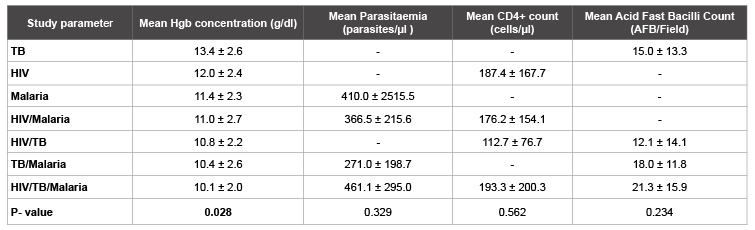
Table 1: Effects of Infection category on the Hb concentration, Parasitaemia, CD4+ count and Acid Fast Bacilli count, indicating levels of disease severity.


Ane Anyangwe Irene1 Mbi Alice Enekembe1 Henry Dilonga Meriki1,2 Nsongomanyi Fritz-Roland Fonkeng1 Theresa Nkuo-Akenji1,3*
1Department of Microbiology and Parasitology, University of Buea, P.O. Box 63, Buea, SW Region, Cameroon*Corresponding author: Nkuo-Akenji T, Department of Microbiology and Parasitology, University of Buea, P.O. 63, Buea, SW Region, Cameroon, Tel: +237 677770798; E-mail: wifon@yahoo.com
Summary: Given that malaria, TB and HIV are the world’s three most serious and common infections prevalent in low income countries, this study was designed to evaluate the impact of these diseases occurring as triple, double and single infections on haemoglobin levels, malaria parasitaemia, acid fast bacilli (AFB) and CD4+ cell counts.
Design: This was a 6-months hospital-based laboratory survey conducted on 400 consented participants between March and September 2009.
Setting: The study was conducted in the Limbe Regional Hospital which is the main reference centre for HIV, TB and malaria for the South West Region.
Results: The mean haemoglobin concentration of those with mono-infection of TB (13.4 ± 2.6 g/dl), malaria (11.4 ± 2.3 g/dl) and HIV (12.0 ± 2.4g/dl) were higher when compared with those of co-infections with malaria/ HIV (11.0 ± 2.7 g/dl), TB/malaria (10.4 ± 2.6 g/dl), HIV/TB (10.8 ± 2.2 g/dl) and HIV/TB/malaria triple infection (10.1 ± 2.0 g/dl). Mean parasite density in malaria mono-infection was 410.0 ± 2515.5 parasites/µl, that of TB/malaria co-infection was 271.0 ± 198.7 parasites/µl, HIV/malaria co-infection was 366.5 ± 215.6 parasites/µl and HIV/TB/malaria triple infection was 461.1 ± 295.0 parasites/µl when CD4+ cell count was considered, those with triple infection had a mean CD4+ cell count of 193.3 ± 200.3 cells/µl, those with co-infections of HIV/malaria and HIV/TB co-infections had CD4+ cell count of 176.2 ± 154.1 cells/µl and 112.7 ± 76.7 cells/µl respectively while patients with HIV mono infection had a mean CD4+ cell count of 187.39 ± 167.71 cells/µl. We recorded the highest mean AFB count in patients with triple infection (21.3 ± 15.9 AFB/ field), followed by those co-infected with TB/malaria (18.0 ± 11.8 AFB/Field) and those with mono-infection of TB (15.0 ± 13.3 AFB/Field). Those with HIV/TB co-infection recorded the least number of AFB count (12.1 ± 14.1 AFB/Field).
Conclusion: We therefore concluded that triple infection with TB, HIV and malaria leads to an increase in malaria parasitaemia, AFB count and decreased Hgb levels with no impact on the progressive depletion of CD4+ cells in HIV infection.
Triple infection; Malaria; Tuberculosis; HIV; Haemoglobin levels; CD4+ cell counts; Acid fast bacilli
Malaria, Tuberculosis (TB) and Human Immune deficiency virus/ Acquired Immune Deficiency Syndrome (HIV/AIDS) are 3 of the world’s most common and serious infectious diseases that underline development in low and middle- income countries [1,2]. These infections are not only associated with poverty, but also occur in the same geographic zone and have major public health implications [3]. These three infections together claimed 5-7 million lives in 2001 [4]; annually, approximately 5 million People die every year of these illnesses with humanitarian, economic and social impact which is still not fully measured [5].
Despite the wide use of life attenuated vaccine and several antibiotics, TB, one of the oldest forms of recorded human affliction is still a big killer among infectious diseases [6]. It is estimated that M. tuberculosis has affected approximately 2 billion people, with 13.7 million existing cases and nearly 2 million deaths annually [7]. There is one death every 15 seconds and 8 million people develop TB every year [6]. Without treatment, up to 60% of people with the disease will die [8]. Essentially most of these cases are in the third world [9] reflecting the poverty and the lack of healthy living conditions and inadequate medical care [10].
