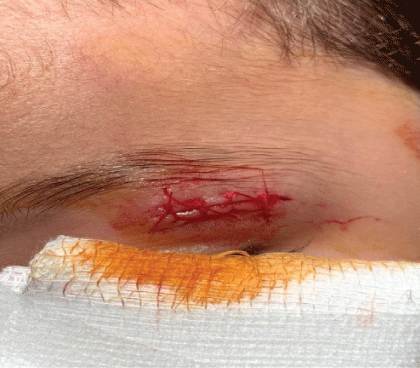
Figure 1: Upper lid tear.


Kashinatha Shenoy M1* Savitha Kashinatha Shenoy2
1Department of Ophthalmology, Medical College and Hospital (MMC&H), Kerala, India*Corresponding author: Kashinatha Shenoy M, Associate Professor, Department of Ophthalmology, Malabar Medical College and Hospital(MMC&H), Atholi, Modakkallur, Calicut, Kerala, India, Tel: +91 9448501547; E-mail: kashinath_sullia@yahoo.co.in
Purpose: This study aims to assess all types of ocular injuries involving anterior and posterior segment of eye presented at Malabar Medical College and Hospital (MMC&H), Calicut, Kerala State, India.
Materials and Methods: This retrospective study was conducted at the Department of Ophthalmology and Emergency Department between January 2017 and December 2018. The medical records of all patients who attended emergency department and outpatient department were retrospectively reviewed. Trained ophthalmologists, optometrists and ophthalmic nurses collected data from medical record department. The descriptive and analytic statistics were carried out.
Results: A total of 218 eyes in 216 patients participated in this study. 180 were male patients (83.33%) and 36 were (16.66%) female patients. Patients of all age groups were considered in this study. Most vulnerable age group was 16-25 years (37.50%) followed by 26-60 years (28.24%). 214 eyes (98.15%) had unilateral involvement and 4 eyes (1.83%) had bilateral involvement.
In our study maximum number of patients were industrial workers followed by farmers. Most common mode of injuries were metallic injury 96eyes (44.03%) followed by non- metallic injury by wood 34eyes (15.59%) and Road Traffic Accident (RTA) 21 patients (9.33%).
The ocular complication related to the different types of trauma were corneal superficial foreign bodies in 96 eyes (44.03%), lid and canalicular tear in 24 eyes (11.00%),corneal epithelial defect in 23eyes (10.55%), subconjunctival hemorrhage in 19 eyes (8.7%), Hyphema in 18 eyes (8.23%),Vitreous hemorrhage in 12 eyes (5.5%), Globe rupture with uveal tissue prolapse in 8 eyes (3.66%), Orbital floor fracture in 7 eyes (3.21%), corneal ulcer in 6 eyes (2.75%),intraocular foreign body in 2eyes (0.91%) (IOFB) and one case of panophthalmitis (0.43%).
Conclusion: Ocular trauma was more common in males. Majority of patients were industrial workers followed by farmers. Cornea was the most commonly affected in our study. Despite our methodology, the inherent limitations of studies should be considered and conclusion drawn from our pooled results should be interpreted with caution. Future large-volume, well-designed with extensive follow-up is awaited to confirm and update the findings of this analysis.
Intraocular foreign body; Open globe; Closed globe; Hyphema; Corneal epithelial defect
Ocular trauma is one of the most neglected area in ophthalmology which causes severe loss of vision in the under developed world. Etiologies of ocular trauma differ in rural area compared to urban area and differ in demographic or socioeconomic classes. Strategies for prevention of ocular trauma require knowledge of the cause or mechanism of injury, which may enable more appropriate targeting of resources towards preventing injuries.
Worldwide there are approximately 6 million people who are blind from ocular injuries, 2.3 million people who are visually impaired bilaterally; these facts make ocular trauma one of the most common causes of unilateral blindness [1].
The classification of ocular trauma was described by Khun F, et al. [2] in 1995. It is divided into two types, open globe and closed globe type. The closed globe type includes contusion and lamellar laceration. The open globe includes rupture, penetration, perforation and intraocular foreign bodies (IOFB).
