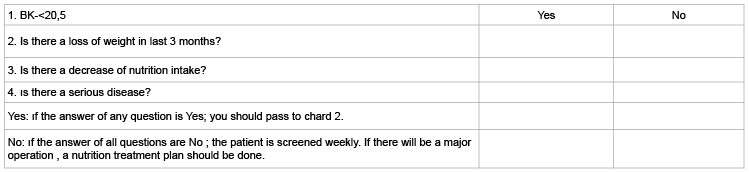
Table 1: NRS -2002 (Nutritional Risk Screening)
Lale Akkaya*1 Can Hüzmeli2 Ferhan Candan3 Naim Nur4 Mansur Kayataş3
1Cumhuriyet University Peritoneal Dialysis nurse, Sivas, Turkey*Corresponding author: Lale Akkaya, Cumhuriyet University Peritoneal Dialysis Nurse, Sivas, Turkey, E-mail: laleber@hotmail.com
Introduction: Malnutrition is seen much morein the peritoneal dialysis patients . Because, Periton Dialysis causes much more loss of body proteins than hemodialysis. Osteoporosis which is a kind of bone interraction seen in chronic renal failure is a long term complication and also it is the result ofthe deformation of bone structre.
Objective: Our aim in this survey is to view the osteoporosis conditions of dialysis patients whohave malnutrition on thecontinous peritoneal dialysis ( CAPD) or not. At the same time, we aimed to find solutions for prevention of the complications that can ocur in these patients.
Material and method: Our subjets are 27 patients who are being observed at Cumhuriyet University Faculty of Medicine Nefrology Department Periton Dialysis Unit.Malnutrition of patients were identified by NRS-2002 valuation questionaire. Patients were divided into two groups the ones who have mulnutrition and the ones who don’t. The scale of bone mineral density, Malnutrition situations and biochemical parameters of patients were obtained. Malnutrition was identified in 14 of (51,8%) 27 patients. Bone mineral density measurements were low in the patients who had malnutrition. A significant relationship between malnutrition andfemur dexa values were observed. ( p<0,05). Serum CRP levels were high in the group of malnutrition.
Conclusion: It is found out that the bone mineral density levels were low for malnutrition patients. So, they should be regularly under consideration for nutrition and osteoporosis.
Malnutrition; Peritoneal dialysis; Osteoporosis
Osteoporosis is defined as the deformation of the microstructure of bone cambium. As a result of this, there occurs a probability of fragment. İt can be diagnosed only by way of bone biopsy. However many patients do not accept this and bone mineral density levels are considered for diagnosis. Secondary hyperparathyroidism, osteomalacia and adynamic bone disease have important role in the etiology of bone disease seen in end stage renal failure. The bone mineral density is an important parameter for objective evaluation of the systematic diseases like osteoporosis . The dual energy x ray absorbsiometry ( DEXA) methods are used to measure the bone mineral density.
Lack of protein and energy in the body is called as malnutrition or protein energy malnutrition. Malnutrition is frequently seen among the dialysis patients. Malnutrition prevelance is seen in dialysis populations is different percentages.( 18-76%) [1-2]. The evaluation of nutrition of dialysis patients can be investigated by the way of biochemical parameters, the speed of protein cathabolism, antropometrical measurements and body composition. And also subjective global evaluation can be used to evaluate malnutrition of the end stage renal failure [3]. Nutritional screening and evaluation: ıt is important to evaluate the nutrition for acute and chronic malnutrition diagnosis in the peritoneal dialysis patients.
The target of this study is to define the level of malnutrition of the patients that were under the treatment of CAPD. Besides, to determine the account of osteoporosis by way of measuring bone mineral density with DEXA method and searching the relationship between the osteoporosis and malnutrition. We aimed to find solutions in preventing the complications of related with osteoporosis.
Our subjects are 27 patients being observed at Cumhuriye Unıversity, Faculty of Medicine Nefrology Department Periton Dialysis Unit (14 female and 13 male). Patients were divided into two groups who have malnutrition and who do not. They were applied personal information forms to identify their socio-demographic clinical features. Their calcium, phosphorus, , blood urine nitrogen, creatine, potassium, albumin,hemoglobin, hematocrite, parathyroid hormone, C-reactive protein (CRP), Kt/v, body mass index and vitamin D levels were determined. For mesuring the bone mineral density, DEXA was applied totheir forearm and femur neck. Patients malnutrition conditions were defined by way of NRS 2002 inquires. Patients who had cancer or who did not have periton dialysis less than 3 months were not included to the survey. According to the World Health organizationcriterions: bone structure T score ≤ 2,5 osteoporosis, T score -2,5-1 osteopeny, T score >1 is considering as normal [4], we evaluated our patients accordng to these criterions.
