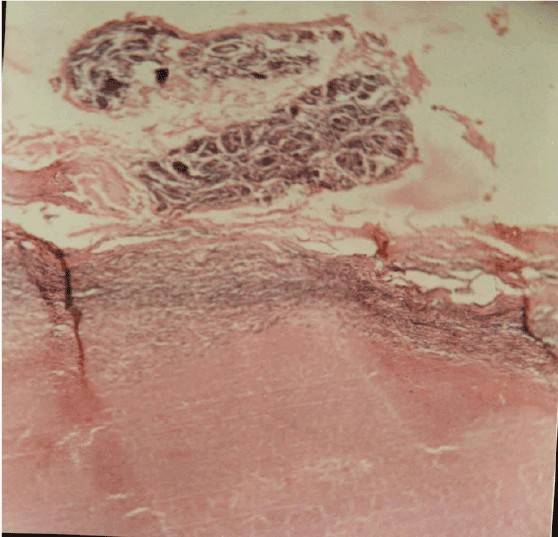
Figure 1: The top shows fibro sclerosis and adenosis of the breast which is separated by thin lymphoid tissue from a confluent tuberculous granuloma.


Wilson Onuigbo1* Gabriel Njeze2
1 Department of Histopathology, National Orthopaedic Hospital, Enugu, Nigeria*Corresponding author: W.I.B. Onuigbo, Department of Histopathology, National Orthopaedic Hospital, Enugu, Nigeria, Tel: +2348037208680; E-mail: wilson.onuigbo@gmail.com
The case report is presented of a patient with tuberculosis diagnosed from a chest wall lump. It turned out to be unusual in that it was situated in a lymph node within the mammary tissue. Its diagnosis in this unusual site highlights the fact that migration is an etiologic factor not only in terms of migration from developing to developed countries but also migration within a developing country itself.
Breast; Lymph node; Tuberculosis; Cancer mimicking; Epidemiology
Tuberculosis (TB) is very common in developing and tropical countries, especially where general health, nutrition, housing and public health services are poor [1]. On taking a look at the world situation, Grzybowski S [2] told the XIV World Congress on Diseases of the Chest in Toronto in 1982 that the incidence rate in the Philippines, for instance, was some 20 times greater than that seen in the United States. Throughout the world, much as the primary pulmonary form is well known, the extra pulmonary forms now constitute what has been termed a diagnostic enigma [3]. However, it was apt awareness that led to the recognition of tuberculous mediastinal lymphadenitis as the source of a chest wall mass in an American woman [4]. Similarly, chest wall involvement related to pacemaker wires has been reported [5]. Therefore, the present paper reports another chest wall mass that was an intramammary tuberculous lymph node in a Nigerian woman.
A 52-year-old female of the Kataf ethnic group hailed from Northern Nigeria but presented at the Trans Ekulu Hospital, Enugu, Eastern Nigeria, with a painless mobile lump in the right breast. She stated that it had been there for some time. The mammary mass was biopsied on suspicion of carcinoma by the junior author (GEN) and referred to the senior author (WIBO) at the National Orthopaedic Hospital, Enugu. The specimen was received in formol-saline. It was a 3.5 cm ovoid mass which was strikingly caseous on section. When processed in the usual way, microscopy of Haematoxylin-Eosin stained slides revealed that the peripheral portion was breast tissue showing fibro sclerosis and adenosis in benign order, while the subjacent lymph node manifested classical caseating granulomas such as were encountered in a survey of peripheral lymph node tuberculosis among the Igbo’s (Figure 1) [6]. Therefore, TB of an intramammary lymph node was diagnosed. Unfortunately, she was an itinerant patient and was lost to follow-up when she left for her abode in the Northern part of the country.
Mammary TB has been described as a rare modern disease in which the correct diagnosis is rarely made without biopsy, the preoperative impression being carcinoma [7]. If tuberculosis is rare in the breast itself [8], how much rarer it must be in any lymph node within the breast proper? In fact, the very existence of such a lymph node is not mentioned in the encyclopedic Ackerman’s Surgical Pathology [9]. Moreover, Egan and Mc Sweeny [10] stated that these nodes “had been disregarded by surgeons and anatomists,” while Jadusingh IH [11] pointed out that “Pathologists should be alert to the existence and potential importance of these lymph nodes.” Therefore, as this curious case substantiates the very existence of intramammary lymph node, it is deemed that documentation is worthwhile.

Figure 1: The top shows fibro sclerosis and adenosis of the breast which is separated by thin lymphoid tissue from a confluent tuberculous granuloma.
A salient feature of worldwide TB is the role of immigration such as the unfolding incidence among Afro-Asian immigrants in the United Kingdom [12]. However, the present case shows that migration within the developing country itself must also be borne in mind. The instant case arrived from the northern part of the country. Unfortunately, her homeward departure made follow-up impossible. Incidentally, this is a recognized problem in the underdeveloped world. See how precise microbiologic diagnosis is usually put at bay as follows: “should this be impossible because of inadequate facilities; a therapeutic trial of antituberculosis drugs can be started. The effect on the disease must be carefully watched” [13].
A survey of the literature indicates that single cases are usually reported. Thus, the case of a 50-year-old North African woman who presented in UK with intramammary tuberculous lymphadenitis was deemed to raise “the possibility that the nodular type of tuberculous mastitis arises in intramammary lymph nodes” [14]. In our own case, while the better management of her presumed tuberculosis could not have been pursued, the acceptable lesson is that mobility within the country itself is contrastable with the better known international migrations.
The authors would like to extend our deepest gratitude to Dr. R. E. Nnabuko for help with the illustration used in this study.
Authors report no conflict of interest.
Download Provisional PDF Here
Article Type: Case Report
Citation: Onuigbo W, Njeze G (2015) Intramammary Lymph Node Tuberculosis Mimicking Cancer. J Infect Pulm Dis 1(1): doi http://dx.doi.org/10.16966/2470-3176.105
Copyright:© 2015 Onuigbo W, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access