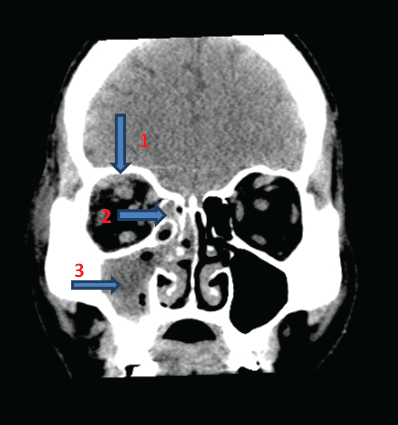
Figure 1: CT ORBITS 1MM CUTS (CORONAL VIEW) SHOWING(1) Bulky right superior rectus; (2) Right ethmoidal sinusitis; (3) right maxillary sinusitis

Namitha Rachel Mathew1* Sudha Girish Menon1 Deepak Nayak2
1Department of Ophthalmology, Kasturba Medical College, Manipal, India*Corresponding author: Namitha Rachel Mathew, Department of Ophthalmology, Kasturba Medical College, Manipal, India, E-mail: namitha132@gmail.com
Orbital cellulitis is an infection of the soft tissues of the orbit posterior to the orbital septum. Delay in diagnosis and management of orbital cellulitis may result in visual loss. Botryomycosis is an extremely rare cause of orbital cellulitis. It is a chronic granulomatous reaction to deep seated bacterial infection which is usually seen in immune-compromised individuals. We report a case of recurrent orbital cellulitis due to botryomycosis in a healthy adult.
Orbital cellulitis is an infection of the soft tissues of the orbit posterior to the orbital septum. It has various causes and may lead to serious complications. Around 11% of cases of orbital cellulitis may result in visual loss. Prompt diagnosis and management is essential to avoid the associated complications [1].
We report a rare case of recurrent orbital cellulitis due to botryomycosis in a healthy adult. Botryomycosis, also known as bacterial pseudomycosis, is a chronic, suppurative, granulomatous, bacterial infection, wherein the organisms form granules (Bollinger’s granules), composed of clumps of bacteria. It is a rare condition that usually involves the skin and sometimes the viscera-liver, lung, kidney, prostate, caecum, brain and lymph tissue [2-4]. Orbital botryomycosis is extremely rare.
A 48-year-old male, was seen in the ophthalmology outpatient clinic with complaints of severe pain, eyelid swelling and diminution of vision in the right eye since 5 days. These symptoms were sudden in onset, and the pain radiated to the right cheek and forehead. He was unable to open the right eye since 2 days.
He gave history of intermittent toothache, involving the right upper jaw since 1 year. There was no discharge from the eye, no history of fever, trauma/sinusitis. He was not a known diabetic/hypertensive.
At presentation, right eye proptosis was present; vision was counting finger at 2 meter, which progressed to no perception of light, within 24 hours. Extra ocular movements were grossly restricted in all gazes. Periorbital edema, diffuse conjunctival chemosis and relative afferent pupillary defect were present. Fundus examination showed optic disc edema. Left eye examination was normal. Systemic examination was unremarkable.
Dental examination revealed 2 infected premolars in the right upper jaw. ENT examination revealed right ethmoidal and maxillary sinusitis.
Blood picture revealed a normal ESR of 4 mm/h and a white cell count of 9,600 cells/mm3 (normal ESR-0-22 mm/h for men, normal white cell count- 3,500-10,500 cells/mm3). Renal function tests, liver function tests and coagulation profile were normal. His blood sugars were on the higher side with a fasting sugar of 168 mg/dl and post prandial of 204 mg/dl. HIV, HBsAg and HCV were negative. Blood culture was also negative. Culture of discharge from the maxillary sinus grewnon-fermenter gram negative bacilli sensitive to ceftriaxone and ceftazidime. Repeat culture was negative. CT brain, orbits and paranasal sinuses showed right eye proptosis, with bulky extraocular muscles; and right maxillary and ethmoidal sinusitis (Figures 1 and 2).

Figure 1: CT ORBITS 1MM CUTS (CORONAL VIEW) SHOWING(1) Bulky right superior rectus; (2) Right ethmoidal sinusitis; (3) right maxillary sinusitis
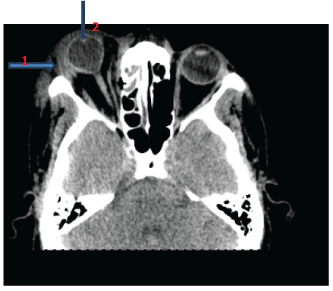
Figure 2: CT ORBITS 1 MM CUTS (AXIAL VIEW) SHOWING- (1) Proptosis of right globe with mild deformation of its shape; (2) Preseptal swelling
He was immediately started on Intravenous Ceftazidime, vancomycin, metronidazole and oral prednisolone, along with topical moxifloxacin and timolol eye drops. He underwent extraction of the 2 infected premolars. On the third day of admission, he underwent right sided functional endoscopic sinus surgery (FESS) with orbital decompression. Histopathology of maxillary sinus showed features of botryomycosis (Figures 3A and 3B).
