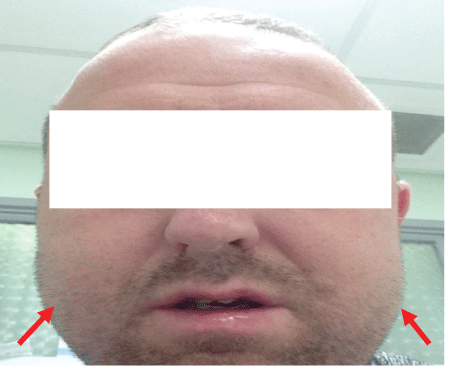
Figure 1: Cheek emphysema.

Herman A1,2 Anmolsingh R1,2 Alappatt A1 Pothula VB1 Kumar BN1*
1Department of ENT, Wrightington, Wigan and Leigh NHS Foundation Trust, UK*Corresponding author: Kumar BN, Department of ENT, Wrightington, Wigan and Leigh NHS Foundation Trust, Wigan, UK, E-mail: nirmalkumar@doctors.org.uk
Objectives: Causes of cervical and facial surgical emphysema with pneumomediastinum are uncommon but can be life threatening and need urgent management in a high dependency setting. We present a case secondary to cocaine induced hypopharyngeal perforation which was not easy to diagnose as the patient was not forthcoming with his history of cocaine use.
Clinicians should maintain a high index of suspicion when patients present with spreading cervical emphysema and also suggest an algorithm for management of non-iatrogenic subcutaneous emphysema and odynophagia.
Case summary: We presented a case report of a 39 year old man presented with three days history of sudden severe odynophagia and coughing frothy blood stained sputum. Initial chest and neck soft tissue radiograph revealed cervical surgical emphysema. After further questioning, he admitted to recent regular cocaine nasal inhalation. Subsequent CT neck and thorax showed extensive subcutaneous emphysema likely due to an esophageal perforation. This was confirmed by gastrografin swallow test, which demonstrated a posterior hypopharyngeal perforation.
The patient was managed conservatively in a HDU by keeping him nil by mouth and treatment with IV Piperacillin/Tazobactam and Clindamycin. He initially received total parenteral nutrition but subsequently refused further intravenous nutrition. He was discharged with nasogastric feeding in the community.
Follow-up swallow test two weeks following discharge showed resolution of the perforation. Subsequent to this, we developed an algorithm with an emphasis on early stabilisation and thorough assessment prior to definitive investigation to improve management.
Conclusion: Cocaine induced pharyngeal perforation is a rare but potentially life-threatening condition if left undiagnosed and without prompt and aggressive conservative treatment. Thorough history taking is vital with maintenance of high level of suspicion as the likely pathologies can be life threatening. Early involvement of multidisciplinary team advice is also critical.
Cervical surgical emphysema is a rare phenomenon, which can be attributed to both primary and secondary causes. It is frequently seen in conjunction with pneumomediastinum [1]. The presence of free air in the subcutaneous layer of the face is commonly associated with facial trauma and iatrogenic injuries, however, has not been reported, to the best of our knowledge, to present in conjunction with cervical surgical emphysema and pneumomediastinum.
We present an unusual case of cervical and facial surgical emphysema with pneumomediastinum secondary to cocaine induced hypopharyngeal perforation. While isolated surgical emphysema in one of these fascial planes has been described before, in this case surgical emphysema involved all three planes. The patient was treated conservatively and achieved complete resolution of the perforation [2-4].
Primary spontaneous pneumomediastinum is described as a benign and self-limiting phenomenon, whereas secondary pneumomediastinum has potentially life-threatening outcomes often requiring surgical intervention, depending on their precipitating factors [2].
Widely accepted pathophysiological explanations for primary cervical surgical emphysema and pneumomediastinum refers to alveolar rupture due to barotrauma causing air leakage, thus leading to free air in mediastinal and cervical fascial planes [1]. Secondary causes include trauma, iatrogenic injury, rupture of hollow viscus, and infection (e.g. necrotizing fasciitis) [2]. In the case that we present, the above mechanism did not provide adequate explanation for the patient’s presentation.
A 39 year old man with a history of depression and previous anabolic steroid abuser, presented late afternoon to the emergency department with three days history of severe worsening odynophagia, sensation of his throat ‘closing up’ and coughing frothy blood stained sputum. His initial symptoms were sudden in onset and occurred while having a boneless chicken meal. At that time, he described a sharp stabbing pain during the course of his meal while swallowing and had to immediately stop eating. He was also complaining of ptyalism (excess salivation) and was unable to tolerate both solids and liquids for the previous 12 hours. The patient presented with a tachycardia of 106 but was otherwise haemodynamically stable with no respiratory distress. Initial full blood count revealed a leucocytosis of 17 with an associated neutrophilia of 16. C-reactive proteins were within normal range.
