Abstract
Resolution of foul smelling purulent pleural fluid (empyema) with intrapleural instillation of TPA in four complicated patients. There are still doubts that TPA is not effective in empyema and recent authors have suggested that TPA is not effective without DNase. These case reports confirm that TPA is very effective in purulent empyema even in patients who are critically ill, provided the dose administered is adequate
Keywords
Intra pleural instillation; Purulent rancid pleural fluid
Abbreviations
TPA: Tissue plasminogen activator; CHF: Congestive heart failure; CXR: Chest X-ray; CT: Computerized tomography; LDH: Lactate dehydrogenase; PFA: Platelet function assays; DVT: Deep vein thrombosis; GERD: Gastroesophageal reflux disease; SOB: Shortness of breath; BiPAP: Bilevel positive airway pressure; ADP: Adenosine diphosphate; EPI: Epinephrine; LLL: Left lower lobe; RLL: Right lower lobe.
Introduction
Purulent pleural effusions occur in 40% to 60% of parapneumonic effusions and are more common in streptococcus infections [1]. In most hospitals TPA (Tissue Plasminogen Activator) is not considered and decortication is the only option. Complications of surgery are not uncommon and morbidity and mortality depends on age and associated comorbid conditions [2]. Four patients with several comorbidities presented with shortness of breath, fevers, and foul smelling viscous purulent fluid was obtained on thoracentesis/chest tube drainage. All patients agreed to TPA after been given the option for intrapleural TPA or surgery/decortication.
Case 1
JW: 77-year-old white female with history of CHF (congestive heart failure), peripheral neuropathy, cerebellar ataxia, gastric bypass surgery, hypertension and diabetes presented with symptoms of increasing shortness of breath, profound weakness and fevers dating back two to three weeks. CXR (Chest X-ray) showed a small pleural effusion and CT (computerized tomography) scan confirmed the small effusion with right lower lobe pneumonia. She was started on oral antibiotics but continued to have persistent symptoms and follow up CXRs a week later showed increasing pleural effusion and pneumonia. Thoracentesis revealed foul smelling viscous pleural fluid that grew out Streptococcus anginosus that was sensitive to most antibiotics (Figure 1) Pleural fluid analysis revealed the WBC of 58,875, neutrophils 90%, LDH (lactate dehydrogenase) >2500, pH-6.3 and glucose <3. On admission a chest tube was inserted under ultrasound guidance and IV antibiotics were initiated and continued for 4 weeks post discharge. PFA (Platelet function assays) were within normal limits and after informed consent was obtained, 25 mg of TPA was instilled intrapleurally daily for three days. Significant resolution of the left empyema was noted on CXR post TPA instillation and patient was discharged on day 5. Complete resolution of her effusion was noted on follow up CT scans 5 weeks post discharge (Figure 2).
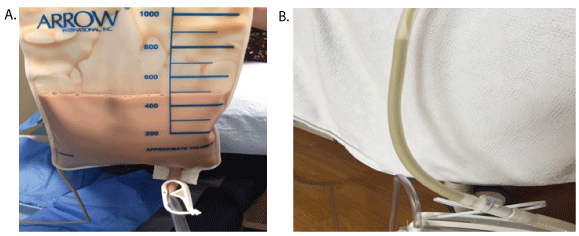
Figure 1: A) Thick, viscous, purulent foul smelling fluid obtained on thoracentesis in Patient 1. All 4 patient’s pleural fluid had similar characteristics. B) Purulent thick viscous fluid noted in chest tube. These viscous effusions could easily obstruct smaller chest tubes.
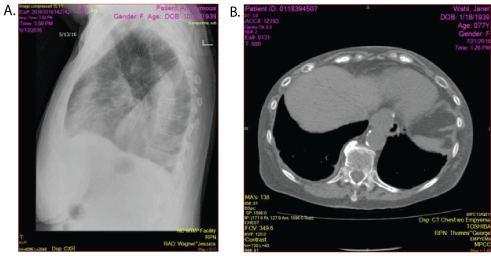
Figure 2: Patient 2-A) Lateral chest X-ray showing a large pleural effusion. B) CT scan showing complete resolution of right pleural effusion 4-6 weeks later.
