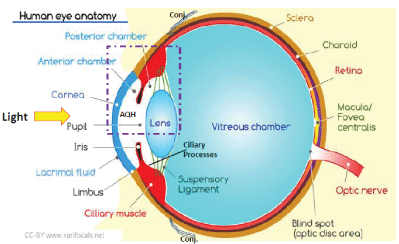
Figure 1A: Anatomical features of the human eye.


Najam A Sharif1-5*
1Vice President, Santen Inc, California, USA*Corresponding author: Naj Sharif, BSc (Jnt Hons), PhD, DSc, FARVO, FBPhS, FAOPT, Vice President, Global Alliances &External Research, Global Ophthalmology R&D, Santen Incorporated USA, 6401 Hollis St, Ste # 125 Emeryville, CA 94608, E-mail: najam.sharif@santen.com
This review article describes research conducted in the discovery and development of drugs to treat seasonal allergic conjunctivitis (SAC), ocular hypertension (OHT) and primary open-angle glauocma (POAG) on the path towards earning the highest degree a university can award to a student/ researcher within the United Kingdom (UK) and Commonwealth countries, the Doctor of Science (DSc). Whilsts a personal journey and treatise of the preclinical research performed to seek, discover, in-license, characterize and develop emedastine [Emadine®] and olopatadine [Patanol®/ Pataday®] for the mitigation of signs and symptoms associated with ocular allergies (SAC), and travoprost [Travatan®] for OHT and POAG, it is hoped to inspire other scientists across the many biomedical disciplines to aspire to accomplish similar scholarly and industrial goals. Additionally, I wish to bring further awareness of the aforementioned ocular diseases that affect millions of people across the world, and challenge researchers to address the unmet medical needs of the many patients who deal with such adversity through their lives and who have to live with a quality of life lesser than worthy of their compatriots. Let us keep forging the path forward to find new treatment options for the patients who suffer from SAC, POAG and related potentially blinding ophthalmic disorders. Since these and other common vision problems often have no early warning signs, regular screening via eye examinations is highly recommended.
Allergic Conjunctivitis, Glaucoma, Patanol, Pataday, travatan, Travoprost
As many scientific researchers can attest, career paths are arduous, lengthy and fraught with failure and disappointment, especially when the research experiments do not yield the results we hope for. Much hard work, patience and perseverance is needed; “never give up, for that is just the place and time that the tide will turn” (Harriet Beecher Stowe); “you just can’t beat the person who never gives up” (Babe Ruth); “in order to succeed; we must first believe that we can” (Nikos Kazantzakis). Indeed, and however, some of us have been extremely fortunate to have been in the right place at the right time, and been blessed to receive timely and very valuable education, training and supportive mentorship to help us succeed. In a humble effort to inspire other students and life sciences researchers and scientists, I offer the following discourse of my own small steps along a protracted career that spanned over three decades. In order to be focused, I will present this personal perspective of the final top “award” afforded to me by the University of Southampton (UK), my esteemed alma mater which I attended in the mid-70s till early 80s, and to which I submitted a thesis for consideration towards the Doctor of Science (DSc) degree in 2018. Upon examination by internal and external reviewers, the University concluded to award me this degree in 2019, for which I am extremely grateful.
I was fortunate to have received the excellent education and training provided by the University of Southampton during my undergraduate and postgraduate time spanning 1978-1982. Professor Robert Walker and Professor Peter Roberts were the key professors who helped shape my interest and career in the biomedical sciences resulting in my pursuit of the BSc (Joint Honors in Physiology & Biochemistry) and PhD (Neuropharmacology) programs, respectively. I am especially indebted to Robert and Peter, along with the many other professors who taught me at the University of Southampton, without whose kind and generous help, support and encouragement I probably would not have achieved much in life. I credit all my accomplishments to the faculty of the University of Southampton for instilling in me a curiosity and drive for biomedical research to ultimately help discover, develop and market medicines to treat human and animal eye diseases, the subject matter of the proposed DSc degree award I aimed for during 2018.
Following awards of my BSc and PhD from the University of Southampton (England, UK), I embarked on two postdoctoral training programs to further my biochemical pharmacology research (at University of Maryland, USA and at Nottingham University, UK). These took me out of my comfort zone, and ultimately led me to apply my training and expertise to perform discovery research to help find drugs to treat neuropsychiatric diseases and chronic pain as a Staff Researcher at Parke-Davis Research Unit (Cambridge, UK), Syntex Research (Palo Alto, CA, USA), and Synaptic Pharmaceutical Corp (Paramus, NJ, USA). In early 1990s, I entered the field of ophthalmology research when I joined Alcon Laboratories, Inc. (TX, USA), which later became Alcon Research, Ltd. (TX, USA) and then a subsidiary of Novartis Pharmaceuticals. I found myself building and establishing multiple research laboratories, recruiting and leading Teams of scientists involved in discovering medicines for treating various eye diseases. My passion for fundamental and applied biomedical research led me to tackle the issues of first understanding ocular physiology, pathology and pharmacology, and then conducting and supervising research to address key eye diseases such as seasonal allergic conjunctivitis (SAC), ocular hypertension (OHT) associated with primary open-angle glaucoma (POAG), dry eye, ocular inflammation and pain, and age-related macular degeneration. However, I decided to focus on SAC and OHT/POAG as my major areas of research, and thus from 1992 to 2018, I passionately, vigorously and relentlessly pursued drug discovery research/development and regulatory science in these areas, along with many talented scientists from various departments in a Team setting, at two major ophthalmology pharmaceutical companies (Alcon-Novartis and Santen Inc USA/ Santen Pharmaceutical Co., Ltd.). Such collaborative efforts helped better define the pathogenesis of these eye diseases, identified some key therapeutic targets, pharmacologically characterized the ocular receptors and enzymes involved and found novel and unique drugs that allowed us to treat the symptoms associated with these diseases and thus bring relief to the millions of patients afflicted with SAC and POAG world-wide. It has been a long but worthwhile journey that my Team members and I have endeavored to capture and relay to other researchers around the world in the form of public presentations at global conferences, peer-reviewed publications and patents, and capturing some of this information in appropriate book chapters and edited works in book format. The aim has been always to learn from and teach each other and share our struggles and positive experiences to foster and enhance global awareness to eye diseases and help find suitable drugs/treatment modalities to treat them to provide relief for the patients. To this end, I have strived and successfully debated with and convinced senior management at multiple pharmaceutical companies I’ve worked at during my >30-year research career, to permit us to publish and share our research findings with the scientific community once we filed suitable patent applications on proprietary materials. Again, I’ve been blessed with success in these matters and my proposed DSc thesis herein will highlight the breadth and depth of pursuit of discovery research in my chosen fields of study, research and development of drugs for the treatment for SAC and OHT/ POAG. I will now provide narratives that demonstrate and capture the essence of the key accomplishments in discovery research in identifying treatment options for SAC and POAG via key publications and patents. This has been a Team effort and I wish to acknowledge the hard work and diligent and thorough research of my co-workers and co-authors of the many papers and patents that resulted from our collaborative research work at the many institutions mentioned above. I shall name the key participants on the Project Teams/Collaborators at the appropriate time in this discourse.
As a rough guide to the scale of the major ophthalmic problems around the globe, the following statistics and epidemiologic data are sobering and deserve to be highlighted. It is estimated by sources such as the World Health Organization (WHO), American Academy of Ophthalmology (AAO) and National Eye Institute (NEI, USA) that by 2020 there will be 2.6 billion people with myopia, >2 billion with presbyopia, 196 million with age-related macular degeneration (AMD), >150 million with diabetic retinopathy, 76-80 million with glaucoma, and many millions who suffer from SAC around the world on an annual basis. Eye disorders causing visual impairment and causes of legal blindness are diverse and affect different races to widely varied degrees around the world (Table 1). Therefore, a concerted effort is required from global scientific and Healthcare communities to thwart and to solve the problems associated with such ocular disabilities.
| Causes of Visual Impairment | Causes of Legal Blindness |
| Non-Hispanic Whites | Non-Hispanic Whites |
| Cataract (42.2%) | Age-related macular degeneration (46.6%) |
| Age-related macular degeneration (28.1%) | Others (27.6%) |
| Others (22.7%) | Cataract (10.3%) |
| Diabetic retinopathy (47%) | Diabetic retinopathy (6.9%) |
| Glaucoma (2.3%) | Glaucoma (5.2%) |
| African Americans | African Americans |
| Cataract (41.7%) | Others (43.8%) |
| Others (27.0%) | Cataract (25%) |
| Diabetic retinopathy (12.2%) | Glaucoma (18.8%) |
| Glaucoma (11.3%) | Diabetic retinopathy (8.3%) |
| Age-related macular degeneration (7.8%) | Age-related macular degeneration (4.2%) |
| Hispanics | Hispanics |
| Cataract (48%) | Others (39.5%) |
| Others (16.2%) | Age-related macular degeneration (23.7%) |
| Diabetic retinopathy (15.0%) | Diabetic retinopathy (18.4%) |
| Age-related macular degeneration (14.5%) | Glaucoma (10.5%) |
| Glaucoma (6.4%) | Cataract (7.9%) |
Table 1: Causes of visual impairment and legal blindness amongst different races (American Assoc. Ophthalmology; National Eye Institute (USA)).
