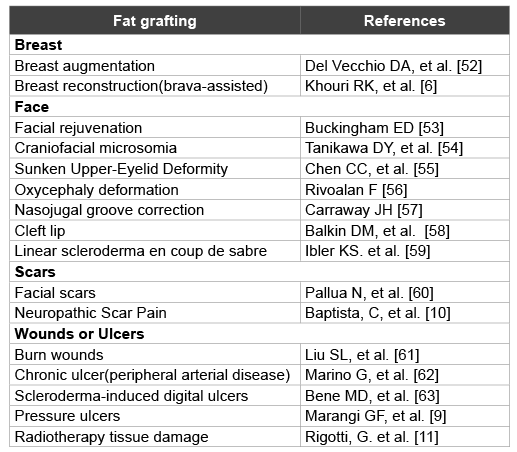
Table 1: Current application of fat grafting: a summary


Yuping Ren1 Mikhail G Kolonin2,3 Yong Li3,4*
1Division of Plastic Surgery, Tongji Hospital, Huazhong University of Science and Technology, Wuhan, 430030, China*Corresponding author: Yong Li, Center of Stem Cell and Regenerative Medicine, The Brown Foundation Institute of Molecular Medicine for the Prevention of Human Diseases, University of Texas Health Science Center at Houston (UT Health), TX77030, USA, Tel: 7135002438; E-mail: Li.1@uth.tmc.edu
In recent years, fat grafting has become a popular method for clinically correcting soft tissue deformities. In order to increase fat graft viability a variety of modifications have been made to current grafting procedures including cell-assisted lipotransfer (CAL), structural fat grafting, fat grafting mixed with adipose stem cells (ASCs), fat grafting mixed with platelet rich plasma (PRP) and fat grafting mixed with both ASCs and PRP; however, the persistence of the grafts after transplantation remains in consistent. In this review, the biological fundamentals of lipotransfer procedures are discussed, the current progress of clinical fat grafting applications in plastic and reconstructive surgery are summarized, and the challenges facing fat transplantation are outlined.
Fat grafting; Adipose stem/stromal cells (ASCs); Platelet rich plasma (PRP); Transplantation; Regeneration; Challenges
Correction of soft tissue contour deformities remains technically challenging for plastic and reconstructive surgeons. The ideal fillers for augmenting contour deformities should be physically and chemically stable, nontoxic, non-immunogenic, noninfectious, non-immunoreactive, and should be inexpensive to obtain and easily stored. Autologous material aspirated from white adipose tissue (WAT) has been recognized as an excellent injectablefiller for defect correction based on its biological characteristics. Through liposuction and minimal processing, large amounts of autologous adipose tissue can be harvested without significant donor-site morbidity. Currently, the use of fat grafting to fill soft tissue voids has become a very popular technique in plastic and reconstructive surgical clinics.
The first use of free autologous fat transplantation in a clinical setting was performed by Dr. Gustav Neuber in 1893. He obtained excellent aesthetic results when he implanted detached segments of fat under the eyes of patients; however, when he tried to transplant larger grafts, the grafts failed. Harvesting the fat, used in the previous procedure resulted in a high degree of donor site morbidity and other complications which have been considered a major limitation for successful fat grafting. In 1987, Bircoll et al. [1] reported their use of liposuction for obtaining fat for breast augmentation and correcting dog-bite injury defects of the right thigh. The autologous fat obtained was transplanted using a small syringe and two and an half years after surgery, the patients presented with excellent aesthetic results. In 1988, Asken [2] described a new method for fat grafting using liposuction and micro lipo injection which resulted in excellent improvements in the contours of the patients’ face after injection. These results encouraged more clinicians to consider the use of lipo-transfer and fat grafting as a method to treat soft tissue deformities. Because the popularity of liposuction grew tremendously during the 1980s, the use of fat transplantation to augment or reconstruct soft tissue defects developed rapidly. Coleman et al. [3,4] optimized methods for harvesting fat and fat transfer in order to provide pure, intact parcels of fat, thus establishing the term” structural fat grafting”. This theory recommends that only a small quantity of fat should be injected in thin layers to increase the surface area the fat has contact with the receptor bed. This method of grafting fat is accepted by numerous plastic surgeons and has generated tremendous interest in the area of fat grafting, which has resulted in long-lasting and naturally-appearing grafts.