In India, injuries are found more in males (81%) [3]. This is true for both rural and urban populations, but in the 0-10 age group, the difference between males and females is less. In sedentary workers, farmers, labourers and industrial workers, the male percentage is as high as 95%. Chemical accidents are a common cause of bilateral eye injury [3].
Ocular trauma is a major cause of preventable monocular blindness and visual impairment in the world [4].Up to 40% of penetrating eye injuries are complicated by the presence of an intraocular foreign body (IOFB) [5,6]. It may be toxic (iron, copper, vegetable matter) or inert (glass or plastic). Vision loss may result from the mechanical injury, blunt trauma or from post-traumatic complications such as endophthalmitis, retinal detachment, metal toxicity and sympathetic ophthalmia [6]. Prompt diagnosis, referral, removal of the IOFB and surgical repair will help to preserve the visual acuity and the globe anatomy.
Birmingham Eye Trauma Terminology (BETT) and Ocular Trauma Classification (OTS) Group subdivided mechanical trauma into open and closed globe injuries [2]. Based on the BETT, the mechanisms of injury were classified as rupture, superficial laceration, penetration, IOFB, perforation, and mixed injury.
Mechanical Trauma can be classified into open globe and closed globe injury by BETT [2].
Caused by blunt trauma where the eye globe is intact.
There are two types of closed globe injuries.
Contusion-No full thickness wound.
Lamellar laceration-partial-thickness wound of the eye wall.
Caused by sharp objects, causing full thickness injury of the eye wall (cornea and sclera). It is classified into rupture and laceration.
Rupture-Full thickness wound of the eye wall and is an inside-out injury. Laceration-It is full-thickness wound. Laceration is subdivided into IOFB, Penetrating injury and Perforating injury.
Penetrating injury-The globe integrity is disrupted by a fullthickness entry wound and may be associated with prolapsed of the internal contents of the eye.
Perforating injury-The globe integrity is disrupted in two places due to an entrance and exit wound (through and through injury). This is a quite severe type of eye injury. Both wounds caused by the same object.
The visual acuity of NLP was confirmed by using an indirect ophthalmoscope (IO).
Zone I-Injuries were confined to the cornea and limbus.
Zone II- Injuries involved the anterior 5 mm from the limbus (not extending into the retina).
Zone III- Injuries which includes the macula and optic nerve is posterior to zone II. Extended to the posterior by more than 5 mm from the limbus.
For IOFBs, the zone was defined at the specific entry site.
For perforating injuries, the zone was defined by the posterior defect, generally exit site.
BETT provides a clear definition for all type of injuries, an unambiguous simple and comprehensive system to classify any type of mechanical globe trauma and preferred terminology for categorizing eye injuries in ophthalmic clinical practice.
Khun F, et al. [2] developed ocular Trauma Score (OTS) in 2002, a simplified categorical system for standardized assessment and visual prognosis in ocular injuries (Table 1).
| Initial visual factor A. Initial raw score (based on initial visual acuity) | Raw points NPL | 60 |
| PL or HM= | 70 | |
| 1/200 to 19/200= | 80 | |
| 20/200 to 20/50 | 90 | |
| ≥ 20/40= | 100 | |
| B. Globe rupture | -23 | |
| C. Endophthalmitis | -17 | |
| D. Perforating injury | -14 | |
| E. Retinal detachment | -11 | |
| F. Relative afferent pupillary defect (RAPD) | -10 |
Table 1: Computational method for deriving the OTS scores [2].
PL- Perception of Light, HM- Hand Movements, NPL-No Perception of Light, Relative afferent pupillary defect (RAPD).
The Ocular Trauma Score (OTS) is used to predict the visual outcome of patients after open-globe ocular trauma. The score’s predictive value is used to counsel patients and their families to manage their expectation.
The OTS is a scoring system that includes VA at presentation and the extent of ocular trauma, as well as the presence or absence of globe rupture, endophthalmitis, retinal detachment, and relative afferent pupillary defect. A higher OTS score is typically associated with a better prognosis.
The OTS scores range from 1 (most severe injury and worst prognosis at 6 months follow-up) to 5 (least severe injury and least poor prognosis at 6 months). Each score is associated with a range of predicted post-injury visual acuities. It has a predictive accuracy of approximately 80%, which means that the OTS will be accurate 4 out of 5 times.
