Abstract
Setting: Blackburn, East Lancashire, a high TB prevalence district of the United Kingdom.
Methods: Continuous prospective monitoring of all isolates of M.tuberculosis, with their drug susceptibility profiles.
Results: Of the 382 isolates in 2000-2009, 54 were of white ethnic origin, 319 of South Asian ethnic origin and 9 of other ethnic origin. There was
no isoniazid resistance in the white ethnic patients in the 10-year cohort, whereas the rate of isoniazid resistance was nearly 6% in the South
Asian group. 4/319 (1.25%) of isolates in the South Asian cohort had MDR-TB.
Conclusion: Drug resistance remains very low in the local white population, but in the South Asian population continues at a level of isoniazid
resistance of 6%, with 4/19 with isoniazid resistance having MDR-TB. The drug resistance profile of the non-white population continues to reflect
that of South Asia, with MDR-TB now appearing in previously untreated recent arrivals.
Introduction
Continuous drug resistance data for M.tuberculosis isolates is available
for the Blackburn, Hyndburn and Ribble Valley local government areas
of East Lancashire, UK (United Kingdom), from 1960 onwards. Those for
1960-84 [1], 1985-89 [2], and 1990-1999 [3] have been published, and
these show drug resistance declining to very low levels in the white ethnic
group, but remaining consistently between 6.5 and 15% in the South
Asian ethnic group, mainly to isoniazid (H), Streptomycin (S) or to these
combined (SH). The Blackburn district of East Lancashire remains one
of the high TB incidence districts in the UK, being over 28/100000 per
annum in 1998 [4], and 37/100000 in 2009 [5].
Methods
Isolates of M.tuberculosis were cultured locally, by Lowenstein-Jensen
slope until May 2004, and then by MGIT (Becton Dickinson) from June
2004 onwards. After local isolation, all samples were sent to the Newcastle
Regional Centre for Mycobacteriology, for species identification and drug
susceptibility testing. The results of such tests have been continuously
prospectively collated (by LPO) since 1981, and are reported here for
isolates from 01.01.00 to 31.12.09 inclusive.
Results
In 2000-04, there were 172 isolates overall, 22 white, 149 South Asian
and 1 in other ethnic groups. For 2005-09 there were 210 isolates overall,
32 white, 170 South Asian and 8 in other ethnic groups. Details of drug
resistance are given in (Table 1), and comparison with earlier data [1-3]
in (Table 2). None of the Multi-Drug-Resistant TB (MDR-TB; resistant
to isoniazid/rifampicin +/- other drugs) had prior TB treatment in the
United Kingdom. One MDR-TB case in 2005-2009 had been a close
contact 18 months earlier of a local MDR-TB case, occurring in a recent
arrival from South Asia. A further close contact of the second MDR
case subsequently developed MDR-TB approximately two years later in
2005-20009. Both of the other MDR-TB cases (n=2) were born in either
Pakistan or India and had subsequently emigrated to the UK.
Discussion
This cohort completes 50 years of continuous drug resistance data, in
an area of the UK, which went from below national average TB rates in
1960-1965 to the highest rate of TB in England and Wales in 1970 [6].
No cases of drug resistance were seen in the white ethnic cases over this
10 year (2000-2009) cohort. With these data, and those from previous
cohorts [1-3], this means only 3 cases of isoniazid resistance were reported
in 30 years in the white cohort. In contrast, the rate of drug resistance,
particularly to isoniazid (approximately 6.0% in these data), has remained
between 4.5-7.4% consistently since 1960 in the South Asian group (Table
2). These data, therefore, continue, together with the previous data [1-
3], to provide substantial indirect evidence of the lack of transmission,
using isoniazid resistance as a surrogate marker, between the main White
and South Asian ethnic groups over nearly 50 years. Analysis of MIRUVNTR
(multiple interspersed repetitive units; variable number tandem
repeat) profiles of the whole East Lancashire TB isolates for 2001-9, has
also recently directly confirmed this lack of inter-ethnic transmission [7].
