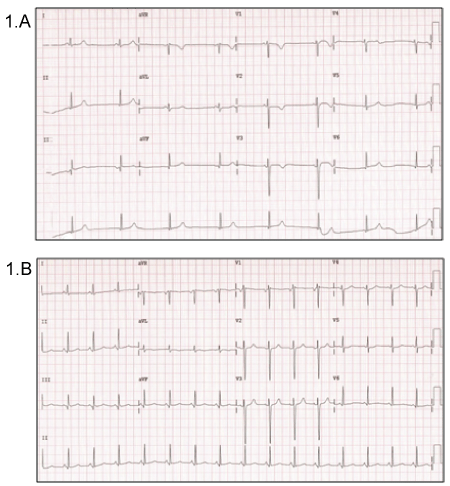
Figure 1: A) ECG 48 hours after cisplatin infusion; B) ECG at hospital discharge.


Martínez-Mateo V* Anguita MF Del Campo LC Paule-Sáncchez AJ
Cardiology Department, Hospital La Mancha Centro, Alcázar de San Juan, Ciudad Real, Spain*Corresponding author: Martínez-Mateo V, Cardiology Department, Hospital La Mancha Centro, Avenida Constitución s/n. 13600, Alcázar de San Juan, Ciudad Real, Spain, Tel: (34) 667982013; E-mail: virgiliomed@me.com
Cisplatin-induced cardiotoxicity is a well describe effect with a low incidence. Supraventricular arrhythmias and coro-nary artery disease are the main cardiac effects. Mechanism by cisplatin induced cardiac toxicity is not well understood. We present a case of asymptomatic transient sinus node dysfunction and decrease left ventricle systolic function as manifestation of cisplatin-acute cardiotoxicity in a 28-year-old female affected by Hodgkin lymphoma treated 6 years before with anthracyclines and mediastinal radiation. These are cisplatin effects rarely describe, being usually acute, reversible and transitoriness. Individual predisposition, administration in combination with other cardiotoxic drugs and previous exposition at anthracyclines and mediastinal radiation are the main risk factor to development of left ventricle systolic dysfunction. Although cisplatin is considered cardio-safe and no cardiac monitoring is generally recommended for its use, our report is important to remind to specialists that usually use cisplatin the importance of prevent, detect and monitor left ventricle systolic dysfunction in patients with these risk factors.
Cardiotoxicity; Sinus Node Dysfunction; Cisplatin; Chemotherapy; Taxane
Direct cardiac toxic effects of chemotherapy, including ischemia, arrhythmias and decrease in left ventricular (LV) function represent an important challenge in cancer survivors. Anthracyclines are the main drug that induce direct cardiotoxicity although other agents, like taxanes, can produce the same effect less frequently, especially when are used in combination with other cardiotoxic drugs or in patients with previous exposition at high doses of type-I cardio toxic agents [1]. Cisplatin, a taxane agent, is associated with several side effects such as myelotoxicity, gastrointestinal toxicity, neurotoxicity, ototoxicity, cardiotoxicity and nephrotoxicity. Cardiac toxicity incidence is low although it was well described, especially supraventricular arrhythmias during drug infusion and coronary artery disease in long-term [2]. We present a case of asymptomatic transient sinus node dysfunction and decrease LV systolic function as manifestation of cisplatin-acute cardiotoxicity.
We describe a case of a 28-year-old female affected by Hodgkin lymphoma. She had neither cardiovascular risk factors nor personal or family history of cardiac disease. Hodgkin lymphoma was initially diagnosed in thoracic localization and treated with chemotherapy (first line ABVD scheme with accumulated doses of Adriamycin 350 mg/kg/ m2) plus mediastinal and cervical radiotherapy (40 sessions). Actually, after a treatment free interval of seven years, she had disease recurrence in mediastinal localization with pulmonary extension. Therefore, a new cycle of chemotherapy was scheduled with second line DHAP (cisplatin, cytarabine and dexamethasone) scheme. The electrocardiogram (ECG) and transthoracic echocardiogram performed before chemotherapy administration were normal. After Forty eight hours of second cycle of chemotherapy, she was incidentally detected significant bradycardia at 40 beats per minute (bmp) during routine vital parameter examination. In physical exploration there was no evidence of congestive signs. The ECG (Figure 1A) showed a low atrial rhythm at 42 bpm with short PR interval and normal QRS morphology. An emergent 2-D transthoracic echocardiogram was performed detecting a mild dilated LV (telediastolic diameter 58 mm) with global hypokynesia and mild systolic dysfunction (LV ejection fraction [EF] 45% measured with Simpson biplane method). A moderate mitral regurgitation (MR) also was detected (Figure 2A). Serum electrolytes were within normal limits and cardiac troponins were undetectable. Patient was monitored and observed bradycardia improved gradually over thirty six hours to his normal baseline heart rate (HR) of 90 bpm (Figure 1B). Patient was discharged after forty eight hours of treatment with enalapril and spironolactone. Two weeks later patient continued asymptomatic and a new 2-D echocardiogram showed normalization of LV dimensions and LVEF (Left Ventricular Ejection Fraction) with MR resolution (Figure 2B). Despite this, enalapril and spironolactone were prescribed indefinitely and a third chemotherapy scheme with brentuximab vedotin was completed followed by successfully hematopoietic stem cell transplantation.