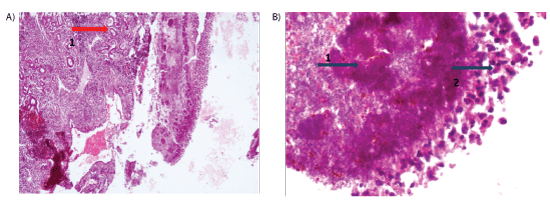
Figure 3A: HPE WITH H& E STAIN 100 X MAGNIFICATION SHOWING SINUS EPITHELIUM WITH (1) Surface amphophilic bacterial colonies, suggestive of Botryomycosis
3B: H&E STAIN WITH 400 X MAGNIFICATION (1) Gram positive bacterial colony surrounded by (2) intensely eosinophilic infiltrate: the Splendore-Hoeppli phenomenon
Following surgery, the pain and swelling decreased and he was discharged on oral and topical antibiotics and oral steroids with follow up appointment after 1 week. After discharge, the patient reported 2 weeks later, with the same complaints of severe pain, swelling and inability to open the right eye since 2 days. Right eye vision no perception of light, with proptosis, gross restriction of extraocular movements in all directions, conjunctival chemosis and relative afferent pupillary defect. Left eye was normal.
He was admitted under the department of neurosurgery and underwent right orbital wall decompression and frontal abscess drainage. The pus sent for culture showed no growth after 60 hours of incubation. Post surgery, the swelling and pain had markedly reduced, and he was discharged on antibiotics after one week. On follow-up after 1 month, all features of orbital cellulitis had resolved. However, right eye vision was still no light perception.
Bollinger first reported botryomycosis (in Greek, botrys - a bunch of grapes, mycosis - fungal origin) in 1870 in the lung of a horse [5].It was originally thought to be a fungal infection. He reported multiple fibrous nodules that contain areas of pus with yellow-white granules resembling those seen in actinomycosis, but there was no evidence of branching filaments characteristic of actinomycosis [4-6]. Later, the bacterial etiology was discovered. Many species of bacteria have been implicated, most commonly Staphylococcus aureus, followed by Pseudomonas aeruginosa, and rarely Streptococcus species and Escherichia coli [7].
Diagnosis of botryomycosis is helped by gram staining, culture and biopsy. On microscopic examination of a haematoxylin-eosin stained specimen, radiating eosinophilic spokes or rings surrounding a central focus of necrosis due to the causative bacteria are seen, which is referred to as the Splendore-Hoeppli phenomenon. These eosinophilic deposits are thought to represent precipitates from antigen-antibody reactions. Epithelioid macrophages and giant cells are also seen. However, this is also seen in actinomycosis, mycetoma and a few parasitic infections making the diagnosis difficult [8].
The radiate structures of Splendore-Hoeppli reaction resemble the sulphur granules in actinomycosis. The absence of central branching filaments in Splendore-Hoeppli phenomenon, distinguishes it from actinomycotic sulfur granules. Also, presence of bacteria on gram staining helps in the diagnosis of botryomycosis. It is very important to reach a correct diagnosis, for the subsequent management [9-11].
Botryomycosis is usually associated with immunocompromised individuals such as those with Acquired Immuno Deficiency Syndrome, severe malnutrition, chronic granulomatous disease, diabetes mellitus, recurrent mucocutaneous candidiasis , and patients on chronic corticosteroid therapy [7,12-14].
Extensive surgical debridement with systemic antibiotics is the treatment of choice especially when there is significant intracranial involvement. High morbidity and mortality are reported in such cases [7]. Our patient had no known risk factors and responded well to surgery and long term antibiotics.
Botryomycosis is a chronic granulomatous reaction to deep seated bacterial infection usually seen in immunocompromised individuals. It may be mistaken for a fungal infection. Gram stain and biopsy helps in the diagnosis. Orbital involvement is very rare. Prompt diagnosis and management are necessary to avoid morbidity and mortality.
Download Provisional PDF Here
Article Type: CASE REPORT
Citation: Mathew NR, Menon SG, Nayak D (2017) A Case of Recurrent Orbital Cellulitis due to Botryomycosis. J Otorhinolaryngol Disord Treat 1(1): dx.doi.org/10.16966/jodt.102
Copyright: © 2017 Mathew NR, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access