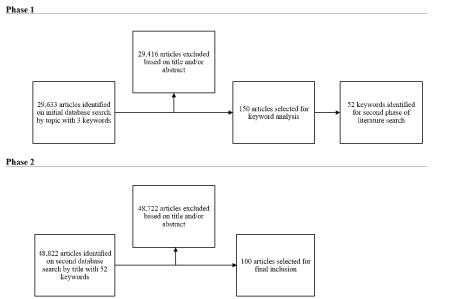
Figure 1: Literature search strategy.

Jennifer L Perez1* Ahmed Kashkoush1 Tejas Karnat2 James Zhou3 Nitin Agarwal1 D Kojo Hamilton1
1Department of Neurological Surgery, University of Pittsburgh Medical Center, Pittsburgh, USA*Corresponding author: Jennifer L Perez, Department of Neurological Surgery, University of Pittsburgh Medical Center, 200 Lothrop Street, Suite B-400 Pittsburgh, USA, Tel: 908-531-1947, Fax: 412-647-0989, E-mail: jlp232@pitt.edu
In order to identify the top one hundred most influential articles in acute ischemic stroke research, we applied a well-established technique of citation analysis to relevant research published between 1988 and 2015. Numerous studies have applied the technique of citation analysis to other fields. However, this is the first paper to apply such a technique in the field of acute ischemic stroke. Using Thomson Reuters Web of Science, a two-step search strategy was conducted to identify publications relevant to the field of acute ischemic stroke. After a thorough analysis of titles and abstracts, a top 100 list of publications was constructed. Various supplementary statistical analyses were conducted to explore the association between author reputation or overall publication influence, and the rate at which publications were recognized and incorporated by other researchers in the field. A list of the top 100 articles in acute ischemic stroke from 1988-2015 was identified and further divided into 7 subcategories. Werner Hacke was the most published first author in this analysis. He and the top 10 most published first authors had publications mainly focused on treatment. The article, “Tissue Plasminogen Activator for Acute Ischemic Stroke” from 1995 was the most cited. Finally, we found no correlation between average citations per year and time to first citation. We demonstrate the utility of a two-phase citation analysis technique in the identification and accumulation the top one hundred most influential publications in acute ischemic stroke from 1988 to 2015.
Ischemic Stroke; Influential; Citation Analysis; Bibliometric Study
There have been many important historical developments in the field of acute ischemic stroke. The current body of literature on the subject is the product of dedicated researchers who spent substantial parts of their academic careers to establishing, expanding, and advancing the field. However, due to the exponential growth of scientific output from 1980 to 2012, many of their valuable contributions may be lost as new articles continue to be published at a rapid rate. A robust framework is necessary to facilitate the identification and accumulation of the most valuable data and to recognize the researchers for the impact of their contributions. Citation analysis is a technique that has been utilized to identify the most impactful publications in various subjects including intracranial aneurysms [1], spinal tumors [2], scoliosis [3] and epilepsy [4]. Using this technique, articles in a particular field were ranked by their relative levels of impact on the scientific community. Such citation analyses are also known as bibliometric studies, and have recently established them as an innovative way to identify impactful publications pertaining to various fields of study [1-4]. We have conducted a citation analysis using the Thomson Reuters Web of Science in order to identify and analyze the top hundred most influential articles published in any journal during the period from 1988 to 2015 that significantly impacted the field of acute ischemic stroke.
Specific inclusion criteria were predetermined in order for studies to be included in the final list of the top hundred publications. First, only studies written in English were considered and the predominant focus of the paper needed to be about acute ischemic stroke. Studies discussing all aspects of pathophysiology, evaluation, treatment, management, or natural history and closely related topics were included; but those that focused on chronic stroke or biochemical etiologies or effects on other organ systems were excluded. Studies dealing with other diseases, such as myocardial infarction or traumatic brain injury, in addition to acute ischemic stroke were excluded. All databases and journals included within the Thomson Reuter’s Web of Science were used to construct the list of eligible studies.