The eye is a window for the brain to perceive the environment around us, and is an indispensable organ for the majority of the animals and humans. Eyesight is critical for survival and people with visual impairment are frightened of losing their sight. Due to their location on the face, the eyes are prone to injury and are constantly being bombarded with airborne allergens, pathogens, light, other forms of radiation and pollution (Figures 1A and 1B). Preserving visual function is therefore a major challenge and we must understand the anatomy, physiology/pharmacology and pathology of the eyebrain axes in order to search for suitable treatment options. Figures 1A and 1B illustrates the basic anatomy of the eye, and the fundamental elements involved in keeping the shape of the globe relatively constant (aqueous [AQH] and Vitreous Humor [VH]; scleral tissue), helping focus the light to the retina (cornea and lens), and maintaining/ nourishing the structures therein (e.g. Anterior Chamber [ANC] tissues such as Ciliary Processes [CP], Ciliary Muscle [CM], Trabecular Meshwork [TM]) and functions of the various compartments (e.g. production of AQH and its drainage from the ANC via two outflow pathways, via the TM and via the cilary muscle and across the sclera [uveoscleral (UVS) pathway]) (Figure 1B). Clearly, with such specialized ocular tissues and cells, dysfunctions within each leads to well defined ocular diseases. The latter range from ocular surface disorders such as dry eye, allergic conjunctivitis, corneal perforation and ocular pain. Within the anterior chamber, malfunctions in the corneal endothelial cells leads to corneal dystrophies, while clogging of the normal AQH drainage pathway (TM) raises intraocular pressure (IOP) to cause ocular hypertension (OHT) that is frequently linked to glaucoma, a blinding disease if left untreated [1-3]. Lens epithelial cell dysfunction causes cataracts, and if the iris repeatedly rubs against the lens, enough cellular debris accumulates in the TM that exfoliation/ pigmentary glaucoma can result. Even though VH acts as a cushion to the surrounding tissues and vascular elements in the posterior chamber of the eye, several retinal diseases prevail (e.g. dry and wet age-related macular degeneration (AMD), retinitis pigmentosa, diabetic retinopathy, glaucomatous optic neuropathy [GON], etc) that require specific treatment modalities. Some the key elements will be discussed below

Figure 1A: Anatomical features of the human eye.
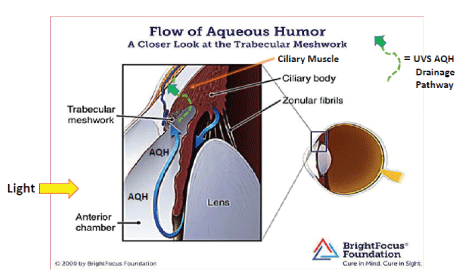
Figure 1B: illustrates the two different mechansims/means utilized by the eye to drain the AQH from the anterior chamber, the conventional trabecular meshwork (TM), and the uveoscleral (UVS) outflow pathways. (Figures gratefully modified from www.varifocals.net and BrightFocus Foundation, respectively).
The most exposed parts of the eye, cornea and conjunctiva, are extremely well innervated and therefore are very sensitive to touch and to irritant substances that land on the ocular surface. Even though regular blinking can mitigate the effects of such insults, the triggering of the cascades of inflammatory reactions and events ensuing from such contact can be rapid and quite detrimental. According to the WHO, conjunctivitis is defined as inflammation of the conjunctiva (the clear membrane lining the inside of the eyelids and covers the white part of the eye) most commonly caused by allergy or infection. Ocular allergies are quite common problems, and they may occur suddenly (acute form), may occur when seasons change (seasonal allergic conjunctivitis, SAC; [4-6], or may occur anytime irrespective of the seasonal change (perennial conjunctivitis). In all instances the allergic reaction mainly occurs in the conjunctiva in response to airborne allergens such as pollen, mold, pet dander, and other pollutant substances. SAC afflicts millions of patients of all ages every few months and causes debilitating and extremely bothersome excessive tearing, intense itching, grittiness, burning, photophobia, redness and swelling of the eyelids, and some pain [4-9]. These symptoms are caused by release of histamine, prostaglandins (mainly PGD2), cytokines (e.g. interleukin-6 [IL-6; IL-8]), chemokines, kinins, platelet activating factor (PAF) and various enzymes (e.g. tryptase; chymase) from resident mast cells in conjunctiva of the eyelids [10,11]. SAC leads to decreased work productivity, increased absenteeism from work and school, limitation of everyday activities, significantly reduced quality of life, including decreased sleep quality. These SAC symptoms combined with seasonal rhinitis cause further ill-health and detrimental psychological ill-effects leading to impaired social interaction on top of the physical morbidity. Overall, SAC and rhinitis due to their perennial/seasonal occurrence requires fast-acting, potent and efficacious treatment options with some durability so the patient does not have to keep dosing and may get even more agitated. Unfortunately, many of the existing drugs available for treatment of SAC at the time of initiation of our drug discovery program around 1993 provided minimal and short-lived symptomatic relief, requiring multiple daily doses that resulted in further corneal and conjunctival pain and discomfort, and ill-health of the corneal epithelial cells causing visual impairment that sometime required further ophthalmic treatments. Therefore, we considered it important to first better understand the ocular allergic disease phenomenon and then to initiate a drug discovery program to find suitable drug candidates to help mitigate the signs and symptoms associated with SAC.
Initial research indicated huge species and tissue heterogeneity of mast cells and their responses to antigens. The Team (Dr. John Yanni, Shouxi Xu, Steve Miller and I, along with several other research and management staff) therefore focused our attention to ocular tissues and isolated human conjunctival epithelial (HCE) and human conjunctival mast (HCM) cells. These cells exhibited profound proinflammatory responses by releasing histamine, interleukin-6 (IL-6) and IL-8, and the HCM cell isolation/characterization procedures (US Patent 5360720) and HCE cell isolation and methods of inhibiting release of these inflammatory mediators (US Patent 6174914) were patented. Concurrently, high-throughput screening (HTS) platforms were established to rapidly screen large numbers of drug candidates for their ability to inhibit histamine receptor sub-type binding and profiling at other receptors (Tables 2 and 3); [12-16]. Additional studies were conducted to study prevention of intracellular second messenger mobilization in HCE and human corneal epithelial [CEPI] cells (Brit J Pharmacol [17-20], and to investigate the abrogation of cytokine release from these cell-types (Figure 2); [19-24]. Additionally, models of ocular vascular permeability and allergic conjunctivitis were established and validated for characterizing key molecules of interest [13,16,25,26]. Such testing schemes allowed us to triage and select top candidates for further detailed characterization for on-target and in vivo off-target side-effects and to help determine their therapeutic indices via the standard dose-response in vitro and in vivo studies. It became evident that the key property needed in molecules to be deemed useful for treating SAC was “mast cell stabilizing activity”, and that histamine-1 receptor antagonist activity was also useful. As such we profiled numerous compounds in vitro and in vivo and first discovered Emedastine (eventually in-licensed from Kanebo Ltd. (Tokyo, Japan) [12,13,21,22,24,25]. This drug was an H1 -receptor selective antagonist that exhibited a high affinity and a profoundly high selectivity for the H1 -receptor (H1: Ki=1.2 nM, H2 : Ki =39,860 nM, and H3: Ki=14,498 nM; Table 2) [12,13], and which potently inhibited histamine-induced cytokine release from HCE cells (IC50=1.2 nM) [22], and potently and efficaciously inhibited guinea pig conjunctival vascular permeability [12,13,22-25]. This drug subsequently exhibited all the necessary characteristics to combat signs and symptoms of SAC in human patients and was approved by the health authority in EU and marketed as Emadine® for the treatment of SAC in EU countries, with a a relatively fact onset of action and duration of action of 8-hrs [27,28]. However, even though Emadine® was more selective, potent and efficacious than other anti-allergic compounds available at the time (e.g. cromolyn; nedocramil; pemirolast; naphazoline and pheniramine combination), and it displayed a fast onset of action [28], it lacked the mast cell stabilizing activity. Therefore, the next phase of our drug discovery focused on this element, and through diligent research our Team discovered a dual pharmacophore that possessed both ocular mast cell stabilizing activity plus H1 -antagonist activity… this was Olopatadine (eventually in-licensed from Kyowa Hakko Kogyo (Tokyo, Japan) [15]. Olopatadine also exhibited robust H1- receptor affinity and selectivity (Figure 3 and 4; Table 2 and 3), and it inhibited H1-receptor binding [15,16], IL-6 and IL-8 release from HCE cells (IC50s- 1.7-36 nM) [21,22], prevented histamine release from human conunctival mast cells (Figure 2) [11,23], attenuated allergic conjunctivitis in Guinea pigs (IC50=0.0067% w/v), and prevented histamine-induced conjunctival edema for up to 24 hrs after topical ocular (t.o.) dosing. Overall, many other anti-histaminic compounds did not match the relative affinities (Table 2) and H1- receptor-selectivities of emedastine and olopatadine (Table 3, Figure 3 and 4). Additionally, decreased chemotaxis and inhibition of eosinophil activation was also demonstrated for Olopatadine. These characteristics were also observed in clinical trials in terms of potency and efficacy of Olopatadine, especially inhibition of ocular itching and redness, and Patanol® (Olopatadine 0.1%; twice-daily t.o. dosing) [23,29,30] was subsequently approved by FDA to treat ocular itching due to SAC in December, 1996.