There are many kinds of guides to identify the malnutrition. For example: subjective Global Evaluation, mini-nutritional evaluation, and NRS 2002 questionnaire. Nowadays NRS 2002 is the most wide spread one, for ESPEN ( European Society of Parenteral and Enteral Nutrition) NRS 2002 , and for old patients the Mini Nutritional Evaluation is adviced. With NRS 2002 patients were evaluated in insufficient nutrition and severity of disease and were scored like below: no (0) insignificant ( 1) avarage (2) and serious (3). Patients with total score ≥ 3 were evaluated as under the nutrition risk [5]. At first , NRS 2002 nutritional screening form was filled (Table 1). If the answers are no, forms have to be filled weekly again. If the answer of any question is yes, then the last screenings have to be done (Table 2).
Data of the survey was evaluated with SPSS 15.0 programme. Percentage and avarage calculations and Mann-Withney U tests were used to evaluate the data.
The avarage ages of the patients were found as 45,6 ± 12. Patients were divided into two groups, the ones with malnutrition (1 male, 13 female) avarage ages of these were 48,3 ± 10,3 years old; dialysis period 55, 6 ± 29,2months; the other ones without malnutrition( 6 male, 7 female) avarage ages 42,6 ± 13,5 years, dialysis period 39 ± 29,7 months.
The relationship between the two groups demographic and biochemical parameters of the patients (Table 3). Any difference between two groups were not identified according to age, gender, dialysis periods, calcium, phosphorus, blood urine nitrogen, creatine, hematocrite, parathyroid hormone, kt/v, body mass index, forearm dexavalues and 25 (OH) vitamin D levels (p<0,05). 14 of 27 patients in our survey ( 51,8%) had malnutrition.10 of the 14 patients with malnutrition were identified having osteopenia, and 4 of them osteoporosis. 3 of 13 patients who do not have mulnutrition were identified osteopenia, and 4 of them osteoporosis.A significant relationship was found between malnutrition and dexa measurements in the both groups (p<0,05).29,6% of SAPD patients were detected osteoporosis and 48,1% osteopenia.
There are a lots of risk factors for the osteoporosis development of patients with chronic renal failure. These are female gender, over aging, decreased calcium intake, secondary hyperparathyroidism, low vitamin D, long term steroid usage, sedentary life and some genetic factors. And also low bone mineral density is known a risk factor for bone fracture [6]. The patients with long term renal failure bone mineral density is detected lowerthan normal healthy population measurements. Patients withthe longer period on the peritoneal dialysis treatment has lower bone mineral density [7].
The Baszko-blaszyk and et al. were found the osteoporosis prevalence of 48,6% and 21,6% in lumbar vertebrae and femoral neck, respectively [8]. Doğukan and et al. showed that periton dialysis patients, osteoporosis prevalence in lumbar vertebra of 25,7%, femoral neck of 28,6% [9]. Ersoy et al. declared that the osteoporosis frequency is 19,2% and 26%. The percentage of 56% patients was osteopenic [10]. Our study detected that 29,6% of CAPD patients have the osteoporosis and 48,1% of them arethe osteopenic.
Loss of protein and energy is important for chronic peritoneal dialysis patients and ıt hasthe negative prognostic factor for morbidity and mortality [11]. Thus, it is important to define the nutrition disorders in time and to treat rightly in the end stage renal disease patients. Especially, because of the protein loss during the periton dialysis, these patients should be checked regularly for malnutrition and osteoporosis. Serum albumin level is a strong evedince of the surviveal of these patients.
In a few survey, It has been detected a negative correlation between the serum albuminin concentration and mortality in hemodialysis and peritoneal dialysis patients [12,13]. The low level of serum albumin is detected as 28% in chronic periton dialysis patients in Turkey [14]. In our study, the low level ofserum albumin was found as 77,7% (<3.5 g/dl). It was higher than other researches [15].
