cases) (Figures 5 and 6). Prior to exclusion, the correlation coefficient was R2=0.56 with the first equation of Abbas and R2=0.64 when applying its algorithm (Figure 7).
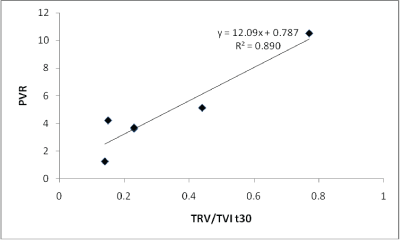
Figure 5: Linear regression analysis between the PVRCATH and the TRV/ TVIRVOT ratio obtained 30 minutes after the PVRT after excluding the 3 highest values.
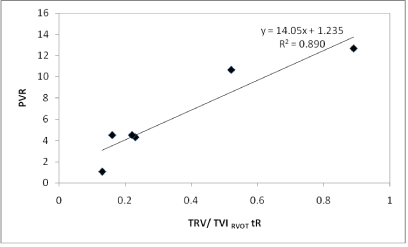
Figure 6: Linear regression analysis between the invasive PVR and the ratio TRV/TVIRVOT obtained in the recovery stage of the PVRT and after excluding the 3 highest values.
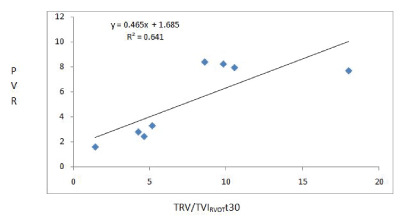
Figure 7: Linear regression analysis between PVRCATH and the VRT/ ITVRVOT relationship obtained in step t30 of the PVRT when applying the Abbas algorithm.
The Youden’s index was estimated obtaining a cut value in the ratio TRV/TVIrvot of 0.24 provides 95% sensitivity and 100% of specificity to determine PVRcath of 4.67 WU in the basal stage of the PVRT (Figure 8). Receiver Operating Characteristic (ROC) curve. In addition to the above, it shows AUC of 1.95% confidence interval between 0.692-1 and significance nivel p<0.0001 (Figure 9).
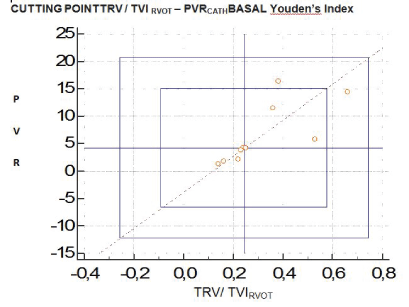
Figure 8: Cut-off value 0.24 gave 95% sensitivity and 100% specificity to determine RVPCATH>4.67 UW in the basal stage of PVRT.
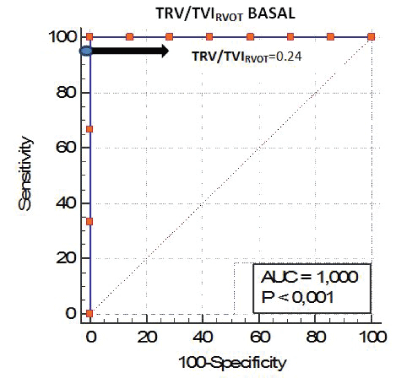
Figure 9: Receiver Operating Characteristic (ROC) curve. A TRV/TVIRVOT ratio of 0.24 (blue) and provided the best-balanced sensitivity and specificity to determine patients with PVR>4.67 WU (areas under the curve [AUC]) of 1.
We found very high correlation (R2=0.97) when comparing values obtained from PVR by the Abbas algorithm (if TRV/TVIrvot<0.275 index, PVRecho=TRV/TVIrvot × 10+0.16. If TRV/TVIrvot ≥ 0.275 index, PVRABBAS=TRV2 /TVIrvoy × 5) and the equation proposed in this work: PVRt=(TRV × RVD/TVIrvot) × Cardiac output correction factor (cfCO TVIrvot) (Figure 10). The correlation obtained when both equations were compared with the values of RHC were high (R2=0.78 and R2=0.84, respectively) (Figures 11 and 12) Bland Altman’s analysis showed satisfactory agreement limits between the methods with average differences similar between the methods (Figures 11 and 12). We obtained MPAP values by echocardiography from the formula proposed by Chemla D, et al. [23]: PMAP=0.61 × PSAP+1.95. High correlation was found in the linear regression analysis between MPAPecho and MPAPcath during times baseline, 30 minutes and recovery (t0, t30 and tR) (R2=0.87, 0.98.0.99) (I.C. 95%) (Figure 13). Bland Altman’s analysis showed satisfactory concordance limits in all cases, with average differences between the RHC of: 2, -0.75 and -1 (Figure 14). The TRVP reported negative in all patients. The CCI was 0.78 between observers and 0.90 observers with excellent agreement force. The Kappa coefficient inter observer was 0.83 with an almost perfect concordance force.
