Abstract
Background: Video-assisted thoracoscopic surgery (VATS) lobectomy is a minimally invasive anatomic lung resection that has been
associated with decreased pain and hospital stay compared to open resection. However, with the higher costs of disposable VATS instruments it
is unclear whether or not the overall hospital costs are equivalent. The objectives of this study are to compare the overall in-hospital costs of VATS
to open lobectomy and assess the financial impact of performing VATS lobectomy procedures in a Canadian tertiary care hospital.
Methods: A retrospective cost analysis was done comparing 78 VATS to 151 open lobectomies. Intraoperative costs, postoperative costs,
total costs and length of hospital stay were compared. A regression analysis was done adjusting for age, gender, tumor size and tumor stage.
Results: The mean intraoperative, postoperative and total costs for VATS and open lobectomy were $4,770 and $2,166 (p=0.01), $3929 and
$5,604 (p<0.0001), and $8,499 and $7,771 (p=0.3), respectively. The median hospital stay for VATS and open lobectomy were 4 and 5 days
(p<0.0001), respectively. The mean intraoperative costs of VATS lobectomy in the first and second 39 VATS lobectomies were $4894 and $4246
(p = 0.003), respectively.
Conclusions: The total cost of VATS lobectomy is equivalent to open lobectomy. Increased cost of disposables and longer operating time
account for higher intraoperative cost of VATS lobectomy. A shorter hospital stay and lack of requirement for the acute pain service (APS) reduce
the postoperative cost of VATS. The intraoperative costs of VATS lobectomies decrease with experience.
Keywords
VATS; Thoracoscopic; Pulmonary resection; Cost analysis; Health economics
Introduction
Video-assisted thoracoscopic surgery (VATS) lobectomy is a minimally
invasive approach for anatomic resection of a lobe most often used for
surgical management of non-small cell lung cancer (NSCLC) and has
replaced traditional open lobectomy in many centers. Previous studies
have shown that overall and disease-free survival are equivalent for both
approaches, with less patient morbidity and shorter hospital stay with the
VATS approach [1,2]. However, cost differences between VATS and open
lobectomy may be significant. Each VATS lobectomy procedure requires
use of expensive disposable instruments such as staplers, cartridges and
retrieval bags, as well as longer operative time due to the higher technical
complexity of the procedure. However, VATS lobectomy has a shorter
postoperative hospital stay.
Previous literature shows conflicting results when comparing the
cost of open lobectomy to VATS lobectomy. Some studies have shown
decreased cost with VATS [3,4] while others demonstrate cost equivalence
[5-7]. To date there has not been a cost-analysis study of VATS versus
open lobectomies in a Canadian health care institution. Given our
single-payer, government-funded healthcare system and its inherent
economic constraints, it is important to analyze global hospital costs when
introducing new surgical techniques to see if there are overall differences
in cost over standard approaches.
Patients and Methods
Ethics approval for this study was granted by the Capital District
Health Authority’s research ethics board. All lobectomies performed at
the QEII Health Sciences Center in Halifax, Nova Scotia, Canada over an
18 month period were reviewed. All open lobectomies were performed
for biopsy proven or presumed NSCLC. Lobectomies which followed a
wedge resection with intraoperative frozen section were included. Cases
where the major vessels and bronchus were not individually identified and
divided were excluded. Four surgeons participated in the study. All VATS
lobectomies were either performed by one surgeon or proctored cases
where the surgeon was teaching another surgeon. Patient demographics,
tumor size and stage were recorded.
Surgical approaches
At our institution VATS lobectomy was performed using two to three 5
-12 mm ports and a 3 to 4 cm utility incision with no rib spreading. A 10
mm 30 degree video thoracoscope was utilized. All vessels were divided
with an endostapler (Ethicon ATS flex or Covidien Endo-GIA) with a
white, gray or tan load (2.5 mm staples). The bronchus was divided with
a blue/purple load (3.5 mm staples) or green load (4.8 mm staples). The
fissure was completed using multiple firings of an endostapler with a green,
blue or purple load. The specimen was always removed in an Ethicon
Endopouch or Cook LapSac bag. Systematic lymph node dissection and
sampling was routinely performed. Paravertebral or epidural catheters
were not routinely used in VATS lobectomy cases.
