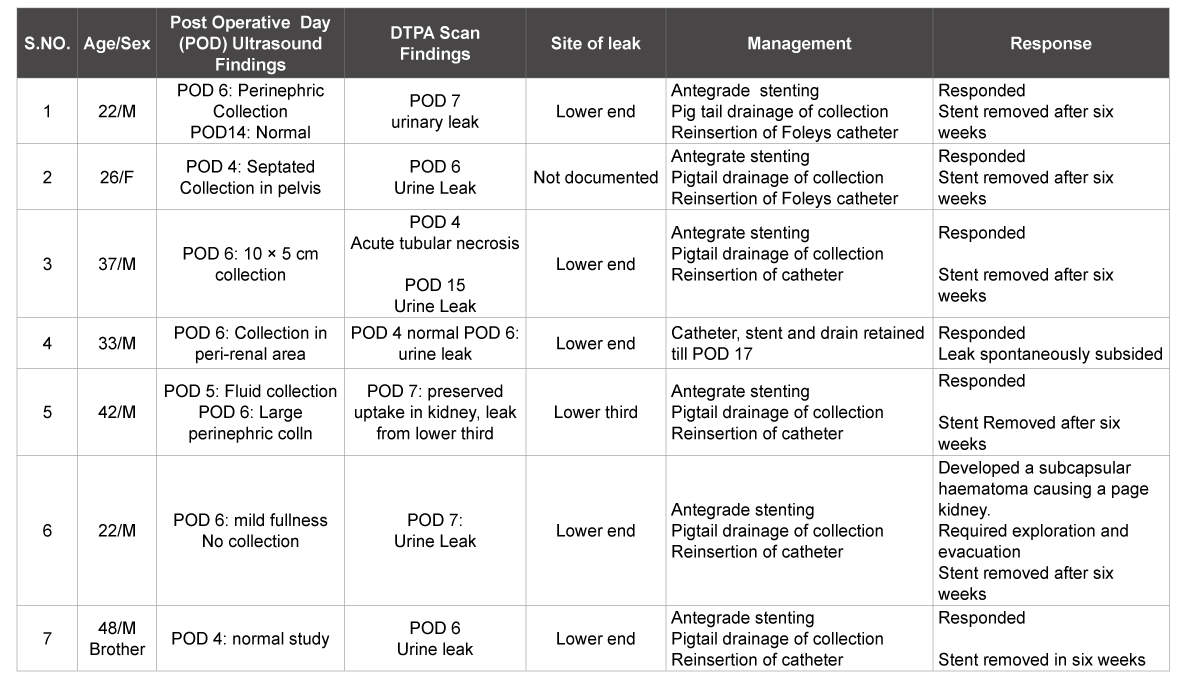
Table 2:Details of the major urological complications encountered
Sandeep Guleria1 Surjeet Kumar2 Praveen Pushkar3 Pankaj Gupta4 Sanjay Sharma5 Sandeep Mahajan6
1Senior Consultant, Department of Surgery and Renal Transplantation, Indraprastha Apollo Hospital, New Delhi, India*Corresponding author: Guleria S, Senior Consultant, Department of Surgery and Renal Transplantation, Indraprastha Apollo Hospital, New Delhi. India, Tel: +919891640002; E-mail: sandeepguleria@hotmail.com
Context: The value of the double J stent in renal transplantation is controversial. However prolonged stenting is associated with major urological complications including sepsis, encrustation, migration and forgotten stents.
Aim: This study reviewed our retrospective experience of 672 renal transplants in which the tied double J stent was used and removed five to six days post transplantation.
Settings and Design: Retrospective analysis of all consecutive renal transplants done at our centre.
Material and Methods: 672 consecutive renal transplants in which the tied double J stent was used. The incidence of major urological complications and infections was evaluated on a follow up of six months.
Results: The urinary leak rate was .01% and the incidence of symptomatic urinary tract infection was 10.6%. Six out of seven leaks responded to radiological intervention in the form of per cutaneous nephrostomy ante-grade stenting and pig tail catheter drainage. The remaining one responded to prolonged catheterisation.
Conclusion: The tied double J stent is an attractive alternative to routine stenting in renal transplant recipients.
Tied double J stent; Renal transplantation; Urological complications
The value of Double J stents in renal transplantation is controversial. Initially double J stents were used for salvage of urinary complication or as a prophylactic measure in cases where the vascularity of the ureter appeared compromised during retrieval [1]. While the routine use of double J stents did result in a reduction in major urological complications they were associated with a significant increase in urinary tract infections. This was borne out in a recent Cochrane review which concluded that major ureteric complications reduced significantly with use of prophylactic ureteric stenting but complications did occur with a prolonged duration of indwelling stent [2]. The complications that can occur with prolonged stent are urinary tract infections (UTI), encrustation, migration and forgotten stents.
