Abstract
Background: Ellis–van Creveld syndrome (EVCS) is a rare disease characterized by various cardiac and skeletal abnormalities. It carries a high mortality in early life and accounts for 50% mortality during infancy. There are only limited numbers of cases reported worldwide.
Case presentation: A 9-years-old girl presented with dyspnoea on exertion of 4 months duration (NYHA II). She was short statured and had bilateral upper limb polydactyly, dysplastic teeth. Cognitive and motor developments were normal. On evaluation, 2D Echocardiography showed common atrium, partial AV canal defect, and mild tricuspid regurgitation. Intraoperatively in addition to above findings the patient also had dual coronary sinus ostiae and persistent left superior vena cava (LSVC) draining into the left atrial roof. The patient underwent successful correction of associated pathologies (Intracardiac repair). The perioperative period was uneventful.
Conclusion: This case is being reported to emphasize the rare occurrence of Ellis–van Creveld syndrome and even rare association of dual coronary sinus ostiae with it.
Keywords
Ellis–van Creveld syndrome; AV canal defect; LSVC
Introduction
The prevalence of Ellis–van Creveld syndrome (ECVS) varies widely in general population from 1 in 60,000 to 1 in 150,000 live births [1]. Approximately 150 cases are reported worldwide. It is an autosomal recessive skeletal disorder with inter- and intra-familial variability and parental consanguinity present in 30% of cases [2].
Prenatal diagnosis can be made with intrauterine growth retardation, skeletal malformations and cardiac defects on ultrasound images. Diagnosis can also be possible using chorionic villi or amniotic fluid analysis if there is a positive history in other siblings. Prognosis depends on the presence of cardiac or respiratory anomalies. 33% can die in infancy or at an early age because of cardiorespiratory problems [3].
The classic tetrad of EVCS consists of chondrodystrophy, polydactyly, ectodermal dysplasia, and cardiac anomalies. The severity of the condition varies from person to person. It is characterized by short ribs, short limbs, postaxial polydactyly, and dysplastic teeth and nails. Congenital heart defects occur in 60% of cases. The cardiac defects vary – common atrium, ventricular septal defect, endocardial cushion defects, persistent left superior venacava (LSVC), pulmonary venous connection abnormalities.
We report a case of EVCS with common atrium, partial AV canal defect, persistent LSVC, severe mitral regurgitation (MR), mild tricuspid regurgitation (TR), mild pulmonary arterial hypertension (PAH) treated successfully.
Case Presentation
A 9-years-old girl presented with dyspnoea on exertion of 4 months duration (NYHA II). On examination, she was short statured and had bilateral upper limb polydactyly, dysplastic teeth. Cognitive and motor developments were normal. Family history revealed no consanguinity and other siblings were normal.
Hemodynamic parameters were unremarkable. Cardiac examination revealed apex beat in left 6th intercostal space, widely split and fixed second heart sound, grade 3/6 pansystolic murmur at the mitral area. Central nervous system and per abdomen examinations were normal.
Chest X-ray showed cardiomegaly (Cardiothoracic ratio=65%) with right atrial enlargement. ECG showed normal sinus rhythm with right axis deviation, evidence of right atrial and right ventricular enlargement.
2D Echocardiography showed situs solitus with enlarged right ventricle (RV), common atrium, partial AV canal defect, mild tricuspid regurgitation (TR), severe MR, pulmonary artery systolic pressure (PASP) of 38 mmHg.
Based on her symptoms and echocardiographic findings we planned to go ahead with intracardiac repair.
Intraoperative
There was presence of bilateral SVC with absent left innominate vein. Right atrium (RA), RV and pulmonary artery (PA) were dilated.
Under cardiopulmonary bypass (CPB) using aortic and tricaval cannulation, aorta cross clamped and the heart was arrested using delNido cardioplegia. CPB was conducted at 28ºC.
Trans atrial (RA) approach was used. Findings were - common atrium, partial AV canal defect, dual coronary sinus ostiae separated by a small muscle ridge, cleft anterior mitral leaflet (AML) (Figure 1).

Figure 1: Schematic representation of intraoperative findings. RSVC: Right Superior Vena Cava; LSVC: Left Superior Vena Cava; LAA: Left Atrial Appendage; PV: Pulmonary Veins; MV: Mitral Valve; TV: Tricuspid Valve; IVC: Inferior Vena Cava; A-Dual coronary ostiae; B-Cleft AML
Cleft AML was closed using interrupted 6-0 polypropylene suture. Mitral valve was competent on saline insufflation test. AV canal defect was closed using single patch technique with treated (0.6% glutaraldehyde) autologous pericardium directing both coronary sinus ostiae to the left atrium.
