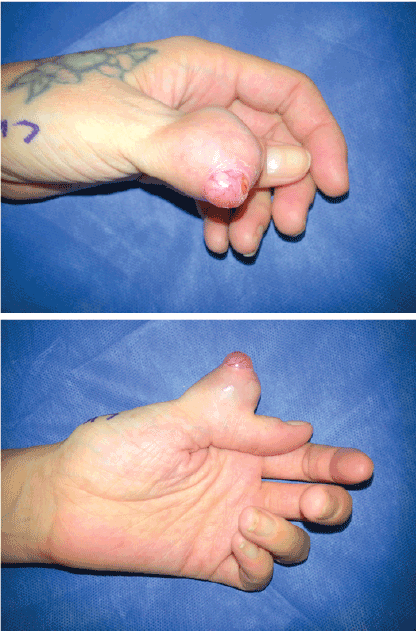
Figure 1: Preoperative view of the left thumb a) Dorsal view b) Lateral view

Samantha Zwiebel1 Christian Curcio2 Laurel Karian3 Jennifer Maerki2 Ramazi O Datiashvili3*
1Division of Plastic Surgery, University of Minnesota, Minneapolis, Minnesota, USA*Corresponding author: Ramazi O Datiashvili, Department of Surgery, Division of Plastic Surgery, New Jersey Medical School, The State University of New Jersey, Rutgers, 140 Brgen Street, ACC E-1620, Newark, NJ 07103, Tel: (973)972-5377; Fax: (973)972-8268; E-mail: datiasro@njms.rutgers.edu
Solitary neurofibroma of a digit is a rare presentation. Diagnostic workup of this lesion highlights the wide scope of differential entities. Patients should undergo both imaging studies and biopsy. Ultrasound and MRI can often narrow the differential diagnosis but must be read by a skilled interpreter. Biopsy should always be performed as a seemingly benign lesion may prove to be malignant. Literature review and a case report are presented.
Digit; Thumb; Softy tissue tumors; Neurofibroma
Soft tissue tumors of the fingers are encountered relatively infrequently by the plastic surgeon. The differential diagnosis is quite broad, including both benign and malignant entities. History and physical exam may reveal an insidiously growing and painless tumor and often do not assist in the diagnosis. Therefore, the appropriate preoperative management strategy to make an accurate diagnosis is essential. This includes various imaging studies (X-rays, Ultrasound, MRI). Typically, lesions should first be biopsied prior to resection. Following a benign diagnosis, tumors that are symptomatic should be completely resected from the base of a healthy tissue bed while avoiding damage to surrounding structures. Rarely, the tumor may prove malignant, in which case surgical management may require ray amputation, and the patient should be examined for metastases.
Here, we report on a 37-year-old female who presented with a large, painful, firm mass of her left thumb that had been present for at least 12 years. An incisional biopsy revealed neurofibroma. The mass was resected without complication and the patient fully recovered. In this report, we present a literature review of digital soft tissue tumors, including the differential diagnosis, diagnostic studies, and surgical management.
A 37-year-old right-hand dominant female presented to the senior author’s (RD) office with a large painful mass over the dorsum of her left thumb proximal phalanx. Her past medical history was limited to asthma, and her only prior surgery was a Cesarean section. She was a former smoker who quit during her workup of the lesion. She reported that the mass had been present for 12 to 13 years and was continuing to increase in size becoming more and e more painful (Figure 1). She denied a history of trauma or any previous lesion at the site.

Figure 1: Preoperative view of the left thumb a) Dorsal view b) Lateral view
On physical exam, there was a 4 × 3 cm mass over the dorsal aspect of the proximal phalanx of the left thumb; the tumor was rounded, rubbery firm, and tender upon palpation. There was an approximately 1 cm2 area at the top of the lesion devoid of overlying skin that revealed white-pink tissue with small vessels coursing throughout the mass. Superficial veins were visible on the lateral aspects of the mass. There were no neurologic deficits, and the patient did demonstrate limited range of motion in the interphalangeal joint. No palpable regional lymph nodes were found upon exam.
The patient underwent imaging studies. X-rays did not reveal any bony involvement. MRI with contrast revealed the mass to be hyperintense and homogeneous. Based on the MRI findings, the Department of Radiology at the Rutgers University Hospital generated a differential that included fibrous histiocytoma both benign and malignant forms, fibromatosis, giant cell tumor of the tendon sheath, epitheloid sarcoma, or synovial sarcoma, among many other possibilities.