Case 2
KK: 55-year-old white female with anti-phospholipid anybody syndrome, history of DVTs (Deep vein thrombosis), pulmonary embolus and bipolar disease presented with shortness of breath, feeling ill, fevers and hemoptysis. CT scan showed a large pleural effusion and thoracentesis revealed foul smelling viscous purulent fluid and the patient was transferred to our facility. Gram stain of the fluid showed many gram-positive cocci in chains and cultures grew out Streptococcus anginosus and Streptococcus intermedius mueller that were sensitive to all antibiotics. Pleural fluid analysis revealed that her LDH >2500, glucose <2, but pH was not recorded. Unfortunately no cell count and differential was obtained. A 28 F chest tube was placed under US guidance and IV antibiotics were initiated. PFA were normal and no hemoptysis was noted for 24 hours after admission. After informed consent was obtained 25 mg of TPA was instilled intrapleurally daily for 2 days. CT scan of chest on day 3 showed complete resolution of her empyema and no further does of TPA was given. Antibiotics were continued for four weeks but she refused CT scans on follow up. CXR done 4 weeks later showed no recurrence of her pleural effusion/empyema.
Case 3
RJ: 58 WM with a history of diabetes, Obesity, GERD (gastroesophageal reflux disease) and obstructive sleep apnea presented to the ER with history of SOB (shortness of breath) and flu like symptoms. He was in respiratory distress with severe hypoxia and BiPAP (Bilevel Positive Airway Pressure) was initiated. He was hypotensive and needed fluid resuscitation, IV pressers and IV antibiotics. His CXR and CT showed a left lower lobe pneumonia with mild to moderate pleural effusion. He continued to deteriorate the night of admission with worsening respiratory failure and renal failure and needed intubation and mechanical ventilation. CXR the next day showed a large pleural effusion and ultrasound estimated to amount to be around 1500 ccc and foul smelling purulent viscous fluid was obtained on thoracentesis. A 28 F Chest tube was inserted under US guidance and pleural fluid analysis showed a WBC of 97,524 with 95% neutrophils, glucose of 2, LDH of >2500 and pH of 6.9. Gram stain of the pleural fluid showed gram positive cocci and cultures grew group A Streptococcus. TPA was considered but not initiated as the PFA ADP (Adenosine Diphosphate) and EPI (Epinephrine) were over 300 and the risk of bleeding was considered to be high. The patient could not been weaned off the ventilator because of the persistent pleural effusion and pneumonia. After 3 days of AB therapy PFA showed the ADP was normal but the EPI was 210. After informed consent was obtained, 25 mg TPA was instilled intrapleurally without difficulty. Hemoptysis occurred a few hours after TPA instillation which was mild to moderate and no further doses of TPA were administered as chest CT the next day showed significant improvement of the empyema but persistent RLL (Right lower lobe) pneumonia. The patient was extubated 2 days post TPA instillation and the chest tube was removed several days later. The patient needed acute rehabilitation for significant myopathy and weakness from this illness. Follow up visits 4 weeks post discharge revealed persistent LLL (left lower lobe) atelectasis/scarring with minimal pleural effusion. Follow up CT scans done 6 months later showed the effusion had resolved and the pneumonic process/scarring to have improved significantly.
Case 4
GB: 83 WF with history of Diabetes, Anemia and Hypertension was admitted with weakness, hyponatremia. Rocephin was initiated for a small R pleural effusion and a RLL pneumonia. She continued to be symptomatic with enlarging pleural effusion and a liter of fluid was obtained on thoracentesis. The pleural fluid was mildly turbid and analysis of the pleural fluid showed the WBC to be 656 with 76% Neutrophils, glucose 172, LDH 407 and cultures were negative. Despite Rocephin, she continued to deteriorate with increasing pneumonia and recurrence of her pleural effusion. Attempt at placing a chest tube under US guidance failed and interventional radiologist under CT guidance inserted a 20F catheter chest tube. She appeared to respond initially but continued to feel weak and her SOB did not improve. The effusion persisted and several days later the pleural drainage turned purulent. Initial evaluation of the fluid revealed WBC of 10,940, 93% neutrophils, glucose of 2, LDH >1925 and cultures were negative. Analysis of the pleural fluid couple of days later showed the WBC of 3,56,500, 87% N, glucose of 57, LDH >2500 and cultures grew out streptococcus anginosis. Her antibiotics were switched to Meropenem and Levaquin. PFA were normal and after informed consent 25 mg of TPA was instilled intrapleurally daily for three days. She had no chest pain but had persistent coughing spells during instillation. The pleural drainage was serosangunious post TPA instillations. Her hyponatremia and anemia noted prior to TPA instillation persisted and she needed blood transfusion and fluid restriction. Follow up CXR and CT scans after 3 doses of TPA instillation showed significant resolution of the effusion but her pneumonic process showed only minimal improvement. The pleural fluid drainage was less than 50 ml 2 days after TPA instillation and the chest tube was removed. IVAB were continued for 4 weeks and follow up CXR and CT chest scan showed minimal pleural effusion and infiltrate.
