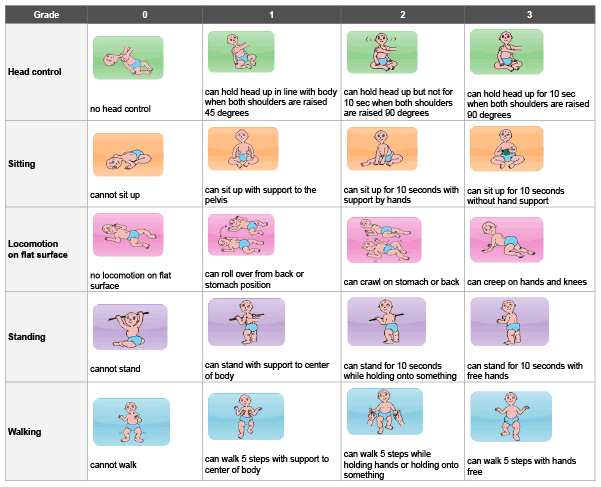
Figure 1: Ability for Basic Movement Scale for Children (ABMS-C)


Keiji Hashimoto1,* Manami Honda1,3 Anri Kamide1 Reiko Horikawa2
1Division of Rehabilitation Medicine and Developmental Evaluation Center, National Center for Child Health and Development, Tokyo, Japan*Corresponding author: Keiji Hashimoto, Division of Rehabilitation Medicine and Developmental Evaluation Center, National Center for Child Health and Development, 2-10- 1 Okura, Setagaya, Tokyo 157-8535, Japan, Tel: +81-3- 3416-0181; Fax: +81-3-3416-2222; E-mail: hashimoto-k@ncchd.go.jp
Objective: This study aimed to follow the data of gross motor function as determined by the mother-rated Ability for Basic Movement Scale for Children (ABMS-C) of healthy babies born at our hospital in the first year of infancy at 1, 3, 6, 9 and 12 months of age.
Material and methods: This study included babies who were born at our hospital land whose mothers gave informed consent to participate in the study. Babies with multiple births, premature babies, and low birth weight babies were excluded. The subjects were comprised of 1,961 babies. Questionnaires were distributed to their mothers, and the babies’ gross motor function and motor developmental age were evaluated according to the ABMS-C and Kinder Infant Development Scale (KIDS) at 1, 3, 6, 9,and 12 months of age.
Results: The mean - 2SD cut-off point for each parameter in the ABMS-C were as follows: ‘head control’ at 6 months (1.916), 9 months (2.304), and 12 months (2.176) of age, ‘sitting’ at 9months (1.9784), and 12 months (2.144) of age, ‘locomotion on flat surface’ at 9 months (0.8298), and 12 months (1.886) of age, and ‘standing’ at 12 months (1.152) of age. The physical motor developmental age (mean) as determined by KIDS was 1.956 at 1 month, 3.06 at 3 months, 6.88 at 6 months, 9.26 at 9 months, and 13.17 at 12 months of age.
Conclusions: By using the normal data of the mother-rated ABMS-C obtained in this study, we may be able to utilize this questionnaire to screen infants for delay of gross motor ability during early infancy.
Gross motor function; Ability for Basic Movement Scale for Children (ABMS-C); Kinder Infant Development Scale (KIDS); Questionnaire survey
Very few studies have investigated the performance of basic movements or gross motor function in pediatric patients at early infancy. It is difficult to administer the rather specialized scales used in rehabilitation medicine. Our group developed a new scale, the Ability for Basic Movement Scale for Children (ABMS-C), to make available an instrument that can easily assess a patient’s ability to perform basic movements at the bedside at a young age. We have already provided evidence for the validity and reliability of the ABMS-C with regard to assessment of functional ability in disabled pediatric patients [1].
On the other hand, there are no normal data for each item of the ABMS-C. Therefore, we cannot evaluate developmental delay of gross motor function in pediatric patients with some developmental disability using the ABMS-C.
