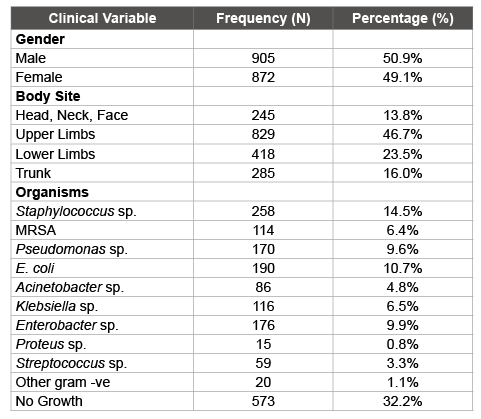
Table 1: Clinical findings and their frequencies with percentages


Habibullah Shah*1 Huma Gul2 Rashid khan2 Atifullah khan1
1Habib Burn Center, Zia Medical complex, University Road, Peshawar, Pakistan*Corresponding author: Habibullah Shah, Consultant Plastic Surgeon, Habib Burn Center, Zia Medical Complex, University Road, Peshawar, Pakistan, Tel: 00923348800339; E-mail: drhabibullahshah@gmail.com
Objective: To determine the bacterial profile of paediatric burn wounds and their antibacterial spectrum in order to understand and help in planning for better antibiotic selection and overall management.
Methods: Retrospective review of prospectively collected data of paediatric age burn patients at Habib Burn Centre Peshawar between January 2013 and December 2015. Culture& sensitivity tests were performed using wound surface swabs and tissue culture over the three-year period. Their results were collected in a predesigned digital form. Statistical analysis was done and results plotted.
Results: 1204 (67.8%) patients tested positive with the commonest bacterial isolate of coagulase negative Staphylococcus species (14.5%, n=258), followed in frequency by E. coli (10.7%, n=190), Enterobacter species (9.9%, n=176) and Pseudomonas species (9.6%, n=170). Multidrug resistant Staphylococcus aureus (MRSA) was found in 114 (6.4%) of cases. The most effective antibacterial was Imipenem with a susceptibility rate of 64.3% in 1143 patients. This was followed in efficacy by Tigecycline (63.9%) and Ofloxacin (54.3%). The least effective antibacterial was Cephradine with effectiveness of only 25.4%. Linezolid and Vancomycin were the most effective against MRSA at 91.2% and 100% efficacy.
Conclusions: Resistance to antibiotics is rapidly increasing in our community and burn wounds are frequently infected by these multidrug resistant organisms. Careful antibiotic selection and effective control of these strains can be translated into lower morbidity and mortality for these patients.
Burn wounds; Bacteriology; Antibacterial spectrum; Paediatrics
Burns have a high incidence among the children in developing countries and are associated with septic complications such wound infection and systemic sepsis due to poor wound care and ineffective systemic and topical treatment [1]. Septic burn wounds complications have disastrous consequences in terms of prolonged morbidity and treatment failures and a very high rate of mortality. Unfortunately, these are very common in our society due to manhandling of burn wounds in general and specifically in children [2].
The bacterial profiles and their antibacterial sensitivity patterns have changed significant over the last 10 years, and the occurrence of fatal septic complications have increased in incidence accordingly [3]. Multidrug resistant staphylococcus aureus, pseudomonas, E. coli, Enterobacter and Acinetobacter are being increasingly found in burn wounds which is very much alarming due to the limited number effective antibacterial drugs [2,4]. The developing countries of Africa, the Middle East and Asia are increasingly reporting the occurrence of these resistant strains which potentially mean the disastrous consequences for patients and societies [4]. Nosocomial infections have increasingly been implicated in transferring fatal septic complications in severely ill patients such as those with burns [5,6]. Considering the weak defense mechanisms and limited physiological reserves of children with burns, it is imperative to be aware of the current trends of burn wound bacteriology so as to know ahead of the expected occurrence of these deadly organisms [6].
Wound care specialists are therefore required to constantly report the occurrence of multidrug resistant bacterial species so that preventive methods are effectively implemented in order to prevent the communities [7]. Studies have reported that hospitals where antibiotic resistance is low, has found resistant organisms which are highly resistant to antiseptic solutions like povidone iodine. This is alarming from public health as well as surgical perspective where wound management is high and the primary antiseptic solution is povidone iodine [8].
We therefore aim to present a comprehensive bacteriological profile of burn wounds in children and to plot their resistance patterns among the commonly used antibacterial drugs. This will help understand the current trends of burn wounds bacteriology and help in better planning of wound care of our patients.
