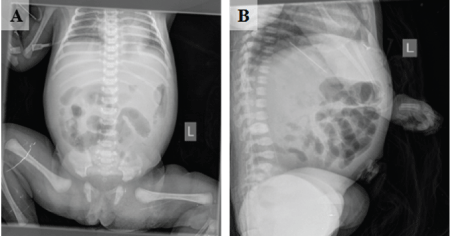
Figure 1: (A&B) X-ray abdomen was unremarkable. Part of the intestine dilated and inflated, and some of the intestines of the left abdomen showed bean like changes.

Kun Wang Jing Cai Xiao Wei Li, Guo Min Zhai Ying Chou Lu Wei Bing He Xiong Sheng Guo Gang Quan Wu*
Dongguan Maternal and Child Health Hospital, Guangdong, China*Corresponding author: Gang Quan Wu, Dongguan Maternal and Child Health Hospital, Guangdong, China, E-mail: mmwgq71@126.com
Background: Gastric duplication is an extremely rare digestive tract malformation with an incidence rate of approximately 17 cases per million, accounting for 2-8% of all digestive tract duplications. Infants the disease lacks obvious symptoms. The incidence of acute cases rarely reported in the neonatal period. Through a review of this case and the historical literature we have accumulated valuable surgical and clinical experience in the treatment of this acute disease.
Case presentation: In this case report, the patient presented with abdominal distension, abdominal pain, fever, vomiting at one week after birth, abnormal abdominal masses were identified by color Doppler ultrasound and X-ray. In order to make a further diagnosis, we performed abdominal puncture on the side of the bed. Through the nature of the peritoneal puncture fluid, we identified the indication of emergency operation in the children. In the operation we found a large amount of brown liquid was identified in the abdominal cavity. A mass was identified in the greater curvature adherent to the transverse colon. That was difficult to separate from the surrounding tissues. The cyst was encased in the greater omentum, and perforation was identified after adhesion separation. The diagnosis of gastric duplication was confirmed by surgery and pathology.
Conclusion: Gastric duplication is an extremely rare digestive tract malformation especially in newborns. Not all gastric duplications are accompanied by obvious clinical symptoms and this condition is typically detected upon examinations. Preoperative diagnosis by ultrasound and X-ray and abdominal puncture facilitated urgent treatment in this case. Surgery is an effective treatment for gastric duplication. The wide local resection of the gastric mass and the cysts performed in this case achieved satisfactory results. Abdominal puncture, as an effective auxiliary examination, plays an important role in the management of neonatal acute abdomen. It also reminds the pediatric surgeon that all kinds of methods should be used in the treatment of neonatal acute abdomen to save lives.
Gastric duplication; Intestinal duplication
Gastric duplication is a rare condition [1-3] accounting for approximately 7% of all gastrointestinal duplication cysts. We report interesting clinical manifestations that were diagnosed with as a gastric duplication cyst.
A 7-day-old girl was admitted to the emergency department with abdominal distension, fever, poor appetite, gain and non-bilious, non-projectile vomiting for two days. The obvious improvement was not achieved after anti-inflammatory treatment for one day. Then, the patient was transferred to our hospital. When admitted, the child was febrile (38.2 degrees). An abdominal examination revealed tenderness and guarding. An abdominal X-ray was unremarkable (Figure 1). Ultrasound imaging revealed a large heterogeneous hypoechoic lesion (26 × 23 mm) adjacent to the duodenum and walled off by the greater omentum (Figure 2). After the brownish-green liquid was drained via an abdominal puncture, the child was sent for emergency surgery. A large amount of brown liquid was identified in the abdominal cavity. A mass was identified in the greater curvature adherent to the transverse colon. That was difficult to separate from the surrounding tissues. The cyst was encased in the greater omentum, and perforation was identified after adhesion separation (Figure 3). A large amount of pus was found in the omental bursa. Wide local resection of the gastric mass along with the cyst was performed. The stomach wall was sutured in layers. The specimen was sent for histopathological examination. The gastric tubes were removed 10 days after surgery, the patient defecated 2 days after surgery and were discharged 17 days after surgery. The operative recovery was uneventful. Histopathological examination revealed gastric mucosa and smooth muscles in the wall of the cyst, which confirmed the diagnosis of a gastric duplication cyst (Figure 4). No incision infection, intestinal obstruction, bleeding or other gastrointestinal complications, such as leakage, occurred in this patient. At the follow-up visit two months later, the patient was asymptomatic and thriving.