In this study, we investigated the gross motor function of healthy babies born in our hospital at 1,3, 6, 9, and 12 months of age with questionnaires distributed to their mothers to elucidate the normal range of data of items in the mother-rated ABMS-C.
Among the women who received medical care for pregnancy and delivery at the National Center for Child Health and Development between December 2010 and January 2015, informed consent for participating in the mother and Child Cohort Study on Children’s Health and Development was obtained and data were collected overtime from 2,404 mothers and their infants. Among them, the babies from multiple births, premature babies, and low birth weight babies were excluded from the present study to investigate the range of data on each item of the ABMS-C in normal infants, and the subjects in this study comprised 1961 babies.
Gross motor function was evaluated according to the ABMS-C [1]. General development was scored according to the Kinder Infant Development Scale (KIDS) [2-4].The KIDS type A is administered to babies of 1to11 months of age, type B to babies of 1year to 2 years 11months of age, and type C to babies of 3 years to 6 years 11 months of age. The mothers were asked to fill out the ABMS-C and the KIDS questionnaires when the babies were 1,3,6,9 and 12 months of age.
The ABMS-C (Figure 1) issued to evaluate the degree of achievement of basic movement in babies by physicians and medical staff in daily practice. There are five evaluation variables: “head control”, “sitting”, “locomotion on a flat surface”, “standing”, and “walking”. Each variable is scored in 4 grades of 0,1,2, and 3. Each variable is scored based on the maximum capacity of babies at that time. For example, if a baby is unable to crawl or crawl on his/her stomach or back but is able to crawl on his/her knees with hipelevatedin “locomotion on a flat surface”, “locomotion on a flat surface” is scored as grade 3.

Figure 1: Ability for Basic Movement Scale for Children (ABMS-C)
KIDS are a tool to evaluate child development by those who observe the daily behavior of children at 0 year 1 month to 6 years 11 months of age. It takes 10-15 min for the examination and the KIDS consist of approximately 130 yes-or-no questions about the daily behavior of children. KIDS can be administered at any time and any place without limitation as a supplementary examination with other intelligence tests. In addition to the total developmental age, scores for developmental sub scales in nine areas of “physical motor”, “manipulation”, “receptive language”, “expressive language”, “language concept”, “social relationships with children”, “social relationships with adults”, “discipline”, and “feeding” can be calculated [2] Hashimoto et al. [3,4] previously demonstrated the validity of KIDS in disabled children.
The statistical software SPSS ® Statistics Desktop Version 22.0 (IBM) was employed.
This study was carried out as part of a large scale birth cohort study in which both mothers and their infants were included as subjects (a mother and small-for-gestational-age child cohort on children’s health and development). This study was approved by the ethical committee of the National Center for Child Health and Development. Informed consent was obtained from all mothers after a detailed explanation of the study was provided.
The characteristics of the infants in this study are summarized in (Table1).This study excluded babies from multiple births, premature babies, and low birth weight babies.
Table 2 summarizes the scores[mean ± standard deviation (SD)]on “head control”, “sitting”, “locomotion on flat surface”, “standing”, and “walking” of the ABMS-C and the physical motor developmental age (month) as determined by KIDS from1to12 months of age.
Table 3 summarizes the cutoff data (mean score -SD cutoff and mean score -2 SD cut off) for each item of the mother-rated ABMS-C at 1, 3, 6, 9 and 12 months of age.
As a result, similar to the Ages & Stages Questionnaires ® third edition (ASQ-3), which is used in the National Birth Cohort Study on Children’s Health and the Environment conducted by the Ministry of the Environment of Japan (the Japan Environment and Children’s Study [JECS]), [5] we can categorize babies into three groups according to the baby’s score on the ABMS-C as follows (Table 3):
i) If the baby’s score is in the □ area in (Table 3), it is above the Mean - SD cut off, and the baby’s gross motor function appears to be on schedule.
ii) If the baby’s score is in the ■ area, it is close to the cutoff. Provide learning activities and monitor.
iii) If the baby’s score is in the ■ area, it is below the Mean - 2SDcutoff. Further assessment with a professional may be needed.