Discussion
Several authors and a few randomized trials have shown the efficacy and safety of intrapleural TPA instillation in complicated pleural effusions and empyemas [3]. However, one randomized trial concluded that TPA was only effective with DNAse [4]. Our case reports again supports the concept that TPA is effective as a single agent not only in parapneumonic effusions but also in purulent foul smelling effusions (empyema). The efficacy of TPA in purulent effusions depends on the dose and chest tube size. Viscous purulent effusions and debris especially after TPA instillation will obstruct smaller chest tubes (Figure 1). Moreover, significant debris with these effusions with particles sizes up to ½ cm are not uncommon after TPA instillation and recommend chest tube size of 20F and larger in these situations [1,5,6]. Prior to TPA therapy, minimal or no drainage was noted in all four patients despite adequate chest tube size and placement. Good response was noted in all patients with first dose of TPA. Residual infiltrates and effusions are present in most all patients after TPA instillation and should not be considered failures, as these changes are also commonly seen post decortication. Associated pneumonia and pulmonary infiltrates do not respond in 3-4 days and if CXRs do not show improvement then CT scans of the chest is necessary to differentiate pleural effusions from pneumonic processes to determine success (Figure 3). Adequate response to TPA should be documented if approximately 2/3 of the pleural effusion/ empyema has resolved. Surgical options should be considered if minimal or no drainage occurs and if CT scans shows no improvement after 1or 2 doses of TPA. Complete resolution of pulmonary infiltrates and effusions are usually evident in 4-6 weeks. The one patient that received only one dose of TPA took over 4 months for his pneumonic process/ infiltrates to improve significantly. The need to add DNase to TPA was not necessary in any of our patients.
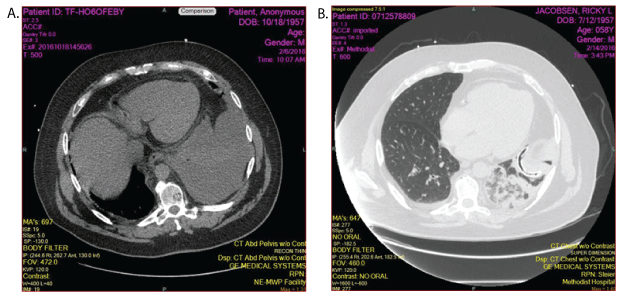
Figure 3: A) Patient 4: CT scan showing a large left pleural effusion. B) CT scan after first dose of TPA reveals the chest tube in adequate position with a small pleural effusion and consolidated lung that could not be differentiated by CXRs.
Conclusions
These four cases support the concept that adequate doses of TPA as a single agent with adequate chest tube size is effective in resolving even thick viscous, foul smelling, purulent pleural effusions (empyema). The cost effectiveness of TPA is estimated to be significant as the patients discussed above would need decortication, ICU stay, and hospital days ranging from 1-4 weeks. The risk of moderate or significant bleeding is less than 1% if the PFA is normal. The value of PFA in TPA/DNase combination has not been assessed and the risk of bleeding is unknown as the degree of augmentation of TPA with DNase is unknown. The addition of DNase may augment the potency of TPA and could be considered if smaller TPA doses are used or if TPA fails.
Download Provisional PDF Here
Article Information
Article Type: Case Series
Citation: Thommi G (2017) Complete Response to Intra Pleural Instillation of TPA in Four Complicated Patients with Purulent Rancid Pleural FLUID (EMPYEMA). J Infect Pulm Dis 3(2): doi http://dx.doi. org/10.16966/2470-3176.125
Copyright: © 2017 Thommi G. This is an openaccess article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
Received date: 07 Mar 2017
Accepted date: 06 Apr 2017
Published date: 12 Apr 2017