In the five years survey which was carried on by Teenhan and his friends, the serum albuminin level 3,5 g/dl and over in chronicperitoneal dialysis patients, the living expectation was found over 50 months. It was seen that the patients whose albuminin level is lower, lost their lifes with in 40 months.
Although the serum albuminin level differs in both inflammation and malnutrition situations, it was agreed that the albuminin can be used as a strong evidence of nutrition even there was inflammation [15,16].
Inflammation plays an important role on malnutrition development of dialysis patients. While with the inflammation, the negative acute phase reactans are decreasing, possitive phase reactans and cytokines increase. Inflammation results with protein catabolism, lipolysis and anorexia. Also, obesity contributes to the inflamation in the chronic renal failure [17,18].
Especially the glucose which is used as osmotic substance for periton dialysis solutions is a responsible for obesity. It is not certain but the surveys attract attention to the fact that increased inflammation indicators hasten the protein waste. In the animal experiments ıt is shown that IL-1, IL-2, IL- 6 and TNF alpha, are the first cytokines that controls the methabolic answers. Increased IL-6 level is related to the protein break down of muscles and usage of IL -6 receptor antibody can prevent this effect. Anorexia is also one of well-known metabolic result of inflammation. IL-1 and TNF alpha’s effect on the satiety point in brain is blamed of this. Many inflammatory diseases are related with the osteoporosis. Many of diseases of like Rheumatoid artrit, systemic lupus, inflammatory intestine disease, chronicle obstructive lung disease and other inflammatory diseases, were found inreased risk for osteoporosis and bone fragility comparing with the healty population [19-21]. Our study has some limitation such as low number (n=27) of studied patients.
In our survey the malnutrition is found as 51.8%.The bone mineral density was detected lower in the patients with malnutrition. The CRP level which is the evidence of inflammation was significantly detected high for this group. As a conclusion, the malnutrition frequency is high for periton dialysis patients. There is a relationship between malnutrition and bone mineral density. We think that this is a result of inflammation. Thus, for CAPD patients, it is important to educate them regularly for dieting and to check their malnutrition levels. At the same time we advice them to be trained about the risk of bone fragility.

Table 1: NRS -2002 (Nutritional Risk Screening)
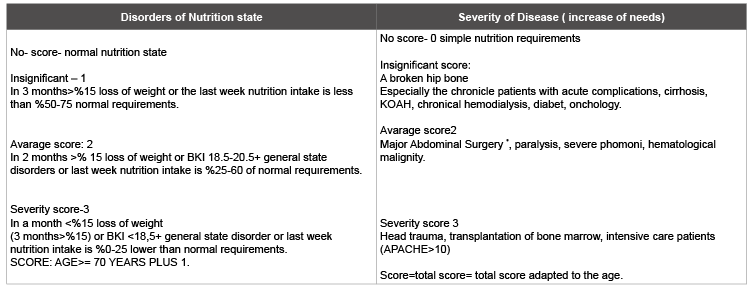
Table 2: The Last Screening
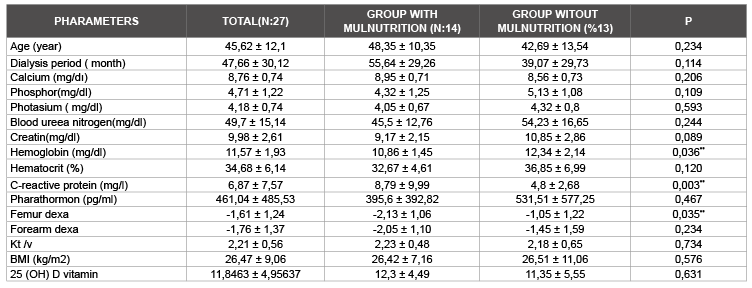
Table 3: The relationship between the two groups Demographic and biochemical parameters of the patients’
Download Provisional PDF Here
Article Type: Research Article
Citation: Akkaya L, Hüzmeli C, Candan F, Nur N, Kayataş M (2015) The Effect of Malnutrition on Osteoporosis for Periton Dialysis Patients and Solutions. Int J Nephrol Kidney Failure 2(1): doi http:// dx.doi.org/10.16966/2380-5498.120
Copyright: © 2015 Akkaya L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access