
Figure 1: OCT of the macula done on the a) right and b) left eye on the second follow up prior to IV treatment showed normal result. At this time, visual acuity on the right eye was 20/125 and on the left eye was no light perception.


Mary Czarina V San Diego* Erwin D Palisoc
Department of Ophthalmology, Jose R Reyes Memorial Medical Center, Philippines*Corresponding author: Mary Czarina V San Diego, Department of Ophthalmology, Jose R Reyes Memorial Medical Center, Philippines, Tel: +639957458461; E-mail: zrina88@yahoo.com
Objectives: To report a case of bilateral optic neuritis as the initial presentation in Human Immunodeficiency Virus (HIV).
Introduction: There are cases of optic neuritis in HIV patients previously reported and usually caused by secondary infections including syphilis or opportunistic organisms. A direct causal link between HIV and optic neuritis has been suggested but presents with systemic manifestations. This report describes a case of optic neuritis with no other clinical manifestations in a patient with HIV, which in turn is significant and alarming in the Philippines given its a high number of HIV cases in the country.
Clinical Presentation: This is a case of a healthy young male who presented with sudden loss of vision on the left eye, followed by progressive blurring of vision on the right eye associated with ocular pain. No comorbidities and no other symptoms were noted. The patient had Visual Acuity (VA) of 20/125 on the right and no light perception in the left eye. The relative afferent pupillary defect was noted on the left eye. Fundoscopy initially showed normal then progressed to blurred disc margins on both eyes. Laboratory exams were unremarkable except for bilateral optic nerve enhancement on cranial imaging. He was referred for counseling prior to HIV screening, revealing patient’s sexual history being a male having sex with male. Intravenous steroids for 3 days shifted to oral for 11 days were given pending result of HIV testing, which was later revealed as positive. After completion of steroids, there was noted improvement of vision to best-corrected visual acuity of 20/32 on the right and 5/200 on the left eye. Follow up done after HIV treatment showed improvement of vision to best-corrected visual acuity of 20/25 on both eyes.
Conclusion: All cases of atypical optic neuritis should be suspected to have underlying HIV infection. Optic neuritis may be the initial and only manifestation in an HIV patient. This reports a case of optic neuritis with no other clinical manifestations in HIV, which is alarming in the Philippines given its increasing number of HIV cases.
Optic neuritis; Human immunodeficiency Virus pathogenesis; secondary infections in HIV; Atypical optic neuritis; Bilateral optic neuritis; HIV in the Philippines
Infection cases of optic neuritis associated with HIV were reported both locally and abroad. However, these were usually caused by syphilis or opportunistic organisms like cyptococcus, histoplasma, herpes zoster and cytomegalovirus [1]. Likewise, a case of bilateral optic neuritis in acute HIV infection was previously reported but was described in the presence of systemic manifestations prior to the development of optic neuritis [2]. This report is quite unique because it describes a case of bilateral Optic Neuritis with no other associated clinical manifestations in a patient diagnosed with HIV. This is significant and alarming in the Philippines given a dramatic increase in the number of newly diagnosed HIV in this country [3].
To report a case of bilateral optic neuritis as the initial presentation in HIV-infected patients.
This is a case of a 22-year-old, apparently healthy male from Metro Manila, the Philippines who presented with sudden loss of vision of the left eye associated with ocular pain. History started nine days prior to consulting when patient began to have ocular pain on the left eye described as sudden, dull, non-radiating, graded 5/10, more prominent with eye movement and occurring mostly in the afternoon lasting more than one hour. No accompanying symptoms noted.
Five days prior to consulting, with the persistence of pain, the patient noted blurring of vision on the left eye. Two days prior to consulting, there was sudden loss of vision of the left eye and beginning blurring of vision on the right eye. Initial consult was done to a private ophthalmologist who advised the patient for admission. However, the patient opted home against medical advice to seek for second opinion from another doctor. Hence, he consulted at our institution.
Past medical and family history was unremarkable. Social and personal history only showed that the patient works as a restaurant staff waiter. Review of systems was unremarkable with no known comorbidities, and no associated signs and symptoms. Ocular history only showed the use of glasses for three years with stable refraction.
The general physical examination and neurological examination were unremarkable except for the eye. Upon the first consult, visual acuity, using Early Treatment Diabetic Retinopathy Study (ETDRS) chart, on the right eye was 20/63 improved to 20/32 on pinhole, and on the left eye was no light perception. Extraocular movements were full. Pupil examination revealed 3mm reactive to light with relative afferent pupillary defect on the left eye. External examination showed no swelling no proptosis and nonhyperemic conjunctiva, Slitlamp examination was normal with clear cornea and unremarkable anterior segment, deep chamber with no inflammatory reaction and noncataractous lens. Fundoscopic findings showed red-orange reflex, clear media, cup to disc borders of 0.3, and distinct disc borders with no hemorrages nor exudates. Ishihara color vision test showed 15 out of 15 for the right eye.