A new ocular trauma score by. Acar U, et al. [7] was introduced in pediatric penetrating eye injuries (POTS). (Table 2) In children visual acuity (VA) and relative afferent pupillary defect (RAPD), can be challenging to obtain, especially those who have just sustained eye injuries. Acar and colleagues developed a pediatric ocular trauma score (POTS) that downplayed presenting VA in its predictive model and removed RAPD. The following equation was used to determine the trauma score in patients for whom an initial VA was not obtained.
| Variables | Raw points |
| Initial visual acuity | |
| NLP | 10 |
| LP/HM | 20 |
| Counting Fingers | 30 |
| 0.1-0.5 | 40 |
| 0.6-1.0 | 50 |
| Age of the pediatric patients( years) | |
| 0-5 | 10 |
| 6-10 | 15 |
| 11-15 | 25 |
| Wound Location | |
| Zone 1 | 25 |
| Zone 2 | 15 |
| Zone 3 | 10 |
| Concomitant Eye Pathologies | |
| Iris prolapse | -5 |
| Hyphema | -5 |
| Organic/unclean injury | -5 |
| Organic/unclean injury | -5 |
| Delay of surgery (>48 h) | -5 |
| Delay of surgery (>48 h) | -10 |
| Vitreous haemorrhage | -20 |
| Retinal detachment | -20 |
| Endophthalmitis | -30 |
Table 2: Pediatric Penetrating Eye Injuries (POTS) and Raw Points [11].
2 × (age+zone) - corresponding pathologies.
In children, eye trauma differs in many ways from that in adults and it is very difficult to obtain sufficient history from children about cause of trauma, mode of injury and they may not be aware of a reduction in their visual acuity. As such, diagnostic delay increases the risk of loss of vision and other complications. Under the best ophthalmic setup, it is difficult to check visual acuity (VA) and relative afferent pupillary defect in children’s, (RAPD) The importance of eye trauma has increased because of the relatively high rate of trauma in the pediatric age group. Various studies have reported that 20-50% of ocular injury admissions are children [8,9] . In the United States, eye injuries are the second most frequent cause of presentation for ocular treatment in pediatric cases, following strabismus. [10,11].
This retrospective study was conducted at the Department of Ophthalmology and Emergency Department between January 2017 and December2018. 218 eyes of 216 patients with ocular injuries were enrolled in this study. Only fresh ocular trauma was enrolled, less than 7 days of injury and old ocular trauma were excluded from this study. Treatment history, surgeries and follow-up were not included in this study.
Approval of the study was obtained from the institutional review board and all the patient’s parents were provided informed consent. The study and data collection protocols conformed to all local laws, and complied with the principles of the hospital.
On arrival to Emergency department or outpatient department, following history were noted from all patients such as gender, religion, caste, residential area, marital status, and occupation and education level of patients. It is important to establish mechanism of injury including blunt or penetrating, velocity of object and any other details relevant to injury. Specific history of trauma including date, time, place and seasonal predilection (rainy seasons, harvesting), road traffic accident (RTA), circumstances of injury (occupational or no occupational), characteristic of traumatic agent (solid, fluid, or gas), mode of injury (projectile object, fall, impact) and persons condition at time of injury and assault. Information about use of protective measures at the time of injury was noted.
Symptoms and signs (pain, redness, and decreased vision), treatment or intervention already given and level of consciousness were noted. Visual statuses before injury (previous history and surgery) were asked. All patients underwent basic eye examination including visual acuity, slit lamp examination, intraocular pressure measurement (IOP) if necessary dilated fundus examination, B-Scan, OCT Macula and CT Scan orbit. Following measures were taken on arrival of the patient to Emergency or outpatient department during eye examination. Use of eye shield to protect the eye from further damage. Administration of systemic analgesics, tetanus toxoid and systemic antibiotics for globe rupture or eye lid injuries. Patients were kept Nilper Oral (NPO) status in preparation for surgery. Avoid IOP measurements in patients with corneal laceration and avoid any pressure on the globe. Do not attempt to pull out any foreign material from the eye which will cause further damage.