Open lobectomy was performed using a fifth interspace posterolateral
thoracotomy with or without rib resection. The majority of vessels were
suture ligated but linear and right-angle staplers were occasionally used at
the surgeon’s discretion. The bronchus was divided with a TA-30 stapler
with a green load. Systematic lymph node dissection or sampling was
routinely performed. A paravertebral block was routinely placed at the
end of the operation.
Post-operative care
Following either VATS or open lobectomy, all patients were monitored
at least one night in an intermediate care unit (IMCU). Patients were
transferred to a ward bed the following morning if deemed to be stable by
the surgical team. Open lobectomy patients were followed by the acute pain
service (APS) for pain management with a paravertebral block or a patientcontrolled
analgesia (PCA) pump. Generalized criteria for removal of chest
tube were less than 300 milliliters drainage over 24 hours with no air leak.
Outcomes
The primary study outcomes were mean intraoperative, postoperative
and total cost of VATS and open lobectomy and median days in hospital.
Secondary outcomes included mean operating theatre time (the time the
patient was in the operating theatre including anesthesia time), mean
operating time (start of surgery until completion of skin closure), median
number of stapler cartridges used, median days in an IMCU and ward
bed, median days requiring a chest tube and APS, number of patients
requiring transfusion of blood products, ICU stay, take back to the OR
and/or a readmission within 30 days, and the number of patients having
a prolonged air leak (defined as requiring a chest tube for greater than 5
days). Primary and secondary outcomes were all compared using either
Student t-test (means), Wilcoxon test (median), or Fisher’s exact test
(proportions). Univariate regression analysis was used to adjust for age,
gender, tumor size and tumor stage.
Cost calculation
All costs were reported in Canadian dollars (CDN), which traded at
approximately par to the United States dollar (USD) during the study
period. Intraoperative costs were computed by summing the cost of
operating theatre time, anesthesia costs, and cost of disposables (eg.
stapling devices and retrieval bags). The average cost of the thoracic
operating theatre was $3.65 per minute, which included nursing costs,
standard operating room equipment, medications and supplies. The cost
for anesthesia was $16.40-32.80 per 15 minute time interval after an initial
fee to induce anesthesia ($213.20). The cost of disposables for VATS and
open lobectomy are listed in tables 1 and 2, respectively. Post-operative
costs were computed by summing the average cost of days in ICU, IMCU
and on the ward, as well as the days followed by APS (Table 3). The days
with a chest tube, return to the operating room during hospitalization, and
readmission within 30 days were also recorded. If a patient returned to the
emergency department or required readmission within 30 days of their
lobectomy, these costs were added to the postoperative cost. A secondary
analysis was performed to compare the first half of VATS lobectomies to
the second half to look at the impact of a “learning curve” on cost.