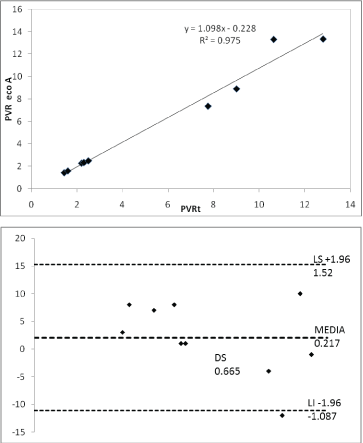
Figure 10: Linear regression analysis and Bland Atlman between the PVR obtained by the Abbas algorithm and the equation proposed in this study (PVRt).
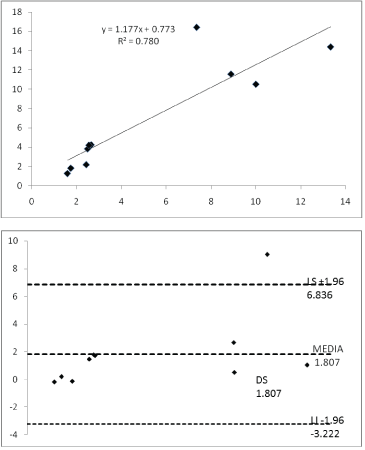
Figure 11: Linear regression analysis and Bland Altman between the PVR obtained by the Abbas algorithm (PVRa) and cardiac catheterization.
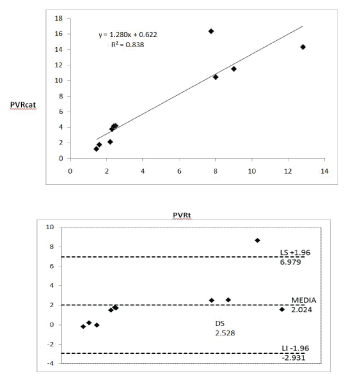
Figure 12: Analysis of linear regression and Bland Altman between the PVR obtained by the equation of this work (PVRt) and cardiac catheterization.
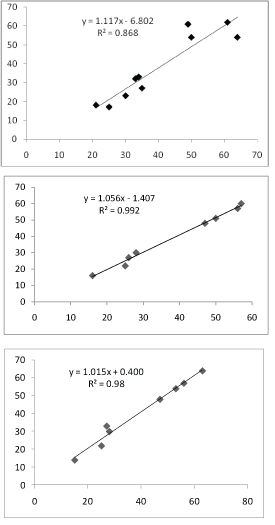
Figure 13: Linear regression analysis comparing the measurement by RHC and echocardiography [23] of the MPAP at time 0, 30 and recovery of the PVRT.
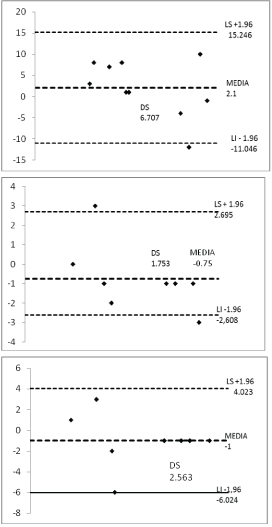
Figure 14: Bland Altman analysis showing satisfactory agreement limits between invasive and non-invasive methods [23] at the time 0.30 and recovery of TRVP.
15 years have passed since Abbas AE, et al. [11] published a simple Doppler echocardiographic equation: PVR=0.16+TRV/TVIrvot × 10. As we know, the PVR is directly related to the Pressure Gradient (∆P) and inversely with cardiac output (CO), according to this author; its equivalents echocardiographic would be represented by the TRV as a measure of pressure gradient and TVI as a Cardiac flow measurement. Unfortunately the work presented had a great limitation because it excluded all patients with moderate and severe tricuspid regurgitation representing the population that could be most favored. In successive years, emerged publications aimed at giving validity to this equation [32-36], discuss its content 16-18 or establishing different approaches and hemodynamic variables for the calculation of PVR [13-16,37,38].