Figure 1: (A&B) X-ray abdomen was unremarkable. Part of the intestine dilated and inflated, and some of the intestines of the left abdomen showed bean like changes.
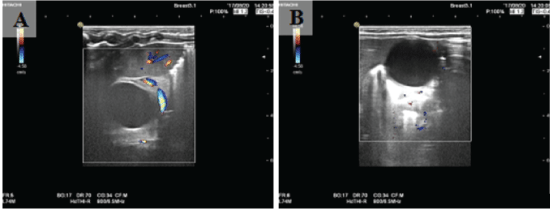
Figure 2: (A&B) Ultrasound showed a large heterogenous hypoechoic lesion 26 × 23 mm adjacent to the duodenum, walled off by greater omentum.
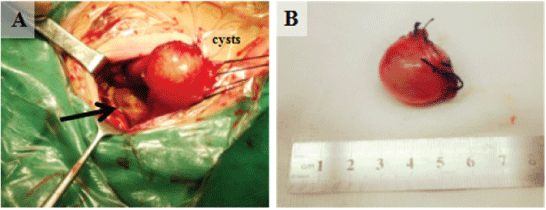
Figure 3: (A) The cysts were gradually separated by thread pulling. A large amount of pus (indicated by the arrow) was found in the omental bursa. (B) Mass resected by open surgery in the case. The size of the mass was approximately 2.5 × 2.0 × 2.5 cm, and the wall was complete.
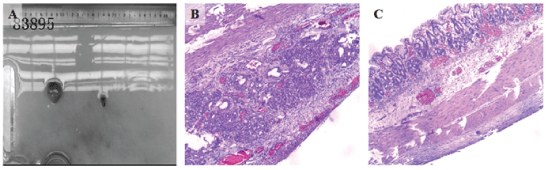
Figure 4: (A) The specimen is collected; the whole body is fixed in formalin. (B&C) Histopathological examination revealed gastric mucosa and smooth muscles in the wall of cyst which confirmed the diagnosis of gastric duplication cyst.
Gastric duplication is a rare malformation of the digestive tract [1- 3]. Techniques for prenatal diagnosis of this disease have developed rapidly; therefore, abnormal abdominal masses can be detected during the fetal period in most fetuses by color Doppler ultrasound. As an effective and non-invasive method, color Doppler ultrasound is a useful examination. However, not all gastric duplications are accompanied by obvious clinical symptoms (e.g., vomiting of bile-free fluid, epigastric pain, and masses, etc.) that can be detected. Therefore, surgical exploration and pathological diagnosis are required; thus a preoperative diagnosis can become challenging.
Furthermore, cystic lesions can be identified via B ultrasound, CT and MRI, which can be utilized to determine the location and size of the lesion and the relationship between the lesion and adjacent tissues [3]. Although the pathology report is required for a final diagnosis, as it is the gold standard; it is always useful to explore the gastric muscle tissues or gastric wall structures in the cyst tissue, and even ectopic pancreatic tissues [4-8].
To our knowledge, this is the youngest patient with a gastric duplication cyst treated by surgery (Table 1). Complete resection remains the most effective treatment for the disease [9]. The operation is complex due to the location and size of the cyst and its relationship to the surrounding tissues. In recent years, laparoscopic technology has developed, rapidly. Studies using this technique have been performed and some have reported a good prognosis [10]. Nevertheless, some controversies, such as the possibility that gastric duplication can transform into malignancy still exist [7]; several pediatric cases with small gastric duplication cysts treated by laparoscopic resection have been reported [14-16,27]. However many scholars suggest that open surgery can provide better surgical fields to completely resect the cyst, thereby reducing the recurrence and canceration rate [11]. According to our previous reports, open surgery is preferable to laparoscopic surgery, but laparoscopic surgery is common in pediatric surgery
| No. | Sex | Age | Complaints | Size (cm) | Surgery | Ref |
| 1 | M | 2 years | AM | Unknown | Open | Gupta AK, et al. [9] |
| 2 | F | 6 years | AM | Unknown | Open | Gupta AK, et al. [9] |
| 3 | M | 4 years | AP, AM, GH | Unknown | Open | Blais C, et al. [10] |
| 4 | F | 14 years | non-bilious projectile vomiting, AM | Unknown | LP | Sasaki T, et al. [11] |
| 5 | F | 24 years | AM | 5 | LP | Tayar C, et al. [12] |
| 6 | M | 2 months | AM | Unknown | LP | Ford WD, et al. [13] |
| 7 | M | 2 years | hemoptysis | Unknown | Open | Menon P, et al. [14] |
| 8 | M | 6 years | AP, AM | 8 × 6 | Unknown | Rodrı´guez CR, et al. [15] |
| 9 | M | 2.5 years | perforation and malignancy | 8 | Open | Tatekawa Y, et al. [16] |
| 10 | F | 82 years | hematemesis | 8 | Open | Klimopoulos S, et al. [17] |
| 11 | M | 1 month | non-bilious projectile vomiting, AM | Unknown | Open | Hishiki T, et al. [18] |
