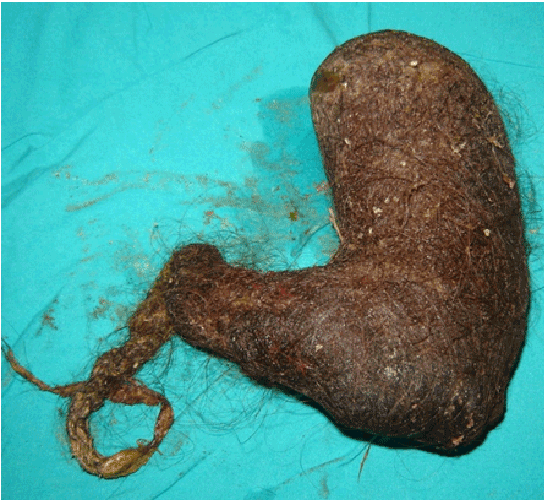
Figure 1: The trichobezoar in the stomach.


Mustafa Erman Dörterler* Mehmet Emin Boleken Ali Suat Erkoç
Department of pediatricsurgery, Harran University, Şanlıurfa, Turkey*Corresponding author: Mustafa Erman Dorterler, Department of Pediatric Surgery, Harran University, Şanlıurfa, Turkey, Tel: +90 (414) 318 34 20; Fax: +90 (414) 318 31 92; E-mail: m.e.dorterler@hotmail.com
Although bezoars of the gastrointestinal system are most frequently noted in the stomach, they may extend to the small intestine. Trichobezoars are generally seen in young females and most patients have psychiatric disorders. Medical, endoscopic, and surgical treatments are available. However, when the bezoar entirely fills the stomach, surgery is the only option.
Rapunzel syndrome; Bezoar
A bezoar is an accumulation of undigested materials in the gastrointestinal system, and it can be classified into four groups: phytobezoars, trichobezoars, lactobezoars, and pharmacobezoars [1,2]. Although bezoars of the gastrointestinal system are most frequently noted in the stomach, they may extend to the small intestine. Trichobezoars are more common in childhood, and most cases are females with psychiatric disorders [3]. Here, we describe a patient who presented to our hospital with chronic abdominal pain and was diagnosed with a gastric trichobezoar attributable to swallowing of hair.
A 14-year-old female presented to our emergency pediatric polyclinic complaining of intermittent abdominal pain for the previous 1 year and abdominal swelling, nausea, vomiting, and an inability to discharge gas or feces for 1 week. Over the previous 3 months, the patient had lost weight, associated with loss of appetite and vomiting after meals. The patient was below the 3% height and weight percentiles. Upon physical examination, the patient appeared pale and a mass was palpable in the left upper abdominal quadrant. Iron anemia was evident on laboratory examination. On questioning, the patient admitted that she ate her own hair. We made an initial diagnosis of a trichobezoar, and laparotomy was performed. The stomach was entered via an anterior gastrotomy and a mass extending toward the duodenum was completely removed (Figure 1). Upon postoperative psychiatric evaluation, slight mental retardation was evident, as was a compulsive disorder. The patient was followed-up by a pediatric psychiatrist and no recurrence was noted over a 6-month period.
Bezoars are masses that form in the digestive tract and are composed of swallowed foreign bodies or undigested foodstuffs. The masses may be formed of fruit and vegetable fibers (phytobezoars), hair (trichobezoars), milk and dairy products (lactobezoars), medications, or various foreign bodies including sand, chewing gum, and cork. Although trichobezoars are generally located in the stomach, they may also be found in the duodenum, ileum, jejunum, colon, or the Meckel diverticulum [4].
Although uncommon, patients may present with various complaints, but the most frequent is epigastric discomfort [1]. Mechanical obstruction caused by a giant trichobezoar with a long tail is termed Rapunzel syndrome. This is an intestinal obstruction that can create acute abdominal problems [5]. Our current case presented with abdominal pain more than 3 months in duration that was affecting daily activities.

Figure 1: The trichobezoar in the stomach.
Trichobezoars are usually found in young females. Most patients have psychiatric disorders and evidence mental retardation [6]. Upon psychiatric evaluation of our current case, her mental level was determined to be border line and obsessive compulsive disorder was diagnosed. The patient was followed-up by a pediatric psychiatrist. The literature contains many accounts of recurrence; to prevent this, predisposing factors must be eliminated [7]. When considering the risk of recurrence of a trichobezoar, it is essential to schedule a thorough psychiatric evaluation, plan medical and behavioral therapy, and monitor the patient closely.
Medical, endosopic, and surgical treatment options are available. Proteolytic agents that have been shown to be effective against phytobezoars have no effect on trichobezoars [8]. Although endoscopy can be used to remove small trichobezoars, endoscopy can only be used for preoperative diagnostic purposes if a trichobezoar completely fills the stomach. In such cases (as in our case), surgical treatment is the only option.
When young females with psychiatric problems present with gastrointestinal symptoms such as abdominal pain and vomiting, the possibility of a trichobezoar must be kept in mind. For Rapunzel syndrome, featuring a giant gastric bezoar, the recommended treatment is open surgery.
Download Provisional PDF Here
Article Type: Case Report
Citation: Dörterler ME, Boleken ME, Erkoç AS (2015) A Rare Cause of Chronic Abdominal Pain: Rapunzel Syndrome. Pediatr Neonatal Nurs Open Access 1(2): doi http://dx.doi.org/10.16966/2470-0983.106
Copyright: © 2015 Dörterler ME, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access