Figure 1: A) ECG 48 hours after cisplatin infusion; B) ECG at hospital discharge.
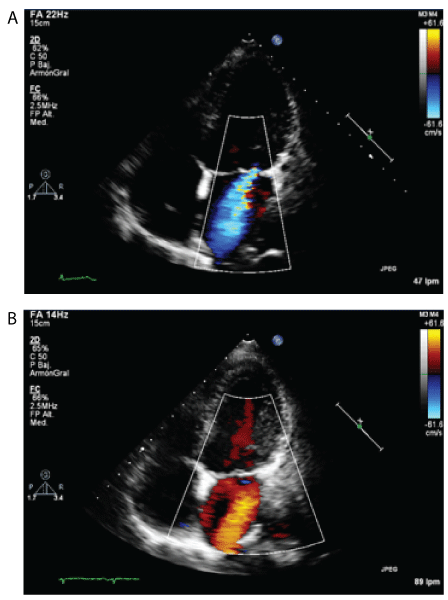
Figure 2: A) 2-D Transthoracic Echocardiographic image of the apical view after 48 hours of cisplatin infusion and B) two weeks later.
Cardiotoxicity secondary to cisplatin administration manifests as both delayed effects (mainly as chronic ischemic cardiomyopathy and arterial hypertension) and acute reactions (acute myocardial infarction and supraventricular arrhythmias) [1]. Mechanism by cisplatin induced cardiac toxicity is not well understood, although oxidative stress activation involving interference with mitochondrial metabolism and nuclear activity inducing apoptosis and cell death have been postulated [3]. To the best of our knowledge, our report is the first case where sinus node dysfunction and decrease of LV systolic function are described simultaneously.
Cisplatin-induced bradyarrhythmias during drug infusion has been reported occasionally in the past, although in the last years various case reports have been published [4-6]. It used to be secondary to sinus dysfunction although atrioventricular block also has been reported [7]. Usually, bradycardia episodes are asymptomatic and reversible and new cycles of cisplatin can administer safely [3].
On the other hand, cisplatin-induced LV systolic dysfunction usually is an acute adverse effect and used to be reversible after drug discontinuation [1,8]. Individual predisposition, administration in combination with other cardiotoxic drugs and previous exposition at anthracyclines and mediastinal radiation are the main risk factors for development of LVEF [1]. Despite patients affected usually have normal LVEF, association of cisplatin-induced cardiotoxicity with these risk factors might means that these patients have poor cardiac contractile reserve or subclinical forms of LV systolic dysfunction [9]. In view of this, although cisplatin is considered cardio-safe and no cardiac monitoring is generally recommended for its use, it is one of the important reminder to specialists that usually use cisplatin the importance of prevent, detect and monitor LV systolic dysfunction in patients with these risk factors.
Cisplatin-induced bradycardia and LV systolic dysfunction are unusual forms of cardiotoxicity with underlying me-chanisms not completely understood. Sinus node dysfunction is usually incidentally detected, while LV systolic dys-function used to be an acute adverse effect more frequent in patients with prior mediastinal irradiation or exposition to cardiotoxic drugs. Both conditions usually are reversible but require cisplatin discontinuation. Although our case is the first report where sinus bradycardia and LV dysfunction have been described simultaneously, and monitored HR in patients receiving cisplatin might be a simple marker to detect and treat LV systolic dysfunction.
Download Provisional PDF Here
Article Type: Case Report
Citation: Martínez-Mateo V, Anguita MF, Del Campo LC, Paule-Sáncchez AJ (2017) A Case Report of Cisplatin-Induced Cardiotoxicity: A Side Effect to Monitor Closely. J Hear Health 3(2): doi http://dx.doi. org/10.16966/2379-769X.136
Copyright: © 2017 Mateo VM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access