An incisional biopsy of the lesion was performed. The specimen resected was 1.7 × 1.4 × 1.1 cm in size. The biopsy site wound was closed primarily. Frozen section pathology revealed myxoid spindle cell lesion, which was ultimately determined to be neurofibroma based on staining with hematoxylin and eosin, as well as positive staining for S-100.The tumor was then excised completely (Figures 2 and 3). The wound was closed primarily. The pathology specimen was white-tan and well circumscribed without a capsule. It measured 4 cm × 3 cm × 2 cm. Final pathology confirmed diagnosis of neurofibroma (Figures 4 and 5). There were no postoperative complications. The wound healed by primary intent. There were no neurovascular deficits postoperatively, and the patient regained full range of motion in all joints of the left thumb (Figures 6 and 7). At six months postoperatively, there is no evidence of recurrence and the patient remains asymptomatic.
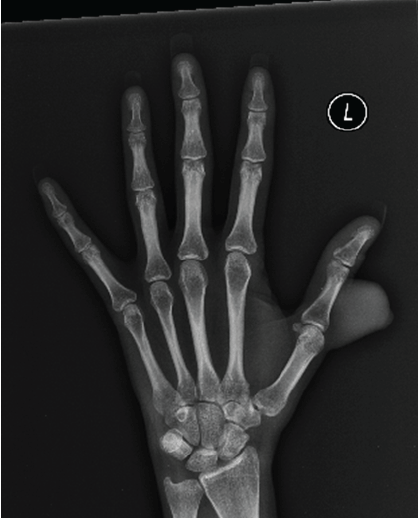
Figure 2: Anteroposterior X-ray of left hand
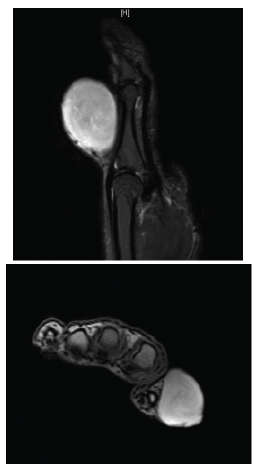
Figure 3: MRI left thumb, with contrast a) Lateral view b) Transaxial view
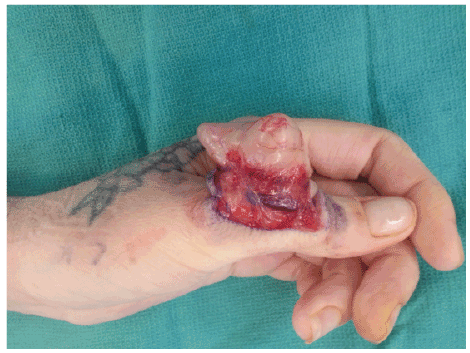
Figure 4: Intraoperative view of lesion
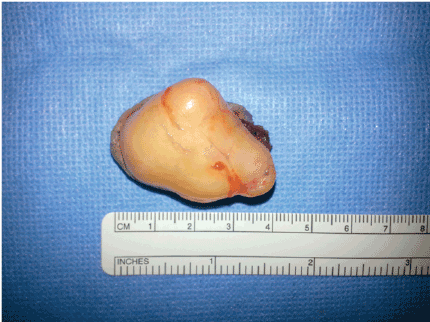
Figure 5: Excised lesion
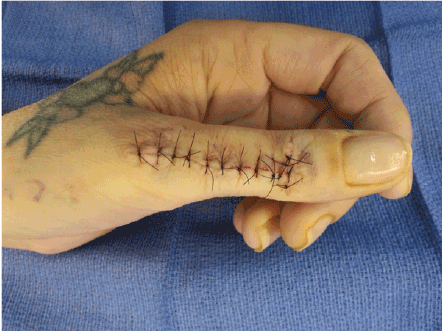
Figure 6: Immediate postoperative view
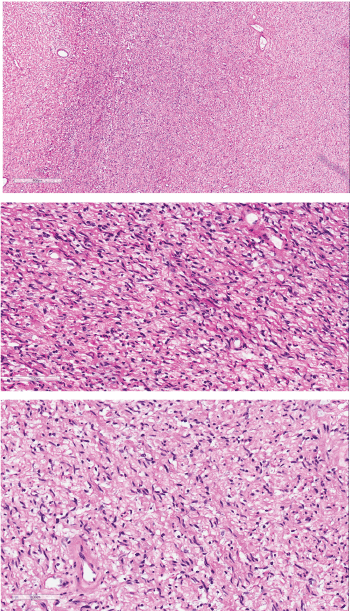
Figure 7: Hematoxylin and eosin staining of excised lesion
a) Hematoxylin and Eosin (4x)-Spindle cells with fibrillar cytoplasm and
elongated nuclei, consistent with neurofibroma.
