
Figure 1: Test in progress on a Balance platform with a Balance screener

Arvind Gupta1 Col BK Prasad2*
1Senior Resident (ENT), INHS Asvini, Mumbai, India*Corresponding author: Col BK Prasad, Professor of ENT, Command Hospital (CC), Lucknow, India, Tel: 8698075965; E-mail: bkp1405@gmail.com
Introduction: Vertigo is known to occur in patients undergoing mastoidectomy. This study was conducted to determine pre and postoperative status of balance, using static posturography, in patients of chronic otitis media undergoing canal wall up and down mastoidectomy.
Material and Methods: 50 patients, having Chronic Otitis Media, without overt vestibular dysfunction, were included in a prospective case control study. 25 of them underwent canal wall up and remaining underwent canal wall down mastoidectomy. Assessment of balance, by computerized static posturography, was done pre-operatively and repeated post-operatively at the interval of one, three and six months. All patients were subjected to balance screener with Modified Clinical Test of Sensory Interaction and Balance for measuring mean postural sway velocity under 4 conditions, namely eyes open on firm surface, eyes closed on firm surface, eyes open on unstable surface and eyes closed on unstable surface.
Results: Mean postural sway velocity in patients undergoing canal wall up mastoidectomy, pre-operatively and after 1 month, 3 months and 6 months were lower in comparison to patients undergoing canal wall down mastoidectomy in similar intervals. The difference was significant, p value being <0.005. The values were deranged post-operatively in both groups but returned to normal in 6 months.
Discussion: Significant occult vestibular dysfunction exists in COM patients post-operatively both in canal wall up and canal wall down surgeries as compared to pre-operatively with possible compensation occurring after 6 month. Static posturography objectively measures postural stability, results of which can be documented graphically and numerically.
Balance; Posturography; Canal wall up and down; Balance platform; Balance screener; Postural sway velocity
The complex integration of sensory and motor systems is required for appropriate body balance, which allows precise maintenance of a stable posture or harmonic motion. Postural impairment in an individual occurs because of proprioceptive, vestibular, or visual alterations, which causes balance problems and interferes with quality of life [1].
Ideally, specific functional tests for the receptors in each semicircular canal, utricle and saccule are needed for a comprehensive vestibular evaluation. However, since all of the five vestibular organs work together in controlling and maintaining balance, three detecting angular acceleration and two detecting linear acceleration, it is difficult to develop and utilize specific tests to evaluate each organ separately. It is also difficult to devise tests that further evaluate right vestibular system versus the left vestibular system and/or isolate one vestibular organ in one ear versus the same vestibular organ in the other ear. Despite these handicaps, some tests have been developed and utilized in differential diagnosis of vestibular disorders.
The advent of computerized static and dynamic posturography has made the classical vestibular system tests more complete [1]. Computerized posturography, a multisensory assessment of balance, consists of two main tests namely sensory organization test (SOT) and Motor co-ordination test (MCT). The SOT battery quantifies an individual’s ability to maintain an upright stance with one or more inaccurate or absent sensory inputs. The MCT battery provides information about an individual’s response time to a perturbation. The test is carried out on a platform called Balance Platform and observed in Balance Screener.
Chronic otitis media (COM) is defined as an inflammatory process of middle ear which persists for more than 3 months which is characterized by irreversible tissue changes with or without tympanic membrane perforation and chronic otorrhea [2]. Some patients with COM suffer from vertigo due to the potent inflammatory response in the inner ear caused by middle ear infectious products, bacterial endotoxins and enzymes migrating through the round window membrane into the fluids of the inner ear, or through the effects of osteitis from mastoiditis on the development and blood supply of the endolymphatic sac or through a fistula in the lateral semicircular canal caused by the disease.