Initial assessment by the emergency department team elicited a diagnosis of sepsis secondary to acute severe tonsillitis. A chest radiograph was obtained and initially reviewed as normal. He was then admitted under otolaryngology overnight and prescribed IV Benzylpenicillin, based on the Trust guidelines on antimicrobials for tonsillitis. IV Dexamethasone, adrenaline nebulisers and regular analgesia were also administered as he was found to be dyspnoeic and continued to report that his throat was ‘closing up’.
The patient was seen by the ENT team where a history of a recent upper right dental extraction 3 weeks prior for dental abscess was also elicited and he had recently completed a course of antibiotics. He denied any focal dental tenderness and physical examination confirmed this. Examination revealed restricted neck movement as well as widespread surgical emphysema overlying both cheeks (Figure 1), neck and supraclavicular fossa. Oral examination revealed Grade 2 tonsils bilaterally with no erythema or exudates. Flexiblenasoendoscopy examination confirmed normal appearance of the oropharynx; making a diagnosis of tonsillitis unlikely. The initial chest radiograph (Figure 2) was reviewed which demonstrated cervical surgical emphysema. However, he continued to be haemodynamically stable with no respiratory compromise. A lateral soft tissue neck X-ray (Figure 3) was taken to rule out any bony food bolus obstruction. An orthopantomogram (Figure 4) was taken and urgent maxillofacial review was sought, which ruled out any likelihood of a dental abscess.

Figure 1: Cheek emphysema.
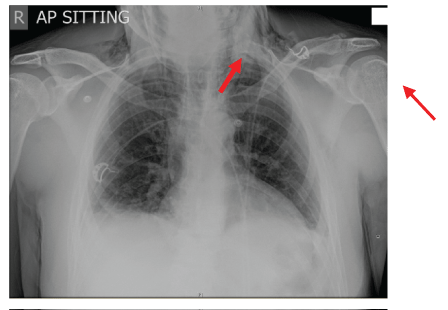
Figure 2: Subcutaneous ephysema (red arrows).
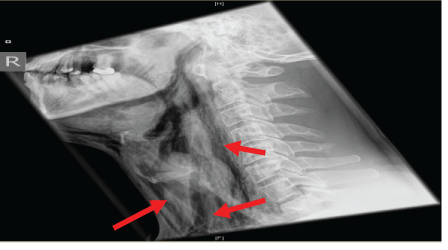
Figure 3: Soft tissue neck X Ray-severe neck emphysema.
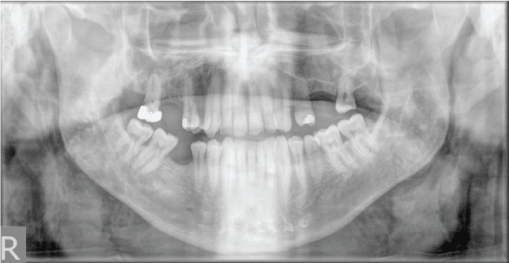
Figure 4: Normal OPG.
Further questioning revealed that he had been regularly inhaling cocaine via both nostrils over the past 2 years. He explained that recently, he started snorting it with greater effort, and noticed he could taste it at the back of throat.
He was then kept nil by mouth, his antibiotics were changed to IV Ceftriaxone and Metronidazole and a CT scan of his neck and thorax (Figure 5) was requested to investigate the source of surgical emphysema. This confirmed extensive subcutaneous emphysema likely due to an esophageal perforation.
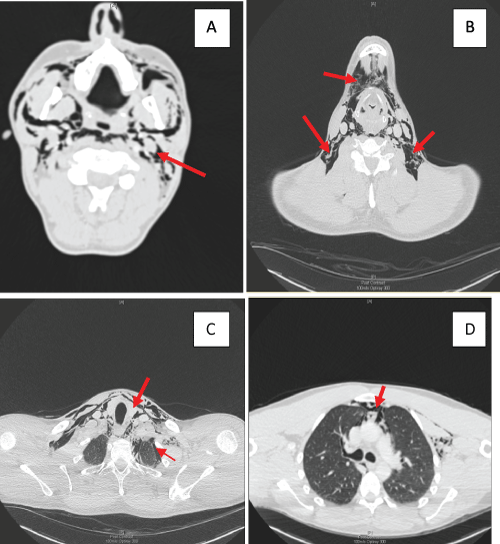
Figure 5: CT Neck and Chest with Contrast.
A and B: Extensive bilateral surgical emphysema, dissecting through the deep spaces and muscles of the neck and chest wall including parotid, submandibular, carotid and retropharyngeal spaces.
C: Trace of pneumothorax particularly in the left apex. There was no pneumopericardium.