Plain orbital X-ray: Orbital plain films of the orbits and sinuses are rarely used for diagnosis in orbital trauma. A 3-view plain film series is most useful in evaluating the bony orbits and the sinuses and in identifying radiopaque foreign bodies. Waters projection provides the best view of the orbital floor and detects air-fluid levels in the maxillary sinuses. Caldwell or anteroposterior view visualizes the medial orbital wall, the lateral and superior orbital rims as well as the ethmoid and frontal sinuses. The lateral view is most useful in visualizing the orbital roof, maxillary and frontal sinuses, zygoma, and sellaturcica.
B scan ultrasound is important to detect, when ocular media is hazy to rule out vitreous hemorrhage, retinal detachment intraocular foreign bodies and scleral rupture. It should be used with caution if ruptured globe is suspected and typically deferred if ruptured globe is known.
This is non-invasive method that does not require direct contact with the eye to detect occult rupture, associated optic nerve injury and small foreign bodies as well as to visualize the anatomy of the globe and orbit.
Axial and coronal views of the brain and orbits without contrast utilizing 1-2 mm cuts should be obtained. Some nonmetallic foreign bodies, such as wood, glass, or plastic, may be difficult to visualize acutely on CT. The sensitivity and specificity of ocular CT in determining occult open globe injury varies. Sensitivities ranging from 56-68% and specificities of 70-100% have been reported in recent studies. [12,13] illustrating the need for surgical exploration for definitive diagnosis and management (Table 3).
| Age | n=216Patients | Percentage (%) |
| 0-15 Years | 39 | 18.05% |
| 16-25 Years | 81 | 37.50% |
| 26-60 Years | 61 | 28.24% |
| Above 61 Years | 33 | 15.7% |
| Both Eyes | 2cases | 0.92% |
Table 3: Patient Profile.
MRI is of limited usefulness in the acute stages of ocular trauma and is contraindicated if any concern exists for metallic intraocular foreign body.MRI is excellent in identifying injuries of the soft tissues of the globe and orbit and can be particularly helpful in localizing an organic foreign body such as wood that appears similar to soft tissue.
To measure the various type of ocular trauma involving eyeorbit, eye lid, anterior and posterior segment and its complications. Treatment history, surgeries and follow-up were not included in this study.
Data were analyzed using IBM SPSS statistics 22.0 (IBM Corp. Released 2013. IBM SPSS Statistics for Windows, Version 22.0. Armonk, NY: IBM Corp.) Categorical variables were presented with frequency and percentage, continuous variables presented with mean and standard deviation.
A total of 218 eyes in 216 patients participated in this study. 180 were male patients (83.33%) and 36 were (16.66%) female patients (Table 3).Patients of all age groups were considered in this study. Most vulnerable age group was 16-25 years (37.50%) followed by 26-60 years (28.24%). 214 eyes (98.15%) had unilateral involvement and 4 eyes (1.83%) had bilateral involvement (Table 4).
| Gender | n=216 | Percentage (%) |
| Male | 180 | 83.33% |
| Female | 36 | 16.66% |
Table 4: Patient Demographics.
In our study maximum numbers of patients were industrial workers followed by farmers. Most common mode of injuries were metallic injury 96 eyes (44.03%) followed by non-metallic injury by wood 34 eyes (15.59%) and road traffic accident (RTA) 21 patients (9.33%) (Table 4 and 5).
| Mode Of Injury | n=218Eyes | Percentage (%) |
| Metallic | 96 | 44.03% |
| Non- Metallic | 122 | 55.96% |
| Wood | 34 | 15.59% |
| Stone | 8 | 3.66% |
| Pen/Pencil | 12 | 5.50% |
| Finger Nail | 16 | 7.33% |
| Assault | 18 | 8.25% |
| Chemical Injury | 4 | 1.83% |
| History of Fall From Bed | 9 | 4.12% |
| Road Traffic Accident | 21 | 9.63% |
Table 5: Causes of Eye Injuries.
