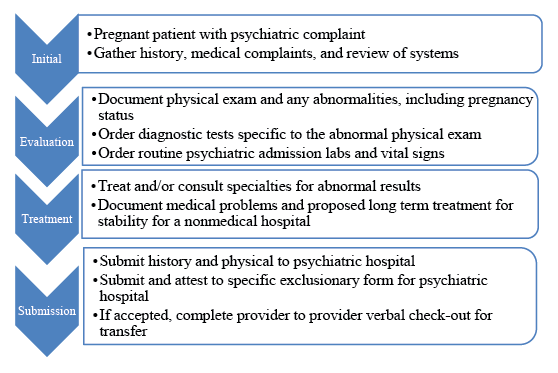
Figure 1: Flowchart for Psychiatric Admission Process [1].


Sandy Lee1 Veronica Tucci2* Nidal Moukaddam1 Ameigh V Worley3 Asim Shah1
1Menninger Department of Psychiatry and Behavioral Sciences, Baylor College of Medicine, Houston, Texas, USA*Corresponding author: Veronica Tucci, Section of Emergency Medicine, Baylor College of Medicine, Ben Taub General Hospital, 1504 Taub Loop, Houston, Texas 77030, USA, E-mail: vtuccimd@gmail.com
Objective: To address the process of admitting pregnant patients to a psychiatric hospital from an emergency room.
Case presentation: A 22 year old G3P0A2L0, 14 week pregnant female presented to the emergency room with a mood and psychotic disorder. She received a “medical clearance” and was placed on the transfer list for a psychiatric hospital. Due to her pregnancy status, she remained in the emergency room for an extended period of time and was rejected from the first hospital. Eventually, she was admitted to the county hospital.
Conclusion: Gaining psychiatric admission for pregnant patients can be cumbersome based on their pregnancy status and physiological changes that present with abnormal appearing labs or vital signs. Consulting with in-house psychiatrists, evaluating/treating medical problems, and documenting acceptable ranges of lab values and vital signs for a pregnant patient may assist in getting a pregnant patient the psychiatric help they need.
Medical clearance; Exclusionary criteria; Pregnancy; Psychiatric inpatient hospitalization; Psychiatric emergency
The deinstitutionalization of psychiatric state hospitals and poor funding for community outreach programs has led to an influx of mentally ill patients in prisons, jails and emergency departments (ED) that assist those in a mental health crisis [1]. Pregnancy does not confer immunity to psychiatric illness, and pregnant women, like many of their mentally ill peers, frequently turn to the ED for help. Unfortunately, the ED is not equipped to provide the kind of long-term care that many of its psychiatric patients require. Many EDs do not even have access to a psychiatrist to assist the Emergency Physician (EP) in stabilizing and managing the patient’s condition prior to inpatient hospitalization. Moreover, even for the fortunate EDs with in-house psychiatrists to help guide management, the bright lights, loud noises, and flurry of activity seen in many EDs are a far cry from the quiet and controlled atmosphere that is best for our patients. In order to transfer patients to an appropriate inpatient setting for managing their acute psychiatric crisis, EPs must medically clear the patient and then find a facility willing to admit the patient to their ward. In this paper, we utilize a case example to demonstrate the various hurdles facing pregnant psychiatric patients and their providers as they attempt to secure admission to a psychiatric hospital. We also propose how providers can work within the system to expedite the process.
A 22 year old G3P0A2L0, 14 week pregnant (confirmed by ultrasound), African American female presented to the county Emergency Department by police for “nudity and bizarre behaviors” in public. Within the ED, she was found to be disorganized, screaming hypersexual statements and required nonviolent restraints as her behavior escalated and she was not responsive to verbal redirection and limit setting by ED staff. She was reportedly off of her psychotropic medications for one week and had a history of multiple psychiatric diagnoses ranging from unspecified mood and psychotic disorder to mild intellectual disability. Two psychiatrists in the ED evaluated the patient and recommended admission to an inpatient psychiatric hospital with a provisional diagnosis of schizoaffective disorder.
Inpatient psychiatric hospitals generally require medical evaluation before they accept patients for admission. This is sometimes referred to as “medical clearance” or a “medical stability assessment.” At a minimum, these evaluations include the patient’s history and physical examination, but they generally also include basic labs, vital signs, and baseline level functional evaluations [2].