Today, fat grafting is utilized as a therapeutic method for the treatment of soft tissue volume loss due to aging, infection (e.g. facial lipoatrophy from human immunodeficiency virus infection), various types of trauma (mainly skin burns), idiopathic abnormalities (e.g. hemifacial microsomia) [5], tumor resection (e.g. breast reconstruction after mastectomy) [6], immune disease [7], and many other causes of soft tissue deficiency resulting in asymmetry or contour irregularity. Some clinicians have also used fat grafts for cosmetic breast augmentation [8] and for treating pressure ulcers [9], painful scars [10] and radiation-induced soft tissue injuries [11] (Table 1). Moreover, Covarrubias et al. [12] reported that patients with skin defects grafted with fat displayed evidence of regeneration including increased dermal thickness, collagen neo formation, and the presence of increased vascularity in skin adjacent to the lipofilling. Current results of fat grafting are impressive and bring significant benefits to patients who have undergone plastic and reconstructive surgery [13].

Table 1: Current application of fat grafting: a summary
It has become apparent over the years that white adipose tissue (WAT) is the most suitable autologous injectable filler for correcting soft tissue defects.WAT contains large numbers of adult stem cells and is an excellent natural resource for human augmentation procedures. During the last decade, several novel adult stem cell populations have been identified and isolated from adipose tissue [14-16]. Te term “adipose-derived stromal/ stem cells (ASCs)” is a term coined by the International Fat Applied Technology Society (IFATS) [17]. ASCs have been shown to be capable of self-renewal, and increased proliferative and multipotent differentiation capabilities. These cells also exhibit similar properties to mesenchymal stem cells (MSCs), which were first described and characterized in the bone marrow [18]. ASCs are localized around blood vessels [19,20] and are abundantly present in WAT where they constitute as much as 1% of the cell population, where as bone marrow MSCs (BM-MSCs) only comprise 0.001–0.002% of the cell population in bone marrow [21]. There are many cell types other than adipocytes within WAT [22]. Once WAT is aspirated and digested utilizing collagenase, the adipocytes can be isolated through centrifugation. The remaining cell fraction, called the stromal vascular fraction (SVF), contains vascular endothelial cells and various types of leukocytes in addition to ASCs [23]. Based on biomarker staining, ASCs can be isolated and characterized in vitro. Though ASCs demonstrate multipotency, not all ASCs can be induced to differentiate into adipocytes. Adipocyte progenitors are a heterogeneous population of cells, with some giving rise to white adipocytes and others give rise to beige adipocytes, which constitute brown adipose tissue (BAT) [24,25]. These ASCs can be distinguished from other adipocyte progenitor populations based on their expression of a variety of surface markers [26]. The regenerative capacity of ASCs during graft setting, and their contribution to WAT regeneration or re growth remains undefined. Recent studies have indicated that ASCs can promote angiogenesis in addition to suppressing inflammation, both of which are known behaviors of BM-MSCs [18].
Matsumoto et al. [27] performed a procedure termed cell-assisted lipotransfer (CAL) where the aspirated fat and the SVF cells are subcutaneously co-injected. Using a severe combined immunodeficiency (SCID) mouse model, the CAL procedure demonstrated superior cell survival and micro vessel formation after transplantation compared to the control non-CAL fat transplanted mice. This study showed that ASCs could differentiate into vascular endothelial cells and contribute to the neovascularization within the recipient tissue quickly after transplantation. Yoshimura and his team [23] have investigated and shown convincing evidence of very dynamic remodeling of the adipose tissue after non vascularized grafting [28]. Two weeks after fat tissue transplantation, they observed three distinct zones within the graft (300 µm from the peripheral edge of the graft toward the center): the surviving area (consisting mostly of ASCs and adipocytes), the regenerating area (transplanted adipocytes dead, but replaced with new adipocytes, ASC’s survived), and the necrotic area (both adipocytes and ASCs dead). It is believed that the adipocytes that died in the graft are due to watershed ischemia in the deep areas of the graft where little vascularization occurs [28]. Most of the cells in the surviving regions were ASCs, suggesting that the ASCs have a greater tolerance to ischemic stress. These findings represent convincing evidence of the importance of ASCs for supporting the success of fat grafting [29].
Taken together, these studies demonstrated that there resident ASCs within fat grafted tissues can: 1) differentiate into adipocytes and add structure to fill the implanted tissue defect [30]; 2) secrete growth factors, cytokines, and chemo-attractants that can enhance angiogenesis and increase localvascularization and blood supply; and 3) inhibit innate immune responses after tissue transplantation [31,32]. ASCs are also involved with establishing fat homeostasis. These properties support successful tissue regeneration and the long-term survival of the fat graft. The surgical procedure, e.g. fat retrieval and the transplantation techniques, including cell-assisted lipotransfer (CAL), also determine the success of fat grafting [29].
