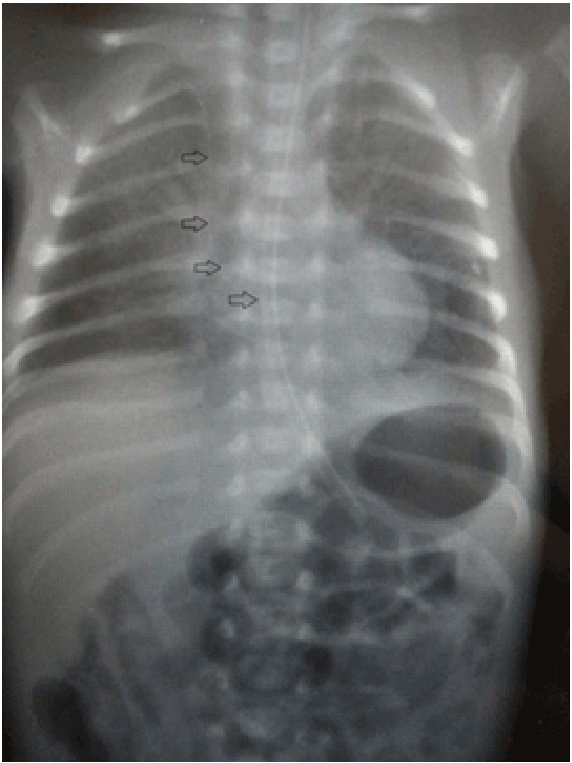
Figure 1: Chest x-ray of patient. Arrows are showing PICC in right ventricle.


Muhittin Celik1* Bedri Aldudak2 Heybet Tüzün1 Osman Akdeniz1 Serhat Samanc1 Osman İyi1
1Department of Pediatrics, Division of Neonatology, Diyarbakır Children Hospital, Diyarbakır, Turkey*Corresponding author: Muhittin Celik, Specialist in Neonatology, Department of Pediatrics, Division of Neonatology, Diyarbakır Children Hospital, Yenişehir 21100 Diyarbakır, Turkey, Tel: +90 412 224 57 51; Fax: +90 412 229 0147; E-mail: mehdincelik@hotmail.com
Pericardial effusion/cardiac tamponade are rare but life-threatening complications of peripherally inserted central catheter. The frequency of pericardial effusion/cardiac tamponade was reported between 0.7-1.8/1000 lines. Timely diagnosis and pericardiocentesis has been proven to be life-saving.
The patient was 1130 g birth weight neonate who presented with sudden cardiac arrest 13 days after the insertion of a peripherally inserted central catheter. The transthoracic echocardiography demonstrated severe pericardial effusion with evidence of cardiac tamponade. This was successfully treated with percutaneous subxiphoid pericardiocentesis. Totally 9 ml of fluid was collected; biochemical analysis showed that TPN solution infused.
Conclusion: Cardiac tamponade should be considered in any newborn with a peripherally inserted central catheter who presents with cardiorespiratory instability (cardiac arrest, bradycardia, cyanosis and metabolic acidosis), even when lines are believed to be placed correctly.
Peripherally inserted central catheter; Pericardial effusion; Prematurity
Peripherally inserted central catheters (PICCs) are commonly used in neonatal intensive care units to provide parenteral nutrition and medications for extremely low birth weight (ELBW) infants [1]. PICCs have been associated with a number of device-specific complications (occlusion, infection, thrombosis, breakage, migration, displacement) including rare but life-threatening complications such as pericardial effusion and cardiac tamponade [2,3].
Incidence of pericardial effusion/cardiac tamponade has been previously reported in literature between 0.7-1.8/1000 lines [1]. Review of literature demonstrated that in the majority of cases, which are complicated by a pericardial effusion after insertion of PICCs; the presentation was more than 48 hours after insertion. The shortest time interval between the insertion of catheter and development of cardiac tamponade in literature is around 24 hours [4,5].
Here, we report a case of successful pericardiocentesis, performed in an ELBW neonate who presented with cardiac tamponade 13 days after the insertion of a PICC.
