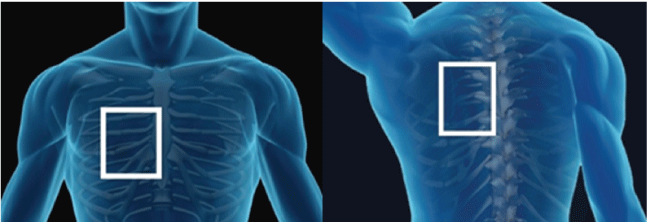
Figure 1: Electrode positions.


Bagh RP*, APRN, AGACNP-BC, FNP-BC
William P. Clements Jr. University Hospital, Dallas, Texas, USA*Corresponding author: Bagh RP, William P. Clements Jr. University Hospital, Professional Office Bldg. 2, Suite 935, 5939 Harry Hines Blvd., Dallas, Texas 75390-9198, USA, E-mail: rose.bagh.fnp@aol.com
Cardioversion is a frequently performed procedure to terminate atrial arrhythmias; commonly atrial fibrillation and atrial flutter, to relieve symptoms and improve cardiac performance. In simple terms, it involves the delivery of high energy electrical shock to patient’s chest wall to the heart to interrupt abnormal electrical currents to restore it to normal sinus rhythm. Prior to performing this procedure, there are several safety checks undertaken for a safe and successful outcome. There is a 48 hours safety window for cardioversion without appropriate anticoagulation and the need for continuation of appropriate anticoagulation for 4-6 weeks after cardioversion to reduce the risk of stroke. Advance practice providers (APPs) are emerging as an integral part of the cardiovascular team and they have been recognized as safe provider to perform cardioversions autonomously with appropriate clinical training using AHA Guidelines directed protocols. The AHA Guidelines for a safe and successful cardioversion will be discussed in this article.
Cardioversion; Arrhythmias; Atrial fibrillation; Atrial flutter; Anticoagulation therapy; Stroke; Risk of stroke; 48 hours safety window; Sinus rhythm
Advance practice providers (APPs) are emerging as an integral part of the cardiovascular team and they have been recognized as safe provider to perform cardioversions autonomously with appropriate clinical training using AHA guidelines directed protocols. A recent evidence-based study also concluded that APPs can safely perform cardioversions autonomously using appropriate tools, protocols, and checklists of procedures directed and supervised by physicians that have effective outcomes and excellent patient satisfaction [1].
Cardioversions and defibrillations are two commonly used procedures for patients with abnormal heart rhythms. Cardioversion is a commonly used procedure to terminate abnormal cardiac arrhythmia, most commonly atrial fibrillation and atrial flutter. To restore a normal heart rhythm, cardioversion delivers high energy electrical shock through the chest wall to the heart muscles. This delivery of high energy electrical shock that is synchronized to the QRS Complex is cardioversion, whereas the delivery of non-synchronized electrical shock that is given randomly during the cardiac cycle is defibrillation [2].
Delivering a synchronized electrical shock that depolarizes the tissue involved in a reentrant circuit during cardioversion terminates arrhythmias. The circuit is unable to propagate or sustain reentry by depolarizing all excitable tissue of the circuit by making the tissue refractory. Cardioversion terminates those arrhythmias resulting from a single reentrant circuit, such as an atrial flutter, an atrioventricular nodal reentrant tachycardia, an atrioventricular reentrant tachycardia, or a monomorphic ventricular tachycardia. Cardiac muscle and conduction tissue are simultaneously activated by high energy electrical impulses. An interruption of reentrant circuits takes place, breaking the repeating cycle, and terminating the arrhythmia. Thereafter, the sinus node begins to fire again restoring a normal heart rhythm.
One of the most common indications for an elective outpatient cardioversion procedure is atrial or supraventricul arrhythmias, especially atrial flutter and atrial fibrillation. The ventricular arrhythmias; ventricular tachycardia and ventricular fibrillation are commonly treated with an emergent defibrillator shock. Elective cardioversion for atrial flutter/fibrillation are commonly performed in the post anesthesia care unit (PACU). In cardiovascular intensive care unit or in an emergency department (CVICU/ED) setting, defibrillation is done in emergent VT/ VF cases. However, there are no rigid rules where one procedure can be done and the other cannot be done. Pregnancy is not a contraindication for cardioversion. Fetal heart monitoring during the procedure is recommended but should not delay emergent defibrillation.
Device related variables: The outcome of cardioversion is based on a number of electrode characteristics. These include electrode position; pad size, and hand-held versus patch electrodes [3]. The amount of energy also has an impact upon the outcome of the cardioversion procedure. It is important to make sure that the skin is clean, dry and free of hair for good adhesion of electrodes. Several studies have suggested that lesser energy is required with electrodes positioned in anteroposterior fashion than anterio-anterior position. The success rate with the anteroposterior electrode position is higher compared to anterio-anterior electrode position [4] (Figure 1).

