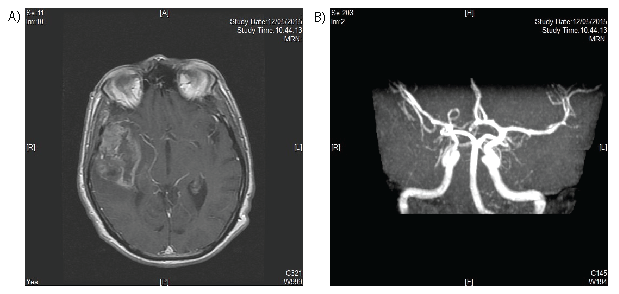
Figure 1: (A,B) Pre-op post contrast MRI (axial seed angio MRI).

Spallone A1,2* Lavorato L1 Di Capua M1
1Department of Clinical Neurosciences-Section of Neurosurgery, NCL (Neurological Centre of Latium) - Neuromed, Rome, Italy*Corresponding author: Spallone A, Department of Clinical Neurosciences-Section of Neurosurgery, NCL-Neurological Centre of Latium, Rome, Italy, Tel: 06763741; E-mail: segreteria1@nclroma.it
The occurrence of post-operative stroke following surgery for brain glioma is a rare complication as a rule related to intraoperative technical difficulties leading to significant vessel occlusion. Ischemic stroke occurring relatively late following an apparently uncomplicated surgery for cerebral glioma is an extremely rare event. We report here a case of a 64-yers-old man who developed a stroke two weeks following an apparently uncomplicated, though technically demanding, gross total removal of a deep temporal glioma and discuss the possible implications of this, though extremely rare, pathological event.
Glioma; Surgery; Stroke; Ischemic
The occurrence of post-operative stroke following surgery for brain glioma is a rare complication as a rule related to intraoperative technical difficulties leading to significant vessel occlusion [1]. Postoperative stroke has a negative impact on quality of life following surgery and may affect negatively postoperative survival of glioma-bearing patients.
Ischemic stroke occurring relatively late following an apparently uncomplicated surgery for cerebral glioma is an extremely rare event: 20 out of 6500 cases (0.03%) in a large cases series from a single Institution reported very recently [2]. We report here a case of a 64-yers-old man who developed a stroke two weeks following an apparently uncomplicated, though technically demanding, gross total removal of a deep temporal glioma.
A 64-years-old right-handed man was admitted in May 2015 with a diagnosis of intracerebral right temporal lesion detected by CTscan (Computerized Tomography Scan). General examination was unremarkable. The patient was a long-time smoker under treatment for mild arterial hypertension. No other risk factors for vascular diseases were encountered. Post-contrast MRI (Magnetic Resonance Imaging) completed with MRI angiography demonstrated an irregularly enhancing round temporo-insular lesion which dislocated superiorly to the right the M2-M3 branches of the right middle cerebral artery (MCA) (Figure 1).

Figure 1: (A,B) Pre-op post contrast MRI (axial seed angio MRI).
The patient underwent an awake gross-total resection of the mass two days after his admission. Surgery was uneventful although the removal of the deepest portion of the tumor had required careful dissection under high magnification from some tightly adherent M3 branches, which were carefully respected. The patient exhibited a slight motor weakness of the left extremities which did not prevent him from walking a few hours following surgery and disappeared a few days later. Postoperative CT-scan (Figure 2) showed some contrast enhancement at the deep periphery of the surgical cavity which was interpreted as possible tumor residual, in spite of the intraoperative impression of gross total removal. Post-contrast MRI performed on the following day showed total removal of the lesion (Figure 3). Post-operative steroid therapy was tapered gradually and the patient was discharged on post-operative day 6th.
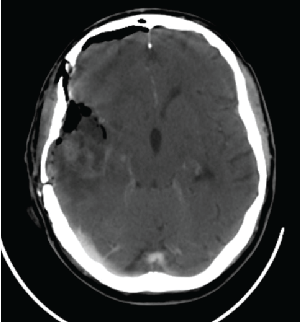
Figure 2: Post-op post contrast CT.
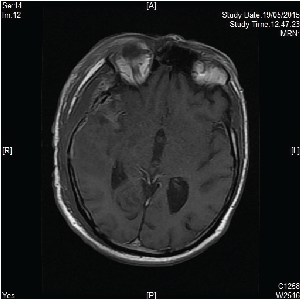
Figure 3: Post-op post contrast MRI (T1 axial)
15 days later he was readmitted on an emergency basis due to sudden occurrence of a left hemiparesis. Emergency CT-scan showed only local swelling. MRI demonstrated early ischemia in the right MCA territory and Angio-MRI showed some possible spasm of the supraclinoid ICA (Internal Carotid Artery) with MCA occlusion at its bifurcation (Figure 4).
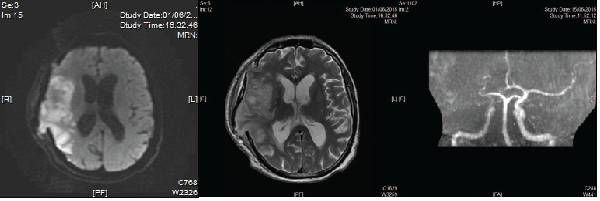
Figure 4: MRI and Angio-MRI (DWI and Angio axial).
In the following days there was a slight improvement of his dense hemiparesis, and the patient was referred elsewhere for possible radiotherapeutic treatment. While waiting for this he developed a significant CSF (Cerebrospinal Fluid) accumulation at the surgical site, which did not respond to local treatment and required implantation of a uni-shunt valve, after which the flap swelling resolved. He was then admitted to an oncological department for post-operative radio- and chemotherapy, which was initiated but soon thereafter interrupted due to supervening pneumonia. This was treated with an initial success, but recurred later and ultimately led to his death, four month following surgery, three month and a half after the stroke. The last CT-scan still did not show residual tumor (Figure 5). The patient underwent surgery of brain glioma resection according to the operating standards. Radiological examinations were subsequently performed with CT scan and MRI (1.5T).