The ocular complication related to the different types of trauma were corneal superficial foreign bodies in 96 eyes (44.03%), lid and canalicular tear in 24 eyes (11.00%) (Figure1-6), corneal epithelial defect in 23 eyes (10.55%) (Figure 7), subconjunctival hemorrhage in 19 eyes (8.7%) (Figure 8), Hyphema in 18 eyes (8.23%), Vitreous hemorrhage in 12 eyes (5.5%) (Figure 9 and 10), Globe rupture with uveal tissue prolapse in 8 eyes (3.66%) (Figure 11-13), Orbital floor fracture in 7 eyes (3.21%) (Figure 14), corneal ulcer in 6 eyes (2.75%) (Figure 15), intraocular foreign body in 2eyes (0.91%) (IOFB) figure 16 and one case of panophthalmitis (Figure 17). %) (Table 6). Closed -globe injury was more common in 196 eyes (89.90%) and open-globe injury was in 22eyes (10.09%) (Table 7).

Figure 1: Upper lid tear.
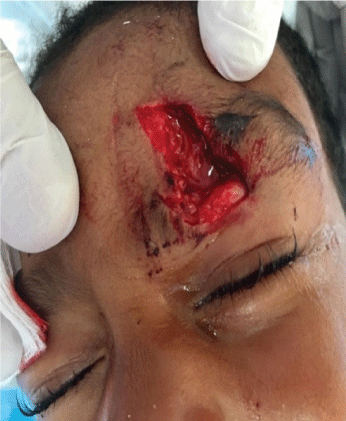
Figure 2: Orbital fat prolapse.
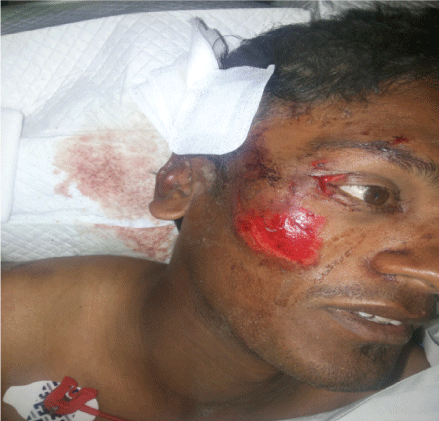
Figure 3: Lateral canthal injury.
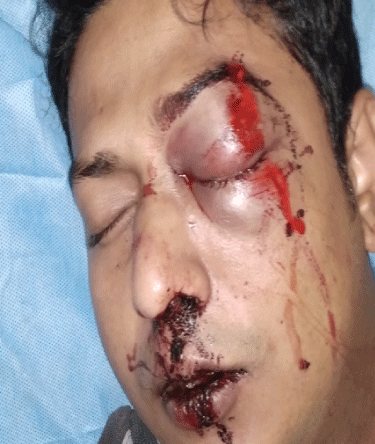
Figure 4: Lid edema.
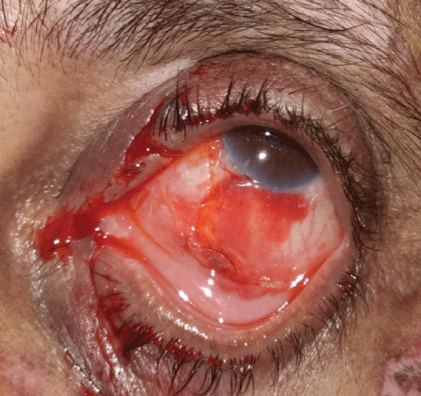
Figure 5: Canalicular injury.
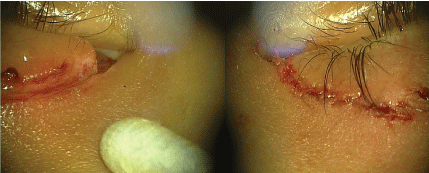
Figure 6: Full thickness lower lid tear.
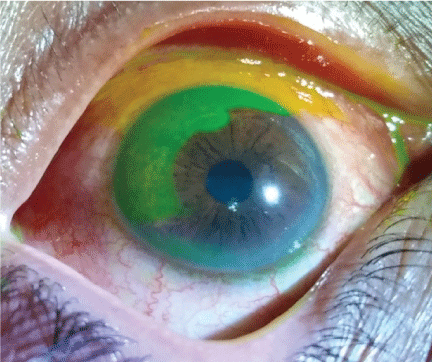
Figure 7: Corneal epithelial defect.