One of the works proposed by another variable echocardiographic to determine the PVR is that presented by Gurudevan SV, et al. [14], they concluded that there is an inverse correlation between systolic velocity of Tricuspid Annulus (tSm) and PVR, determining that a velocity <10 cm/s equals a PVRcath>12.5 UW. Haddad F, et al. [13] proposed an index to obtain PVRecho=SPAP/(HR × TVIrvot) where a cut value of 0.076 provided 86% sensitivity and 82% specificity to determine IPVR>15 WU/m2. He also mentioned that patients with elevated values of PVR didn’t correlated well using the equation proposed by Abbas (R2=0.46).but with the lowest values yes.
An index proposed by Scapellato F, et al. [15], requires the measurement of the Pulmonary Preeyective Period (PPEP), Pulmonary Acceleration Time (PAT) and Total Systolic Time (TST) (PVR=PPEP/PAT/TST; reported high correlation with PVR obtained by catheterization Cardiac(R2 =0.96). An index>2.6 predicts a PVR>2.5 WU when the resistances are between 0-8 WU. This equation didn’t apply in the work of Haddad F, et al. [13] by low correlation (R2 =0.30).
Vlahos AP, et al. [32] conducted a prospective study in 12 patient’s candidates for liver transplantation and obtaining PVR by right catheterization. They analyzed the index TRVTVIrvot and TRV/TVIrvot corrected by the diameter of the RVOT, finding that both correlated well with PVRcath (R2 =0711 and R2=0731, respectively), even in patients with elevated values of PVR. They concluded in their study that the relationship TRVTVIrotv with a value of 0.38 can provide a specificity of 100% for PVR of 8 WU.
Opotoswky AR, et al. [17], in 2013 published a paper where they derive 2 equations to estimate the PVR from the relationship between SPAP and TVIrvot, validated these equations and compared with the equation of Abbas AE, et al. [11] (model 1). The derived models were: PVR=1.2 × SPAP/TVIrvot (Model 2) and PVR=(SPAP/TVIrvot)+3, if the systolic notch is present (Model 3). They found that model 1 consistently underestimated the PVR estimated by catheterization, especially for those with high PVR. The derivative models showed no bias, model 3 was best correlated with PVRcath (R2=0.80 vs R2=0.73 and R2=0.77 for Models 1 and 2, respectively). This approach caused discomfort in Abbas AE, et al. [11], because precisely in that year, they published an article 12 proposing a new equation: PVRecho=TRV2 /TVIrvot × 5-0.4 for patients with higher PVR who had a TRV/TVIrvot index ≥ 0.275, being this cut-off point for PVR>6 UW (ROC curve). Currently his two works have worldwide acceptance and recognition and PVRecho equation=RTV/TVIrvot × 10+0.16, is part of the list of hemodynamic variables validated and obtained by Doppler echocardiogram.
In a more current work (2017), Kaga S, et al. [16], proposed an equation based on the difference of the initial and final diastolic pressure gradient obtained by means of Pulmonary Regurgitation (PR) and CO: (early-diastolic PA-RV pressure gradient-end-diastolic PA-RV pressure gradient)/echocardiographic cardiac output. They analyzed the linear correlation between the Abbas equations (2003 and 2013) and the Scapellato equation with catheterization, obtaining correlation coefficients of 0.54. 0.66 and 0.54 respectively. The best correlation with catheterization was obtained for the equation proposed in its work (R2=0.81) followed by the index of Lindqvist (0.76) [39].
In the present work, with the first group of 20 patients, validated the usefulness of this equation, presenting a small discrepancy in the value of the correlation constant: PVRecho=TRV/TVIrvot × 10+0.36. The analysis of Bland Altman showed limits of satisfactory concordance (mean +/-0.36, L: 0.12-0.61). In the second part of the work were included 10 patients with clinical indication and echocardiographic of PVRT, analyzing mainly the recorded variations of PVR and MPAP, essential to establish the positivity of the test. The calculation of the MPAP was obtained by means of the equation proposed by Chemla D, et al. [23]: MPAP=0.61 × SPAP+1.95 and the PVR with the relationship TRV/TVIrvot to evaluate its behavior in high values of PVR.