Figure 5: Post contrast CT showing no tumor recurrence.
Stroke following glioma surgery has a negative impact on the quality of life and ultimately on survival following surgery for brain glioma, although post-operative survival did not seem to be highly correlated to stroke occurring after surgery in a large, recently published case material [2].
Post-operative stroke is usually considered the result of a technical failure during surgery. Stroke occurring late (two to three weeks) after glioma surgery, and involving the same vascular territory, is an extremely rare event (0.03%) [2], rather difficult to explain. A careful review of the relevant literature did not found more than 7 papers devoted to the impact of glioma surgery on the local cerebral arterial network with clinical consequences [1-7].
Post-operative vasospasm was detected in a significant proportion of patients following glioma surgery (23-48%) [2,4,5] and was implicated in the late occurrence of post-operative stroke in one thoughtfully described case [3]. This might suggest caution in performing long dissection and aggressive tumor removal in cases of deep glioma either encasing or tightly adhering to significant arterial branches.
In the present patient removal of the deepest portion of the lesion required careful microdissection of some M3 branches to which the tumor was tightly adherent. Early postoperative CT-scan control showed some local enhancement which was initially interpreted as a tumor residual (in spite of the intraoperative impression of gross total removal) whilst MRI control performed on the next day confirmed the intraoperative impression of total removal. We attributed this discrepancy to the technological superiority of the MRI. We wonder now if the post-contrast enhancement shown by the early CT central could not be explained rather as the “contrast leakage” phenomenon which can be observed in cases of severe vasospasm following SAH (Subarachnoid Hemorrhage).
Postoperative course was rather uneventful. Two weeks later the patient was readmitted with an ipsilateral MCA-occlusion related stroke. Post-stroke clinical course was never benign, and the patient died due to supervening respiratory complications four months after surgery without showing signs of tumor recurrence. No significant vascular risk factor was identified, apart from the patient to be smoker. We wonder if vasospasm could have been a significant factor in the development of MCA occlusion, and the prolonged dissection close to significant arterial branches would have promoted such a phenomenon, although these vessels appear to be well patent following surgery, and were rather distant from the site of the MCA occlusion. Stroke involved the same vascular territory, and this suggests the existence of a causal relationship between tumor removal and later occurring stroke. If a surgical trauma to a vessel leading to its occlusion is excluded, as it was in the present case, vasospasm and its retrograde spreading toward the main branches could be a sound explanation. This, as also suggested by others [1,7], could represent a warning against the attempt to achieve total tumor removal in the presence of either significant vessel encasement or tight vessels adherences to tumor boundaries. On the other hand, leaving tumor remnants, particularly in high-grade gliomas, represents “per se” a significant risk in terms of possible postoperative hemorrhage and/or brain swelling, and this means that an appropriate surgical strategy is left to the wise judgment and the experience of the operating surgeon, who should have in mind that manipulating vessels during the removal of a deep-seated glioma is risky; and even if the vessels remain patent at the end of surgery a stroke could occur later, although in extremely rare circumstances.
We did not use any preventive measures against postoperative vasospasm in the present patient. If we would assume that vasospasm would play a role in the later occurrence of stroke, postoperative preventive use of well-known pharmacological preventive measures as nimodipine and for similar drugs should be considered, although the extreme rarity of this pathological condition does not seem to allow definitive conclusions on the specific topic.
In conclusion the role of postoperative vasospasm in the late occurrence of stroke following glioma surgery, although likely, remains speculative.
Download Provisional PDF Here
Article Type: Case Report
Citation: Spallone A, Lavorato L, Di Capua M (2016) Lately-Occurring Stroke following Glioma Surgery: Report of a Case and Review of the Literature. J Neurol Neurobiol 3(1): doi http://dx.doi. org/10.16966/2379-7150.134
Copyright: © 2016 Spallone A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access