The study is a retrospective of prospectively collected data of paediatric burns that were treated at Habib Burn Centre Peshawar, a private specialist centre for the management of burn patients. Patient data which was collected between January 2013 and December 2015 was retrospectively analysed. All patients who were included in the study and who were treated at the centre were consented before initiation of any kind of procedure and they were informed about inclusion into the study. Samples were sent from wound surfaces of patients either in the form of swabs or tissue samples at their admission time before they were administered with systemic antibiotics or wound antisepsis.
Paediatric age (1 to 16 years) patients of either gender, irrespective of their location and type of burns were included in the study. Additionally, patients with complete follow-up and bacteriological records from their wounds were included.
Patients previously treated elsewhere and patients who only required outpatient treatment were excluded. Also, patients with incomplete bacteriological studies due to any reasons were also excluded.
Data was collected about patient demographics such as age and gender. Type of burn, total burn surface area (TBSA), the type of organism which was isolated and the susceptibility spectrum of the commonly used antibacterial drugs were also recorded.
Data was entered and analysed using the IBM SPSS Statistics, version 22.0. Age groups were plotted against the type of burns, and their TBSA patterns. Similarly, organisms obtained from samples were plotted against the drugs against which they were resistant and those to which they were susceptible. All data is presented in charts and tables.
Of the total 1777 patients, 905 (50.9%) were male and 872 (49.9%) were female patients (Table 1). Mean age was 10.0 years ± 3.42 SD and mean TBSA was 23.26% ± 11.52 SD (Table 2). The commonest type of burn was scalds which occurred in 1412 (79.5%) cases and was followed in frequency by flame burns (15.2%). The most commonly involved body site was upper limbs (46.7%) (Table 1).

Table 1: Clinical findings and their frequencies with percentages
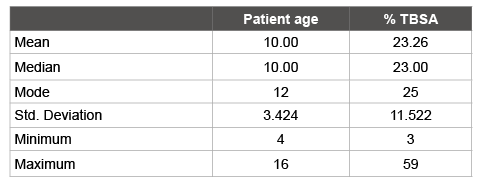
Table 2: Descriptive statistics for age and %TBSA
1204 (67.8%) patients tested positive on culture and sensitivity testing of their wounds with the commonest bacterial isolate of coagulase negative Staphylococcus species (14.5%, n=258). This was followed in frequency by E. coli (10.7%, n=190), Enterobacter species (9.9%, n=176) and Pseudomonas species (9.6%, n=170). Multidrug resistant Staphylococcus aureus (MRSA) was found in 114 (6.4%) of cases while the Bacteroides species was not found in any specimen (Table 1 and 3).
Overall, the most effective antibacterial was Imipenem with a susceptibility rate of 64.3% in 1143 patients. This was followed in efficacy by Tigecycline (63.9%) and Ofloxacin (54.3%). The least effective antibacterial was Cephradine with effectiveness of only 25.4%. Linezolid and Vancomycin were the most effective against MRSA at 91.2% and 100% efficacy. Pseudomonas species was most sensitive to Tigecycline at 100% susceptible while 80% were susceptible to imipenem. The antipseudomonal penicillin Ticarcillin was active only against 57.6% of this species (Table 3).
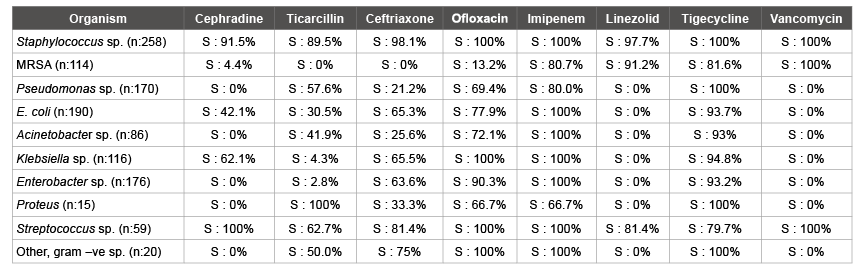
Table 3: Bacterial isolates and their antibacterial susceptibility patterns
Burn wounds are a major health burden both in the developed as well as developing nations [9]. Infection of burn wounds with resistant organisms is an identified complication which is due to loss of the mechanical barrier of intact skin surface [2]. Over the last decade, susceptibility patterns are rapidly changing all over the world, and this is creating a virtual inefficacy of the available antibacterial drugs for treating such infections [3]. Burn wounds infection is correlated to TBSA and the delay in presentation as well as local practices regarding treatment of virulent strains. It has been shown that ward practices such as dressing changes and bed sheet transfers increase the airborne infectious agents for more than one hour [10]. Multidrug resistant staphylococcus aureus (MRSA) and a diverse variety of gram negative organisms are involved in severe burn wound infections leading to uncontrolled wound and systemic sepsis [11,12]. In most situations, the MRSA, Pseudomonas and E. coli like organisms form biofilm where they remain in a low bio-active form. This leads to decreased effectiveness of antibacterial drugs due to limited penetration of the biofilm as well as the destruction of the organism itself [12].