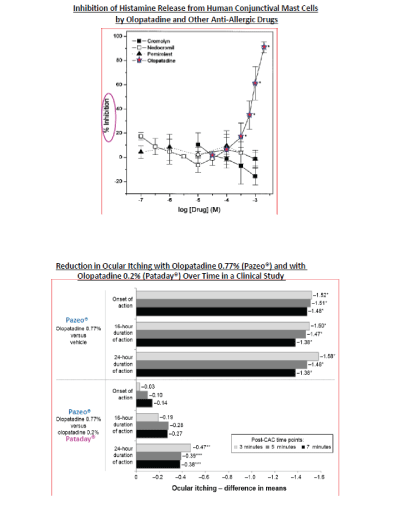
Figure 2: Comparative affinities of Olopatadine and other anti-allergic drugs for H1-receptors as shown by their relative abilities to displace [ 3H]-pyrilamine from the H1-receptor [12-17].
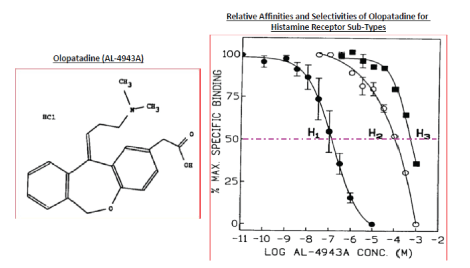
Figure 3: Olopatadine chemical structure and its relative affinities for H1 -H3 receptors. Note the very high relative selectivity of Olopatadine for displacing [3H]-pyrilamine from the H1 -receptor, [ 3H]-tiotidine from the H2 -receptor, and [3 H]-N-methyl histamine from the H3 -receptor [15,16].
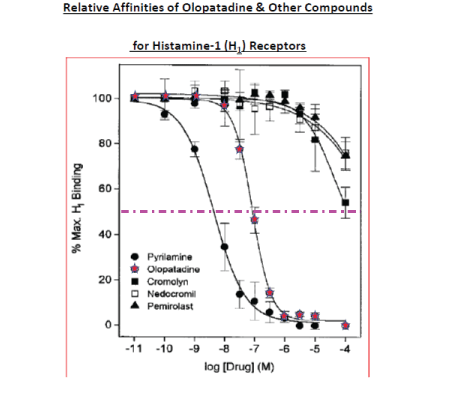
Figure 4: Ability of Olopatadine and other anti-allergic drugs to inhibit the release of histamine from human conjunctival mast cells is shown in Figure 4A. However, Figure 4B depicts the relative reduction in ocular itching due to 0.2% Olopatadine (Pataday®) and 0.7% Olopatadine (Pazeo®) [13].
| Compounds | Inhibition of Receptor Binding to Histamine Receptor Subtypes (Ki, nM) | ||
| H1 Receptors | H2 Receptors | H3 Receptors | |
| Pyrilamine | 0.7 ± 0.1 | 8,612 ± 1,275 | 9,820 ± 1,098 |
| Promethazine | 1.0 ± 0.20 | 402 ± 146 | 14,650 ± 5,783 |
| Ketotifen | 1.2 ± 0.1 | 1,122 ± 127 | 2,458 ± 203 |
| Emedastine | 1.2 ± 0.1 | 39,860 ± 7,453 | 14,498 ± 2,257 |
| Diphenhydramine | 11.9 ± 2.9 | 1,595 ± 141 | 31,480 ± 12,020 |
| Pheniramine | 32.3 ± 2.8 | 14,475 ± 939 | 10,190 ± 1,190 |
| Olopatadine | 36.0 ± 5.7 | 153,983 ± 94,313 | 137,980 ± 28,603 |
| Antazoline | 39.3 ± 3.4 | 40,850 ± 3,794 | 35,295 ± 8,380 |
| Levocabastine | 52.6 ± 9.9 | 27,075 ± 4,996 | 9,506 ± 5,825 |
| Loratadine | 111.9 ± 23.4 | 21,323 ±± 16,298 | 6,620 ± 743 |
Table 2: Relative affinities of various key compounds for histamine
receptor sub-types.
Note: Low Ki number implies a high affinity. Table is arranged to reflect high-to-low H1-receptor affinities [12,13,15,16].
| Compound | Relative Selectivities for Histamine Receptor Sub-types |
||
| H1 relative to H2 | H1 relative to H3 | H3 relati e to H2 | |
| Emedastine | 33,217 | 12,082 | 3 |
| Pyrilamine | 12,303 | 14,028 | <1 |
| Olopatadine | 4,277 | 3,833 | <1 |
| Antazoline | 1,039 | 898 | 1 |
| Ketotifen | 935 | 2,048 | <1 |
| Levocabastine | 515 | 181 | 3 |
| Pheniramine | 448 | 315 | 1 |
| Azelastine | 436 | 1,200 | <1 |
| Promethazine | 402 | 14,650 | <1 |
| Diphenylhydramine | 134 | 2,645 | <1 |
Table 3: Relative selectivities of various compounds for histamine
receptor sub-types (H1-H3).
Note: The larger the number in the above Table, the greater the selectivity. Focus has been drawn to the H1 -receptor since that is most important for ocular anti-histaminic effects of compounds [12,13,15,16].
Not content with its 8-hr Duration of Action (DoA) and the need to dose twice-daily, the Alcon Anti-Allergy Team proceeded to develop novel formulations to overcome Olopatadine’s solubility limitations and obtained US FDA approval of Pataday® (Olopatadine 0.2%, oncedaily t.o. dosing) in December, 2004 (DoA=12-hrs; [31,32], and FDA approval in 2015 for Pazeo® (Fig. 4B; Olopatadine 0.77% once-daily t.o. dosing; rapid onset of action in minutes followed by a DoA up to 24hrs after a single topical ocular drop instillation [7,9,33]. In comparison, other marketed drugs for SAC treatment at that time (Naphcon-A®, Elestat®, Zaditor®) only provided relief of ocular itching and redness between 4-8-hrs and need to be dosed t.o. 2-3/times daily [4-6,23]. Many of the formulations of Olopatadine [Patanol® ; Pataday®; Pazeo®], with Pataday® now available over the counter, are now approved by many health authorities across the globe to help alleviate the suffering of patients that fall victim to the signs and symptoms of SAC every few months throughout the year. Last but not least, the Olopatadine franchise was further enhanced by another Team of Alcon scientists, led by Dr. Michael Wall, who developed a nasal formulation of Olopatadine (0.6%) [Patanase® (Olopatadine 0.6%; approved by FDA in April, 2008) to treat seasonal allergic rhinitis (SAR; [34].
It is noteworthy that as with every drug, the benefit/risk ratio deserves high consideration. As such the ocular anti-allergic drugs and their efficacy discussed above has to be balanced with their side-effects.
Whilst well tolerated, both emedastine and olopatadine can cause a drying effect on the ocular surface due to their low affinity/potency muscarinic receptor antagonist activity. However, if used as prescribed there have not been any serious issues reported for either drug. SAC patients (5% or less) reported some transient ocular side-effects such as the following: blurred vision, burning or stinging, conjunctivitis, dry eye, foreign body sensation, hyperemia, hypersensitivity, keratitis, lid edema, pain and ocular pruritus. Similarly, whilst antihistaminic compounds when taken orally can cause drowsiness, neither emedastine nor olopatadine show this propensity when dosed topically to the eye under the prescribed conditions. Further human experiences with both drugs in terms of side-effects and contraindications can be found in the published literature [35-37], and of course in the appropriate package insert labeling information and dosing directions for Patanol®/ Pataday®/Pazeo®, for example (e.g. https://www.accessdata.fda.gov/scripts/cder/daf).
Taken together, a concerted, diligent and determined effort was expended by our Teams to search for, discover, characterize, in-license and develop novel formulations of Emedastine and Olopatadine for ocular and nasal indications to treat SAC and SAR in patients at a global level. With very close collaboration amongst the key leaders and scientists, including Dr. John Yanni, Dr. Dan Gamache, Dr. Gus Graff and I, and our respective group members and many colleagues in the Development division, the global registration and marketing of Emedine®, Patanol®, Pataday® and Pazeo® were made possible. Mr. Shouxi Xu and Mr. Steve Miller, along with many other laboratory personnel such as Lori Weimer, Milton Brady, Laura Lang, Donna Steven’s, Joan Spellman and others, exemplarily executed the foundation building and subsequent work done in our respective laboratories, and helped us spear-head this effort. Their many contributions, along with those of many other team members, are humbly acknowledged and were responsible for our collective success in bringing these important products to the market for the clinical management of SAC and SAR, two very common and bothersome diseases that afflict millions of people on a global scale and which cause untold discomfort, itching and pain, photophobia and general malaise, and rob the patients’ ability to perform other essential tasks [4-11]. We were fortunate enough to be able to deploy modern techniques and technologies at the time to find, in-license from Kyowa Hakko Kogyo (Tokyo, Japan), pharmacologically and functionally characterize the world’s first dual pharmacophoric molecule (Olopatadine; H1 -antagonist+mast cell stabilizer) for ocular utility, now approved for treatment of SAC and SAR, and thereby help reduce the suffering of many millions of patients around the world that become incapacitated by these diseases every few months every year. This collective and collaborative effort earned the main Team (Dr. John Yanni, Dr. Naj Sharif, Mr. Shouxi Xu, and Mr. Steve Miller), the “Sir James Black Award” for contributions to drug discovery by the British Pharmacological Society in December, 2017).
