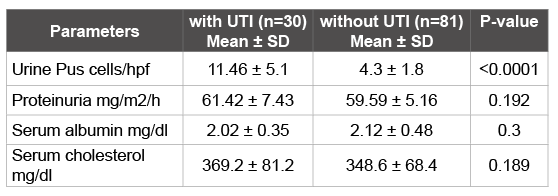
Table1: Baseline parameters of the nephrotic children with/without UTI.
SD Standard Deviation, hpf high power field
Biswanath Basu1* Dhiman Baur2 Sucharita Datta3 Mohua Bose4 Ashis Saha2
1Division of Pediatric Nephrology, Department of Pediatrics, NRS Medical College & Hospital, Kolkata, India*Corresponding author: Biswanath Basu, Department of Pediatrics, NRS Medical College & Hospital, Kolkata 700004, West Bengal, India, Tel: +91-9231236001; E-mail: basuv3000@gmail. com
Background: Prevalence of UTI in nephrotic children is high. It precipitates relapse and delays remission. The study was conducted to evaluate the prevalence of UTI, causative organisms and antibiotic sensitivity pattern in nephrotic children.
Methods: This prospective study was carried out in a tertiary care Government Medical College of Eastern India for a time period of 1y among the admitted cases of nephrotic children between the age group of 2y to 12y. Urine specimens were routinely obtained by clean catch method following careful preparation of urethral orifices. The specimens were inoculated immediately on MacConkey’s agar and blood agar plates. Identification of the organisms and antibiotic susceptibility testing was performed according to CLSI guidelines 2010 by Kirby-Bauer disc diffusion method.
Results: Total 111 nephrotic children were enrolled. Incidence of UTI was fairly high (27%) in nephrotic syndrome. E.coli (46%) was the most common organism responsible for UTI. Overall meropenem was the most sensititive perenteral drug (83%) for all isolates followed by amikacin (66%). Levofloxacin was the most common oral sensitive drug (75%).
Conclusion: Common isolates of UTI in nephrotic children have developed resistance to commonly used oral or perenteral drugs. Empirically oral levofloxacin or perenteral amikacin should be started in nephrotic children with suspected UTI when culture report is pending to prevent full blown relapse and early response of proteinuria. Meropenem may be kept as reserve drug.
Nephrotic syndrome; Urinary tract infection; E. coli; Meropenem; Levofloxacin
Urinary Tract Infection (UTI) and nephrotic syndrome are two most common renal diseases in children. The prevalence of UTI is 3-5% in girls and 1% in boys and the incidence of nephrotic syndrome is 2-3 /10,000 children per year [1]. UTI is a common complication and also an important precipitating factor of nephrotic syndrome. The prevalence of UTI among nephrotic children ranged from 20 to 60% with varying causative organisms and antibiotic sensitivity pattern [2-6]. However UTI is an important but often under-diagnosed association in children with nephrotic syndrome [7]. Breakthrough UTI precipitate new relapse in nephrotic syndrome. Also persistent UTI complicate the management of new relapse and hindering remission [2]. So this observational study was carried out to determine the incidence of UTI in admitted nephrotic children during the study period of 12 months from April 2011 to March 2012 with causative organisms and antibiotic sensitivity pattern in Eastern India.
This prospective study was carried out in a tertiary care Government Medical College of Kolkata, India. The admitted cases of nephrotic syndrome who fulfilled the International Study of Kidney Diseases (ISKDC) criteria (urinary spot protein/ creatinine >2, serum albumin <2.5 g/dl, serum cholesterol >200 mg/dl and edema) [8] between the age group of 2y to 12y were included in this study. Presence of any anogenital abnormalities, known anatomical abnormalities of genitourinary tract (e.g. Vesico Ureteric Reflux, Ureteric calculus), patients already on antibiotic prophylaxis and UTI developed after hospital admission were excluded from this study. The presence of UTI was searched in every case by urine culture and sensitivity immediately after admission. A clean-catch midstream urine specimen was used. Contamination by periurethral and prepucial organisms was minimized by washing the genitalia with soap and water. The specimen was directly collected in a sterile container. Prompt plating of the urine specimen, within one hour of collection, was done. If delay was anticipated, the samples were stored in a refrigerator at 4°C for up to 24 hours [9]. The urine culture was done according to standard guidelines in MacConkey’s agar and blood agar. The antibiotic susceptibility testing was performed according to CLSI guidelines 2010 by Kirby-Bauer disc diffusion method [10]. For this study, only culture proven case that is ≥ 105 CFU/ml of urine of a single pathogen was regarded as UTI [11-14]. Our institutional ethical committee had approved this study (IBR No. NMC/ETHI/GEN-25/52).
Out of 111 patients enrolled 30 had evidence of UTI. Characteristics of the children suffering from UTI and without UTI are described in (Table 1).

Table1: Baseline parameters of the nephrotic children with/without UTI.