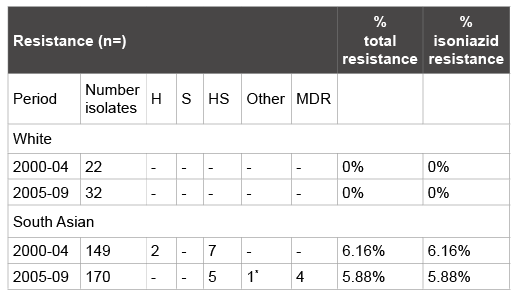
Table 1: Drug resistance 2000-2009
*
HS+Ethambutol
(Other ethnic groups 1 isolate in 2000-04, and 8 in 2005-09, all fully
susceptible)
*
HS+Ethambutol
(Other ethnic groups 1 isolate in 2000-04, and 8 in 2005-09, all fully
susceptible)
H= Isoniazid S=Streptomycin E=Ethambutol
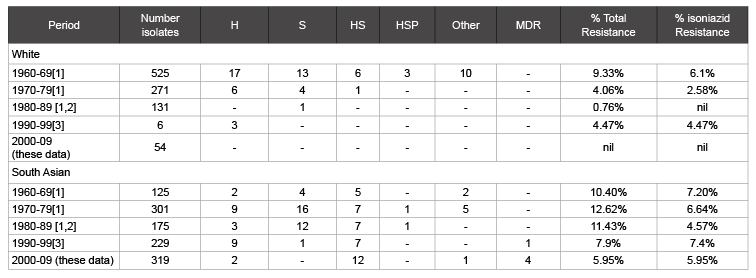
Table 2: Drug resistance 1960-2009 in newly diagnosed patients
H= Isoniazid S= Streptomycin P=Para-amino-salicylic acid MDR= Multidrug resistance
The first case of MDRTB was seen in our South Asian population in
1990-1999 [3]. In this 10 year cohort there were 4 cases, 2 previously
untreated new entrants from India (A) and Pakistan (B). The 2 further
cases were (C) in a household contact of (A), and (D) a close social contact
of case (C). A, C and D had identical MIRU-VNTR profiles [7]. All have
been cured and remain under long term follow-up. The occurrence of the
MDR-TB cases highlights the significance of rising drug resistance rates
in South Asia, with primary resistance rates of 0-51.2% reported including
0-14.2% MDR-TB in untreated patients and 10.7-58.3% in those with a
prior treatment history [8-12]. Since the South-Asian cohort currently
make up 90% of all local TB cases, and this cohort, particularly those
born abroad, have an annual incidence 20-30 times that of the UK born,
either white or South-Asian, it is not surprising that drug resistance, and
particularly MDRTB is detected more frequently in this group. The types
and incidence of drug resistance, of the overseas born, will continue to
drive the drug resistance profile of low burden countries, such as the UK
with a high proportion of TB cases born abroad [5].
Conflicts of Interest
None
Author Contributions
LPO prospectively collated the data, and ran the clinical service and
treated the patients. The other authors provided the bacteriology service
and quality control of the isolation of mycobacteria.
Funding
None
Download Provisional PDF Here
Article Information
Article Type: Short Communication
Citation: Ormerod LP, Maynard P, White R, Burch K
(2015) Drug Resistance Trends in M.tuberculosis:
Blackburn 2000-2009 Completion of 50 Years
Continuous Surveillance. J Infect Pulm Dis 1(1):
doi http://dx.doi.org/10.16966/2470-3176.103
Copyright:© 2015 Ormerod LP, et al. This is an
open-access article distributed under the terms
of the Creative Commons Attribution License,
which permits unrestricted use, distribution, and
reproduction in any medium, provided the original
author and source are credited.
Publication history:
Received date: 23 Sept 2015
Accepted date: 19
October 2015
Published date: 24 October 2015