Instrument |
Cost |
Ethicon ATS45 handle |
384.51 |
Ethicon ATS45 reload (white) |
154.20 |
Ethicon ATS45 cartridge reload (blue/green) |
143.98 |
Ethicon Echelon 60 handle |
426.66 |
Ethicon Echelon cartridge reload (all) |
198.09 |
Covidien Tristaple handle |
195.50 |
Covidien EndoGIA45 reload (purple) |
227.37 |
Covidien EndoGIA45 reload (tan) |
221.05 |
Covidien EndoGIA60 reload (purple) |
276.05 |
Covidien EndoGIA60 reload (tan) |
277.35 |
Ethicon Endopouch 10 mm SpecimenRetrieval Bag |
79.75 |
Table 1: Cost of disposables for VATS lobectomy (all costs are in Canadian
dollars)
Instrument |
Cost |
Ethicon TLC75G stapler |
167.08 |
Ethicon TLC75G reload |
95.77 |
Ethicon TX30V stapler |
138.34 |
Ethicon TX30V reload |
56.56 |
Ethicon TX30G stapler |
119.43 |
Ethicon TX30 reload |
49.21 |
Ethicon TX60G stapler |
127.95 |
Ethicon TX60 reload |
63.19 |
Table 2: Cost of disposables for open lobectomy (all costs are in Canadian dollars)
Expense |
Cost |
ICU bed (per day) |
1938 |
IMCU bed (per day) |
945 |
ward bed (per day) |
525 |
APS (initial consult) |
252 |
APS (per day) |
175.56 |
Table 3: Postoperative costs (all costs are in Canadian dollars)
Results
A total of 78 VATS and 149 open lobectomies were performed during
the study period. Patient demographics, pathological tumor stage and
the operations performed are summarized in table 4. While the majority
of lobectomies were performed for proven or presumed NSCLC, three
patients (3.8%) in the VATS group (final pathology showing colorectal
metastasis in two cases and breast metastasis in one case) and 12 patients
(8.1%) in the open group (final pathology showing colorectal metastasis
in four cases, renal cell metastasis in three cases, endometrial metastasis
in one case, adenocarcinoma in situ in one case, lymphoma in one case,
tuberculosis in one case and fibrosis in one case) did not have NSCLC on
final pathology. One VATS lobectomy was converted to open lobectomy
and this was included in the cost analysis as a VATS lobectomy.
Factor |
VATS Lobectomy (n=78) |
Open Lobectomy (n=149) |
p-value |
| Male: Female |
35:43 |
66:83 |
0.93 |
| Mean age (years) |
67.4 |
66.1 |
0.29 |
| Mean tumor size (cm) |
2.7 |
3.0 |
0.20 |
| Pathologic Stage |
|
|
0.16 |
| Pathologic Stage I |
54 (69.2%) |
87 (58.4%) |
|
| Pathologic Stage II |
16 (20.5%) |
26 (17.4%) |
|
| Pathologic Stage III |
5 (6.4%) |
23 (15.4%) |
|
| Pathologic Stage IV |
0 (0%) |
1 (0.7%) |
|
| Stage not applicable |
3 (3.8%) |
12 (8.1%) |
|
| Operation |
|
|
0.15 |
| RUL lobectomy |
32 (41.0%) |
52 (39.9%) |
|
| RML lobectomy |
6 (7.7%) |
11 (7.4%) |
|
| RLL lobectomy |
12 (15.4%) |
21 (14.1%) |
|
| LUL lobectomy |
19 (24.4%) |
43 (28.9%) |
|
| Segmentectomy |
3 (3.8%) |
0 (0%) |
|
| LLL lobectomy |
6 (7.7%) |
19 (12.8%) |
|
RML & RLL
bilobectomies |
0 (0%) |
3 (2.0%) |
|
Table 4: Patient demographics, tumor staging and operations performed
Primary outcomes
The primary outcomes are given in table 5. The mean intraoperative,
postoperative and total costs for VATS and open lobectomy were $4,770
and $2,166 (p=0.01), $3929 and $5,604 (p<0.0001), and $8,499 and
$7,771 (p=0.3), respectively. The median hospital stay for VATS and open
lobectomy were 4 days and 5 days (p<0.0001), respectively. A regression
analysis controlling for age, gender, tumor size and stage showed the
adjusted difference in mean intraoperative, postoperative and total costs
were $2413.45 (p<0.0001), $1792.15 (p=0.01) and 621.29 (p=0.37),
respectively, suggesting there was no statistically significant difference
between the adjusted and unadjusted costs.
Outcome |
VATS |
Open |
p-value |
Mean intraoperative cost
(Canadian dollars, range) |
4570
(3709-8486) |
2167
(1233-4807) |
<0.0001 |
Mean postoperative cost
(Canadian dollars, range) |
3929
(1470-26,220) |
5605
(2529-60,078) |
0.01 |
Mean total cost
(Canadian dollars, range) |
8499
(4303-30,937) |
7771
(4354-62,707) |
0.3 |
| Median days in hospital (days, range) |
4
(2-73) |
5
(3-31) |
<0.0001 |
Table 5: Primary outcomes
Secondary outcomes
The secondary outcomes are given in table 6. Operating time for VATS
was significantly longer than open lobectomy. No difference was found
for length of stay in the IMCU for VATS and open lobectomy patients.