In our centre we started using routine stents in renal transplantation in 1995 and in a prospective randomized case controlled trial between the stented and non stented patients demonstrated an incidence of major urological complications (MUC) of 1.8% and 5.8% respectively [3]. Concerned by reports of high rates of infective complications we shifted to the tied double J stent in 2004. We report our experience with the tied double j stent in six hundred and seventy two consecutive live related renal transplant recipients.
This is a retrospective analysis of all renal transplants done at our centre from 2004. Patients with a follow up of less than six months, and where a graft nephrectomy had to be performed for reasons other than urological were excluded. Patients where uretero-ureterostomies were performed were also excluded from the study. The kidneys were retrieved by either the open technique or by the laparoscopic donor nephrectomy. In all the patients included, the allograft was placed in the iliac fossa and an approximately 1.5 cm cystotomy was done on the antero-lateral aspect of the bladder and the tip of the foley’s catheter was pulled out. A 6 Fr 24 cm double J stent was tied to the eye of the catheter using a 2-0 prolene suture and the catheter pushed back. The uretero-neocyststomy was done using Lich Gregoir extravesical method using two 4-0 polydiaxone sututes in a continuous fashion. A suction drain was placed in the iliac fossa before closure in all patients. The catheter was retained for five to six days in all patients. The drain was kept till the drain output was less than 25 ml in 24 hours. A Doppler Ultrasound and a Diethyl Triamine Penta Acetic acid (DTPA) scan was done in the first week on all patients. If the drainage increased, a fluid creatinine along with serum creatinine and a repeat DTPA scan were performed. In case a urine leak was suggested the drain and catheter with stent were retained if not already removed. In case they were removed then ante grade stenting under ultrasound guidance was attempted along with a drain in the iliac fossa.
All patients who were discharged with an ante grade stent were called for stent removal after six weeks.
Various immunosuppressive protocols were used in this period depending on the patient profile. All patients were on triple drug immunosuppression and this was either Tacrolimus or Cyclosporine based. All recipients were started on a steroid dose of 20 mg on the first day and this was gradually tapered to 5 mg by the end of twelve months. Mycophenolate Mofetil was used in 653 of these patients as the second immunosuppressant. The remaining 19 were on azathioprine. All recipients were started on co-trimoxazole 480 mg once daily for three months.
Tacrolimus levels were monitored frequently keeping them between 8-12 ng/ml in the first three months, 6-8 ng/ml in the next six months and less than four at the end of the year. All patients were followed closely for at least six months and a routine ultrasound along with urine microscopic examination with culture were obtained once a month. Occurrence of any hydronephrosis in the transplanted kidney was evaluated with a DTPA scan. Incidence of Urinary tract infections (UTI) was recorded and all positive cultures were treated aggressively by appropriate antibiotics.
Six Hundred and seventy two patients were operated during this period. Thirty -two were deceased donor transplants including two with simultaneous pancreas and kidney transplants and rest were live donor renal transplants. Recipient age ranged from 6 years to 60 years. Kidneys were retrieved by open method in 522 cases and in the remaining one hundred and eighteen were retrieved by laparoscopy. Uretro-uretrostomy was performed in one patient, due to an accidentally reverse placed allograft, and was excluded from the study. Seventeen patients expired and five graft nephrectomies had to be performed. The causes of graft nephrectomy and death are enumerated in Table 1.
Records of follow up for six months were available for 650 patients. All urological complications were recorded.
Urine leak was seen in seven patients (0.01%). Only one of these patients had a cadaveric graft. The remaining six were live donor kidneys retrieved by the open donor nephrectomy and had single renal artery on imaging as well as on exploration.
In six of the seven patients the leak presented as either pain or decreased urine output after catheter and stent removal. Initial routine ultrasound in four of these patients had shown a small perinephric collection on the fourth post operative day but the drain had decreased to minimal and hence these collections were ignored. Their catheters with stent were removed on the seventh post operative day after which recipients complained of pain abdomen and a decrease in urine output. A Leak was confirmed on DTPA scan and antegrade stenting was done for all the patients under ultrasound guidance. The Foleys catheter was re inserted of catheter and pigtail drainage of perinephric collection was done. The graft could be salvaged in all these patients with minimal invasion (Table 2).