According to the WHO, glaucoma is categorized as progressive damage to the optic nerve that connects the eye to the brain. Initially, loss of vision occurs in the periphery and can progress to severe vision impairment. This is known as open-angle glaucoma of which the most common type is Primary open-angle glaucoma (POAG), the 2nd leading cause of global irreversible blindness that currently afflicts millions of people. The projections for POAG incidence range from ~80 million by 2020 to >112 million by 2040 [38-41]. Associated with such global visual impairment is poor quality of life, lost revenue and a huge medicinal and/or surgical treatment burden on nations around the world. Ocular hypertension (OHT), due to elevated intraocular pressure (IOP), is the major risk factor associated with POAG [1- 3,39,40]. POAG is a progressive degenerative optic neuropathy where the optic nerve thins (due to loss of axons of the dead or injured retinal ganglion cells [RGCs]), the lamina cribosa tissue is displaced and begins to collapse [42-45], and connections to the brain thalamic nuclei and visual cortex are lost [1-3,39,40]. IOP is controlled by the rate of AQH production by the ciliary processes and the rate of efflux from the ANC through the conventional outflow pathway (TM), and to a lesser degree via the uveoscleral (UVS) pathway (Figure 1A and 1B). By the late 1980s, pharmaceutical or surgical treatments to treat this blinding disease were centered around the use of a few old drugs (e.g. Betablockers [timolol, betaxolol], alpha-adrenergic agonists [brimonidine, apraclonidine] and carbonic anhydrase inhibitors [dorzolamide, brinzolamide]; Table 4) which had relatively low efficacies, short duration of action, and many side-effects [1-3,39,40]. The latter drugs worked to reduce production of AQH and thus reduced IOP which is not good for the overall health of the intra-ocular tissues within the ANC that require nourishment via the freshly generated AQH. At the time, pilocarpine (a muscarinic agonist; 2-4-times daily t.o. dosing) and trabeculoplasty were the only means for enhancing AQH outflow to lower IOP [1-3,39,40].
| Pharmacological Class of Compounds | Examples of Approved Drugs | Mechanism(s) of Action | Comments |
| Cholinergic muscarinic receptor agonists | Pilocarpine, carbachol | Increase conventional outflow of AQH | The oldest drug therapy for glaucoma; use limited by 4x daily topical ocular [t.o.] dosing and browe ache/ meiosis |
| Beta-adrenergic receptor antagonists (“beta blockers”) |
Timolol, betaxolol, levobunolol | AQH Inflow suppression | Widely utilized; 2x-t.o. daily dosing; can induce bradycardia; contra-indicated in asthmatics |
| Carbonic anhydrase inhibitors | Dorzolamide, brinzolamide | AQH Inflow suppression | Oral acetazolamide and methazolamide were used in the past; currently used for acute IOP control instead of chronic therapy; 2x-t.o. daily dosing |
| Alpha2-adrenergic receptor agonists | Epinephrine, Apraclonidine, Brimonidine | AQH Inflow suppression and increase uveoscleral outflow | Epinephrine and dipivefrin used historically; brimonidine widely used nowadays; 2x- daily t.o. dosing |
|
Prostaglandin analogs (FP-receptor agonists) |
Latanoprost, Travoprost [AL- 6221], Bimatoprost, Tafluprost |
Increase uveoscleral, and also conventional, outflow of AQH | The most widely-used, most potent, and most efficacious drug class enabling 1x-t.o. dosing; cosmetic side-effects |
| Prostaglandin Conjugates | Latanoprostene bunod (Latanoprost conjugated to an nitric oxide [NO] donor ) | Increase uveoscleral, and also conventional outflow of AQH | Efficacious IOP-lowering using dual mechanisms of action; 1x-t.o. dosing; propensity for greater hyperemia induction due to NO |
| Rho kinase inhibitors | Ripasudil, Netarsudil | Increase conventional, outflow of AQH (perhaps also enhancing episcleral venous outflow) |
Relatively efficacious IOP-lowering; propensity for greater hyperemia induction |
| Combination products | Examples include: brimonidine+brinzolamide; travoprost+timolol; latanoprost+netarsudil | Enhancement of outflow and suppression of inflow of AQH | Efficacious IOP-lowering using dual mechanisms of action; 1x-t.o. dosing; |
Table 4: Approved drugs for combating OHT/POAG and their mode(s) of action
My interest in prostaglandins (PGs) began in the early 1990s when I joined Alcon Laboratories, Inc (Fort Worth, Texas, USA). Whilst a number of naturally occurring PGs had been shown to lower IOP in animals after t.o. installation, these were deemed too labile, caused many undesirable ocular side-effects and were thus unsuitable as drug candidates. We felt that by chemically modifying some of the classes of PGs we could find compounds that could become drugs to treat POAG. Pharmacia/Pfizer were in the lead at the time with their prototypic FP-receptor agonist, latanoprost, which eventually gained FDA approval for glaucoma treatment in 2001 (Table 4). Although the Alcon Team was behind the competition, we felt that we could generate a better, perhaps more efficacious drug to lower and control IOP and thus treat POAG. The task I set for myself was to establish, validate and utilize a high-throughput screening (HTS) platform to permit the discovery of novel PGs as therapeutics to treat ocular hypertension (OHT) and POAG. Additionally, it was important to demonstrate that the PG receptors we wished to engage with our future drug(s) were present in the appropriate human ocular tissues and cells. The Team of talented, hard working and dedicated scientists in my group included Drs. Brenda Griffin, Terry Davis and Julie Crider, and Gary Williams, Shouxi Xu, and Colleen Drace. This Team was strengthened by the subsequent recruitment of additional key scientists such as Drs. Curtis Kelly, Raj Patil, and support staff including Parvaneh Katoli and Linya Li. A few years later, additional scientists such as Drs. William Howe, Iok-hou Pang, Debra Shade, and Peggy Hellberg, Anna Carpenter joined my group. Additionally, the In Vivo Pharmacology group (under the leadership of Dr. Marsha McLaughlin) was merged with my Molecular Pharmacology Unit, and a Core Ocular Pharmacology Department was created which I led and managed for many years.
PG receptors of different classes were localized and quantified using computerized autoradiographic techniques utilizing thin sections of postmortem human eyes and radioligands such as [3H]-PGF2α, [3H]- PGE2, [3H]-AL-5848 [travoprost acid] and [3H]-BWA868C (e.g. FPreceptors as shown in figure 5, table 5 [46-49]). An RT-PRC technology approach was also taken to determine the distribution of PG receptor mRNAs in human ocular tissues of interest [50,51] using internal resources and external collaborations. Numerous PG receptorspecific-binding assays [52-57] (Tables 6 and 7) and in vitro functional assays [58-70], using human ocular and other cell-types bearing the receptors and enzymes of interest and various second messenger readouts (Tables 8 and 9) were rapidly established and validated using a variety of PG agonists and antagonists. These multiple assays allowed us to screen hundreds of PG compounds that our expert and talented medicinal chemists (e.g. Dr’s. Tom Dean, Mark Hellberg, Robert Saliah, Zixia Feng, Peter Klimko, Paul Zinke, Ray Conrow, Dennis Dean, and Brian Severns, Pete Delgado, Mike Gaines and many others) designed and synthesized (see ahead). These novel compounds were rank-ordered based on their relative affinities, agonist potencies and intrinsic activities [e.g. 53,56,58, 60-69], and in some cases antagonist activities [64]. In conjunction with academic collaborators such as Drs. Ata Abdul-Latif, Shahid Husain, Sunny Ohia, Catherine Opere, Fatou Njei-Bye, Janet Parker, Craig Crosson, etc., I also established productive relationships and tested many lead compounds for their ability to contract ocular and other tissues [71,72]. Additional profiling of key compounds of interest was conducted at outside contract facilities under my direction in order to define their side-effect (off-target) profiles. A select number of lead PG compounds were tested for their ability to lower and control intraocular pressure (IOP; a key risk factor for development of glaucoma) in rabbit, cat and Cynomolgus monkey models of OHT, led by Drs. Marsha McLaughlin, Verney Sallee, Carol Toris, and Byron Li, Tony Wallace, Daniel Scott, Laura Klekar, Terri Kraus, Shenouda Yacoub, and many other colleagues). The in vitro and in vivo studies allowed us to determine good correlations for the ability of PG compounds to bind to FP-receptors, induce intracellular second messenger production, and to cause feline meiosis and to lower monkey IOP [73]. As a result of such research conducted over many years, we were able to identify, characterize (Figures 6-9, Tables 7-9), and nominate clinical candidate FP-receptor agonist PGs whose proof-of-concept was evaluated in several clinical trials (e.g. Figure 10), and which culminated in the approval of once-daily t.o. dosing of Travatan® (0.004% travoprost isopropyl ester; a potent, and efficacious FP-receptor full agonist for once-daily t.o. dosing at night; Fig. 6) by the US Food and Drug Administration and European Medicines Agency for the treatment of OHT associated with glaucoma [74-76]. Many colleagues, too numerous to mention here, in the Development Division covering formulations research, pharmacokinetics, clinical pharmacology, toxicology, regulatory science, packaging, and of course clinical trials ensured the afore-mentioned success. Additional clinical candidates that emerged included other FP-class PG agonists (e.g. AL12182 [77,78]) and numerous other efficacious ocular hypotensive drug candidates [79-83] that demonstrated clinical efficacy in terms of reducing IOP in OHT/POAG patients. In an effort to expand the PG franchise, we discovered certain DP-receptor agonist PGs, for which receptors were visualized by autoradiography and shown to be present in the ciliary processes and ciliary muscle of human eyes (key sites of action of these types of compounds [48,49]), that appeared as another useful class of IOP-reducing compounds. Subsequently, several potential clinical candidates were discovered and which demonstrated ocular hypotensive efficacy in OHT/POAG patients (e.g. AL-6598) [75,79].