One patient in the open lobectomy group transferred directly from the
ICU to an outside institution and therefore did not require an IMCU or
ward stay. Patients in the VATS group did have a significantly shorter ward
stay. APS was not routinely used for VATS patients; however this service
was generally used following open lobectomy. Therefore the difference in
median days required of this service is significant between the two groups.
Outcome |
VATS |
Open |
p-value |
| Mean operating time (mins, range) |
213 (117-378) |
170 (77-540) |
<0.0001 |
| Mean theatre time (mins, range) |
277 (191–499) |
225 (123–714) |
<0.0001 |
| Median cartridges (number, range) |
11 (5-34) |
5 (1-14) |
<0.0001 |
Requiring ICU
(patients, percentage) |
2 (2.6%) |
5 (3.4%) |
1 |
Median days in IMCU
(days, range) |
1 (1-8) |
1 (0-11) |
0.22 |
| Median days in ward bed (days, range) |
3 (0-67) |
4 (0-17) |
<0.0001 |
| Median days of APS (days, range) |
0 (0-5) |
4 (0-6) |
<0.0001 |
| Median days of chest tube (days, range) |
3 (1-35) |
4 (1-37) |
<0.0001 |
pRBC transfusion (patients,
percentage) |
3 (3.9%) |
15 (10.1%) |
0.1238 |
| Prolonged air leak (patients, percentage) |
13 (16.7%) |
25 (16.8%) |
1 |
| Second operation (patients, percentage) |
2 (2.6%) |
4 (2.7%) |
1 |
| Re-admission (patients, percentage) |
3 (3.9%) |
4 (2.7%) |
0.69 |
Table 6: Secondary outcomes
There was a shorter duration for chest tubes in the VATS patients, however
no difference was found in the number of patients with prolonged air leak.
The intraoperative costs between the first and second 39 VATS
lobectomies were found to be significantly different (Table 7). However,
no difference between the postoperative and total costs was found. Figure 1
is a plot of the two main variables contributing to intraoperative costs:
theatre time and disposable endostapler cartridges. The graph shows that
the cost of both variables decreases with experience. Lines of best fit for
both cartridges and theatre time shown on the graph demonstrate that the
reduction of endostapler cartridges with increased experience contributed
the most to reducing the intraoperative costs for VATS lobectomy.
Outcome |
First VATS Lobectomies (39) |
Second VATS Lobectomies (39) |
p-value |
Mean intraoperative cost
(Canadian dollars, range) |
4894
(2782-8486) |
4246
(2709-6942) |
0.003 |
Mean postoperative cost
(Canadian dollars, range) |
4123
(1470-12,385) |
3736
(1470-26,220) |
0.64 |
Mean total cost
(Canadian dollars, range) |
9017
(4303-17,054) |
7982
(4587-30,937) |
0.23 |
| Median days in hospital (days, range) |
5
(2-21) |
4
(2-73) |
0.01 |
Table 7:Comparison of the primary outcomes between the first and second 39 VATS lobectomy cases
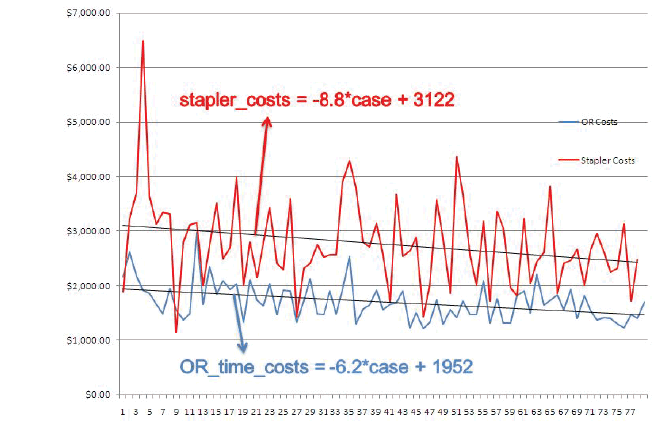
Figure 1: A plot of the cost of staplers (red) and operating time (blue)
with experience. The line of best fit is steeper for the cost of staplers,
suggesting use of fewer cartridges with experience contributed the
most to reducing intraoperative costs.