In June 2016, a query from the Web of Science Core Collection of the Thomson Reuters Web of Science was conducted in a twophase approach (Figure 1). In the first phase, a topic search of the Web of Sciences database was conducted with the following query: (acute) and (ischemic) and (stroke). This query yielded 29,633 results, which were then sorted in descending order by the total number of citations. Within the first 217 studies, 150 papers involving topics on “acute ischemic stroke” research met the inclusion criteria based on a thorough review of both the titles and abstracts. Subsequently, each paper was rigorously analyzed to create a list of keywords for the second phase of data collection. Fifty-two keywords were extracted from the initial 150 articles (Table 1). These 52 keywords were then used to query the database a second time. The exact search term is shown in table 1. This second phase of the search yielded 48,722 articles, which were sorted in descending order by number of citations. Within the first 370 studies, the top 100 with most citations were selected in accordance with the inclusion criteria for final inclusion in this paper. Two authors (AK and TK) conducted the initial review-any articles that were in question were passed on to the primary author (JP) for further clarification. All final articles were analyzed and approved by the senior authors. For every study that was selected for inclusion in the top 100 list, the following pieces of information were extracted: title, authors, year of publication, year of first citation, year of peak citations, total number of times cited (through 2016), and number of times cited in 2015. Using this information, we were then able to calculate the average number of citations/year and the number of years until peak citation.
All extracted publications were classified by topic and study design. Topics included pathophysiology/risk factor for disease, epidemiology/ public health, treatment (anticoagulation, thrombolytics, or procedural), and evaluation (including clinical classification and diagnostics). Study designs were assigned as interventional trial, meta-analysis, guidelines, observational, experimental (animal studies), and literature reviews. The average citation count per year (annual citation rate) was utilized to standardize article recognition as papers monotonically accumulate citations with increasing time from publication. Annual citation rates were compared across topics and study design groups utilizing a Kruskal-wallis test. Individual groups were compared using a Bonferroni post-hoc analysis, with correction for multiple comparisons. Statistical significance was adjusted accordingly (p=0.05/n), where n is the number of comparisons being evaluated [5].
There were 48,722 articles that matched the second phase search criteria, and 100 were included in the final list based on review of titles, abstracts, and the entire text of the publication in selected instances when additional clarification was needed. Any article that did not discuss or directly mention “acute ischemic stroke” after the second phase of the search and subsequent ranking in descending order of citations was not included in the top 100 list of papers. Therefore, we went through 370 articles to yield a list of 100 articles. The top 10 most cited articles in acute ischemic stroke from 1988-2015 were compiled in table 2, along with additional statistical information concerning each publication’s citations over time. This information includes the number of years from publication until the most cited year, the number of times each article was cited in 2015, and the total number of citations (through 2015, 2016). The final list of top 100 articles is listed in supplementary table 1 and 2 shows the ranking of journals from the list of 100 articles in descending order of the number of publications that were included in the final list. Stroke had the most articles published with a total of 35. The next most represented journal was The New England Journal of Medicine with 13 published articles. The third most represented journal was Lancet with 10 articles, followed by The Journal of the American Medical Association with 7 articles. Supplementary table 3 lists all first authors with more than one publication from the final list of hundred studies along with their associated topics of publication. Werner Hacke had the most publications of all the first authors with a total of 6 and all his articles dealt with treatment. Harold Adams ranked second with 4 publications, which dealt with the evaluation and treatment of acute stroke. The most cited article was by the NINDS (National Institute of Neurological Disorders and Stroke) rt-PA Stroke Study Group [6], which was cited 5285 times (average 53 citations/year). The oldest article was published in 1988 by Gelmers et al. [7]. The three most recent articles were all published in 2015 by Goyal et al. [8], Saver et al. [9], and Jovin et al. [10] respectively.
| ((acute AND ((ischem*) OR (non-hemorrhagic)) AND ((stroke) OR (cerebrovascular accident) OR (infarc*))) AND (manage* OR treat* OR thromb* OR microbubble* OR plasminogen OR therap* OR tPA OR “tPA” OR rtPA OR ultraso* OR transcranial OR recanalization OR oxide OR nitr* OR embolectomy OR reperfusion OR angio* OR desmoteplase OR prourokinase OR urokinase OR alteplase OR metalloproteinase OR “interleukin-1” OR urokinase OR minocycline OR nimodipine OR “s100” OR streptokinase OR gavestinel OR coil OR stent OR aspiration OR outcome* OR complicat* OR analy* OR decompens* OR deficit* OR mortality OR intracranial OR sten* OR rankin OR barthel OR hyperthermia OR casuality OR intracerebral OR resolution)) |
Table 1: Search strategy for second phase of literature search.