In the current case, our patient’s history was limited by her acute psychiatric state. On examination, she was found to be mildly tachycardic, but her heart rate normalized once her agitation was addressed. The labs showed mild anemia (often seen during pregnancy) and hypokalaemia at 2.8. Her potassium was repleted and repeat testing showed a normal level of 4.2. Following correction of these abnormal findings, the Emergency Physician determined that the patient was stable for inpatient psychiatric treatment. She was placed on a transfer list and copies of her visit were sent to local inpatient psychiatric units for consideration.
The patient’s length of stay in the county ED was over 15 hours before she was rejected from the first psychiatric hospital who had reviewed her file. Each psychiatric hospital dictates its own criteria for admission and this particular one required approval from the director for pregnant patients.
After a total of 35 hours in the ED, no other admitting facility could be secured despite having no physical symptoms requiring inpatient obstetric admission, so she was admitted to the adjoining psychiatric unit of the county hospital. The case illustrates the lengthy wait time for a pregnant patient requiring psychiatric admission, as well as consequences of not understanding the medical clearance requirements prior to beginning the admission process.
Several studies comment on psychiatric disorders in pregnant patients, and for those with severe cases, inpatient hospitalization is necessary. In 2011, 136 million visits were made to the ER in the United States[3]. Of those, 892,000 were transferred to a psychiatric hospital [3]. It is unclear how many of those transfers were pregnant, and no studies to date define the number of mental health emergencies in pregnant patients visiting the ED. That said, it is estimated that 10-15% of pregnant patients suffer from mental illness, particularly depression [4].
Khalifeh et al. [5] analyzed the United Kingdom National Confidential Inquiry for Suicide and Homicide for those with mental illness and their findings suggest that suicide in the perinatal period were higher for those with depression who did not receive psychiatric treatment. There is even more limited data on bipolar disorder and schizophrenia in pregnancy. Some studies have found a high rate of relapse (25-70%) in bipolar disorder during the postpartum period [6,7]. For those with any mental illness during pregnancy, if left untreated, the illness can affect prenatal care and thus lead to negative outcomes for the fetus/neonate, and mother [8].
The term “medical clearance” is more accurately defined as a medical assessment and stabilization. It is the process by which an emergency physician attests objectively and subjectively that the patient does not have an emergent medical condition that would preclude them from receiving mental health care at a hospital that would be better served on a medical floor. It has been proposed that the form include medical diagnoses with management/treatment recommendations for those assuming patient care at another hospital [9]. There is no clear consensus for a medical clearance of a patient before being considered for admission [1], but generally each hospital requires that such “stability” include normal limit vital signs (i.e. systolic blood pressure (SBP) 80-180, diastolic blood pressure (DBP) 50- 110), complete blood count, basic metabolic panel, urine drug screen, urine pregnancy test, and occasionally, a creatinine phosphokinase test. Accepting hospitals also look for a medical review of systems and physical exam to rule-out of medical causes that could present with psychiatric symptoms [9].
Pregnancy is wrought with physiological changes which can pose problems for those seeking psychiatric admission. Certain hospitals automatically exclude pregnant females, while others exclude those <20 weeks, >32 weeks, or high risk pregnancies (various Houston exclusionary forms). By properly documenting the normal values of pregnant patients, this may facilitate the admission process. The cardiovascular system has the most pronounced changes starting in the first trimester and rising again during delivery [10]. Generally, cardiac output increases greatly due to increase in stroke volume (increase blood volume and decrease systemic vascular resistance (SVR)) or heart rate [11]. Heart rate may increase by 10-18 beats per minute (bpm) [11]. Blood pressure generally falls by up to 10 mm Hg in the first trimester because of a decrease in SVR[10], with SBP and DBP reaching its lowest at about 24 weeks and resuming non-pregnant values by term [10]. On physical exam, one may hear a S3 gallop, low grade systolic ejection murmur, or louder S2 split on inspiration from increased blood flow [11]. Respiratory changes are minimal in pregnancy and one will find no major changes in respiratory rate or physical exam despite an increase of oxygen consumption by 30-50 mL/min [11,10].