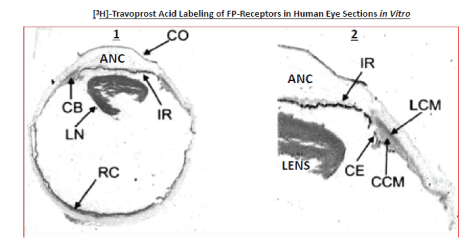
Figure 5: Visualization of the sites of action FP-receptor agonists in human eye using in vitro autoradiography performed on sections of postmortem human eyes using [3H]-AL-5848 (free acid of Travatan®) as the radioligand. The left panel shows the whole eye, whereas the right panel just focuses on the front of the eye. ANC=anterior chamber; CO=cornea; CB=ciliary body; IR=iris; LN=lens; RC=retinachoroid; LCM=longitudinal ciliary muscle; CE=ciliary epithelial cells; CCM=circular ciliary muscle [47].
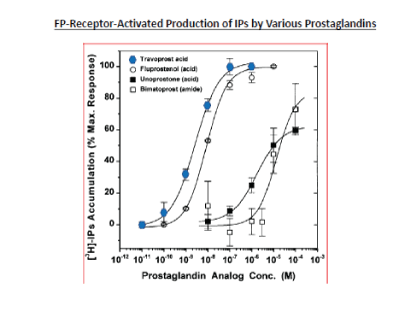
Figure 6: Relative agonist potencies of various FP-receptor agonists to stimulate the production and accumulation of [3H]-IPs as an index of functional activity in primary human TM cells. (Modified with gratitude from [69].
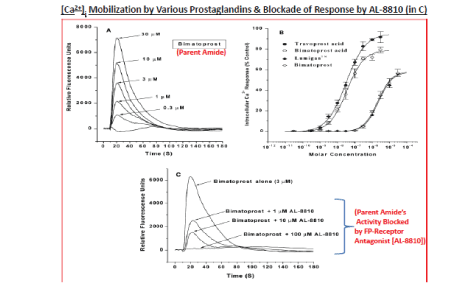
Figure 7: The stimulation of [Ca2+]i production in Swiss 3T3 mouse fibroblast in response to various FP-receptor agonists is shown. Panel A displays the time-course and concentration dependence of [Ca2+]i mobilization by bimatoprost the whole amide molecule. Panel B depicts the concentration-response curves for the free acids of Travoprost and Bimatoprost, and to bimatoprost (amide) either purchased as the powder or the ophthalmic Lumigan® solution containing 0.03% bimatoprost diluted to the required concentrations. Finally, panel C shows that in the presence of the FP-receptor antagonist, AL-8810, the responses to Bimatoprost are blocked with increasing antagonist concentrations, thus indicating that bimaoprost’s actions are mediated via the FP-receptor [139].
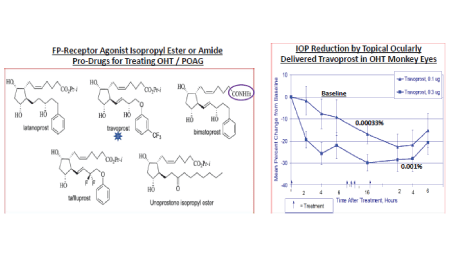
Figure 8: The chemical structures of various FP-receptor agonists are shown in the left-side panel. The right-side panel depicts the ability of two different t.o. doses of Travoprost to reduce the IOP in the OHT eyes of Cynomolgus monkey eyes.
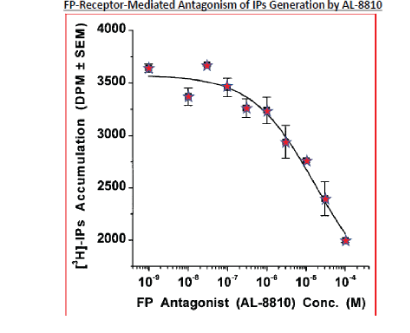
Figure 9: Antagonism of the fluprostenol (FP-receptor agonist)-induced [3H]-IPs generation by AL-8810 in isolated primary human TM cells. The concentration-dependent blockade of fluprostenol’s functional activity by the FP-receptor antagonist, AL-8810, is clearly demonstrated. (Modified with gratitude from [69].
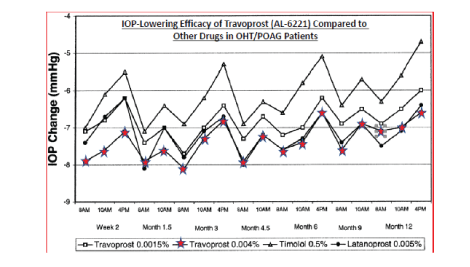
Figure 10: Clinical data depicting the IOP-lowering efficacy of two different concentrations of Travoprost (0.0015% and 0.04%) compared with timolol (0.5%) and Latanoprost (0.005%) in OHT/POAG patients are shown. [75].
| Total [3H]PGF2αBinding (DLU/mm2) | Non-specific [3H]PGF2αBinding (DLU/mm2) | Specific [3H]PGF2α Binding (DLU/mm2) | % Specific [3H]PGF2αBinding | |
| Human Ocular Tissues | ||||
| Iris sphincter muscle | 26,317 ± 8,262 | 7,056 ± 1,401 | 19,262 | 73.2% |
| Longitudinal ciliary muscle | 18,767 ± 3,607 | 6,026 ± 1,846 | 12,741 | 67.9% |
| Neural retina | 17,966 ± 3,718 | 8,422 ± 2,030 | 9,544 | 53.1% |
| Iris (minus sphincter muscle) | 9,436 ± 1,065 | 5,660 ± 1,184 | 3,776 | 40.0% |
| Circular ciliary muscle/ciliary epithelium | 7,337 ± 1,250 | 4,782 ± 1,218 | 2,554 | 34.8% |
| Choroid | 5,992 ± 2,046 | 4,322 ± 1,431 | 1,671 | 27.9% |
| Cornea | 6,693 ± 1,388 | 5,135 ± 989 | 1,558 | 23.3% |
| Lens | 15,211 ± 3,477 | 13,325 ± 3,150 | 1,886 | 12.4% |
Table 5: Distribution of FP-receptors in various ocular tissues of human eyes using [3H]PGF2α as the radioligand and using quantitative
autoradiography.
DLU=digital light units as captured by the image analysis equipment during quantification of the receptor autoradiographs [46,152].
| Natural PG | PG Binding Inhibition Constants (Ki, nM) and Receptor Selectivity (x) |
|||||||
| DP | EP1 | EP2 | EP3 | EP4 | FP | IP | TP | |
| PGD2 | 81 ± 5 | >19,000 (x 234 ) |
2973 ± 100# | 1115 ± 118 (x 14) |
± 180 (x 26) | 2500 ± 760 (x 31) | >140,000 (x 1728) | >35,000 (x 432) |
| PGE2 | >10,000 (x 667 vs EP1) |
26 ± 10 | 4.9 ± 0.5 # | 3 ± 0.2 | 0.9 ± 0.03 | 3400 ± 710 (x 227 vs EP1) | 53708 ± 2136 (x 3581 vs EP1) | >10,000 (x x 667 vsEP1) |
| PGF2α | 18,000 ± 6,460 (x 138) |
594 ± 12 (x 5) |
964 ± 64 # | 24 ± 8 (x 0.2) | 432 ± 25 (x 3) |
130 ± 6 | ≥ 50,000 (x 385) | ≥ 190,000 (x 1462) |
| PGI2 | 3537* (x 3) | >15,000 (x 11) |
nd | 5375 ± 1394 (x 4) |
8074 ± 254 (x 6) |
>86,000 (x 62) | 1398 ± 724 | >65,000 (x 46) |
Table 6: Relative affinities of natural prostaglandin for PG receptor sub-types and their relative selectivities for the cognate receptor ligands [56].