COM is of two types - mucosal and squamous. Mucosal COM is usually managed by tympanoplasty after the ear is made dry by medical treatment. Resistant cases, which do not dry up easily, require mastoidectomy. In these cases, Canal wall up (CWU) mastoidectomy is done to remove granulation tissue and/or hypertrophied mucosa and to achieve aditus patency with atticoantral ventilation. Repair of tympanic membrane and reconstruction of ossicular chain is done simultaneously. Squamous COM invariably requires surgical management either by canal wall up or canal wall down (CWD) mastoidectomy. The choice of procedure is based on extent of cholesteatoma, hearing status, Eustachian tube function, degree of pneumatisation of mastoid, presence or absence of complications and the condition of contra lateral ear. CWU mastoidectomy is preferred approach in cases of acquired cholesteatomas, secondary to tympanic membrane retraction pockets, restricted to attic and antrum with relatively good condition of mucosa of mesotympanum and rest of mastoid air cells. CWD mastoidectomy is preferred in cases of more extensive cholesteatoma, posterior canal wall erosion, possibility of poor follow up, unwillingness for second look surgery, complicated ear and in only hearing ear.
Patient with COM undergoing mastoidectomy often have a history of imbalance, dizziness or vertigo post operatively. Mastoidectomy results in the formation of a mastoid cavity which is anatomically and physiologically unsatisfactory. It can be associated not only with chronic ear discharge from the cavity but also vertigo due to exposure of semicircular canal or manipulation of middle ear ossicles during surgery [3].
Considering the current lack of research on the use of Computerized posturography, this study, using static posturography, was conducted to determine the pre-operative status of balance in patients of COM undergoing CWU and CWD mastoidectomy and to test the hypothesis that the two groups develop imbalance post-operatively and that there is a difference in status of balance in the two groups.
This prospective case control study was done between October 2014 to September 2016 in the Department of Otorhinolaryngology and Head & Neck Surgery of a tertiary care hospital of Indian Armed Forces. Clearance from Institutional Ethical Committee was obtained. A total of 50 patients, aged between 13 to 50 years, having squamous COM, were included in the study. There was no sex bias. 25 of them underwent CWU mastoidectomy and remaining 25 underwent CWD mastoidectomy. Assessment of balance was done by computerized static posturography once pre-operatively and thereafter post-operatively at the interval of one month, 3 months and 6 months in both groups of patients.
Patients with squamous COM without any overt vestibular dysfunction were included in the study. Patients with the following features were excluded:
A pre-designed proforma was used to record relevant information from individual patients. A detailed history was taken. ENT evaluation was carried out and final diagnosis of squamous COM arrived at. After taking an informed consent, assessment of balance was done by static posturography on balance platform (Figure 1), pre and post operatively. All patients were subjected to the balance screener with the Modified Clinical Test of Sensory Interaction and Balance (MCTSIB) using Balance Manager System using the NeuroCom System Version 9.0 (NeuroCom International Inc., Clackamas, Oregon, USA). The complete MCTSIB system includes static platform, integrating pressure sensors, data acquisition system and in-built software application for posturography data analysis.

Figure 1: Test in progress on a Balance platform with a Balance screener
MCTSIB measures the postural sway during four test conditions:
The subjects were asked to stand barefoot on the sensing platform surface of Static Force Plate (size 18 × 18 inches) with his/her feet aligned to previously determined markings, corresponding to foot size. They were made to stand straight with arms along the sides of the body, without moving during the whole recording period. Three trials, each of 10 seconds duration, of above mentioned four conditions were recorded in each patient. Evaluation parameters were determined during four test conditions as below:
The test was terminated when the participant (a) opens his or her eyes in an eyes closed condition (b) raises arms from sides (c) loses balance and requires manual assistance to prevent a fall.
Mean postural sway velocity was calculated (degree/second) by the software taking average of three test trials of each condition. Mean postural sway velocity value of Condition IV in which patient relies on his/her vestibular function for maintaining balance was noted for analysis in our study. Preoperative mean postural sway velocity value was compared with the post operative values at one month, 3 months and 6 months interval in both groups of patients.
A descriptive statistical analysis was done, calculating the mean and the standard deviation. For Intra group analysis, we have used paired t-test to find the difference between preoperative and post-operative values of mean postural sway velocity. For Inter group analysis, we have used unpaired t-test to compare between CWU and CWD mastoidectomies. The significance level was set at 5%, meaning that p value <0.005 was accepted as significant. Statistical analysis was done using SPSS (Statistical package for social sciences) Version 20.0.