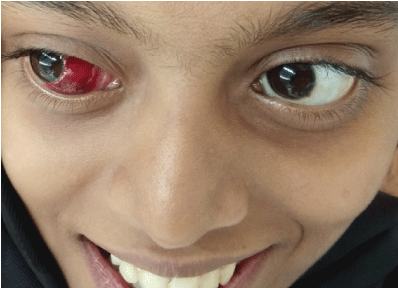
Figure 8: Subconjunctival hemorrhage.
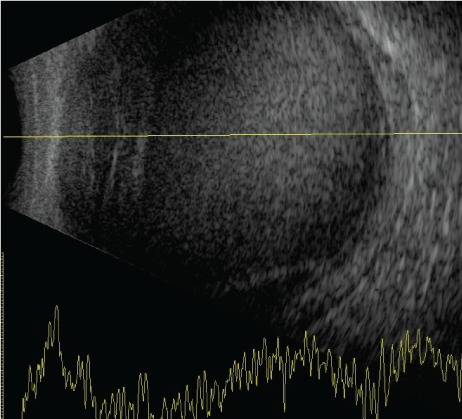
Figure 9: B scans showing vitreous hemorrhage.
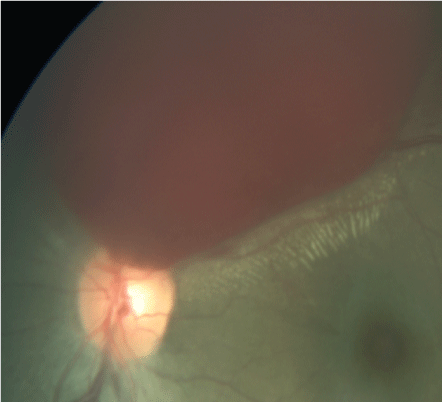
Figure 10: Left eye pre-retinal haemorrhage.
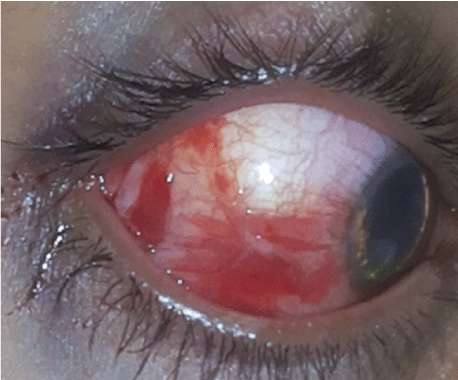
Figure 11: Scleral tear.
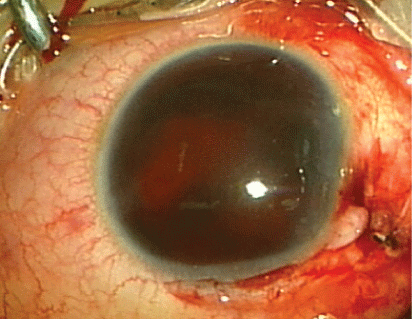
Figure 12: Limbal tear with foreign body.
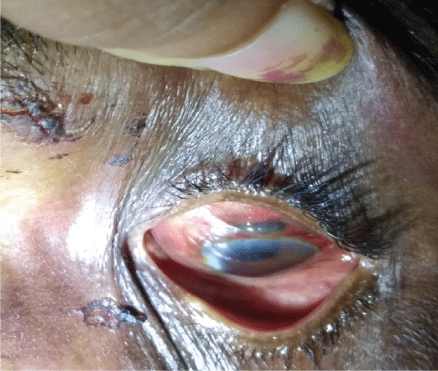
Figure 13: Uveal tissue proplapse.
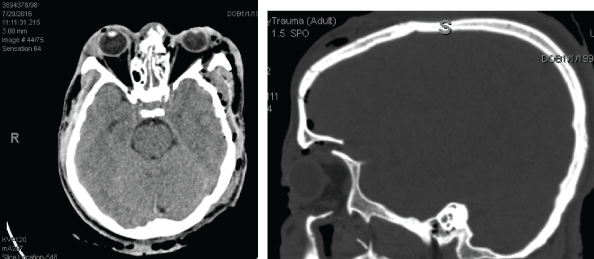
Figure 14: CT scan showing left eye orbital floor fracture.