| PG Analog | PG Receptor Binding Inhibition constants (Ki nM) and FP Receptor Selectivity (x) |
|||||||
| DP | EP1 | EP2 | EP3 | EP4 | FP | IP | TP | |
| Travoprost acid ((S)-Fluprostenol) |
52,000 ± 7,200 (x 1,486) |
9,540 ± 1,240 (x 273) |
nd |
3,501 ± 461 (x 100) |
41,000 ± 2,590 (x 1,171) |
35 ± 5 |
≥ 90,000 (x 2,571) |
≥ 121,000 (x 3,457) |
| (R/S)-Fluprostenol | > 50,000 (x 510) |
12,300 ± 1,240 (x 126) |
>100,000# | 4,533 ± 597 (x 46) |
14,400 ± 1,550 (x 147) |
98 ± 9 | >60,500 (x 617) |
121,063 ± 20,714 (x 1,235) |
| Bimatoprost acid (17-phenyl-PGF2α) | >90,000 (x 1,084) |
95 ± 27 (x 1) |
nd | 387 ± 126 (x 5) |
25,700 ± 2,060 (x 310) |
83 ± 2 | >100,000 (x 1,205) |
>77,000 (x 928) |
| Latanoprost acid (PHXA85) | ≥ 20,000 (x 204) |
2,060 ± 688 (x 21) |
39,667 ± 5,589# |
7,519 ± 879 (x 77) |
75,000 ± 2,830 (x 765) |
98 ± 11 | ≥ 90,000 (x 918) |
≥ 60,000 (x 612) |
| Bimatoprost (Amide) | >90,000 (x 14) |
19,100 ± 1,450 (x 3) |
nd | >100,000 (x 16) |
>100,000 (x 16) |
6,310 ± 1,650 |
>100,000 (x 16) |
>100,000 (x 16) |
| Unoprostone (UF-02; Acid) | >43,000 (x 7) |
11,700 ± 2,710 (x 2) |
nd | ≥ 22,000 (x 4) |
15,200 ± 3,500 (x 3) |
5,900 ± 710 |
>30,000 (x 5) |
>30,000 (x 5) |
| S-1033 (Na+-salt) |
90,000 (x 4) |
13,500 ± 1,670 (x -2) |
nd | ≥ 77,000 (x 4) |
6,650 ± 610 (x -3) |
22,000 ± 2600 |
>30,000 (x 1) |
>30,000 (x 1) |
Table 7: Relative affinities of synthetic prostaglandins for PG receptor sub-types and their relative selectivities [56].
| Compound | Agonist Potency (EC50; nM) at Various Prostaglandin Receptors and Subtypes | ||||||
|
DP-receptor (↑ cAMP) |
EP1-receptor (PI turnover; or other response) | EP2-receptor (↑ cAMP; or other response |
EP3-receptor (various functional responses) |
EP4-receptor (↑ cAMP ) |
IP-receptor(↑cAMP or other response) |
TP-receptor (PI turnover; or other response) | |
| PGD2 | 74 | 3190* | 58,000 | nd | >10,000 | >10,000 | >10,000 |
| PGI2 | >10,000 | 319* | >10,000 | 3019#; | >10,000 | 7 | >10,000 |
| PGE2 | >1000 | 2.9* | 67 | 19.9#; 45##; 4.5** |
40 | 3310 | >10,000 |
| PGF2α | >10,000 | 29* | >10,000; | 691#;>10000##; 2000** |
>10,000 | 3,000* | >10,000 |
| Bimatoprost acid | >10,000 | 2.67* | >10,000 | nd | >10,000 | >10,000 | >10,000 |
| Travoprost acid | >10,000 | nd | >10,000 | >10,000 | >10,000 | >10,000 | >10,000 |
| Latanoprost acid (PHXA85) | >10,000 | 119* | 20,000* | 12,000@ | >10,000 | >10,000 | >10,000 |
| Cloprostenol | >10,000 | 93* | >10,000 | 228 | >10,000 | >10,000 | >10,000 |
| S-1033 | >10,000 | >30000@ | >10,000 | >10000@ | >10,000 | >10,000 | >10,000 |
| Unoprostone (UF-021) | >10,000 | >30000@ | >10,000 | >10000@ | >10,000 | >10,000 | >10,000 |
Table 8: Relative agonist potencies of natural and synthetic prostaglandins for PG receptor sub-types.
Data are from various sources using different methodologies and functional readouts [56].
| Compound | Stimulation of PI Turnover and Production of IPs (Functional Response) in Different Cell Types (Agonist Potency, EC50 [nM]) |
||||
| Human ciliary muscle (CM) cells | Human Trabecular meshwork (TM) cells | Human cells (HEK-293) expressing cloned human ocular FP receptor |
Mouse Swiss 3T3 fibroblasts |
Rat A7r5 vascular smooth muscle cells | |
| Travoprost acid ((+)-fluprostenol) | 1.4 ± 0.2 | 3.6 ± 1.3 | 2.4 ± 0.3 | 2.6 ± 0.2 | 2.6 ± 0.5 |
| Bimatoprost acid (17-phenyl-PGF2α) | 3.8 ± 0.9 | 28 ± 18 | 3.3 ± 0.7 | 2.8 ± 0.2 | 2.8 ± 0.6 |
| (±)-Fluprostenol | 4.3 ± 1.3 | 11 ± 2 | 4.6 ± 0.4 | 3.7 ± 0.4 | 4.4 ± 0.2 |
| PGF2α | 104 ± 19 | 62 ± 16 | 29 ± 2 | 26 ± 3 | 31 ± 3 |
| Travoprost (Isopropyl ester) | 123 ± 65 | 103 ± 27 | 40.2 ± 8.3 | 81 ± 18 | 46 ± 6 |
| Latanoprost acid (PHXA85) | 124 ± 47 | 35 ± 2 | 45.7 ± 8.4 | 32 ± 4 | 35 ± 8 |
| Latanoprost (Isopropyl ester) | 313 ± 90 | 564 ± 168 | 173 ± 58 | 142 ± 24 | 110 ± 19 |
| Unoprostone(UF-021; acid) | 3503 ± 1107 | 3306 ± 1700 | 3220 ± 358 | 617 ± 99 | 878 ± 473 |
| Unoprostone isopropyl ester | 8420 ± 912 | 2310 ± 1240 | 9100 ± 2870 | 560 ± 200 | 458 ± 85 |
| Bimatoprost (amide) | 9600 ± 1100 | 3245 ± 980 | 681 ± 165 | 12100 ± 1200 | 6850 ± 1590 |
Table 9: Relative agonist potencies of various synthetic prostaglandins for FP-receptors expressed in various cell-types [56].
Given that PGs generally have several biological activities, it is important that as the ocular utility of FP-receptor agonists has expanded to include many different types of prostanoids, the following side-effects have been noted with Travatan®, akin to other FP-agonists including latanoprost, bimatoprost, tafluprost. The most common ocular adverse event observed in controlled clinical studies with Travatan® 0.004% was ocular hyperemia which was reported in 35 to 50% of patients. Approximately 3% of patients discontinued therapy due to conjunctival hyperemia. Ocular adverse events reported at an incidence of 5 to 10% included decreased visual acuity, eye discomfort, foreign body sensation, pain, and pruritus. Ocular adverse events reported at an incidence of 1 to 4% included, abnormal vision, blepharitis, blurred vision, cataract, cells, conjunctivitis, dry eye, eye disorder, flare, iris discoloration, keratitis, lid margin crusting, photophobia, subconjunctival hemorrhage, and tearing. Nonocular adverse events reported at a rate of 1 to 5% were accidental injury, angina pectoris, anxiety, arthritis, back pain, bradycardia, bronchitis, chest pain, cold syndrome, depression, dyspepsia, gastrointestinal disorder, headache, hypercholesterolemia, hypertension, hypotension, infection, pain, prostate disorder, sinusitis, urinary incontinence, and urinary tract infection. The latter are reported in the package insert for this ocular hypotensive drug.
Based on the success of the research and development of Travatan®, additional drugs classes were sought for the treatment of OHT/ POAG. Thus, we also found some relatively potent and efficacious ocular hypotensive rho kinase inhibitors as designed and synthesized by Drs. Mark Hellberg, Jesse May, H-H Chen, and many others, and those tested by Drs. Raj Patil and Curtis Kelly, and by Shouxi Xu, Linya Li, Colleen Drace and Gary Williams, and by the Team members of Dr. Marsha McLaughlin’s group under my direction [84-89] (Figure 11). Likewise, a proposal made by Dr. Jesse May and I in the mid/ late-1990s resulted in launching another drug discovery program, this time centered around the role of serotonin (5-hydroxy tryptamine; 5-HT) receptors in modulating OHT since there was ample internal evidence and literature supporting such an approach [90-98]. However, the task was rendered extremely difficult since there were 7 known 5-HT receptors and multiple sub-types known, and with agonists and antagonists for each, the exact target to pursue was obscure. Conflicting literature and compound classes showing IOPlowering, and with major species differences, our Team set to work out which receptor(s) were involved using our OHT monkey model. Such arduous research conducted over several years, and using a broad array of agonists and antagonists and numerous kinds of assays [90- 106] led to the identification of a novel class of 5-HT agonists with high affinity and selectivity for the 5-HT2A receptor sub-type [107-117] which efficaciously lowered and controlled IOP in OHT monkey eyes, and which resulted in a number of clinical trials of lead compounds (e.g. AL-34662; AL-37807) [100,107,109,115] (Figure 12). The design and synthetic efforts, behind these serotonergic drug candidates and other key compounds in this series, of our expert medicinal chemists, such as Drs. Jesse May, Anura Dantanarayana, Suchi Mohapatra, H-H Chen, Paul Zinke, Abdel Namil, Zixia Feng, and many others are gratefully acknowledged.