A male neonate; 1130 g weight with a 29 week of gestation was born with an Apgar of 5 and 8 at 1th and 5th minute respectively. He was ventilated with nasal Continuous Positive Airway Pressure (nCPAP) for 3 days because of respiratory distress. A PICC (Vygon, Germany) was inserted electively on 5th day of life through the basilic vein in the right cubital fossa to access central vein. The chest X-ray showed the right position of the catheter. On day 13, unexpectedly, the patient deteriorated; he developed cardiac arrest and cardio-pulmonary resuscitation was initiated. He was intubated and subsequently was put on mechanical ventilation for respiratory support. Chest X-ray showed the catheter tip in the right atrium (Figure 1). The PICC was pulled back. Oxygen requirement of the patient increased up to 1.0, he developed tachycardia (heart rate 210/min) and hypotension (mean blood pressure <15 mm/Hg). Depending on the clinical findings pericardial effusion was suspected. Transthoracic echocardiography demonstrated marked pericardial effusion with evidence of cardiac tamponade. Pericardiocentesis was performed and 9 ml of fluid was aspirated. Biochemical analysis showed that it was composition of TPN solution. Echocardiography five minutes later showed increased contractility. The patient recovered quickly and mechanical ventilation support was discontinued after an hour. In follow up, echocardiograms performed in each 2 weeks showed no reaccumulation of the fluid and normal cardiac filling and contractility.
Pericardial tamponade should be considered immediately in any infant with PICC line who has a rapid onset of bradycardia, hypotension, desaturation, congestive heart failure and cardiac arrest. Pericardial tamponade is a rare but serious life threatening complication of PICC. The mortality rate of pericardial tamponade has been reported to be as high as 67% [6].
Agarwal et al. have reported a case of pericardial tamponade in a 24- week premature infant. Autopsy showed a pericardial effusion, a total of 5 ml of fluid was aspirated from the pericardial cavity [5]. The etiology pericardial effusion is not clear; however several possibilities have been proposed based on clinical and autopsy findings [7-9]. The myocardium in neonates may have areas of weakness; so it is not completely muscularized and because of this it is vulnerable to injury [8]. Repeated contact of the catheter tip with the cardiac wall with each contraction leads to endothelial cell damage and subsequent adherence of platelets and activation of the coagulation cascade. The resulting thrombus fosters attachment of the catheter tip to the heart, causing irritation of the endothelial cell lining by the infusate, causing osmotic injury. Through the damaged lining, fluid then diffuses into the pericardial space forming an effusion. In our case, we did not appreciate any thrombus at the catheter tip on echocardiogram or on removal.

Figure 1: Chest x-ray of patient. Arrows are showing PICC in right ventricle.
The biochemical analysis of pericardial fluid in our case was in compliance with TPN. Review of literature suggests that most cases of the pericardial effusion resulting from central lines do not show evidence of trauma, supporting the hypothesis that there is osmotic diffusion of infusate even before overt myocardial perforation occurs [7].
It is recommended that routine radiography should be performed on patients with tips near the heart to ensure that the tip has not migrated. The PICC tip should remain outside the cardiac silhouette but still within the vena cavae. Tip position in the high superior vena cavae or below the inferior vena cavae/right atrial junction should keep the PICC outside the pericardial reflections and thus minimize the risk of perforation. Studies have also suggested that the accuracy of chest radiography is suboptimal in predicting catheter position. Previous studies reported that the sensitivity and specificity of cheat radiography in evaluating inappropriate catheter position were 32% and 89% [10]. Therefore, at the slightest suspicion of such a complication, prompt evaluation with ultrasound of the abdomen and heart must be performed to save valuable time.
In conclusion, Any unexplained sudden onset of shock like symptomsinclude tachycardia, non-attributable to usual causes in neonates with a PICCs should raise the suspicion of migration of the PICCs tip causing pericardial effusion and pericardial tamponade.
Download Provisional PDF Here
Article Type: Case Report
Citation: Celik M, Aldudak B, Tüzün H, Akdeniz O, Samanci S, et al. (2015) Cardiac Tamponade in a Very Low Birth Weight Neonate with Peripherally Inserted Central Catheter. Pediatr Neonatal Nurs Open Access 1(1): doi http://dx.doi.org/10.16966/2470-0983.103
Copyright: © 2015 Celik M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access