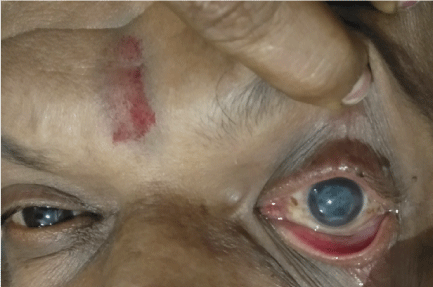
Figure 15: Corneal ulcer.
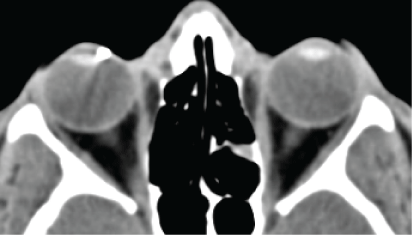
Figure 16: CT scan showing right eye intra ocular foreign body.
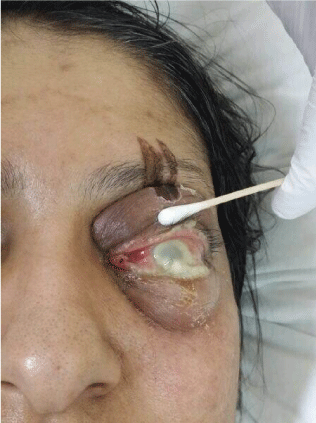
Figure 17: Traumatic panophthalmitis.
This retrospective, hospital-based study provides data on the current pattern of serious ocular injuries in patients attended to a tertiary care teaching centre in the emergency and outpatient department of ophthalmology.
A significant number of injuries were industrial related workers followed by farmers with wood injuries. As most of these injuries occurred in middle aged patients, it underscores a lack of awareness among patients about the hazards of work and not wearing proper protective glasses during working. Despite of the protective nature of the orbit, there is still risk of injury to the globe. Ocular trauma or eye injury remains a common and preventable cause of blindness throughout the world [14,15].
Ocular trauma is one of the major worldwide causes of preventable morbidity and accounts for half a million cases of monocular blindness worldwide [14,15].
This is the most recent and large-scale epidemiological study of ocular trauma in southern India. As observed in this study (male: female-3:1), several workers have reported male predominance in case of ocular trauma. Higher preponderance of ocular trauma in males can be explained by their increased outdoor nature of job, such as farmers, factory workers and drivers [16].
The life time prevalence of ocular trauma is estimated with an annual incidence of about 8.1% per 100,000 US persons. [17-19]The most common types of injuries are foreign bodies (35%), open wounds , contusions (25% each) and burns 15%. 90% of all eye injuries can be prevented with use of protective eye wear [20].
The most common ocular part involved was anterior segment mainly cornea.
In our study maximum number of patients was industrial welding workers followed by farmers.
The study revealed that the most injuries occurred at industrial area and lack of basic safety precautions was the common factor. These findings have implications for health and safety strategies in prevention of serious eye injuries. The current emphasis on safe work environments must be expanded.
In developing countries ocular trauma has not been studied extensively. This study in a developing country such as India underscores that trauma remains a significant cause of monocular vision loss in all age groups with a large proportion affecting younger patients, thereby entailing increased lifetime of disability years. The stress to adopt the use of protective eyewear to avoid most workplacerelated injuries and early interventions are other aspects highlighted by this study.
Despite our methodology, the inherent limitations of studies should be considered and conclusion drawn from our pooled results should be interpreted with caution. Future large-volume, well-designed with extensive follow-up is awaited to confirm and update the findings of this analysis.
The authors of the paper do not have a direct financial relationship with the commercial entities mentioned in the paper that might lead to a conflict of interests.
Download Provisional PDF Here
Article Type: RESEARCH ARTICLE
Citation: Shenoy MK, Shenoy SK (2020) Incidence of Ocular Trauma in Malabar Region of Kerala. Retrospective Study. J Ophthalmic Stud 2(2): dx.doi.org/10.16966/2639-152X.117
Copyright: © 2020 Shenoy MK, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access