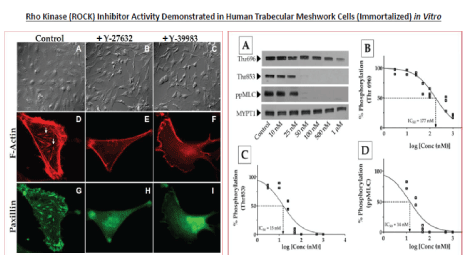
Figure 11: The effect of two different rho kinase (ROCK) inhibitors on cell morphology of immortalized human TM cells is shown. The large left-side panel shows the effect of treatment of hTM cells with Y-27632 (5 µM) and Y-39983 (1 µM), relative to the control vehicle-treated cells. The ROCK inhibitors caused shrinkage and retraction of the cells, which assumed a stellate appearance, and loss of all stress fibers and focal adhesions. Phosphorylation of MYPT1 (myosin light chain [MLC] phosphatase complex of Type 1) at Thr853 and Thr696 inhibits dephosphorylation of MLC, leading to an increase in actomyosin contraction. The large right-side panel shows the concentration-response curves for Y-27632. Y-27632 opposed ROCK-dependent phosphorylation of MYPT1 predominantly at Thr853 with a corresponding decrease in MLC phosphorylation [86].
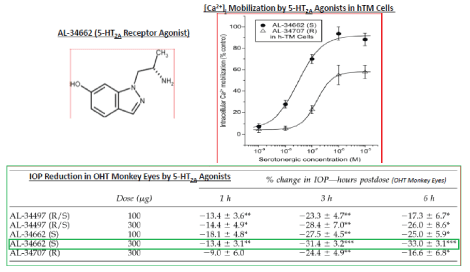
Figure 12: Serotonergic 5-HT2 receptor agonist (AL-34662) and its ability to stimulate [Ca2+]i mobilization in human TM cells and to lower IOP in OHT monkey eyes is shown. (Modified with gratitude from [109].
The last key discovery of new ocular hypotensive drugs that showed remarkable IOP-lowering efficacy in the monkey model of glaucoma/ OHT involved bradykinin (BK; a nonapeptide). Even though historically both PGs and kinins had a somewhat checkered history of notoriety for being inflammatory agents, the success of several FP-receptor agonist drugs (e.g. latanoprost; travoprost, bimatoprost, tafluprost) as potent and powerful ocular hypotensive drugs [reviewed in 76] encouraged our teams to pursue BK agonists for OHT treatment as well. The sense of excitement and pursuit of this target was rewarded by the discovery of the presence of B2 -receptors, by immunohistochemistry, in key tissues (ciliary muscle [118], TM [119] and non-pigmented ciliary epithelial cells [NPCE] [120]) in human and monkey eye sections (e.g. Figure 13). Since peptides generally are poor candidates for topical ocular dosing, it was gratifying that intravitreal (ivt) BK (but not Des-Arg9 -BK [a B1 -BK receptor-selective agonist]) in rabbits quickly lowered IOP [119]. Soon after that began a search for a non-peptide B2 -receptor-selective small molecule that could be administered to the cornea/conjunctiva t.o. rather than injected ivt. From the literature I discovered FR-190997 [121], that we obtained and characterized as a potent high affinity B2 -receptor partial agonist (Figure 14), and thus our drug discovery program was launched. FR 190997 and several other analogs were characterized using in vitro and in vivo assays/models and promptly patented [122-125]. FR-190997 stimulated [Ca2+]i , PGE2 release and MMP production in isolated human TM and CM cells (Figure 14), and it effectively reduced IOP in the OHT monkey eyes in animals composed of several colonies by promoting AQH efflux via the uveoscleral outflow drainage pathways (Figure 15) [126,127]. However, research conducted on isolated perfused porcine eye demonstrated that FR-190997 also could enhance outflow via the TM pathway [126]. Further work resulted in finding yet another non-peptide B2 -receptor agonist lead compound in this novel class of ocular hypotensives, BK2A78 [128]. Again, many different Teams of Alcon scientists were involved in these collective studies encompassing in vitro assays and in vivo models (many mentioned in the above discourse), including additional collaborators in academia such as Drs. Craig Crosson, Shahid Husain, Carol Toris, Sunny Ohia, Juana Galler, and Carlos Belmonte.
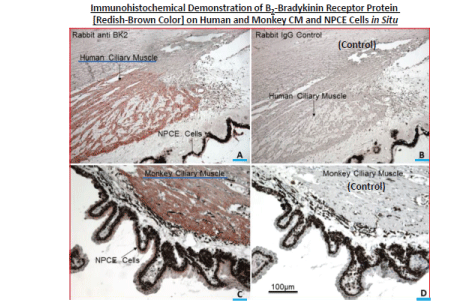
Figure 13: Immunohistochemical demonstration of the presence of B2 -bradykinin receptor protein in human and monkey ciliary muscle and on non-pigmented ciliary epithelial (NPCE) cells [118].
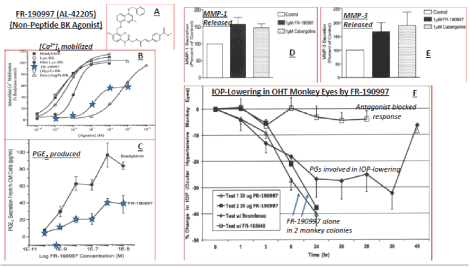
Figure 14: The stimulation of [Ca2+]i mobilization, PGE2 and MMP production in human CM cells, and lowering of monkey IOP by the B2-receptor agonist, FR-190997, is displayed [126].
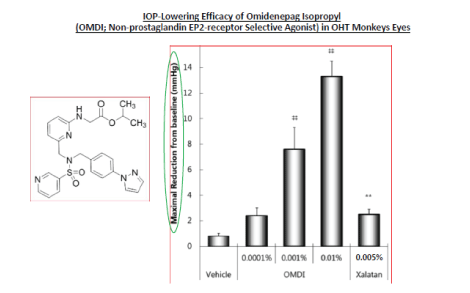
Figure 15: The chemical structure and the ability of different concentrations of Omidenepag Isopropyl (OMDI) to lower IOP in OHT monkey eyes relative to the effect of latanoprost (Xalatan® 0.005%) are shown. Note the very high IOP-reducing efficacy of OMDI relative to Xalatan® [132].
During the aforementioned research, we began postulating the potential use of dual pharmacophore agents and drug conjugates (as opposed to using fixed-dose combination products such a Duotrav® (Travoprost+Timolol) for example). The idea was to link PGs to other IOP-lowering drugs in order to achieve additive IOP-lowering efficacy in animals and humans to treat glaucoma, and this concept was successfully patented [129]. Most recently, since I noticed the profound and rather rapid onset of action of a novel non-PG EP2 - receptor agonist drug (omidenepag isopropyl [OMDI]; Figure 15; [130]) to lower IOP in OHT monkey eyes, we postulated that OMDI may be of value in emergency treatment of rapidly rising IOP and/ or for treating angle-closure and uveitic glaucoma. Accordingly, this hypothesis led to the filing of a patent application [130-132] and presentation of this work at a recent conference [133]. In order to correlate the functional activity of OMDI free acid with EP2- receptors, the historic quantitative autoradiographic distribution of [3H]-PGE2-labeled receptor sites in human eye sections became useful (Table 10). The relatively high density of specific [3 H]-PGE2 - labeled receptor binding to both longitudinal and circular ciliary muscle [79] provides some basis of the action of OMDI lowering IOP in OHT/POAG patients by stimulating uveoscleral and TM pathways.
During our research in PGs to find drugs to treat OHT/POAG, the world’s first FP-receptor antagonist (AL-8810; Figure 9 [64,134]) was discovered that we patented [135-138] and out-licensed to Sigma Chemicals / RBI and Cayman Chemicals so that other researchers could benefit from this discovery. AL-8810 has proven a useful pharmacological tool for interrogating the role of FP-receptors and mechanisms of actions of other drugs in physiological [139] and under pathologic conditions [140-142]. Thus, AL-8810 has shown efficacy in combating symptoms of traumatic brain injury [140], reducing ischemic brain damage [141], decreasing demyelination and motor dysfunction [142], and preventing early labor amongst many other diseases and conditions (e.g. inflammation) (see a recent review [136]). Additional key tools that our research in PGs helped generate included [3H]-AL-5848 (free acid of Travatan®; [47]) and [3H]-BWA868C [48] as radioligands to help characterize and visualize FP- and DP-receptors respectively, in a quantitative manner in human eye sections, and thus help define the mechanism(s) and sites of action of these PG drugs that lower IOP in humans. Furthermore, we performed quantitative pharmacological receptor-displacement experiments using a novel phosphor-imaging technique and defined the PG inhibition constants of many PGs for un-dissectible tissues on sections of human eyes [49], a feat that has not been matched yet as far as we know.
| Human Ocular Tissue | Total [3H] PGE2 Binding(DLU/mm2; x 102) | Non-specific [3H] PGE2 Binding(DLU/mm2; x 102) | Specific [3H] PGE2 Binding (DLU/mm2; x 102) | % Specific [3H] PGE2 Binding as % ofTotal Binding |
| Longitudinal ciliary muscle | 397 ± 57 | 81 ± 6 | 316 | 80% |
| Retina | 482 ± 20 | 197 ± 11 | 285 | 59% |
| Circular ciliary muscle | 267 ± 39 | 59 ± 5 | 208 | 78% |
| Iris | 294 ± 17 | 115 ± 18 | 179 | 61% |
| Ciliary epithelium/process | 163 ± 13 | 73 ± 7 | 90 | 55% |
| Choroid | 121 ± 12 | 73 ± 7 | 48 | 40% |
| Cornea | 106 ± 11 | 87 ± 8 | 19 | 19% |
| Lens | 260 ± 10 | 256 ± 10 | 4 | 2% |
Table 10: Quantitative autoradiographic distribution of EP2-EP4 prostaglandin receptors in human ocular tissues using [3H]PGE2 as the radioligand [79].