In order to ascertain the 6 month post-op change in mean postural sway velocity relative to pre-op values for each surgery type, we also utilized Ordinary Least Squares (OLS) Regression analysis to minimize the sum of squared differences between observed and predicted values of the dependent variable (mean postural sway velocity). It has the added advantage of allowing for incorporation of other covariates such as age and gender, thus permitting multivariate ‘adjusted’ analysis. OLS regression generates a coefficient for the independent variable of interest (time), which represents the magnitude of difference (between pre-op versus 6 months post-op) associated with our dependent variable (mean postural sway velocity). Statistical analysis was performed using STATA statistical software package.
In order to compare the relative difference in pre-operative and 6 months post-op mean postural sway velocities for CWU and CWD surgeries, we used a ‘difference-indifference’ regression analysis strategy wherein we compared the difference in mean postural sway velocity values of preoperative recordings (time=t0 ) and 6 months post-operative recordings (time=t6 ) for CWU relative to CWD surgery. This strategy essentially obtains the difference between t0 and t6 for each surgery type and the subsequent values (difference of first differences) between CWU and CWD surgeries. It is specified through an interaction term of time (t0 , t6 ) with surgery type (CWU, CWD). The coefficient of this interaction term (6 months post op* CWD surgery in table 7) provides the mean difference-in-difference estimate of interest. Statistical analysis was performed using STATA statistical software package.
Following are the observations and results of the study:
Out of 50 patients of squamous COM, 25 underwent CWU & 25 underwent CWD mastoidectomy. Mean age of patients who underwent CWU mastoidectomy was 38.6 with standard deviation of 10.160 while mean age of patients who underwent CWD mastoidectomy was 37.7 with standard deviation of 9.800. There was no significant difference in the mean age of patients undergoing CWU & CWD mastoidectomy as p value was 0.821 (unpaired t test) as shown in Table 1.
| Group | Number of patients | Age (years) | p-value | |
| SD | ||||
| CWU | 25 | 38.6 | 10.160 | 0.821 |
| CWD | 25 | 37.7 | 9.800 | |
Table 1: Mean age (years) in squamous COM patients who underwent CWU & CWD mastoidectomy.
Out of 50 patients of squamous COM, mean pre-operative postural sway velocity of 25 patients who underwent CWU mastoidectomy was 2.076 deg/sec with standard deviation of 0.163 while mean pre-operative postural sway velocity of patients who underwent CWD mastoidectomy was 2.188 deg/ sec with standard deviation of 0.103. There was significant difference pre-operatively in mean postural sway velocity of patients undergoing CWU&CWD mastoidectomy as the p value was 0.005 (unpaired t test) as shown in Table 2.
| Group | Number of patients | Mean postural sway velocity (deg/sec) | p-value | |
| Mean | SD | |||
| CWU | 25 | 2.076 | 0.163 | 0.005 |
| CWD | 25 | 2.188 | 0.103 | |
Table 2: Comparison of mean postural sway velocity in squamous COM patients pre-operatively who underwent CWU & CWD mastoidectomy
In patients who underwent CWU mastoidectomy, the mean postural sway velocity 1 month post-operatively was 2.544 deg/ sec with standard deviation of 0.189; the difference between pre-operative and post-operative values was significant, as p value was <0.001 (unpaired t test). Mean postural sway velocity 3 month post-operatively was 2.212 deg/sec with standard deviation of 0.136; the difference between pre-operative and post-operative values was significant, as p value was 0.002 (unpaired t test). Mean postural sway velocity 6 month postoperatively was 2.104 deg/sec with standard deviation of 0.137; the difference between pre-operative and post-operative values was not significant, as p value was 0.514 (unpaired t test) as shown in Table 3.