We further analyzed these two variables to compute the theoretical
optimal use of theatre time and disposable endostapler cartridges for
VATS lobectomy. Two scenarios were created where the intraoperative
cost of VATS equaled the intraoperative cost of open lobectomy. In the first
scenario the theatre time was minimized and the maximum number of
endostapler cartridges was computed. In the second scenario, the number
of endostaplers cartridges was minimized and the maximum theatre time
was computed. Using the minimum theater time for a lobectomy in our
study (123 minutes for an open lobectomy) as the theatre time for a VATS
lobectomy, a maximum of six endostapler cartridges can be used. If the
minimum number of endostapler cartridges in our study (five) were used
for a VATS lobectomy, the maximum theater time that can be used is 161
minutes.
Discussion
In the adoption of new surgical technology or techniques, it is essential
that comparison be made to the pre-existing standard of care. While
numerous studies have evaluated VATS versus open lobectomies in terms
of postoperative pain, morbidity and survival [1,2], relatively fewer studies
have analyzed cost differences between the two techniques. With health
care resources increasingly strained by a growing elderly population
and global economic uncertainty, cost differences become paramount to
analyze. In particular, the Canadian, single-tier, government funded public
health care system is especially vulnerable and cost containment must be
made whenever possible. Detailed cost analysis studies are essential to
guide institutional decision-making prior to adoption of newer surgical
techniques.
Intraoperative cost
Consistent with previously published literature [3,5-7] our study
showed that intraoperative costs were significantly higher for VATS
lobectomy compared to open resection, mainly due to longer operating
time and use of disposable instruments. Furthermore, the introduction of
VATS lobectomy in an institution inherently includes a surgeon learning
curve. Improvements in the cost of VATS with experience have been
reported in previous studies [4,6,8]. There was a significant difference
between the intraoperative cost between the first and second 39 VATS
lobectomies. The intraoperative cost decreased due to a reduction in
both theatre time and use of fewer stapler cartridges, with a larger impact
on cost resulting from decreased cartridges as illustrated in figure 1.
Our analysis of optimizing theater time and endostapler cartridge use
provides helpful benchmarks for surgeons to achieve in order to make
intraoperative VATS costs more equivalent to open resection. With more
judicious use of disposable instruments (eg. dividing multiple vessels
with a single cartridge firing), one can realize ongoing cost savings with
increased VATS experience.
Postoperative cost
The postoperative costs of open lobectomy were higher due to longer
surgical ward stay and higher use of APS. Table 8 shows no difference in
the days in IMCU between VATS and open lobectomy groups; however,
open lobectomies stayed in hospital longer. Most open lobectomies
have paravertebral catheters and are followed by APS for a median of
4 days, while the majority of the VATS lobectomy patients only require
intermittent intravenous and oral analgesics managed by the surgical
team, resulting in significant cost savings for VATS.
Outcome |
1st VATS
Lobectomies (39) |
2nd VATS
Lobectomies (39) |
p-value |
Mean operating time (min, range) |
236 (132–378) |
189 (117–310) |
0.0003 |
Mean theatre time (min, range) |
301 (208-499) |
253 (191-366) |
<0.0001 |
Median no. cartridges (count, range) |
13.5 (5-34) |
11.1 (6-20) |
0.01 |
Mean theatre costs
(Canadian dollars, range) |
1840 (1301–2988) |
1565 (1206–2207) |
0.0003 |
Mean stapler costs
(Canadian dollars, range) |
2951 (1145–6484) |
2592 (1423–4360) |
0.05 |
Table 8: Comparison of the secondary outcomes between the first and
second 39 VATS lobectomy cases
Total cost
Our study found no significant difference between the total in-hospital
cost of VATS and open lobectomy, which is consistent with the majority
of the previous studies [5-7]. Retrospective cost-comparison studies in
Europe [5] and Asia [6] demonstrate that VATS lobectomies are associated
with shorter hospital stay, but intraoperative costs are significantly higher
compared to open lobectomy. Ultimately, these studies showed no
difference in the total cost between the two techniques. An older study
in Japan [9] and a more recent retrospective study in France [3] found
total cost of VATS to be lower than open lobectomy. However, a significant
portion of the cost difference in the study by Ramos et al. is due to the fact
that most VATS lobectomy patients did not require an overnight stay in
a high dependency unit, whereas all VATS and open lobectomy patients
in our study were routinely admitted to these units postoperatively.