b) Hematoxylin and Eosin (20x)-Spindle cells with fibrillar cytoplasm and
elongated nuclei, consistent with neurofibroma.
c) Hematoxylin and Eosin (20x)-Spindle cells with fibrillar cytoplasm and
elongated nuclei, consistent with neurofibroma.
Digital neurofibromas are rare, there only few case reports in literature [1-6]. Neurofibromas can present as isolated lesions or as a manifestation of neurofibromatosis. The percentage of isolated lesions associated with neurofibromatosis is only 10% [7,8]. The differential diagnosis for soft tissue tumor of the digit is extensive and includes both benign and malignant entities. The most common benign soft tissue tumors of the digits are ganglion cysts, giant cell tumors, fibromas, glomus tumors and schwannomas. Giant cell tumors are reported to be the second most common tumors of the hand [9,10]. Fibromas account for 1-3% of the hand tumors [11,12]. Glomus tumors are associated with neurofibromatosis type 1 but may present in isolation [9]. Schwannomas and neurofibromas are the most common tumors of the hand arising from neural tissue [10]. Of malignant lesions, skin malignancies are the most common. Although squamous cell carcinoma comprises approximately 75% of these lesions, skin malignancies may also present as tumors, as in eccrine sweat gland tumors and Merkel cell carcinoma [13]. Epithelioid sarcoma, synovial sarcoma, and malignant fibrous histiocytoma have high rates of local recurrence and metastasis, and thus may require amputation for adequate treatment [13,14].
Given this extensive differential diagnosis, imaging is an important step in the pre-operative evaluation of the patient. In addition to regular X-rays, suggested imaging studies for the finger tumors include ultrasound and MRI to assess extent of the lesion, involvement of surrounding structures and to narrow the differential diagnosis. Ultrasound is relatively inexpensive and easily accessible, but technically difficult and conveys less information. MRI offers superior imaging with greater anatomic detail and a higher likelihood of accurate diagnosis, but is more expensive [15]. Most soft tissue tumors will have similar clinical presentations and therefore all soft tissue tumors of the digit must be biopsied prior to complete resection due to malignant potential. Specimens submitted for pathology may be differentiated based on cell morphology which is revealed by staining with hematoxylin and eosin, and diagnosis-specific stains such as S100 and EMA [10].
Both schwannomas and neurofibromas are derived from a neoplastic Schwann cells. Histologically, neurofibromas feature neoplastic Schwann cells, perineural-like cells, and fibroblasts in a mucocollagenous matrix. These are histologically distinct from schwannomas, which present as spindle-shaped Schwann cells embedded in Antoni A and B patterns of compact, elongated cells and loose, less cellular regions, respectively. Both entities stain positive for S-100, as this stain is specific to neural crest derived tissues. Neurofibromas stain positive for CD34, an intercellular adhesion protein and cell surface glycoprotein with a poorly understood function, and stain negative for EMA, a cell surface mucin glycoprotein expressed by most glandular and ductal epithelial cells and some hematopoietic cells. In contrast, schwannomas stain positive for EMA and negative for CD34 [16].
Following biopsy, all symptomatic benign lesions should be completely resected with care taken not to disrupt nearby structures, in particular the digital nerves. Involved tissue should be resected as closely as possible to the tissue bed [17,18]. Malignant lesions will likely require the care of a multidisciplinary team with assessment of metastasis and consideration for the role of radiation therapy or chemoradiotherapy [18]. Subungual lesions require avulsion of the nail plate and separation of the nail bed from tumor when possible, with complete excision of the tumor
Download Provisional PDF Here
Article Type: Case Report
Citation: Zwiebel S, Curcio C, Karian L, Maerki J, Datiashvili RO (2016) A Solitary Neurofibroma of the Thumb: Literature Review and Case Report. J Surg Open Access 2(5): doi http://dx.doi.org/10.16966/2470-0991.129
Copyright: © 2016 Zwiebel S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access