Causes of Graft Nephrectomy |
Post Renal transplant Deaths |
| Hyperacute rejection /Accelerated AR 3 Renal vein Thrombosis 1 Renal Artery Thrombosis 1 |
Acute Cardiac Deaths 9 Sepsis 4 Pneumonia 1 DIC 1 CMV Infection 2 |
| Total 5 | 17 |
Table 1: Causes of Graft Nephrectomy and Death in the 672 renal transplant recipients at a six month follow up.
One patient developed a subcapsular hematoma with a page kidney after antegrade stenting and had to be re explored for evacuation of the subcapsular hematoma. The stent was left indwelling for 6 weeks in all these patients and all these patients had normal renal function at the time of stent removal.
In the remaining patient, the drain showed an increased output from POD 4 and drain fluid chemistry showed creatinine value of 2.4 mg/dl when the serum creatinine was 1.4 mg/dl. The catheter, DJ stent and the drain were retained and slow decrease in drainage was observed till it ceased on the sixteenth post-operative day.
Urine leaks in six of the seven patients were demonstrated on DTPA to be from the vesicoureteric junction. All six patients with ante-grade stents have been followed for six months after stent removal. Three patients had mild non-obstructive hydronephrosis documented on DTPA, but none required any further reconstructive surgery.
None of the patients in our series with tied stents had significant ureteric obstruction. Mild asymptomatic hydronephrosis was detected at follow up ultrasound in 23 of our patients including three where antegrade stenting was done for urinary leak, but the renal parameters were stable in all of these patients. All these patients were subjected to nuclear renography and excellent drainage was documented in all of them. None required intervention.
One hundred and seventy two episodes of asymptomatic bacteriuria occurred in one hundred and thirty patients and all of these were treated with appropriate oral antibiotics for fourteen days. Sixty nine patients developed febrile urinary tract infection which was managed aggressively with parenteral antibiotics for ten to fourteen days according to the appropriate sensitivity report. None of these patients suffered graft loss because of infections.
Since the stent was removed in all patients along with catheter, there was no incidence of forgotten, migrated or calcified stents. Interestingly, in three patients the stent did not come out with catheter and either the knots were found loose or the prolene tie broke. Cystoscopy was performed in all these patients before discharge to remove the stent.
The use of stents has been a major controversial issue in renal transplant surgery literature. Contrary to the higher past incidence of major ureteric complications to the range of 20-30% causing significant morbidity and mortality, the contemporary literature boasts of only a 5-10% incidence of MUC [4,5]. This change has occurred gradually with better preservation of donor ureteric vasculature by avoiding dissection between lower pole of the donor kidney and the ureter, recognizing the importance of lower polar vessels and most importantly, the use of newer immunosuppression protocols with low dose steroids [1]. That such low incidence of ureteric complications can be achieved even without a stent is the major reason why prophylactic stenting is avoided by many transplant surgeons. Although the overall mortality and graft loss because of ureteric complications have decreased but whenever a major early ureteric complication occurs it may require a number of secondary interventions, re exploration and reconstruction.

Table 2:Details of the major urological complications encountered
Two meta-analysis have addressed this issue and both demonstrate that prophylactic stenting does lead to significant decrease in ureteric complications [2,6]. Prophylactic stenting was being practiced at our centre since 1994. In a prospective randomized control study from our centre, we documented a significant reduction in ureteric complication rate in the stented group. However there was a higher incidence of urinary tract infections in these patients [3].
An issue of additional cost associated with routine use of stent after transplant has been raised as the number needed to treat to prevent one ureteric complication is between 10-30 [2]. Tavakoli et al. [7] evaluated the cost effectiveness of routine stenting in a prospective randomized controlled study where they stented 112 patients and no stent was used in 78 patients and found that overall surgical complication rate was significantly higher in the non stented group (11.5% vs 0.9%) and the expenditure was significantly high for the non stented group. The study found routine stenting to be more cost effective. In another study from the University of Michigan, the authors evaluated the direct cost of stenting and stent removal with costs in management of morbidities of ureteric complications and found that 22-23 stentings can be performed at the cost of treating one patient with a ureteric complication and concluded prophylactic stenting to be financially advantageous [8].
G Morris-Stiff and colleagues had first described tying of the DJ stent to the catheter [9]. In their experience of fifteen patients the stent was removed after a mean of 8 days. None of their patients developed urinary sepsis. In 2005, Sansalone et al. [10] published their eight years experience with tied stents in 590 patients. Nine of their patients required surgical revision. We were able to salvage all our grafts without redoing the uretero-vesical anastomosis. Only one patient required re exploration for a subcapsular hematoma that was causing a page kidney after antegrade stenting.