Patient came off CPB in first attempt in sinus rhythm with minimal inotropic supports. But developed desaturation and arterial blood gas (ABG) analysis showed pO2 of 45mm Hg. We ruled out pulmonary causes and the anatomy was reassessed. We could find LSVC was draining into the roof of the left atrium (LA). LSVC was disconnected from the LA roof, dissected and routed to Right SVC (retro-innominate) (Figure 2). Following which oxygen saturation was improved to 98% (ABG – pO2 >120 mm Hg with FiO2 of 60%). The patient was extubated after 6 hours and the perioperative period was uneventful.
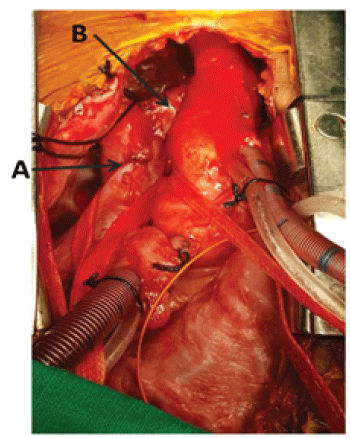
Figure 2: Intra-operative picture: A-Right SVC and Right atrial (RA) junction; B-LSVC routed to RSVC.
Contrast venous angiogram (via subclavian vein) showed LSVC draining into RSVC with normal flow. Postoperative Echo showed intact patch, no residual shunt, and mild central MR jet with good biventricular function.
At 6 months follow up, patient was asymptomatic with similar Echo findings as previous.
Discussion
The first full description of the syndrome was given by Richard Ellis and Simon Van Creveld in 1940. A large number of cases have been reported in the Amish Community of Lancaster, Pennsylvania, USA but, the disease has been described in other population and is known to affect all races.
Treatment depends on which body system is affected and the severity of the problem. The condition itself is not treatable, but many of the complications can be treated. A multidisciplinary approach is encouraged for proper management and rehabilitation of patients with ECVS. Antibiotic prophylaxis to prevent bacterial endocarditis is crucial when dealing dental problem in these patients because of the high prevalence of cardiac anomalies. Genetic counselling is recommended for prospective parents from a high risk group or who have a family history of EVCS.
Although there is no systematic follow-up of EVCS series reported, the prognosis is linked to the respiratory difficulties in the first months of life and these difficulties are related to thoracic narrowness and possible heart defects.
Literature search reveals only few reports of surgical repair of EVC syndrome and only one case of dual coronary sinus ostiae associated with EVC syndrome [4].
Haci et al. [5], reported a case of 16-month-old girl with the classic signs of EVC syndrome along with thymic hypoplasia. Mitral clefts were repaired by direct suturing, the single atrium was repaired by creating a new septum with a pericardial patch leaving the coronary sinus in the left atrium [5].
Mundayat Gopalakrishnan et al. [4] reported a case of 30 years old female with EVC syndrome with single atrium, mitral and tricuspid regurgitation, left superior vena cava, dual coronary sinus ostiae who underwent successful surgical correction.
In a series of patients with Double-outlet right atrium (DORA), 11 patients survived the surgical repair, the only death occurred in the patient with Ellis van Creveld syndrome [6].
There was one case of EVCS with polydactyli and atrioventricular canal defect in each series of atrioventricular canal defects [7,8].
Even though several different techniques have been described to deal with persistent LSVC, we routed the LSVC to the RSVC (retroinnominate).
Although the occurrence of EVCS with dual coronary sinus ostiae is rare, appropriate surgical repair allows us to obtain excellent results.
Acknowledgement
We sincerely thank Dr. Mundayat Gopalakrishnan for granting the permission to reproduce Figure 1 from the article, “Ellis Van Creveld Syndrome with Partial Atrioventricular Canal Defect, Persistent Left Superior Vena Cava, Dual Coronary Sinus Ostiae - A Case Report”.
Article Information
Article Type: Case Report
Citation: Maruti HY, Nareppa U, Bhaskar BV, Shivaprakash S, Hittalamani S, et al. (2017) Ellis-Van Creveld Syndrome with Dual Coronary Sinus Ostiae: A Case Report. J Hear Health 3(3): doi http://dx.doi. org/10.16966/2379-769X.140
Copyright: © 2017 Haranal Maruti Y, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
Received date: 18 Oct 2017
Accepted date: 24 Nov 2017
Published date: 30 Nov 2017