Figure 1: Electrode positions.
Patient with device: Patients with permanent pacemaker/implantable cardioverter defibrillator (PPM/ICD) require special attention to electrode placement. Electrodes should be placed at least 12 cm away from the device. Preferably the electrode pads should be in the anteroposterior position and avoid any contact with the skin overlying the device.
Patient related variables: The type of arrhythmia and the patient’s clinical condition are important determinants for a successful outcome of the procedure. Patients with primary atrial fibrillation are easier to cardiovert than patients with secondary atrial fibrillation resulting from an uncompensated congestive heart failure and hypotension. The duration or amount of time an arrhythmia, both atrial and ventricular, has been present also determines the outcome. The longer the duration, the harder it is to keep patients in rhythm. The more recent the onset of an arrhythmia, the greater is the success with cardioversion. Some studies have shown that patients with more recent onset of arrhythmia have higher chances remaining in sinus rhythm for a longer period of time compared to the patients who have had chronic arrhythmias.
The energy requirements are different for organized and non-organized arrhythmias. Organized arrhythmias, such as atrial flutter, arise from a discrete reentrant circuit which is easily depolarized by smaller amounts of current of 100 Joules (J). Higher energy of 200-360 J is often required for non-organized rhythms, such as atrial fibrillation, polymorphic ventricular tachycardia, and ventricular fibrillation. The wave fronts are multiple and involve more myocardial mass, thereby requiring more energy (200-360J) for termination.
Antiarrhythmic drugs: Loading patient with adequate amount of antiarrhythmic drugs prior to an elective cardioversion have resulted in better outcomes and patients tend to remain in normal sinus rhythm for a longer period of time compared to patients who are not loaded with antiarrhythmic drugs (AAD).
A cardioversion procedure is performed in a hospital-based setting, such as PACU, as an elective outpatient procedure on closely monitored stable patients. It is also performed as an emergent procedure for a hemodynamically unstable patient in a CVICU/ED setting in a hospital or in a procedure room that is specially equipped for cardioversion. Patients are connected to monitors for continuous monitoring of heart rate, rhythm, oxygen levels, breathing rate, and blood pressure. The electrical shocks during cardioversion are painful, so moderate conscious sedation is performed by anesthesiologist to put patients asleep transiently. Intubation with endotracheal tube is not necessary for this procedure. The skin is shaved, cleaned, and dried after which two electrode patches or paddles are applied to the skin. After these preparatory steps and when the patient is adequately sedated, high energy electrical current is delivered through these patches. The amount of energy used depends upon the arrhythmia. Subsequent higher energy electrical shocks may be needed if the initial attempt at converting the heart rhythm to sinus rhythmis unsuccessful [2].
The cardioversion procedure itself takes only a few seconds once all the preparatory setups described above are complete. The patient usually awakens and is alert five to ten minutes after the procedure when the anesthesia wears off.
The cardioversion procedure in itself can sometimes initiate other fast or slow arrhythmias. In order to avoid provoking a dangerous arrhythmia, the electrical shock must be timed with the heartbeat. Occasionally after cardioversion, the sinus node may not work properly and a very slow heart rate may result in some patients, especially in patients who have been on rate controlled with beta blocking agents. To correct this problem, it may be necessary to pace and at times (rarely) a temporary or a permanent pacemaker insertion may be required. Practitioner should be prepared to trans-cutaneous pace patients for persistent bradycardia or defibrillate patients for unstable ventricular rhythms. Sometimes a stroke can occur if the electrical shock either causes a clot that is already present to dislodge and travel to the brain or to another part of the body. These scenarios are less likely in patients who have had an arrhythmia for less than 24 to 48 hours. However, Cardioversion does not cause “formation of a new clot.”
Table 1 is the summary of recommendations for electrical and pharmacological cardioversion of AF and Atrial Flutter [5].

Table 1: 2014 AHA/ACC/HRS Guidelines for Management of Patients with Atrial Fibrillation.
Download Provisional PDF Here
Article Type: Mini Review
Citation: Bagh RP, APRN, AGACNP-BC, FNP-BC (2017) Keys to a Safe and Effective Cardioversion. J Hear Health 3(3): doi http://dx.doi.org/10.16966/2379-769X.138
Copyright: © 2017 Bagh RP, APRN, AGACNP-BC, FNP-BC. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access