On the other hand, malaria is prevalent in tropical settings where access to preventive and curative services is limited [11] and HIV/AIDS has a devastating effect on human lives [12]. In 2013 thirty five million people were living with HIV and more than two thirds of new HIV infections are in Sub-Saharan Africa [13]. Few studies have been carried out to assess the severity of co-infection of these diseases and their effects on parameters such as Haemoglobin (Hgb), Malaria parasitaemia, Acid Fast Bacilli (AFB) and CD4+cell counts. Such studies are necessary to generate data which can be exploited for better management of these infections.
We administered a standard questionnaire to obtain demographic data, clinical symptoms of patients and the hygienic conditions they were living in additionally, knowledge of patients on HIV, TB and malaria, their risk factors, modes of transmission, preventive measures and past medical history was also assessed.
The malaria parasite was counted against 200 leucocytes in a thick film, while assuming an average leukocytes count of 8000 cells/µl of blood [14]. Malaria parasitaemia was categorized as low (<5000 parasites/µl), moderate (5000 -10000 parasites/µl blood) and high (>10000 parasites/ µl blood)
Following the manufacturer’s instructions, Hgb concentration was measured using the URIT-12 haemoglobin meter (URIT medical electronic Co. Lt Guangxi, China). Briefly a drop of blood was placed on the Hgb concentration electronic test card which was inserted into the haemoglobin meter and the Hgb read directly.
AFB counts were determined from sputum smears stained using the Ziehl Nielsen staining technique and at least 100 microscopic fields were examined following standard procedures [15].
The Uni- Gold rapid test kit (Trinity Biotech PLC, Bray, Ireland) was used to detect HIV/AIDS-1/2 antibodies. Essentially, 50 µl of freshly collected whole blood was dropped on the sample pad of the HIV test strip and allowed to freely diffuse into the strip. Test results were read after 15 minutes from corresponding colour changes on the control and patient portion of the strip. All HIV positive results by Uni-Gold rapid test were confirmed with SD Bioline (Standard Diagnostics, INC. 156-68 Hagaldong, Korea) which differentiated infections caused by HIV-1 from HIV-2. HIV seropositive status was based on the presence of antibody to either HIV-1 or 2 in blood.
Total CD4+ cell counts were determined using Becton Dickinson FACS Flow counter (KAPTAN SCIENTIFIC INC.). Subjects with CD4 cell count < 200 cells/mm³ of blood were considered to be in the advanced stage of HIV disease, while those with counts 200-499 and ≥ 500 were considered to be in the chronic and asymptomatic stages of HIV disease respectively.
Ethical approval and Administrative authorisation were obtained from the South West Regional Delegation for Public Health and the Limbe Regional Hospital. Each participant signed a consent form before enrolment.
Epi Info Version 3.5.3 was used to enter data and Excel 2007 was used to obtain the general statistics parameters of mean and Standard Deviation (SD). Chi square analysis was used to verify statistical difference. P-value of ≤ 0.05 was considered to be significant.
Out of the 400 participants 244 were females (61%) and 156 males (39%). The age range of participants was 15-49 years and mean age was 33 ± 9.5 SD years. The overall prevalence of TB, HIV and malaria occurring as mono-infections was 11.8%, 29.8% and 23.3% respectively. When co and triple infections were considered, there were 39 (9.8%) TB/HIV, 6 (1.5%) TB/ malaria, 85 (21.3%) HIV/ malaria and HIV/TB/malaria 10 (2.5%).
Overall, the mean haemoglobin concentration for the entire study population was 11.4 g/dl. Mean Hgb concentration was 11.0 ± 2.7 SD, 10.8 ± 2.2, 10.4 ± 2.6 and 10.1 ± 2.0 in patients infected with HIV/malaria, TB/HIV, TB/malaria and TB/HIV/malaria respectively. The mean Hgb concentration of those with TB mono infection (13.4 ± 2.6), malaria mono infection (11.4 ± 2.3) and HIV alone (12.0 ± 2.4) were higher when compared with co- infections. Those with triple infections had the lowest mean Hgb concentration. The difference in mean Hgb was statistically significant (p=0.028).
The mean parasite density in single malaria infection was 410 ± 2515.5 parasites/µl. When this was compared with the parasite density in co and triple infections, those with TB/HIV/ malaria triple infection had the highest mean parasitaemia (461.1 ± 295.0 parasites/µl). The lowest mean parasite density (271.0 ± 198.7 parasites/µl) was observed in patients coinfected with TB/malaria. However the difference in the mean parasite density was not statistically significant (p=0.329).
Mean CD+4 cell count for the study population was 178 ± 159.4 cells/ µl. Patients with TB/HIV/malaria triple infection had the highest mean CD4+ cell count of 193.3 ± 200.3 cells/µl, followed by patients with HIV mono infection (187.4 ± 169.7 cells/µl) while TB/HIV co-infection had lower CD4+ cell counts of 112.7 ± 76.7 cells/µl. However the difference in CD4+ cell counts in the various infection categories was not statistically significant (p=0.562).