Furthermore, mean length of stay in their open lobectomy patients was
14 days. This is significantly longer than in our study, with median length
of stay of 4 days for VATS lobectomy and 5 days for open lobectomy. In
fact the median length of stay in our study was shorter than that reported
in most other studies. Cho et al. [6] reported a mean length of stay for
VATS and open lobectomy of 7.1 and 11.5 days, respectively. Casili et al.
[5] reported a similar mean length of stay of 7.1 and 12 days for VATS
and open lobectomy, respectively. However, one study in the United
States utilizing a fast track program for VATS lobectomy reported a
median length of stay of 3 days [10]. A significant reduction in hospital
stay for VATS patients is an important variable in maintaining patient
throughput in a Canadian hospital. Since thoracic surgery is usually
limited to larger metropolitan cities in Canada, hospital bed availability
is a rate limiting factor in determining whether or not surgical cases
may be performed on a daily basis. A reduction in hospital stay may
translate into more available surgical beds to perform a greater number
of cases.
Regarding overall costs, two large American database reviews yield
somewhat conflicting results. One study showed VATS to be more cost
effective compared to open lobectomy [4], while the second study from a
different database showed no difference in total cost [7]. A study in Poland
suggested that VATS lobectomy is not cost effective for middle income
countries [11] while an older Korean study showed VATS to be more
expensive compared to open lobectomy [12]. A review of VATS technology
in 2003 suggested VATS would have limited utility in developing countries
because of the high intraoperative costs [13]. To our knowledge, our study
is the first Canadian cost analysis of VATS vs. open lobectomy, although a
Canadian study of laparoscopic versus open colectomy showed an overall
cost savings for the laparoscopic technique which was achieved through a
shorter hospital stay [14].
This study is inherently limited by its retrospective design, similar
to all previous studies looking at this issue. There were also differences
in surgical technique in particular for open lobectomy, especially in
the use of disposable instruments which could vary the intraoperative
costs considerably. However, postoperative care was routine among
the two groups, particularly in terms of overnight IMCU stay, routine
APS involvement for open cases, and generalized criteria for chest tube
removal and discharge home. Nevertheless, this study demonstrates
that within a Canadian health care institution the total in-hospital costs
of VATS lobectomy are equivalent to open resection, with potential for
further intraoperative cost saving with ongoing surgeon experience.
Conclusion
The total in-hospital cost of VATS lobectomy is not significantly
different from open lobectomy. Intraoperative costs were higher for VATS,
but postoperative costs are less than open lobectomy. VATS lobectomy
patients spend one less day in a ward bed representing an opportunity
to treat more patients with the currently available beds. There appears
to be a significant impact of a learning curving when introducing
new technology into an institution that is realized as higher initial
intraoperative costs. This should not discourage institutions from
introducing new technology since with increased experience further cost
savings may be realized.
To make VATS lobectomy overall more cost effective than open
lobectomy, the two variables than can be controlled and optimized by the
surgeon are operating time and judicious use of disposable instruments.
Surgeons are encouraged to prospectively and accurately track these two
variables to optimize their performance in a cost efficient manner.
Acknowledgement
The authors would like to thank the Nova Scotia Capital District
Health Authority (CDHA) for providing funding for this project through
a CDHA Research Grant.