| Parameter | Squamous COM patients undergoing CWD surgery (n=25) | P value | |||
| Mean postural sway velocity (deg/sec) | Pre-op | Post-op 1 month | |||
| Mean | SD | Mean | SD | <0.001 | |
| 2.188 | 0.103 | 2.676 | 0.158 | ||
| Post-op 3 month | |||||
| Mean | SD | <0.001 | |||
| 2.380 | 0.106 | ||||
| Post-op 6 month | |||||
| Mean | SD | 0.110 | |||
| 2.236 | 0.105 | ||||
Table 3: Comparison of mean postural sway velocity in squamous COM patients undergoing CWU mastoidectomy surgery pre-operatively and after 1 month, 3 months and 6 months
In patients who underwent CWD mastoidectomy, the mean postural sway velocity 1 month post-operatively was 2.676 deg/ sec with standard deviation of 0.158; the difference between pre-operative and post-operative values was significant, as p value was <0.001 (unpaired t test). Mean postural sway velocity 3 month post-operatively was 2.380 deg/sec with standard deviation of 0.106; the difference between pre-operative and post-operative values was significant, as p value was <0.001 (unpaired t test). Mean postural sway velocity 6 month postoperatively was 2.236 deg/sec with standard deviation of 0.105; the difference between pre-operative and post-operative values was not significant, as p value was 0.110 (unpaired t test) as shown in Table 4.
| Parameter | Squamous COM patients undergoing CWD surgery (n=25) | P value | |||
| Mean postural sway velocity (deg/sec) | Pre-op | Post-op 1 month | |||
| Mean | SD | Mean | SD | <0.001 | |
| 2.188 | 0.103 | 2.676 | 0.158 | ||
| Post-op 3 month | |||||
| Mean | SD | <0.001 | |||
| 2.380 | 0.106 | ||||
| Post-op 6 month | |||||
| Mean | SD | 0.110 | |||
| 2.236 | 0.105 | ||||
Table 4: Comparison of mean postural sway velocity in squamous COM patients undergoing CWD mastoidectomy surgery pre-operatively and after 1 month, 3 months and 6 months
On sub group analysis it was found that mean postural sway velocity in squamous COM patients undergoing CWU mastoidectomy surgeries, pre-operatively and after 1 month, 3 months and 6 months were 2.544 deg/sec with standard deviation of 0.189, 2.212 deg/sec with standard deviation of 0.136 and 2.104 deg/sec with standard deviation of 0.137 respectively whereas in patients undergoing CWD mastoidectomy surgeries, pre-operatively and after 1 month, 3 months and 6 months were 2.676 deg/sec with standard deviation of 0.158, 2.380 deg/sec with standard deviation of 0.106 and 2.236 deg/sec with standard deviation of 0.105 respectively. The values were higher in the patients undergoing CWD mastoidectomy in comparison with patients undergoing CWU mastoidectomy and the difference was significant, p value being <0.005 (Table 5).
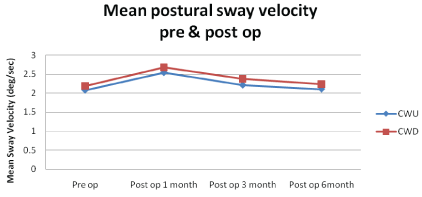
Table 5: Comparison of mean postural sway velocity in COM patients undergoing CWU and CWD mastoidectomies, pre-operatively and after 1 month, 3 months and 6 months
Bivariate OLS regression results for CWU surgery indicate that compared to pre-operative values, the mean postural sway velocity at 6 months post-op follow up increased by 0.028 degree/sec, but this increase is not statistically significant (p value being 0.523). These results remain unchanged upon adjusting for gender and age in a multivariate regression framework.
With respect to CWD surgery, compared to pre-operative values, the mean postural sway velocity at 6 months post-op follow up increased by 0.048 degrees/sec, but this increase is not statistically significant (p value being 0.117). Similar to the observation from CWU surgery, these results remain unchanged upon adjusting for gender and age in a multivariate regression framework (Table 6).
| Canal Wall- Up surgery | Canal Wall- Down surgery | |||||
| Covariate | Coefficient | Standard error | p-value | Coefficient | Standard error | p-value |
| 6 months post op (compared to pre-op) | 0.028 | 0.044 | 0.523 | 0.048 | 0.030 | 0.117 |
Table 6: Bivariate regression results for mean postural sway velocity for CWU and CWD surgeries
As per results in Table 7, we observed that the mean postural sway velocity (on average) for cases of CWD surgery is significantly higher than for those who underwent CWU surgery. More importantly, we see that while CWD surgery is associated with a gain in mean postural sway velocity by 0.020 degrees/sec compared to CWU surgery, this difference is not statistically significant (p value being 0.706). Results remain unchanged upon adjusting for age and gender.