| 12 | M | 50 years | non-bilious projectile vomiting | Unknown | Unknown | Fukumoto K, et al. [19] |
| 13 | F | 2.2 years | non-bilious projectile vomiting | 10 × 7 × 4 | Open | Stock F, et al. [20] |
| 15 | F | 14 years | AP, AM | 4.5 × 5.5 × 3.7 | Open | Ordeanu C, et al. [21] |
| 16 | F | 10 months | non-bilious projectile vomiting, AM | 8 × 6 | Unknown | G KK, et al. [22] |
| 17 | F | 11 days | non-bilious projectile vomiting | Unknown | Open | Chin AC, et al. [23] |
| 18 | F | 2.5 years | GH, CWM, EF | 4 × 5 | Open | Kesieme EB, et al. [24] |
| 19 | F | 25 years | AM | Unknown | Open | Samona S, et al. [25] |
| 20 | M | 2 months | non-bilious projectile vomiting | 8 × 3 × 3 | LP | Takazawa S, et al. [26] |
| 21 | M | 1 month | vomiting and high-grade fever | 2.0 × 1.5 | Open | Qinghua L, et al. [27] |
| 22 | F | 7 days | AD, AP, fever, non-bilious projectile vomiting | 2.6 × 2.3 | Open | Present study |
Table 1: Summary of gastric duplication cyst.
Although gastric duplication is a rare digestive tract malformation; an increasing number of cases have been diagnosed using innovative technologies, which has even made a diagnosis in the fetal period possible. The typical clinical features of the disease include a cystic mass in the upper abdomen, vomiting, and fever, which have been discussed in many case reports. Changes in the gastric wall are occasionally found via upper gastrointestinal radiography. Gastric duplication has a possibility of malignant transformation [11].
Surgery is an effective method, however, open surgery or laparoscopic surgery is as effective as controversial treatment. We suggest that the choice of surgical approach is closely related to the location, size, and tissues surrounding the cyst. Children with clinical symptoms should undergo surgical treatment. Surgical treatments can be delayed for asymptomatic gastric duplication in neonates, however, a chance of malignant transformation is noted, and neonates should also undergo regular follow-up and elective surgical treatments [28- 29]. The associated mechanism of malignant transformation of gastric duplication cysts remains unclear, and further investigations are required.
In addition, cases exhibit similarities and differences. Time is important, especially for newborns. We believe that surgery is an effective treatment for gastric duplication. Clinical, laboratory and radiographic factors should all be considered when making a decision regarding treatment for gastric duplication. Based on our summary of reports in the literature (Table 1), four clinical features- abdominal distension, abdominal pain, fever, and a history of vomiting-are predictive of the need for operative intervention during the patient’s hospital stay and should be weighted heavily in the decision-making algorithm for operative versus non-operative treatment.
This research did not receive any specific grants from funding agencies in the public, commercial, or not-for-profit sectors.
Kun Wang and Jing Cai drafted the manuscript, and Gangquan Wu supervised the writing of the manuscript. Xiaowei Li, Guomin Zhai, and Yingchou Lu performed the perioperative management of the patient. Kun Wang and Gangquan Wu performed the operation. Weibing He and Xiongsheng Guo supervised the management of the patient. All authors read and approved the final manuscript.
Not applicable
Written informed consent was obtained from the family of the patient for the publication of this case report.
The authors declare that they have no competing interests.
We would like to thank the patients for their participation in this project. Thanks to other authors for contribution to this case. All authors read and approved the final manuscript.
Download Provisional PDF Here
Article Type: CASE REPORT
Citation: Wang K, Cai J, Li XW, Zhai GM, Lu YC, et al. (2018) Diagnosis and Treatment of Gastric Duplication in Neonates-A Case Report and Review of the Literature. J Surg Open Access 4(4): dx.doi.org/10.16966/2470-0991.174
Copyright: © 2018 Wang K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access