Two relevant findings were evidenced with the calculations:
1. The measurements of MPAP obtained by this formula were sustained similar to those reported by the catheterization in all phases of measurement of the test (t0, T30 and TR) with high linear correlation (t0 R2=0.87, 0.99 and 0.98, respectively). 2. The correlation coefficient obtained when comparing the PVRecho and PVRcath values ascended from R2=0.70 to R2=0.78 when we applied the Abbas algorithm and in the cases with VRT/TVIrvoy index ≥ 0.275 it increased even more when omitting the highest values , R2=0.92 (t0), R2=0.89 (t30 and tR). The cut-off point (TRV/TVIrvot ≥ 0.275), specifies when in the linear regression analysis the correlation ceases to be linear to define the relationship between variables by an exponential growth curve, expressing the basis of the Abbas algorithm in its second work.
It’s evident analyzes these finding that the TVIrvot variable of the TRV/TVIrvot index, is responsible for opening the widest gap between invasive and non-invasive methods. Very possibly by not taking into account the dilation of the right ventricle present in all cases of patients with elevation PVR [40,41]. It’s thus that this work proposes an equation with reasoning more pathophysiologic than statistical, incorporating in its calculation. We also include a correction factor of the CO applicable in all patients according to the value of TVIrvot that we call cfCOTVIrvot suggested by the repeated observation of its decrease proportional to the degree of dilatation and systolic dysfunction of the RV. This corresponds approximately to the near value of the CO if we divide the TVI between 2 when its value is below 10 cm, above this value, we will find normal values of CO (4-6 Lt/min) allowing to standardize it to 5. At the other end, TVIrvot values below 6 would correspond to a very low CO estimate with probable severe right heart failure or shock (heart rate (CI) <2.2 lt/min/mt2).
The proposed equation is as follows:
PVRecho=[[(TRV RVD)/TVI rvot]×cfCOTVIrvot*
TVIrvot<10cfCOTVIrvot=TVIrvot/2
ifTVIrvot≥10cfCOTVIrvot=5
The linear regression analysis between the values obtained from PVR with this equation and that of Abbas with his algorithm reported a high correlation, R2=0.97, but when comparing the algorithms of Abbas, the PVRt with the RHC, we obtained a greater correlation with our proposal (R2=0.84).
Limitations: low number of patients to perform the TRVP, however it is important to note that a total of 50 measurements were made. In all cases where it is not possible to measure the TRV or TVIrvot, it will not be possible to perform the PVR calculations, not representing the case of this investigation.
In this work we conclude: 1. The algorithm of equations proposed by Abbas to determine PVR according to the relationship TRV/TVIrvot is ≥ 0275 is useful and easy to estimate [2]. The equation proposed in this work: PVRecho=(TRV × RVD/TVIrvot) × cfCOTVIrvot, is practical and applicable in all cases of pulmonary hypertension, representing an alternative to that offered by Abbas AE, et al. [13]. It’s possible to perform the PVRT, TRVP through of Doppler echocardiography based on the high correlation found in this work between the values of MPAP and PVR when compared with the invasive method and echocardiographic.
Further studies of TRVP are recommended by comparing both methods (echocardiography, RHC) to give more statistical weight and validity to echocardiographic methods and therefore, the applicability in the test.
The authors of the present work do not declare conflicts of interest.
To God for giving us life and putting us on the path where sensitive people march with a high sense of vocation and service. To Dr. Rita Tamasaukas for advice on statistical analysis, revision and correction of the manuscript. To Ing. Daniela Gálatro for her collaboration in elaborating the tables and graphs of the linear regression analysis and Bland-Almant. To the Medical team, Technicians in echocardiography and nursing who work in the Departments of Cardiology and Intensive Therapy of the University Military Hospital “Dr. Carlos Arvelo.”
Download Provisional PDF Here
Article Type: RESEARCH ARTICLE
Citation: Muñoz-Hernández TT, Hirschhaut-Schor E, Tovar-Blanco SF, Lara-Boada GJ (2019) The Age of Non-Invasive Measurements: Echocardiographic Equations Methods to Determine Variables in the Pulmonary Vascular Reactivity Test. J Surg Open Access 5(6): dx.doi. org/10.16966/2470-0991.200
Copyright: © 2019 Muñoz-Hernández TT, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access