The initial assessment was optic neuritis of the left eye, and beginning optic neuritis of the right eye. The patient was requested with Optical Coherence Tomography (OCT), perimetry, cranial Magnetic Resonance Imaging (MRI) and laboratory workup. OCT of the macula was unremarkable and perimetry done revealed junctional scotoma (Figures 1 and 2). Perimetry of the left eye was not done since the patient already has no light perception on this eye. Cranial MRI showed: 1) signs of bilateral optic neuritis more prominent on the left side; 2) suggestion of minimal signal changes both in occipital white matter, nonspecific with possibility of demyelination not ruled out; 3) Small cavernoma, left (Figure 3). Laboratories requested showed normal complete blood count, urinalysis, BUN and Creatinine (Figure 4).

Figure 1: OCT of the macula done on the a) right and b) left eye on the second follow up prior to IV treatment showed normal result. At this time, visual acuity on the right eye was 20/125 and on the left eye was no light perception.

Figure 2: Visual field testing (Central 30-2 pogram) of the right eye reveals a superotemporal arcuate defect extending from the blind spot to the vertical midline. There was no light perception on the left eye.

Figure 3: Cranial MRI showed: a) optic nerve enhancement showing signs of bilateral optic neuritis more prominent on the left side; b) minimal symmetrical high T2/FLAIR signal changes in both occipital periventricular white matter with possibility of demyelination not ruled out; and small cavernoma, left with minimal contrast enhancement and no surrounding edema.

Figure 4: Laboratory exam prior to treatment a) Complete Blood Count, Urinalysis, BUN were within normal b) Chest X ray showed normal findings.
Follow up showed the same ocular examination findings except for decreased color vision test on Ishihara test on the right eye with 10 out of 15. At this point, the impression was still optic neuritis since the case has typical presentation of pain prior to loss of vision, normal disc margin, relative afferent pupillary defect, color defect and MRI findings of optic neuritis. However, atypical presentation of optic neuritis was considered since the patient is male with bilateral eye involvement and no light perception of the left eye. The systemic association was reviewed focusing on the possible causes of atypical type of optic neuritis. Review of systems was unremarkable. History including past medical, family, social and personal history were reviewed as well. There were no rash, fever, sores, joint pains, back pain, vomiting, headache, cough, family history of blurring of vision, recent travel to an endemic area, and lymphadenopathy. There were no signs and symptoms of syphilis, sarcoidosis, vasculitis, neuromyelitis optica, compressive and infiltrative disease, Leber’s hereditary optic neuropathy, Lyme disease, pulmonary tuberculosis pointing to systemic associations to atypical type of optic neuritis.
MRI showed negative for compressive, infiltrative disorders that may present with optic nerve edema. A neurologic examination done was unremarkable, negative for Brudzinski’s sign and nuchal rigidity which may signal meningeal process, supported by no dural nor meningeal enhancement on MRI. Aside from the absence of neurologic weakness, the patient did not present with chancre, skin rashes, lymphadenopathy, and neuropsychiatric signs such as consciousness disorders, memory loss, frequent headaches, and muscle weakness that may suggest syphilis. With review of systems showing no difficulty of breathing or cough, chest X-ray revealed negative for nodal enlargement, parenchymal disease and fibrosis suggestive of sarcoidosis and tuberculosis. Chest X-ray also showed no nodular, diffuse nor cavitary involvement seen in Wegener granulomatosis. Testing of antibody titers for Lyme was not done since it is not endemic in the area and there was no history of travel. The patient had no family history of blurring of vision consistent with Leber hereditary optic neuropathy. He had no history of cat exposure pertinent to cat-scratch disease. There were no noted joint pains nor rash, no retinal/choroidal and lid involvement consistent with systemic lupus erythematosus and vasculitis. No proteinuria nor hematuria on urinalysis noted with normal blood urea nitrogen and creatinine, in which such abnormalities may point to focal segmental glomerulonephritis in vascular disease like Wegener granulomatosis. There were no history of recurrent optic neuritis, no loss of bowel and bladder control, no intractable nausea and vomiting and hiccups pertinent to neuromyelitisoptica.