In our study we isolated more than ten different kinds of pathogens with majority of gram negative organisms. These organisms were Pseudomonas species, E. coli, Acinetobacter sp., Klebsiella, Proteus sp., and a few other rare gram negative organisms. MRSA was found in 6.4% samples while the coagulase negative Staphylococcus was found in 14.5% samples. Streptococcus pyogenes were found in 3.3% cases while the rest of the 43.3% cases were comprised of gram negative bacteria. In a recent study by Azzopardi et al. [11] gram negative organisms were the predominant types with majority of cases of Pseudomonas aeruginosa, Klebsiella pneumoniae, Acinetobacter baumanni, Enterobacter and Proteus species. They have concluded that gram negative organisms are a major determinant of morbidity and survival and targeting them exclusively by regular bacterial culture studies of the burn wounds can be translated into effective infection control and improved survival with less morbidity [11].
Bashir et al. [13] in a study from Karachi, Pakistan, conducted a detailed study about clinical isolates of Staphylococcus species and compared their susceptibility to the common first line agents. They concluded that Vancomycin was the most effective antibacterial drug for these organisms and it was effective in 81.2% cases. However, erythromycin and bacitracin demonstrated low to mid-range efficacy against these organisms [13]. These findings are in agreement with our study where we found 100% effectiveness of Vancomycin against MRSA and 100% efficacy against other strains of Staphylococcus species.
In another study by Biswal et al. [14], P. aeruginosa susceptibility rates were studied against the common antibacterial drugs and it was noted that this organism is resistant in 81% of cases to aminoglycosides; up to 70% were resistant to beta lactams, while only 13% isolates showed resistance to carbapenems. We found Pseudomonas aeruginosa to be susceptible to Ticarcillin, Ofloxacin, Imipenem and Tigecycline in more than 50% cases. The most effective drug was Tigecycline, which was effective in 100% cases of Pseudomonas aeruginosa. Ceftriaxone, which is a commonly used antibiotic for preoperative and postop systemic prophylaxis, was only effective in 21% of cases. This is very alarming, since the commonly available antibiotics such as Cephradine and Ceftriaxone are successful in very low number of P. aeruginosa cases. A major reason for the high ceftriaxone resistance could be attributed to the widespread use of this class of antibiotics in wards and emergency departments for treatment of common infections and it has been observed that patients remain on prolonged courses of this drug without evidence of a susceptible infectious agent. Blind systemic prophylaxis is proven in many meta-analysis and controlled trials, to be ineffective against development of infection. Despite the evidence suggesting these trends, it is used vastly and without evidence of infection [1,4].
Drug resistance in our study was high in our study with many multidrug resistant gram negative and positive organisms isolated from wounds of the burn patients. This means that our patients are at increased risk of contracting these highly lethal organisms both in their wounds and systemically. High resistance patterns are associated with prolonged morbidity and mortality in burn patients, especially in the paediatric population where physiological reserves are low. Patients can be protected from these highly virulent organisms by adopting uniform antibiotic prescription policies across hospitals. One effective way to limit inoculation of burn wounds is to improve burn wound care at our local hospital and to educate the public to avoid the application of hazardous and contaminated material on burn wounds. Effectively controlling infection of burn wounds will ultimately be translating into better overall morbidity and mortality and less load on hospitals and specialist centres.
Burn wound infections are frequent and most commonly involve multidrug resistant pathogens. Infections of these wounds are also associated with high rates of morbidity and mortality. Identification of burn wound pathogens, therefore, is crucial in developing wound care policies. Currently, the most common multidrug resistant organisms are from both gram-positive and gram-negative species with limited number of antibacterial drugs available for adequate control. Careful antibiotic selection to control the existing pathogens is the need of the moment in order to reduce infection related morbidity and mortality. Uniform institution wide antibiotic protocols are required to reduce the emergence of resistant strains.
Download Provisional PDF Here
Article Type: Research Article
Citation: Shah H, Gul H, Khan R, Khan A (2016) Bacterial Profile of Paediatric Burn Wounds and their Antibacterial Sensitivity Patterns. J Surg Open Access 2(2): doi http://dx.doi.org/10.16966/2470-0991.116
Copyright: © 2016 Shah H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access