Motor development in typical infants and toddlers is predictable and shifts from reflexive to purposeful movement, leading to the abilities to move against gravity, transition in and out of different body positions, and explore the environment by crawling, walking, and climbing. For infants born prematurely and for infants and toddlers who are not achieving typical motor milestones, discriminative measures to identify delays in motor development and the reasons for the delays are important, as are measures that are predictive of future diagnosis such as cerebral palsy [6].
The systematic review by Spittle et al. [7] evaluated assessments used to discriminate, predict, or evaluate the motor development of preterm infants during the first year of life. Eighteen assessments were identified; nine met the inclusion criteria. The Alberta Infant Motor Scale (AIMS), Bayley Scale of Infant and Toddler Development - Version III, Pea body Developmental Motor Scales - Version 2, Test of Infant Motor Performance (TIMP), and Toddler and Infant Motor Examination have good discriminative validity when examined in large populations. The AIMS, Prechtl’s Assessment of General Movements (GMs), Neuro Sensory Motor Development Assessment (NSMDA), and TIMP were designed for preterm infants and are able to detect more subtle changes in movement quality.
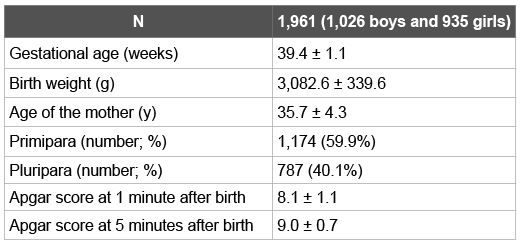
Table 1: Profiles of the participants
Results are shown as mean ± standard deviation or number (percent)
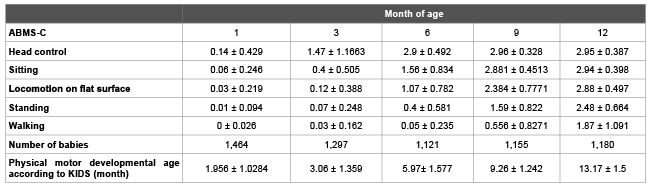
Table 2: Scores on each item of the ABMS-C and motor developmental age as determined by KIDS Results are shown as mean ± standard deviation.
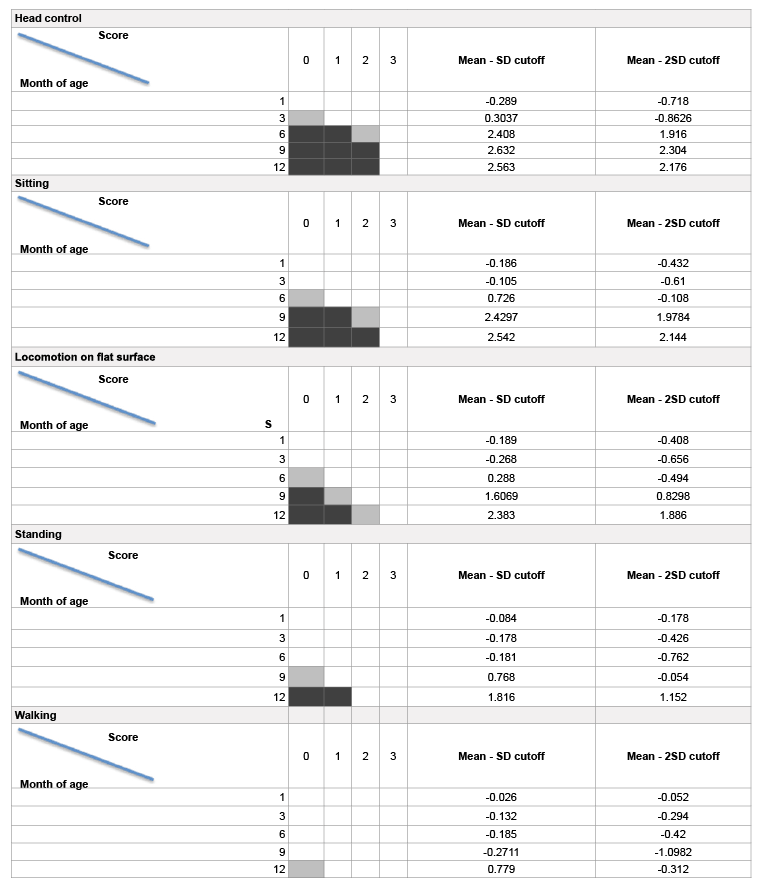
Table 3: Cutoff data for each item of the mother-rated ABMS-C
1. If the baby’s score is in the □ area, it is above the Mean - SD cutoff, and the baby’s gross motor function appears to be on schedule.