Since the patient was not noted to have any of these, and he was, at this time, noticed to be coming in at the clinic with a male partner, another possible cause was considered. The patient was referred for counseling prior to HIV testing at Research Institution for Tropical Medicine (RITM). Upon counseling, the patient’s sexual history revealed that he is a homosexual male having sex with another male with multiple partners. Regular follow up to our institution was done while awaiting result for HIV screening.
Upon follow up, the patient noticed worsening of blurring of vision of the right eye. The ocular exam showed the same findings except for worsening visual acuity of 20/125, not improved on pinhole, and progression of fundoscopy to blurred disc margins for both eyes (Figure 5). The result for HIV screening was still waiting to be released at this time. The patient was consequently admitted for three days with intravenous (IV) Methylprednisolone 250 mg every 6 hours for 3 days. He was referred to neurology and was assessed to have optic neuritis, both eyes. The patient refused to undergo lumbar puncture, as requested by Neurologist to rule out for multiple sclerosis, clinically isolated syndrome, presenting as optic neuritis. CSF examination was requested by Neurology team to check for immunoglobulins and/or presence of oligoclonal bands to rule out Multiple Sclerosis (MS) as an initial presentation even if the patient is clinically negative for the latter. Despite this, however, MRI revealed negative for MS and only showed optic nerve enhancement. He was, then, discharged with oral Prednisone 1 mg/kg/day for 11 days.

Figure 5: Fundus photo showed: a) on the right eye: blurred disc margin at temporal more on inferotemporal area; b) on the left eye: blurred disc margin at temporal, cup-to-disc-ratio 0.3.
After completion of intravenous steroids, there was an improvement of vision on both eyes with visual acuity on the right eye of 20/80 improved to 20/50 on pinhole, and on the left eye, able to count fingers at 3 feet. Fundoscopy showed distinct disc borders from previously blurred disc margins. There was still relative afferent pupillary defect on the left eye and color deficit on Ishihara test.
After completion of eleven days of oral Prednisone, vision improved in both eyes with visual acuity of 20/63 improved to 20/32 with pinhole on the right eye, and 5/200 on the left eye. It was at this time when the result for HIV screening was released, revealing positive HIV antibody. The patient was referred back to Research Institution for Tropical Medicine (RITM).
The patient underwent anti-retroviral therapy consisting of Lamivudine, Zidovudine, and Efavirenz. Seven months after episode of vision loss, after completion of HIV treatment, there was noted improvement of vision with visual acuity of 20/63 on the right eye and 20/200 in the left eye, both eyes had best-corrected visual acuity of 20/25. There were still relative afferent pupillary defect on the left eye and improved color deficit on Ishihara test with 13 out 15 on the right eye and 1 out of 15 on the left. Repeat complete blood count, urinalysis, fecalysis, and chest X-ray done were normal. Drug testing was negative for Cannabinoids and Methamphetamine and rapid plasma reagin was nonreactive. CD4 count done showed 677 (Figure 6). Currently, the patient has maintained his vision with best-corrected visual acuity of 20/25 on both eyes.
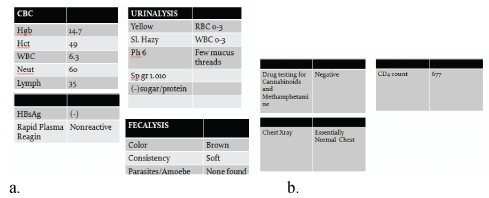
Figure 6: Laboratory exams seven months after treatment showed a) Unremarkable for complete blood count, urinalysis, fecalysis, HBsAg and rapid plasma reagin. b) Drug testing for Cannabinoids and Methamphetamine was negative, chest X ray showed normal and current CD4 count is 677 cells per cubic load millimeter of blood.
This is a case describing a 22-year-old male, a homosexual with multiple sexual partners, who developed atypical optic neuritis in association with HIV. HIV was associated with optic neuritis in this case with confirmation of positive screening, in the absence of other possible systemic disease, no other associated signs and symptoms, and unremarkable laboratory findings.
Optic neuritis is defined as inflammation of the optic nerve. It may be due to a variety of causes including demyelination, immunemediated, direct infections, granulomatous optic neuropathy and contiguous inflammatory disease [4].
Optic neuritis can present with normal or indistinct disc borders. Retrobulbar neuritis occurs far enough behind the optic disc with a normal optic disc appearance during the acute episode. This is the same in this case report, initially presenting with normal disc appearance in the first few days of loss of vision. In approximately one-third of the cases, optic neuritis involves the anterior portion and the optic disc appears edematous, which is usually hyperemic and diffuse. This disc swelling, also known as papillitis, is an inflammation at the optic nerve head (intraocular optic nerve) and is most common in postviral and infectious neuritis than in demyelinating neuritis [5].