Platelet rich plasma (PRP) is an autologously derived biological material that has recently been used to facilitate fat graft survival. PRP was first described in 1975 by Oon and Hobbs [33] and first applied clinically in 1987 by Ferrari et al. [34] PRP is typically derived by centrifuging the patient’s whole blood to remove the erythrocytes and concentrate the platelets. The concentration of platelets in PRP is many times greater than that of peripheral blood [35]. The platelets contain α-granules, which are endowed with a great variety of growth factors including platelet-derived growth factor (PDGF), transforming growth factor-β (TGF-β), vascular endothelial growth factor (VEGF), epidermal growth factor (EGF), etc. After activation, typically after injury and coagulation, these factors are released by the platelets [36]. More than 500 clinical applications of PRP have been reported including its use for enhancing bone regeneration [37], wound healing [38], skin rejuvenation [39] and indeed fat augmentation [40].
Gentile et al. [40] performed a comparative translational study on fat grafting for the maintenance of tissue volume in breast reconstruction and found that the fat graft survival rate was 63% in patients treated via SVF-enhanced autologous fat grafts, 69% survival in patients treated with PRP-mixed fat grafts, and only 39% in patients treated with fat grafts alone. Retrospective studies from a cohort of 82 patients showed that fat grafts mixed with PRP reduced patient recovery time and improved the overall aesthetic outcome of facial lipofilling, compared to lipofilling using fat alone [41]. Moreover, numbers of animal studies have prospectively demonstrated that tissue grafting is improved with the use of PRP [42-44]. PRP can be viewed as a growth factor ‘factory’ supporting neoangiogenesis and enhancing the viability of the transplanted fat cells, which results in superior regeneration and grafting outcome.
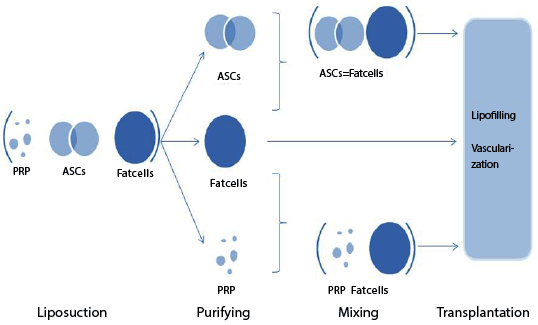
Figure 1:The strategies of fat grafting after transplantation
Although autologous fat grafting is a popular option for soft tissue augmentation, the technical challenges and potential complications of performing the procedure including the unpredictable and low survival rates of the graft limit its clinical application; moreover, central partial ischemia/necrosis often occurs in large areas of the transplanted fat. In addition, recent studies have shown that ASCs can promote tumor growth, [45-47] which have raised serious concerns regarding the safety of lipotransfer procedures [48,49]. Great variations with regard to fat graft survivability (40% to 80%) are also a concern which is probably due to technical procedure differences when harvesting the fat [50,51]. Other challenges include the critical maintenance of cell viability during the fat grafting procedures; however, there are no current techniques that have been developed to evaluate the donor fat for its ability to preserve the cellular viability. In addition, the extent to which ASCs or PRP can improve the outcomes of fat grafting in various procedures is still under investigation, though the results appear quite promising.
Fat grafting has become a popular procedure performed by plastic and reconstructive surgeons for facelifts, breast augmentation, and the treatment of other soft tissue defects. Several strategies have been performed to improve fat grafting as presented in Figure 1. Although the current grafting procedures, including cell-assisted lipotransfer (CAL), are effective methods that offer great potential for enhancing soft tissue regeneration, there remain many uncontrollable factors that can interfere with the efficacy, sustainability, and safety of current fat grafting techniques. Rigorous basic science and clinical studies involving both surgeons and research scientists are ongoing in an effort to improve the safety profile and outcomes of fat transplantation.
The authors would like to thank Dr. Kinga Vojnits for educational discussion and Mr. James Cummins for his editorial assistance.
Download Provisional PDF Here
Aritcle Type: Review Article
Citation: Ren Y, Kolonin MG, Li Y (2015) Fat Grafting with Adipose Stem Cells: The Successes and Challenges. Int J Stem Cell Res 1(2): doi http:// dx.doi.org/10.16966/2472-6990.106
Copyright: © 2015 Ren Y, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access