An externally draining 8 French catheter inserted through a direct suprapubic bladder puncture and across the ureteroneocystostomy was described by Minee et al. [11]. The externally draining catheter was routinely removed on POD 5. 13 out of their 196 recipients (6.6%) developed MUC (ureteric stricture in 10 and leak in 3) including five who required surgical revision.
In our series of tied double j stents, we encountered a MUC rate of 0.010% (7/648 patients). All the seven patients had urinary leaks from the lower ureter and none developed significant ureteric obstruction. This is significantly less as compared to the MUC rate in literature with the routine use of double J stents. The routine use of tied double j stent helps decrease significantly the urological complications along with a decrease in the cost and a decrease in the workload of the unit.
Although a clear mandate seems to be emerging that the routine use prophylactic stenting prevents MUCs but stents have been associated with significant infective complications including graft loss, the incidence and magnitude being directly proportional to the duration of the indwelling stent after transplantation. In a Cochrane review of randomized controlled trials available on this issue it was observed that the incidence of stent related complications is high if stents are kept for >6 weeks [2]. Tavakoli et al. [7] in a prospective RCT observed significantly higher rates of UTI if the stent was left more than 30 days after transplant. In a retrospective randomized study from a single centre in Greece, Giakoustidis D et al. [12] reviewd records of 44 and 73 patients of stented and non stented ureterovesical anastomosis where stents were removed at POD 14 endoscopically. The incidence of UTI was similar in both the groups and though the incidence of urinary leaks was similar but the gravity of leak was less en to avoid re-exploration and reanastomosis in the stented group. Minee et al. [11] used 5 day external stents after KT in their non randomized study and found that the advantage of prophylactic stenting persisted even with this duration in living donor transplants. They defined ureteric complications as only those requiring percutaneous nephrostomy or surgical revision and did not include UTI in their study. They also mentioned that these benefits did not reflect as such in cadaveric transplants where complications occurred in 8.5%.
In a study from Italy, Sansalone et al. [10] observed that most MUCs occur within 14 days of transplant and hence used tied stents in 590 patients and observed an overall complication rate of 1.5 % (9/590 patients, leak 2, obstruction 7). In this study all these 9 patients required a major reconstructive procedure.
All our seven patients with MUC developed urine leak which was diagnosed only after stent removal in six of the patients. Renal allograft was salvaged in all these patients using minimally invasive radiological techniques i.e. percutaneous nephrostomy and antegrade stenting. A Leak was diagnosed in one patient with increased drainage and then the stent and per urethral catheter were retained leading to spontaneous resolution and avoidance of intervention.
The incidence of UTI in recipients with stent is variable in literature. Ranganathan et al. [13] suggest a very high incidence of 71% on stents. Other studies quote the incidence to be between 30-50%. The incidence is significantly high when stents are kept for more than 30 days. We saw UTIs in 20% of our patients which were asymptomatic in most of them and only 10.6% patients developed febrile UTI requiring admission and parenteral antibiotics.
Other recommended measures to prevent UTI in stented patients after transplant are early endoscopic removal of stent at 2 weeks [12] and compulsory double voiding within five minutes of first micturition. The latter was used in a prospective RCT and was shown to reduce the incidence of positive culture to 3.3% as against 34.4% in control [14].
We are aware that the greatest limitation of our study is that it is a retrospective study and not a randomized control study. However MUC are so few in both groups currently that the number of patients in both groups would have to be enormous to demonstrate any statistical significance and draw any conclusions.
The tied J stent apart from saving an additional procedure and decreasing the workload of the unit also eliminates the possibility of a migrated, calcified or a forgotten stent. It is associated with a lower incidence of positive urine culture. It also has a low incidence of MUC’s
The incidence of ureteric stricture was nil in our patients unlike other series with prophylactic stenting. This may be related to the fact that we routinely harvest the gonadal vein with the ureter and perform a widely spatulated anastamosis with full thickness of the bladder wall as after retrieving the tip of the Foley’s catheter though the cystotomy the resultant hole invariably becomes large.
Thus to conclude the tied double j stent is an attractive alternative to routine stenting in renal transplant recipients.
Download Provisional PDF Here
Article Type: Research Article
Citation: Guleria S, Kumar S, Pushkar P, Gupta P, Sharma S (2015) The Tied Double J Stent: A Novel Method for Preventing Early Ureteric Complications in Renal Transplantation. Int J Nephrol Kidney Failure 1(1): doi http://dx.doi.org/10.16966/ijnkf.105
Copyright:© 2015 Guleria S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access