Lab values may show compensated respiratory alkalosis [11]. Hematologically, plasma volume increases greatly and red cell volume increases, leading to physiologic anemia with a decline in hematocrit [11]. The average hemoglobin (Hb) level is 11-12 g/dL in pregnancy, and those with a Hb of less than 11 g/dL should prompt further work-up of anemia [10]. White blood cell levels may fall between 5,000-12,000/L in pregnancy but can reach up to 15,000/L [10]. Due to elevated and sustained estrogen levels, pregnancy also increases coagulability and thus risk for thromboembolism, prompting further work-up if a female complains of lower extremity pain [10]. Dependent edema is normal in pregnancy, especially during the latter third trimester[11]. Other changes found in pregnancy include increased urinary frequency, glucosuria, a slight decline in creatinine (0.5-0.6 mg/dL) and blood urea nitrogen (8- 10 mg/dL), acid reflux symptoms, constipation, increase in total alkaline phosphatase, cholesterol, postprandial hyperglycemia (due to human placental lactogen), and an increase in thyroid hormone binding globulin[11].
The manifestations of normal maternal physiology may prevent a patient from being “medically cleared” for transfer due to the inflexibility of exclusionary criteria at inpatient hospitals. At present, there is no modification for the pregnant state allowing for these physiologic changes. In addition to being excluded due to normal maternal variations as noted above, many inpatient units have pregnancy (regardless of trimester or presence/absence of complications) as an exclusionary criterion, leaving the patient and physician with a limited number of facilities from which to choose.
The medical clearance/stability process can be cumbersome and claims have been made that lab work in the ED is unnecessary and often does not change the outcome [12]. Nonetheless, these facilities are the gatekeepers for the admission process and long-term care. Psychiatric hospitals have different capabilities (i.e., physical therapists in-house), staffing ratios, administrative burdens and even prior experience (i.e., a patient that committed suicide using tubing from oxygen).
EPs unfamiliar with the process should consult with an in-house psychiatrist. If the EP has no access to a psychiatrist, we recommend obtaining the exclusionary criteria from each of the local inpatient facilities. Knowing upfront what is required by a particular facility before the patient is able to be accepted will avoid ED frustrations of refusing a medically cleared patient while also minimizing the length of stay for the pregnant patient in the ED. Ignorance of exclusionary criteria will inevitably lead to an increased cost burden related to prolonged stays. It is also imperative that EPs understand the administrative burdens and criteria at potential local facilities which often reflect staffing limitations and training. Understanding such limitations will enable the EP to prioritize to which facility they will attempt to initially admit the patient (Table 1).
| Vital signs (VS): Blood Pressure: Temperature: Respiration: Weight: | ||
| Yes | No | Exclusionary Criteria |
| Patient is being transferred primarily for placement | ||
| Patient has a primary diagnosis of mental retardation and/or developmental disabilities without psychiatric symptom or diagnosis | ||
| Patient has a primary diagnosis of alcohol or substance use without psychiatric symptom of diagnosis | ||
| Patient who has overdosed and are in the Intensive Care Unit (ICU) and have not regained full consciousness and do not have stable VS for the last 8 hours after discharge from ICU care | ||
| Patients with physical ailments that may be better treated in a medical facility with support and monitoring | ||
| Symptomatic cardiovascular and respiratory problems | ||
| Pregnant patient who is <20, >36 weeks gestation and/or a patient with high risk pregnancy requiring more than normal prenatal care | ||
| Tubing that requires maintenance by a nursing staff (foley catheter, feeding tube, Hep locks, subclavian lines, tracheostomy tube) and a patient who is unable to care for themselves | ||
| Ongoing IV therapy, Hep locks, subclavian lines, suctioning | ||
| Active pulmonary TB or medical isolation | ||
| Medical equipment that may require electricity or oxygen therapy | ||
| Patient requiring physical therapy or rehabilitative services | ||
| Post-operative patients require, 48 hours of stable vital signs and lab values | ||
| Systolic blood pressure >180 or <80 and diastolic blood pressure >110 or <50 | ||
| Patient with out of control diabetes or is in diabetic ketoacidosis | ||
| Patient with infectious process requiring IV antibiotics | ||
| Dementia, delirium, brain injury or severe cognitive impairment | ||
| Patient unable to complete activities of daily living (ADLs) independently | ||
| Patient requiring peritoneal or renal dialysis | ||
| Lab abnormalities: Acetaminophen level >100 mg/dL, WBC >15,000, Temp >101, Blood alcohol level >180 mg/dl, CPK >1,500 or >1,000 with elevated temperature and muscle rigidity | ||
| Patient requiring blood, platelet, or active parenteral chemotherapy administration | ||
| Open, drainage wounds, stage 2-4 pressure ulcers requiring sterile equipment or packing | ||
| Patient requiring 1:1 sitter | ||
| Patient with a history of multiple falls or condition that causes falls | ||
| Patient with end stage disease | ||
| Patient with a history of violence may need approval from Chief Medical Director | ||
Table 1: Sample Exclusionary Criteria for Psychiatric Admission (Adapted from various sample exclusionary criteria).