In the early 2000s, a significant controversy was ignited with claims of a new mechanism of action of Lumigan® [bimatoprost (17-phenyl-PGF2α-amide)] via a postulated “prostamide receptor” [143]. This was deemed as an attempt by a competitor company to try to differentiate this drug from classical FP-receptor class agonists such as Xalatan® and Travatan® (both isopropyl esters). However, like many other researchers [144-151] it was believed that in fact this amide was no different since in vivo it would be hydrolyzed to its free acid form [144-151] and thus the latter would activate the FPreceptors just like Travatan® and Xalatan® free acids. Furthermore, the FP-receptor antagonist (AL-8810) completely blocked the effects of bimatoprost in various cell-type-based and tissue-based functional assays (e.g. Figure 7) [67-72,76,134,139,149]. Detailed studies were therefore conducted and published in reputable journals to refute the claim of bimatoprost mediating its effects through this enigmatic and mysterious “prostamide receptor” postulate [67-72,76,134,139,149]. Subsequent to these several publications, I was invited to speak at numerous national and international conferences and at various Universities to present our research on discovery, development of ocular therapeutic PG drugs, novel PG tools and the lack of evidence supporting bimatoprost’s mechanism of action via the mysterious “prostamide receptor”. Taken together, I was extremely fortunate in leading teams of talented scientists at Alcon to research and discover novel PG therapeutics (e.g. Travatan® [47,74,76]; AL-6598 [75,59]; AL12182 [77,78]), and tools such as AL-8810, the world’s first FP-receptor antagonist [64,134,135,136], developing, validating stand utilizing the phosphor-based receptor autoradiography technology [47-49,152] and using the novel and newly created highly selective radioligands for mapping the FP-receptors using [3H]-AL-5848 [46,47] and DPreceptors using [3H]-BWA868C [48,49] in human ocular tissues, and performing pharmacological receptor displacement experiments on tissues that were very difficult to dissect out for individual studies [49,152].
A troublesome finding from a number of clinical studies was that some OHT/POAG patients either respond poorly or were totally recalcitrant to latanoprost, the first FP-receptor agonist introduced into medical management of OHT/POAG [153-155]. This phenomenon was attributed to a genetic polymorphism of the FP-receptor and its down-stream coupling mechanism [153-155]. Additionally, it was reported that twice-daily dosing of FP-agonists such as bimatoprost and latanoprost resulted in significantly reduced IOP-lowering efficacy than once-daily dosing [156]. Interestingly, the Alcon-supported research that resulted in cloning of the human ciliary body FP-receptor, that I actually initiated with Dr. Garret FitzGerald at Uni’ Pennsylvania, helped explain the latter clinical findings. Thus, it became evident that the FP-receptor is prone to desensitization when excessive stimulation of the signal transduction pathway occurs, where the intracellular machinery associated with the FP-receptor becomes uncoupled [157]. Consequently, low concentrations of the agonist drugs and a lower frequency of exposure to the t.o. FP-agonist drug treatments are preferred to avoid loss of their efficacy. Through such awareness, this aspect has been successfully adopted by the medical community “less is more”.
As numerous clinical trials during the 2000s demonstrated, the IOP reduction achieved by several different classes of drugs significantly reduces the progression rate of glaucomatous damage and thus preservation of vision [1-3,39,40,76]. Hence, a 10-13% reduction in visual acuity is achieved for every 1mmHg of IOPlowering [1-3,39,40,76]. However, regardless of the great benefit that ocular hypotensive drugs impart to the OHT/POAG patients, there are thousands of patients around the world whose IOPs are within the desired “normal range” and have normotensive glaucoma (NTG; [158]) and whose vision continues to decline. These NTG patients continue to lose their sight, as do OHT/POAG patients as well, despite being on ocular hypotensive therapies. Thus, it has become clear that IOP reduction is not the complete solution to help preserve vision for some patients, and the concept of directly protecting and preserving RGCs and their axons (optic nerve) (“neuroprotection”) needs embracing [159]. To this end, several theories and treatment regimens have been proposed with intensified search for neuroprotectants for central nervous system (CNS) and ocular degenerative diseases [160- 165]. The loss of or diminution of ATP in mitochondria of neurons, in addition to mitophagy disorders in the CNS and retina, has gained much acceptance as to the etiologies of glaucoma and CNS diseases [160-165] with notable successes as potential treatments in animal models of glaucoma/GON. Accordingly, many years ago we showed that indeed human and rat retinas subjected to hypoxic insults show much lower levels of ATP as determined by nuclear magnetic resonance technology, and that ATP concentration could be enhanced in the retinas by blocking the effects of N-methyl-D-aspartatereceptor induced retinal toxicity with MK-801, and by blocking Ca2+-overloading using a Ca2+-channel blocker (diltiazem) [163]. It is therefore pleasing that these early studies have had a direct influence on today’s concepts and acceptance of treatment strategies for GON involving maintenance of energy production and metabolic balance in the retina, a tissue whose energy needs are extremely high [160-165].
All of the above-described research and drug discovery was acknowledged by the The Glaucoma Foundation, and I received the Dr. Roger Vogel Award for exemplary “Pharmaceutical Research” in 2014. This recognition was very humbling and satisfying, and propelled me to continue my drug discovery research in the ensuing years. Therefore, it is imperative that we all continue to seek new and innovative tools (e.g. diagnostic/prognostic biomarkers [166], and disease modifying drugs [161,162,164,165], devices [167], gene-therapies [168], and celltherapies [169] to combat GON [162] induced by OHT and by many other detrimental factors in various forms of glaucoma [1-3,39,40,161].
It has been a pleasure and a privilege to have worked at Alcon Labs/ Alcon Research Ltd/ Alcon-Novartis over the course of 22-years, the longest tenure of my career at a single pharmaceutical company. I have greatly appreciated the opportunity to recruit, train, manage and work with many talented scientists when I first established the HTS platform and multiple Labs for conducting discovery research at Alcon. With some success came career progression with increasing responsibility and scope that helped expand my role and permitted the amalgamatiion and integration of a number of diverse groups into a cohesive single department (Core Pharmacology, Imaging and Biomedical Engineering). Whilst challenging at times, I enjoyed interacting with these colleagues with diverse talents as they pushed and pulled me in different directions as I grew in my leadership role! I learnt a lot, and thank the many colleagues who unselfishly taught me fundamentals of ocular science and who collaborated with my group members and I to achieve some of the most rewarding goals of my research career as described above. The excellent encouragement and support of my mentors and supervisors as Heads of Research and Development during my tenure at Alcon, including Drs. Dalip Ravel, Bill York, Prem Mahendroo, Gerald Cagle, Stella Robertson, Lou DeSantis, Evan Kyba, Marty Wax and John Yanni to name a few, is gratefully acknowledged. As stated at the outset, the above accounts of the discovery, characterization, development and healthy authority approvals of drugs to treat SAC and glaucoma were based upon the Project Team approach. The fruits of labor earned could only have happened due the sustained efforts, dedication, due diligence and industrious participation of Teams of scientists all working together to achieve our organizational and corporate goals. I was only a small cog in the overall operation in the drug discovery campaigns I either helped initiate, nurture, guide and direct or I participated in as a member of the various Project Teams. If I forgot to mention and thank other colleagues, my apologies.
Finally, the intention of this article has been to describe the collective efforts of many to bring suitable products to the market place and to introduce them into medical treatments of a couple of ophthalmic diseases to help patients worldwide suffering from such visual impairment ailments. As such, I declare that there is no conflict of interest in providing this treatise to help future drug hunters gain an insight into the drug discovery research processes, to learn about the history of the discovery/characterization of some now well-known drugs, to review some of the diverse kinds of data gathered during such studies, and to guide and inspire students of pharmacology interested in ocular sciences. I hope this article will accomplish these goals.
It is the humbling and gratifying to report that the International Society Eye Research (ISER) awarded me the coreted Ernst barany prize for “outstanding contributions to ocular pharmacology”- (November 2020).
Download Provisional PDF Here
Article Type: REVIEW ARTICLE
Citation: Sharif NA (2020) Research, Discovery and Development of Novel Therapeutics for the Eye Diseases Allergic Conjunctivitis and Glaucoma. J Ophthalmic Stud 2(2): dx.doi.org/10.16966/2639-152X.118
Copyright: © 2020 Sharif NA. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited..
Publication history:
All Sci Forschen Journals are Open Access