| Rank | Publication | Years until most cited year | Annual citation rate | Number of Citations in 2015 |
Total Citations through June 2016 |
| 1 | Tissue plasminogen activator for acute ischemic stroke. The National Institute of Neurological Disorders and Stroke rt-PA Stroke Study Group. N Engl J Med. 1995;333(24):1581-7. | 14 | 240 | 14 | 5285 |
| 2 | Adams HP, Bendixen BH, Kappelle LJ, et al. Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke. 1993;24 (1):35-41. | 20 | 154 | 256 | 3707 |
| 3 | Hacke W, Kaste M, Bluhmki E, et al. Thrombolysis with alteplase 3 to 4.5 hours after acute ischemic stroke. N Engl J Med. 2008;359 (13):1317-29. | 4 | 251 | 351 | 2260 |
| 4 | Hacke W, Kaste M, Fieschi C, et al. Intravenous thrombolysis with recombinant tissue plasminogen activator for acute hemispheric stroke. The European Cooperative Acute Stroke Study (ECASS). JAMA. 1995;274 (13):1017-25. | 4 | 91 | 71 | 2005 |
| 5 | Furlan A, Higashida R, Wechsler L, et al. Intra-arterial prourokinase for acute ischemic stroke. The PROACT II study: a randomized controlled trial. Prolyse in Acute Cerebral Thromboembolism. JAMA. 1999;282 (21):2003-11. | 10 | 106 | 110 | 1904 |
| 6 | Hacke W, Kaste M, Fieschi C, et al. Randomised double- blind placebo-controlled trial of thrombolytic therapy with intravenous alteplase in acute ischaemic stroke (ECASS II). Second European-Australasian Acute Stroke Study Investigators. Lancet. 1998;352 (9136):1245-51. | 17 | 83 | 123 | 1570 |
| 7 | Hacke W, Donnan G, Fieschi C, et al. Association of outcome with early stroke treatment: pooled analysis of ATLANTIS, ECASS, and NINDS rt-PA stroke trials. Lancet. 2004;363 (9411):768-74. | 5 | 106 | 90 | 1372 |
| 8 | Adams HP, Del zoppo G, Alberts MJ, et al. Guidelines for the early management of adults with ischemic stroke: a guideline from the American Heart Association/American Stroke Association Stroke Council, Clinical Cardiology Council, Cardiovascular Radiology and Intervention Council, and the Atherosclerotic Peripheral Vascular Disease and Quality of Care Outcomes in Research Interdisciplinary Working Groups: The American Academy of Neurology affirms the value of this guideline as an educational tool for neurologists. Circulation. 2007;115 (20):e478-534. | 4 | 133 | 94 | 1334 |
| 9 | The International Stroke Trial (IST): a randomised trial of aspirin, subcutaneous heparin, both, or neither among 19435 patients with acute ischaemic stroke. International Stroke Trial Collaborative Group. Lancet. 1997;349 (9065):1569-81. | 3 | 53 | 41 | 1052 |
| 10 | Jauch EC, Saver JL, Adams HP, et al. Guidelines for the early management of patients with acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2013;44 (3):870-947. | 2 | 74 | 446 | 1037 |
Table 2: The top 10 most cited articles in acute ischemic stroke research.
Figure 2A shows the number of publications per year, while figure 2B shows the publications in each topic category per year. Both figures demonstrate that the number of published articles had a peak from 1998 to 2000 only to decline thereafter. The predominant topic discussed throughout was treatment during acute stroke. Thrombolysis was discussed primarily in the 1990s. Non-thrombolytic therapy was discussed in articles predominantly published in the early 2000s.