Optic neuritis typically occurs in young, female patients with periorbital pain with eye movement prior to subacute monocular visual loss that develops over several days. Other findings include RAPD if unilateral or asymmetric if bilateral, dyschromatopsia, particularly for red, out of proportion to the visual acuity loss, generalized reduction of sensitivity and any pattern of visual field loss in perimetry, and improvement within 1 month usually [5]. In this case, the patient was assessed to have optic neuritis due to the typical presentation of periorbital pain prior to the loss or decreased vision, fundoscopic findings of initially normal to blurred disc margins on fundoscopy, normal anterior segment with afferent pupillary defect, color defect with Ishihara test and MRI findings of optic nerve enhancement.
Most cases of optic neuritis are isolated or with underlying demyelinating cause and do not require further workup unlike those with atypical features. These atypical features include age of onset <15 or >45 years old, progressive visual loss over 2 weeks, simultaneous bilateral vision loss, no light perception vision, absence of periocular pain, lack of substantial visual recovery within 3 months, visual decline after withdrawal of corticosteroids, severe optic disc edema, disc hemorrhage, macular star, contributory systemic diagnoses (sarcoidosis, rheumatological disorders, immune-compromised state, underlying infection, cancer) and atypical imaging features [5,6].
The diagnosis of the atypical type of optic neuritis for this case is based on the unusual features of the patient including male gender, bilateral involvement of the eyes, and systemic association with HIV as the cause of the inflammation. Optic neuritis occurs more commonly in females in approximately 77% with a ratio of 3:1 as compared to male [5,7]. It is more commonly unilateral and bilateral involvement occurs usually in children with postviral infection [5]. This patient is male, homosexual with multiple sexual partners, which may suggest related infectious cause associated with the development of optic neuritis. In this case, the patient had no other associated clinical manifestation and the HIV antibody was positive. HIV is an important consideration, even in the absence of associated symptoms, in the Philippines given its high number of newly diagnosed HIV cases. According to the latest HIV/AIDS Registry of the Philippines (HARP) report, a total of 840 new HIV cases were reported just in April 2019. Twenty percent had clinical manifestation of advanced HIV at the time of diagnosis. Among new cases, a total of 789 cases (94%) were male. The median age was 27 years old, with more than half of the cases were 25-34 years old, and 29% were 15-24 years old. Almost one third (32%) were from National Capital Region. The predominant mode of transmission is through sexual transmission (98%), mostly from menhaving-sex-with-men, which accounted for 57 percent. Other modes of transmission include needle sharing among injecting drug user (1%) and mother-to-child transmission (less than 1%) [3]. The blurring of vision in HIV in the absence of anterior segment manifestations involves posterior segment structures including the retina, choroid, and optic nerve head. Disorders of at least one of these structures are seen in more than 50% of patients who are HIV positive. Neuroophthalmologic manifestations can be directly due to HIV itself or to secondary causes of HIV like Cryptococcal meningitis, meningeal and parenchymal lymphoma, neurosyphilis and toxoplasmosis [8].
The pathogenesis of optic neuritis is not well understood. It occurs due to inflammatory processes which lead to delayed type IV hypersensitivity reaction induced by released cytokines and other inflammatory mediators from activated peripheral T-cells that can cross the blood-brain barrier and cause hypersensitivity reaction to neuronal structures leading to destruction of myelin, neuronal cell death, and axonal degeneration. Permanent vision loss in 40 to 60% and visual deficit in optic neuritis is a result of axonal loss in the optic nerve and retina and corresponding retinal nerve fiber layer thinning [7].
A direct causal link between HIV and optic neuritis has been suggested previously and may be related to the effects of HIV on the immune system. The pathogenesis of HIV includes replicating itself using host cells, initially being captured by dendritic cells making their way to the lymph nodes and to peripheral blood, where HIV targets CD4+ lymphocytes, a T-cell surface marker [9].
Acierno MD mentioned that there is an association of HIV in the development of optic neuritis, cause directly by HIV itself or through secondary infections as in the case of syphilis or opportunistic organisms such as Cryptococcus, Histoplasma, Herpes Zoster, Toxoplasmosis and Cytomegalovirus [10]. In this case, systemic association with secondary opportunistic infections in HIV was ruled out with no other clinical manifestations. Neurologic examination was unremarkable, and negative for Brudzinski’s sign and nuchal rigidity consistent with the meningeal process, which may suggest other secondary opportunistic infectious diseases in HIV like cryptococcal, tuberculous, Listeria species, lymphomatous etiology, supported by no dural or meningeal enhancement on MRI instead of CSF examination.