| Covariates | Comparison group | Coefficient | Standard Error | P value |
| 6 months post op | Pre-op | 0.028 | 0.044 | 0.521 |
| Canal Wall Down surgery | Canal Wall Up surgery | 0.112 | 0.040 | 0.005 |
| 6 months post op* Canal Wall- Down surgery | 0.020 | 0.053 | 0.706 |
Table 7: ‘Difference in difference’ estimates comparing time t0 and t6 for CWU and CWD surgeries
This prospective comparative analytical cohort study was conducted to determine the pre and post-operative status of balance in patients of squamous COM undergoing CWU and CWD mastoidectomy surgeries using computerized static posturography.
The objective of this study was to evaluate the vestibular function by objectively assessing the status of balance by posturography in patients undergoing CWU and CWD mastoidectomy pre-operatively and post-operatively. We also aimed to study the integrity of the vestibular system and its role in maintaining balance in these patients post-operatively
To balance with the feet in-place, the position of the body’s centre of gravity (COG) must be maintained vertically over the base of support. The limit of stability (LOS) is approximately 12.5 degree from backward most to forward most point and laterally 16 degree from left to the right most point [4]. A person attempting to maintain balance spontaneously sways back and forth and from side to side. Limits of sway is always well within LOS.
Sensing the position of COG relative to the gravity and the base of support requires a combination of visual, somatosensory and vestibular inputs. Vision measures the orientation of eyes and head in relation to surrounding objects. The somatosensory input provides information on the orientation of body parts relative to one another and to the support surface. The vestibular system measures gravitational, linear and angular acceleration of head in relation to inertial space. Vestibular input is critical for balance when visual and somato-sensory inputs are misleading or unavailable [5,6].
Computerized static posturography is a quantitative method of assessing upright balance function under a variety of tasks that effectively simulates conditions encountered in daily life. Static posturography is carried out by placing the patient in a standing posture on a fixed instrumented platform (force plate) connected to sensitive detectors (force and movement transducers), which are able to detect the tiny oscillations of the body. As the patient makes small movements, they transmit in real time to a computer. The forces measured by the force plate are recorded and transformed by special software in equilibrium parameters and scores which can then be compared with normal ranges [7].
Vestibular dysfunction has been enumerated in terms of dysfunction in the vestibulo-ocular reflex (VOR) system and the vestibulo-spinal reflex system [8]. Tests of VOR system like caloric test, vertical axis rotation of the entire body, and electronystagmographic evaluations of spontaneous and positional nystagmus provide information about lateral semicircular canal lesion and its symmetry. These tests do not characterize the vestibular dysfunction in terms of patient’s functional status because such subjects are examined in “passive” positions in which balance is not required. VOR tests, thus, have limited value for identifying balance deficits related to vestibular dysfunction.
Early in 1979, Paparella et al reported air caloric test for otitis media. They described different caloric responses according to the conditions of otitis media [9]. In 2008, Gianoli and Soileau reported the correlation between caloric test and rotational chair test in patients with COM. They concluded that the incidence of abnormalities on caloric test was high and correlated well with rotational chair test abnormalities (80% accuracy). They suggested the validation of air caloric test for evaluating vestibular function in patient with COM [10].
In a study in year 2012, 59.5% patients with unilateral simple COM were recorded to have complaint of dizziness/vertigo. There was a higher incidence rate of abnormal results in either air caloric test or Vestibular Evoked Myogenic Potential (VEMP) test (81.1%) for the same patient group. This study demonstrated that most patients with COM suffered from vestibular abnormalities through vestibular function tests; however, it seemed that no significant correlation existed between the results of vestibular function tests and symptoms of dizziness/vertigo. It was suspected that mechanism of central compensation occurred due to chronic process of otitis media. In consequence, patients with COM would not suffer from an episode of dizziness/vertigo despite the abnormal vestibular function test results. There was not a significant relationship between the results of caloric test and VEMP test. Since caloric test and VEMP test were applied to evaluate different locations of the vestibular system, the correlation might not be high [11].