In figure 3, we have categorized the top hundred articles into one of seven categories: epidemiology, treatment (anticoagulation, thrombolytics, or procedural), evaluation, and pathophysiology/risk factors. The acute therapy (all modes) category was devised to include published articles that discussed anticoagulation (such as aspirin and heparin), thrombolytic therapy, and procedural intervention (such as thrombectomy and hemicraniectomy). The most popular category was acute therapy (all modes) with 63 articles. The second most popular was thrombolysis with 28 publications. A Kruskal-Wallis test demonstrated that the median annual citation rate across all groups was significantly different (p=0.012). In particular, publications regarding procedural intervention were more likely to be cited at a higher rate than those in the evaluation group (p=0.016, Bonferroni post-hoc analysis). Figure 4 demonstrates the distributions of annual citation rate across study designs. Our data indicated that interventional trials were cited at a higher rate than other study designs (p=0.004, Bonferroni posthoc analysis).

Figure 1: Literature search strategy.
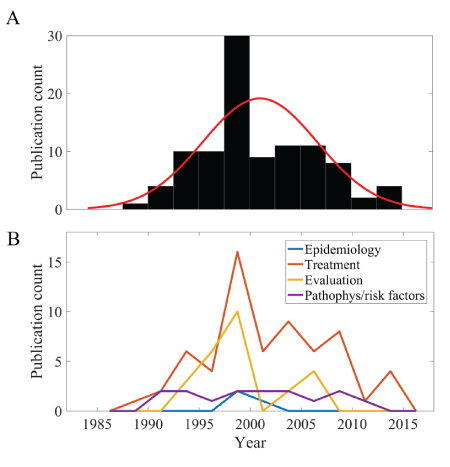
Figure 2: (A) Publication count by year with approximated normal distribution overlaid for all research topics.
(B) Publication count per year by research topic.
The correlation between “average citations per year since publication” and “the number of years until peak citations” is outlined in supplementary table 3. Our data suggested that the rate at which a particular publication is first recognized has very little bearing on how widely it is cited by other researchers in the field. In supplementary figure 1 and 2, we showed the number of citations per year for the top 5 most cited publications: NINDS [6]; Adams et al. [11]; Hacke et al. [12], Hacke et al. [13], and Furlan et al. [14]. The oldest of the top 5 most cited articles, by Hacke et al. [13] had an initial peak in citations in the late 1990s and another, smaller peak in early 2010s. The publication by the NINDS rt-PA Stroke Study group was consistently cited from the late 1990s to the 2010s. Hacke et al. [12] had a citation peak between 2011 and 2013, Furlan et al. [14] had a citation peak between 2005 and 2009, and Adams et al. peaked in 2012.
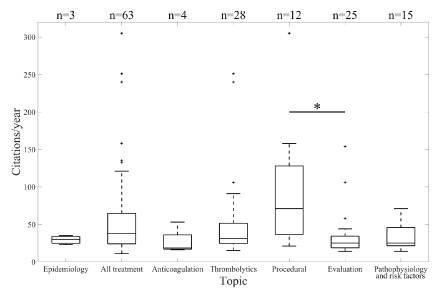
Figure 3: Citations/year by research topic. Annual citation rate statistically different between ‘Procedural’ and ‘Evaluation’ groups (p=0.016, Bonferroni post-hoc analysis). All differences between each of other groups were non-significant. Asterisk (*) denotes significant difference. Plus-signs (+) denote outliers in the data within each group.
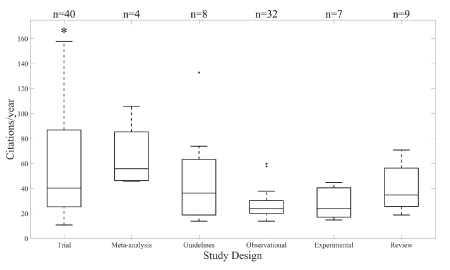
Figure 4: Citations/year by research topic. Annual citation rate statistically different between ‘Trial’ and all other groups combined (p=0.0036, Bonferroni post-hoc analysis). Annual citation rate >300 citations/year not shown. Asterisk (*) denotes significant difference. Plus-signs (+) denote outliers in the data within each group.
In putting together this list of the top hundred most cited publications in the field of acute ischemic stroke, we aimed to identify and recognize the researchers who have had the most impact to the field of acute ischemic stroke in the past century. We believe the results of this bibliometric study will not only rightfully recognize the tremendous scholarship of important, impactful researchers, but also highlight and catalog the rich developmental history of the field of acute ischemic stroke.