There is no well recognized clinical syndrome of optic neuritis specifically caused by HIV. This may be an indirect or direct effect of HIV on optic nerve fibers similar to those seen outside CNS or that HIV infection itself directly contributed to the development of optic neuritis. Evidence suggests that the direct degeneration of ganglion cell axons in the optic nerve can be primarily due to the HIV virus itself, or indirectly with secondary infection or as mediated by HIV-infected macrophages or monocular phagocyte [10]. The current widely accepted theory suggests that the pro-inflammatory cytokine tumor necrosis alpha plays a key role. Other proposed mechanism includes damage secondary to activated microglia and macrophages releasing neurotoxic agents. Consistent with this proposed inflammatory pathogenesis, steroid responsiveness is thought to be a feature of idiopathic optic neuritis in HIV-infected patients [11].
Larsen M, et al. reported a case of the development of optic neuritis in an HIV patient with systemic manifestation in the early course. The acute viral disease and bilateral optic neuritis were caused by acute HIV infection and correlated through positive HIV antibody tests, negative p24 antigen test and the relatively low RNA PCR count [2]. This is similar to this case report with bilateral optic neuritis as the early manifestation of a positive HIV patient but presented with no other associated symptoms.
This case presents a healthy young male patient having no manifestation of HIV and no clinical signs and symptoms pertinent to other atypical causes of optic neuritis such as syphilis, sarcoidosis, systemic lupus erythematosus and vasculitis, Wegener granulomatosis, neuromyelitisoptica, compressive and infiltrative disorders, Lyme disease, Leber hereditary optic neuropathy, meningeal process, and cat scratch disease. Being atypical type of optic neuritis, this patient was reassessed with other possible cause of optic nerve involvement like HIV in this case. The discussion showed that several studies have proposed a direct causal link between HIV and optic nerve involvement, and reported HIV in optic neuritis but presented with other manifestation/s and secondary opportunistic infection/s. As mentioned, there is no well recognized clinical syndrome of optic neuritis specifically caused by HIV, at this point; the causal relationship of optic neuritis with HIV cannot be conclusively ascertained in this case.
This is the importance of this study, that is, to report a case of HIV being presented only and initially with optic nerve involvement. This is important especially in the Philippines considering the widespread cases of HIV infection and in the vast majority of these cases presenting with decreased/loss of vision, in this case, in the early phase of the disease. Thus, this study suggests high suspicion in a patient presenting with atypical optic neuritis to include HIV-1 infection as a differential diagnosis or an etiology pointing to this assessment and in need of further evaluation and management.
The limitation of this study is due to the lack of confirmatory evidence with other requested laboratories including the lumbar tap refused to be done by the patient. This is also in consideration with no other associated clinical findings and financial constraints of the patient.
The patient was also lost to follow up for four months, within which, no other intervention was done. Despite these, however, he still has no other clinical manifestations and already started with HIV treatment. It is most importantly noted that, at this time, the patient is contented and comfortable with his improvement of vision.
All cases of atypical optic neuritis should be suspected to have underlying HIV infection. Optic neuritis may be the initial and only manifestation in an HIV patient. This case reports a case of optic neuritis with no other clinical manifestation in HIV, which is alarming in the Philippines given a dramatic increase in the number of HIV patients. Studies have proposed a direct causal link between HIV and optic nerve involvement, and showed reports of HIV in optic neuritis but presenting with other manifestation/s and/or secondary opportunistic infection/s. As mentioned, there is no well recognized clinical syndrome of optic nerve involvement specifically caused by HIV. At this point, the causal relationship of optic neuritis with HIV cannot be conclusively ascertained in this case. Thus, this also suggests future researchers investigate HIV manifesting only as optic neuritis, and further studies to ascertain optic neuritis being manifested in HIV. Despite this, however, given this case, there should be investigation for HIV in atypical cases of optic neuritis among high risk and suspected individuals.
This case report is consented by the patient, who is informed and advised, and who fully understood the study with only verbal consent. The identity of the patient is not revealed in this report. The study is approved by the Institutional Review Board in the institution.
The diagnostics suggested and management are based on the clinical case and literature including evidence-based studies. Those procedures or requested laboratories refused by the patient are not done.
The intervention is focused on the treatment of the patient with more benefits considered than harm, and not on the interest of the study itself.
Download Provisional PDF Here
Article Type: CASE REPORT
Citation: San Diego MCV, Palisoc ED (2019) Atypical Optic Neuritis in HIV: A Case Report. J Ophthalmic Stud 2(2): dx.doi.org/10.16966/2639- 152X.115
Copyright: © 2019 San Diego MCV, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access