D: Pneumomediastinum communicating via the deep spaces of the neck into superior, anterior mediastinum and posterior mediastinum surrounding the esophagus including the pretracheal space.
Water soluble contrast swallow test (Figure 6) was performed one week following his admission. Gastrografin was preferred to barium as a contrast agent due to the ongoing odynophagia and dysphagia, which might increase aspiration risk as well as chemically induced mediastinitis. The swallow test revealed a perforation of the posterior wall of the pharynx at C4/C5 into the prevertebral space and a significant aspiration of contrast despite good cough impulse.
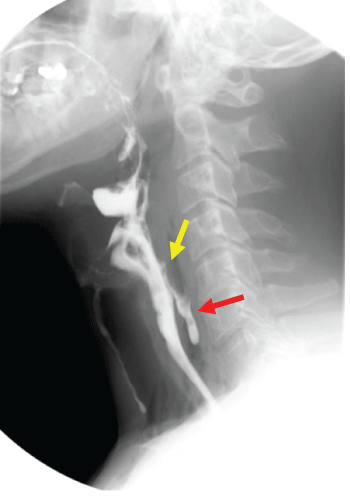
Figure 6: Gastrografin Swallow test.
Non-surgical intervention was recommended by the Upper Gastrointestinal surgeons in view of the patient’s clinical stability, small size of perforation, absence of clinical signs of mediastinitis, and the nature of tissue necrosis and vasoconstriction induced by cocaine that may impede postoperative healing. They advised a repeat swallow test to be performed at least two weeks following the initial imaging to allow adequate healing time.
The patient was admitted to the intensive care unit and continued to be kept nil by mouth for a week and treated with IV Piperacillin/ Tazobactam and clindamycin for seven days as per microbiology guidelines.
He received total parenteral nutrition via a peripheral intravenous line for the first three days but subsequently refused further intravenous nutrition.
A possible alternative to this was nasogastric feeding, but all insertion technique options posed some risks. Insertion guided by fibreoptic nasendoscopy would be ideal but the perforation site could not be visualized directly. Endoscopy guided insertion was contraindicated as it required injection of air into the aerodigestive tract. Radiologically guided insertion posed similar risks. In light of the patient’s refusal for further intravenous nutrition with the potential for deterioration in nutritional status and subsequent poor wound healing, the greater benefit of inserting a nasogastric tube blindly by an otolaryngology consultant was taken. The patient accepted the risks of this and the procedure was carried out. A chest X-ray was performed immediately following insertion but prior to use to ensure correct placement. The patient was trained on the use of the nasogastric tube and was subsequently discharged home with strict instruction of nil by mouth and nasogastric feeding in the community. He had a total inpatient stay of eleven days.
Follow-up swallow test two weeks following discharge showed a resolution of the pharyngeal perforation but a persistence in aspiration of contrast associated with weak cough impulse (Figure 7).
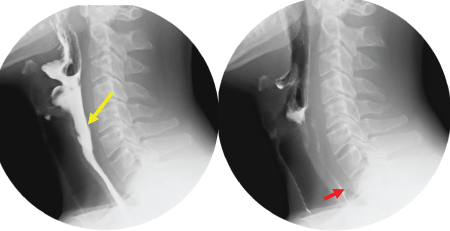
Figure 7: Follow-up contrast swallow showing resolution of perforation (yellow arrow) and persistence of aspiration (red arrow).
The patient did not attend his follow-up clinic appointment. We were informed by the community team that patient had pulled out his nasogastric tube prior to his follow-up swallow test and would not be attending any follow-up appointment as he felt an improvement (Figure 8).
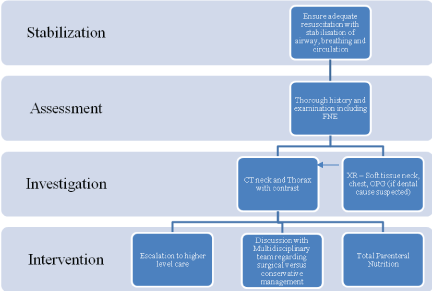
Figure 8: Algorithm for otolaryngologists managing patients presenting with non-iatrogenic subcutaneous emphysema and odynophagia.
Cocaine hydrochloride (C17H21NO4 .HCl) is an illegal Class A drug under the Misuse of Drugs Acts in the United Kingdom extracted from the coca plant Erythoxylon coca. This popular addictive recreational drug is available in two main forms: hydrochloride salt and freebase [5].
The hydrochloride salt is made by neutralisation of the alkaline cocaine base with acid and is available in powder form, which is commonly administered by intranasal ‘snorting’ or intravenously by turning it into liquid. The freebase form is made by heating the salt with substances such as ammonia and/or baking soda. As it is made without neutralisation of its alkalinity, this more volatile form provides more potent and immediate effect. A type of the freebase form is ‘crack’ cocaine, which is usually administered by smoking [5].