The oldest article in the final list was “A Controlled Trial of Nimodipine in Acute Ischemic Stroke,” which was published in 1988. At the time, studies suggested that increased cellular calcium concentrations accumulated in neurons that incurred ischemic damage [15]. In a prospective, double-blind, randomized, placebo-controlled trial, the authors used nimodipine, a calcium-channel blocker, during a four-week treatment period and found that all-cause mortality was significantly reduced with nimodipine as compared with placebo (8.6% vs 20.4%). The nimodipine group also saw a significantly better neurologic outcome according to the Mathew scale. Interestingly, the improvement in survival was restricted to men. In short, the data indicated that patients with acute ischemic stroke may have benefited from early treatment with nimodipine. However, this is no longer used as a standard treatment for acute ischemic stroke. The most cited article in the final list was “Tissue Plasminogen Activator for Acute Ischemic Stroke” by Brott et al. [6], which was a randomized, double-blinded trial of intravenous recombinant tissue plasminogen activator (t-PA). The trial consisted of two parts; in part 1, the researchers found no significant difference between the t-PA group and the placebo group when assessed for neurologic improvement at 24 hours but did find a significant benefit for the t-PA group at three months for all four of the following outcome measures: Barthel index, modified Rankin scale, Glasgow outcome scale, and NIHSS. However, they found an increased incidence of symptomatic intracerebral hemorrhage in the t-PA group, but concluded that treatment with IV t-PA within 3 hours of the onset of ischemic stroke improved clinical outcome at 3 months. In 2015, the American Heart Association/American Stroke Association updated its thrombolytic inclusion and exclusion criteria to reflect a 4.5hour window for t-PA administration in selected patients following a 2014 meta-analysis [12,16,17].
The two most studied topics were thrombolytic therapy and non-thrombolytic therapy. We found 25 publications devoted to thrombolytic therapy and 14 publications devoted to nonthrombolytic therapy. Both these topics fall under a broader category of “acute therapy (all modes)” which include both thrombolytic, non-thrombolytic, and other acute therapies such as embolectomy or thrombectomy which undoubtedly made up the bulk of the top 100 publications at 42 total publications. Publications concerned with thrombolytic therapy discussed interventions such as t-PA, intraarterial urokinase, and desmoteplase. In the current study, we also found no correlation between average citations per year and time to first citation. We determined that in the field of acute ischemic stroke, more influential articles did not necessarily have a shorter amount of time before initial and peak recognition by the scientific community in terms of being cited by other studies in the same field. The two-phase search process used to assemble the final list of the top one hundred acute ischemic stroke articles (Figure 1, Table 1) was previously conducted in a similar manner, and was shown to be a robust approach of citation analysis [1,3]. By choosing the top 150 articles in accordance with our inclusion criteria in the first phase, subsequently extracting keywords, and starting a second-phase search allowed us to focus on acute ischemic stroke related articles with more precision (as evidenced by our article yield diminishing from 29,633 to 16,759 from the first to the second-phase search results).
There were several limitations to our technique of citation analysis. First, the number of citations an article received may contain certain biases including self-citations and negative citations. Further, inherent bias from the authors of this manuscript in identifying keywords may exist. Finally, it is possible that newer publications may be too recent to have a consequent total number of citations by the 2016 cutoff. As the field continues to evolve, further analysis on influential publications may be warranted. Despite these limitations, we believe our twophase search process allowed us to identify and delineate the top one hundred most influential articles in acute ischemic stroke research.
Our two-phase citation analysis technique provides a robust framework to facilitate the identification and accumulation of the most valuable data in the field of acute ischemic stroke, and to recognize the researchers for the impact of their contributions. The predominance of treatment focused publications can be used to identify the trends in therapeutic strategies for acute ischemic stroke, and to help elucidate areas where high quality research studies are needed.
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Download Provisional PDF Here
Article Type: REVIEW ARTICLE
Citation: Perez JL, Kashkoush A, Karnati T, Zhou J, Agarwal N, et al. (2018) The 100 Most Influential Publications in Acute Ischemic Stroke. J Neurol Neurobiol 4(3): dx.doi.org/10.16966/2379-7150.153
Copyright: © 2018 Perez JL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access