Based on AFB count of the study population, the mean AFB count was 15 AFB/Field. Those with TB/HIV/ malaria triple infection recorded the highest mean count (21.3 ± 15.9 AFB/Field) followed by those coinfected with TB/ malaria (18.0 ± 11.8 AFB/field). The count for TB/HIV co-infection and TB mono infection was 12.1 ± 14.1 AFB/field and 15.0 ± 13.3 AFB/field respectively (p=0.234) (Table 1).

Table 1: Effects of Infection category on the Hb concentration, Parasitaemia, CD4+ count and Acid Fast Bacilli count, indicating levels of disease severity.
Knowledge of the effects of the co-existence of HIV, malaria and TB on the overall health of patients is important for proper management of these diseases. Existing data are not sufficient to provide a clear picture on the interactions between TB, HIV and malaria co-infections. It is barely 16 years that a picture of an association between these infections began to emerge [4,16]. An understanding of the transmission and clinical features of TB, HIV and malaria co-infections is important particularly since these infections are prevalent in poor countries such as Cameroon that have limited resources for prevention and treatment.
In this study, TB/malaria, HIV/TB, HIV/malaria and HIV/TB/malaria co-infected patients recorded lower mean Hgb levels compared with those for mono infections of malaria, HIV and TB. The lower levels of Hgb in co-infected patients could be as a result of an increased burden on erythropoiesis (production of red blood cells). In co-infected persons, P. falciparum and HIV use up erythropoietin (a protein) which is the most important single factor which controls the process of erythropoiesis.
Studies have shown that HIV can complicate the diagnosis of TB [17,18], others have shown that TB and malaria are more prevalent in the rainy season [4,19] and that there is an association between HIV, malaria and TB co-infections and disease severity. However most of these have used small sample sizes. In the present study in which a larger sample was used, it was established from our data that malaria parasitaemia was higher in triple infections (461.1 ± 295.0 parasites/µl) when compared with parasitaemia in dual infections of HIV/malaria (353.7 ± 292.0 parasites /µl) and TB/malaria (271.0 ± 198.7 parasites /µl) or malaria occurring as mono infection (410.0 ± 2515.5 parasites /µl). The finding that parasitaemia was higher in subjects infected with triple infections of HIV, TB and malaria suggests that immunity was compromised by these diseases.
A related study in Cameroon showed a higher risk of TB and malaria co-infections in HIV positive subjects [19]. The present study has gone further to show an association between triple co-infections of malaria, HIV and TB and severity of these co-infections as assessed by the differences in their levels of Hgb, malaria parasitaemia, CD4+cell count and AFB counts in Cameroon. Some studies have shown associations between co-infections and CD4+ cell counts [16] but no clear relationship has been established. Based on this study the mean CD+4 cell counts for the study population was 178 ± 159.4 cells/µl. Patients with TB/HIV/ malaria triple infection had the highest mean CD4+ cell count followed by patients with HIV alone (187.4 ± 169.7 cells/µl) while those with HIV/ malaria and TB/HIV co-infection had CD4+ cell counts of 176.2 ± 154.1 and 112.7 ± 76.7 cells/µl respectively. However the difference in CD4+ cell counts in the various infection categories was not statistically significant (P=0.562). This is different from the study carried out by [20] reported that an increase of one log in HIV viral load occurs during febrile malaria episodes enhancing susceptibility to malaria in HIV infected patients and this was found to facilitate the geographic expansion of malaria in areas where HIV prevalence was high.
Tuberculosis has been found to serve as a “sentinel” for HIV seroprevalence [21]. People with HIV have suppressed immunity and as a result, a higher chance of reactivation of dormant TB bacilli. In the present study, Patients with triple infections had the highest mean AFB count and this group has a higher chance of reactivation of dormant TB bacilli than their counterpart with dual and mono infections. Those co-infected with HIV/TB had lower AFB count than those with TB only suggesting that HIV complicates the diagnosis of TB due to alteration of the normal host immune response to Mycobacterium tuberculosis in persons with HIV. Cavitation and transfer of bacilli into respiratory secretions is markedly reduced hence making diagnosis difficult.
The data from the present study indicates that triple infection with TB, HIV and malaria increase malaria parasitaemia, AFB count and decreased Hgb levels with no impact on the progressive depletion of CD4+ cells in HIV infection.
Download Provisional PDF Here
Article Type: Research Article
Citation: Irene AA, Enekembe MA, Meriki HD, Fonkeng NF, Nkuo-Akenji T (2016) The Effect of Malaria/HIV/TB Triple Infection on Malaria Parasitaemia, Haemoglobin Levels, CD4+ Cell and Acid Fast Bacilli Counts in the South West Region of Cameroon. J Infect Pulm Dis 2(1): doi http://dx.doi.org/10.16966/2470-3176.110
Copyright: © 2016 Irene AA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access