2. If the baby’s score is in the ■ area, it is close to the cutoff. Provide learning activities and monitor.
3. If the baby’s score is in the ■ area, it is below the Mean - 2SD cutoff. Further assessment with a professional may be needed.
In the field of pediatric rehabilitation, to assess the motor function of children with disability, the GMFCS, gross motor function measure (GMFM), functional independence measure for children (Wee-FIM), pediatric evaluation of disability inventory (PEDI), and Bailey motor developmental scale are very well known. Morris et al. [8]reported that the GMFCS has had, and continues to have, a major effect on the health care of children with cerebral palsy. The number of citations of the GMFCS has been increasing every year, and the classification system has had good acceptance internationally and across the spectrum of health professionals for use in research design and clinical practice by providing a system for clearly communicating children’s gross motor function. In a systematic literature review of assessment measures, Ketelaar et al. [9] concluded that only two evaluative assessment measures, the GMFM and the PEDI, fulfill the criteria for reliability and validity with respect to responsiveness to change in a child’s condition. After testing the reliability of the WeeFIM in 37 non-disabled children and 30 children with disabilities, Otten bacher et al. [10] found this instrument to be reliable. However, these instruments are not commonly administered during actual examinations by pediatricians because of difficulty of assessment.
It is difficult, however, to administer the rather specialized scales used in rehabilitation medicine. Our group developed the ABMS-C to make available an instrument that could easily assess a patient’s abilities to perform basic movements at a young age. One of the more useful points of the ABMS-C in comparison with other scales such as the GMFCS is that we can record the child’s ability to perform five different basic movements and then can monitor the progress of that child’s ability to perform each individual movement.
In this study, we could obtain data on the mother-rated ABMS-C from over 1,000 healthy normal infants. By using these data, we may be able to utilize this questionnaire to screen young infants for delay of gross motor ability.
There were several limitations in the present study. First, the assessments in this study were carried out based on mother-rated questionnaires and not on objective development tests administered by specialists. We must consider the possibility that mothers may tend to overestimate their own baby’s development compared with evaluation by a specialist. Last, to predict gross motor functional ability and general motor developmental ability, it is necessary to evaluate children at 2 or 3 years of age. Follow-up studies on the development of the children at 2 or 3 years of age using the same measure should be performed in a future study.
This study was supported by Health Labour Sciences Research Grant “Investigation of the pathogenesis of growth and developmental disorders in the mother-child cohort study (H22-next generation; general -008)” and the Grant from the National Center for Child Health and Development “Investigation of the pathogenesis of growth and developmental disorders in the seiiku birth cohort study (25-4, 26-19)”.
Download Provisional PDF Here
Article Type: Research Article
Citation: Hashimoto K, Honda M, Kamide A, Horikawa R (2016) Investigation of Normal Data for the Mother-Rated Ability for Basic Movement Scale for Children (ABMS-C) During the First Year of Infancy. Pediatr Neonatal Nurs 2(1): doi http://dx.doi.org/10.16966/2470-0983.109
Copyright: © 2016 Hashimoto K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access