Cocaine induced pneumomediastinum has been documented in several case reports including both smoking inhalation and nasal insufflation method [3,4].
The commonly described pathophysiology, mainly in smoking inhalation, refers to alveolar barotrauma due to a combination of forced inspiration with a closed mouth and nose followed by the Valsalva manoeuvre to ensure maximum absorption across the alveolar-capillary barrier. This mechanism, however, inadvertently cause excessively raised intrathoracic pressure leading to alveolar rupture and release of air into the mediastinum and at times, cervical fascial layers as well [1].
The barotrauma theory, however, did not provide a sufficient explanation to the aetiology of hypopharyngeal mucosa perforation, as described in this case report. A more plausible mechanism would be the direct topical effect cocaine has on mucosal linings. The patient in this case report used cocaine via nasal inhalation only. Frequent use via forceful snorting allowed residues of the powder to build up on the posterior pharyngeal wall, which would exert a direct toxic effect to the exposed mucosal lining.
Cocaine is known to be a potent vasoconstrictor, which can induce focal areas of tissue necrosis and perforation [6]. It is, however, increasingly sold as a mixture with other compounds, also known as adulterants, to potentiate its stimulating effect and to increase the profit margin of the dealers [6,7].
Hundreds of adulterants or ‘cutting agents’ have been identified with varying levels of detrimental effects to the aerodigestive tract linings [6-8]. Kudlacek O, et al. [6] reported over 80% of cocaine retrieved from drug users in Austria from 2012 to 2015 contained 24 different substances, including Paracetamol, Phenacetine, Caffeine, Lidocaine and the anthelmintic drug, Levamisole [6].
Levamisole was discontinued for human use as an anthelmintic medication in the early 21st century and has recently gained publicity due to its reported toxic side effects and its role in some fatalities [6]. Pharmacodynamic studies have concluded that its main role as adulterant is to extend the effects of cocaine due to its longer systemic availability and lipophilic nature as it may more readily penetrate the blood-brain barrier [6,7]. Its toxic side effects ranged from hypersensitivity reaction, immunomodulation leading to vasculitis and severe agranulocytosis to vasculopathy induced direct toxicity to the heart and central nervous system, which may lead to death [8].
Lee KC, et al. [7] however, reported that most Levamisole adulterated cocaine induced symptoms will resolve following complete cessation of cocaine without requiring any intervention.
Treatment modalities for esophageal perforation varied widely and are mostly beyond the expertise of an otolaryngology department. Therefore, the involvement of the upper gastrointestinal surgeons and perhaps cardiothoracic surgeons as well are necessary.
Esophageal perforation, in general, can be treated conservatively or surgically. Surgical options ranged from simple chest drain insertion, to lateral thoracotomy for drainage of collection followed by T tube insertion into the perforation site to aid healing, to complete oesophagectomy [9].
Individual assessment of patients based on their clinical status, comorbidities, perforation site, mode of presentation and duration from perforation to presentation are recommended to decide on the appropriate treatment option.
Muir AD, et al. [9] found that patients with cervical esophageal perforation had the lowest mortality rate, which might be due to the absence of gastric content leak. They also demonstrated that aggressive conservative management, which included adequate resuscitation with keeping patient nil by mouth and administration of broad-spectrum intravenous antibiotics had similar outcome to those managed surgically [9].
Specific to our patient, as described previously, his stable clinical status, small perforation size, the isolated location at the hypopharynx and absence of significant clinical signs of mediastinitis made the conservative treatment modality preferable. The vasoconstriction leading to ischaemic mucosa surrounding the perforation would present an unfavourable environment for tissue regeneration, which is critical in surgical T tube insertion.
We suggest the following algorithm for otolaryngologists managing patients presenting with non-iatrogenic subcutaneous emphysema and odynophagia.
Cocaine induced pharyngeal perforation remained a rare but potentially life-threatening condition if left undiagnosed and without prompt and aggressive conservative treatment.
Learning points:
- Thorough history taking is vital to ascertain rare causes of severe odynophagia.
- High level of suspicion needs to be maintained in cases of surgical emphysema of unknown aetiology as the likely pathologies can be life threatening.
- Early involvement of multidisciplinary teams for advice regarding conservative versus surgical management.
Download Provisional PDF Here
Article Type: CASE REPORT
Citation: Herman A, Anmolsingh R, Alappatt A, Pothula VB, Kumar BN (2019) Cocaine Induced Pharyngeal Perforation-an Unusual Case Presentation of Facial and Cervical Emphysema with Pneumomediastinum. J Surg Open Access 5(1): dx.doi.org/10.16966/2470-0991.177
Copyright: © 2019 Herman A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access