SD Standard Deviation, hpf high power field
As per urine culture E.coli (46%) was the most common organism responsible for UTI followed by K. Pneumoniae (27%), E. fecalis and S. aureus (10% each) and P. mirabilis (7%). According to sensitivity pattern (Figure 1) E. coli was mostly sensitive to meropenem (93%) followed by levofloxacin (86%), amikacin (71%), gentamycin (43%), ofloxacin (36%), cotrimoxazole (29%), cefotaxime and ciprofloxacin. (21% each), ceftriaxone and cefixime (14% each). K. pneumoniae was mostly sensitive to meropenem (88%) followed by amikacin and levofloxacin (75% each), gentamycin (43%), ciprofloxacin (38%) and lastly ofloxacin, cotrimoxazole, cefotaxime and cefixime (25% each). P. mirabilis was found sensitive to levofloxacin, ciprofloxacin, ofloxacin, meropenem, amikacin and gentamycin equally (50% each). E. fecalis, a gram positive isolate, was sensitive to vancomycin and linezolid in all cases (100%), while to levofloxacin, meropenem and amikacin in 1/3 cases (33%). S. aureus, the other gram-positive organism was 100% sensitive to vancomycin and linezolid and meropenem, whereas 66% was sensitive to levofloxacin, amikacin, co-amoxyclav and co-trimoxazole and only 33% to gentamycin.
Overall meropenem was the most sensititive drug (83%) for all uropathogens followed by levofloxacin (75%) and amikacin (66%). However, commonly used drugs like gentamycin (40%), co-trimoxazole (30%), ofloxacin (27%), cefotaxime (17%) and ceftriaxone (7%) were significantly less sensitive.
Incidence of UTI is fairly high in nephrotic syndrome. A high prevalence (66.7%) of UTI had recently been documented in two studies from Africa by Adeleke et al. [4] and Adeodoyin et al. [3]. Similar high prevalence of UTI had also been reported in studies from India by Gulati et al. [2], Alawadi et al. [6] and Senguttuvan et al. [5] where its frequency were 40.26%, 22.8 % and 46% in order.
In our study, E. coli was the most common organism responsible for UTI followed by K. pneumoniae, E. fecalis, S. aureus and P. mirabilis. Senguttuvan et al. [5] in their study reported almost similar findings, where E. coli was the most common isolate (36.6%), followed by K. pneumoniae (27.5%) and P. aurogenosa (12.55%). Gulati et al. [2] also reported a higher prevalence of E. coli (60%) than non E. coli gram negative organisms (30%) and gram positive organisms only in 10% of patients. In the study of Adeleke et al. [4], Staphylococcus aureus was the commonest organism comprising 67.9% of isolates, followed by Klebsiella (17.9%) and Pseudomonas (14.2%). In their study, Ibadin et al. [15] reported 54.3% isolates as Staphylococcus aureus. This variation may be due to geographical variation of the organism causing UTI. So in this region of World E. coli is the commonest organism.
In our study, it was revealed that the gram negative organisms were mostly sensitive to meropenem followed by levofloxacin and amikacin. Isolates were comparatively less sensitive to more commonly used antibiotics like gentamycin, ofloxacin, ceftriaxone, cefotaxime, coamoxyclav, cefixime and ciprofloxacin etc. On the other hand the gram positive organisms were fully sensitive to vancomycin and linezolid in comparison to other common antibiotics. Senguttuvan et al. [5] studied that amikacin amd cefotaxime were most sensitive in UTI. Adeleke et al. [4] in their study found that the sensitivity of Staphylococcus aureus organism to ceftriaxone and ciprofloxacin was 100%, while to commonly used antibiotics such as nalidixic acid and ampicillin was low. Gentamycin and streptomycin had 100% coverage for the gram-negative organisms, while Staphylococcus aureus showed poor susceptibility to these antibiotics. But Adeodoyin et al. [3] in their study from Africa found an increased efficacy of fluroquinolones and third generation cephalosporins for the common organisms of UTI in nephrotic syndrome.
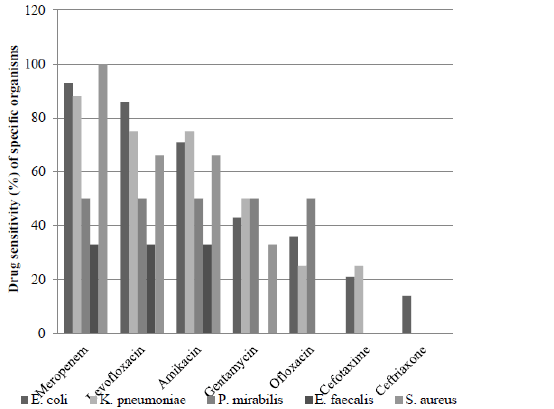
Figure 1: Comparison of drug sensitivity pattern of common isolates
E. coli is the commonest organism responsible for UTI in nephrotic children. Common isolates of UTI in nephrotic children have developed resistance to commonly used oral or per-enteral drugs. Empirically oral levofloxacin or perenteral amikacin would probably be the most effective antibiotics in suspected UTI. Meropenem may be kept as reserve drug.
The authors have declared that no Conflict of interest exists. No external support for the work, received in the form of grants and/or equipment and drugs.
Download Provisional PDF Here
Article Type: Research Article
Citation: Basu B, Baur D, Datta S, Bose M, Saha A (2015) Bacteriological Profile and Sensitivity to Antibiotics of Common Isolates Responsible for Urinary Tract Infection in Nephrotic Children. Int J Nephrol Kidney Failure 1(3): http://dx.doi.org/10.16966/2380- 5498.116
Copyright: © 2015 Basu B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access