We recommend that EPs who do not have the benefit of a psychiatrist or who are unable to secure copies of their inpatient unit’s exclusionary criteria start by ordering, at a minimum, a complete blood count, basic metabolic panel, a urine drug screen, and a pregnancy test. We also recommend EPs correct or otherwise explain any laboratory values outside the acceptable range. For example, retesting the patient’s white blood cell count after their agitation has been controlled or retesting their creatinine level after they have received intravenous fluids.
If a new pregnancy is diagnosed at this visit, confirming intrauterine pregnancy location, gestational number, placentation, and fetal cardiac activity via ultrasound (US) is imperative. For previously confirmed intrauterine gestations, obtaining fetal heart tones using fetal Doppler US (normal 120-160 bpm) for pre-viable fetuses (<23 weeks) or performing fetal monitoring via a non-stress test (NST) with the aid of a Labor & Delivery nurse or Obstetrician, is indicated. There should be a thorough assessment evaluating potential high-risk obstetrical parameters (such as a pre-eclampsia workup for hypertension, proteinuria, or persistent headache; evaluation of vaginal bleeding; ruling out preterm labor with uterine tocometry or cervical fetal). For pregnancies presenting with possible labor, high risk findings, or abnormal fetal surveillance, EPs should initiate an obstetrical consultation. Obstetricians who refer their patients to the ED for psychiatric evaluation may help facilitate this process as well by documenting the pregnancy location, fetal heart tones (FHT), NST and any other specific recommendations for management of the pregnancy if admitted to an inpatient psychiatric unit.
The early postpartum period or even post 2-year delivery have also been found to be periods of increased psychiatric admissions [13], thus EPs should carefully describe findings in their documentation along with any recommendations for care. Depending on the hospital, many will also require a physician-to-physician discussion of the patient’s medical status, laboratory values, and reason for psychiatric admission (Figure 1).

Figure 1: Flowchart for Psychiatric Admission Process [1].
The psychiatric admission process for a pregnant patient can be confusing, but this editorial attempts to clarify the sequence of events for expedited care. If a patient is rejected from the first psychiatric hospital, EPs should attempt to rectify the reason. This may be in the form of lab values or clarifying documentation for submission to another hospital. Some studies have looked at wait times in the ER in regards to insurance status and perceived wait times by providers for the general ED population [14,15], but there is currently no data specifically looking at the wait times for the pregnant population seeking psychiatric admission.
Based on the providers’ experience with the admission process, collecting necessary labs, documenting medical issues and their treatments, and explaining abnormal pregnancy values/status, these items will present favorably for those reviewing the case. For those who are repeatedly denied admission and/or have been in the ED for an extended period of time, the only remaining option may be admission to a medical floor with both Obstetric and Psychiatric service consultations.
While it would be ideal for pregnant patients to have no admission bias against them, especially when psychiatrically indicated, working within the confines of the system will increase efficiency and quality of care until changes are made.
Download Provisional PDF Here
Article Type: Case Report
Citation: Lee S, Tucci V, Moukaddam N, Worley AV, Shah A (2016) Pregnant and Virtually Abandoned: The Multiple Hurdles of Medically Clearing and Admitting a Pregnant Patient to an Inpatient Psychiatric Unit. J Psychiatry Ment Health 1(1): doi http://dx.doi.org/10.16966/jpmh.105
Copyright: © 2016 Lee S, et al. This is an openaccess article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access