Various studies done in the past have shown high incidence of vestibular dysfunction in COM post-operatively. Nystagmic responses on CWD mastoidectomy side were greater when compared to responses from the healthy ear. Labyrinthine preponderance was observed on the CWD mastoidectomy side. Paradoxical stimulation in hot caloric tests was a frequent finding. Hypofunctional responses were not found in any of the stimulation events, mainly on the CWD mastoidectomy side [12].
In a prospective study, static and dynamic postural control was measured on a Balance Master computerized force plate in 24 severe hearing impaired patients before and after cochlear implantation (CI) surgery, and 19 healthy adults. The test battery consisted of MCTSIB, rhythmic weight shift, walk across and Tandem walk test. Postural control was significantly worse in CI candidates that in healthy adults. In contrast, caloric testing of the vestibular organ was normal in majority of CI candidates and remained normal after CI surgery. Static and dynamic standing balance parameters remained unchanged after CI surgery for vast majority of parameters although postural control was impaired [13].
We used static posturography in our study where patients with squamous COM were detected to have vestibular dysfunction on the basis of their mean postural sway velocity scores done before surgery. Finding was compared with postoperative mean postural sway velocity scores in both types of surgeries, namely CWU and CWD mastoidectomies. Literature search on our part failed to show any such study published till date.
One group of 25 patients, who underwent CWU mastoidectomy, were found to have increased mean postural sway velocity after 1, 3 and 6 month post-operatively which signifies imbalance due to vestibular dysfunction. The mean postural sway velocity gradually decreased post-operatively after 3 month. It decreased further after six month though it was not equal to pre-operative value and the difference was found to be insignificant.
Another group of 25 patients, who underwent CWD mastoidectomy, were found to have increased mean postural sway velocity after 1, 3 and 6 month post-operatively which signifies imbalance due to vestibular dysfunction. The mean postural sway velocity gradually decreased post-operatively after 3 month. It decreased further after six month though it was not equal to pre-operative value and the difference was found to be insignificant.
Thus our study has demonstrated significant occult vestibular dysfunction in COM patients post-operatively both in CWU and CWD patients as compared to pre-operatively with possible compensation occurring by six months. It also showed that the mean postural sway velocity for cases of CWD surgery is significantly higher than for those who underwent CWU surgery. Drilling close to the semicircular canal and clearing disease from posterior hypotymanum during mastoidectomies may be significant factors causing imbalance pos-operatively. The mastoid cavity, left open after meatoplasty in CWD mastoidectomy, communicates directly to the external auditory canal. This, probably, gives air caloric effect causing imbalance and relatively worse postural sway than in CWU mastoidectomy.
Posturography recently has been accepted as an important part of functional investigation, aimed at identifying and assessing vestibular dysfunctions. It is an objective technique used to measure postural stability on static or dynamic measuring platforms. It is not burdened by subjective interpretation. The results can be documented both graphically and numerically. As the sample size of this study is small and has used only static posturography, it is important that a larger study be conducted using both static and dynamic posturography
This study did not involve any funding from any organization. There was no conflict of interest involved. The authors sincerely acknowledge the contribution of Ms Parvati Singh B. Tech, MBA, MPA, (PhD student in the Dept of Public Health, University of California, and Irvine, USA) for doing the statistical analysis for this study.
Both the authors have contributed intellectually in this study. First author has selected the cases, carried out posturography tests and followed up all the 50 cases. Second author, who is also the corresponding author, has contributed in terms of study concept, drafting and revision of manuscript as well as guided the first author in his dissertation on this subject.
Download Provisional PDF Here
Article Type: RESEARCH ARTICLE
Citation: Gupta A, Prasad BK (2018) Assessment of Balance by Posturography - A Comparative Study in Pre and Post Operative Patients Undergoing Canal Wall Up and Canal Wall Down Mastoidectomy. J Otorhinolaryngol Disord Treat 1(1): dx.doi.org/10.16966/jodt.103
Copyright: © 2018 Gupta A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access