Abstract
Background: Cytomegalovirus enteritis (CMV) post coronary-bypass grafting has never been reported in an immunocompetent patient not on
steroids. Moreover, there are no cases in the literature where in CMV enteritis led to small bowel ischemia.
Case: An immunocompetent patient presented with NSTEMI, triple-vessel disease and severe left ventricular dysfunction. He underwent
urgent CABG. He developed multiple complications including gastrointestinal bleeding, acute abdomen and dialysis-resistant lactate acidosis.
He underwent laparotomy and resection of perforated small bowel.
Results: Histology revealed CMV enteritis.
Conclusions: CMV enteritis must be considered and actively sought in immunocompetent patients who develop GI complications post CABG.
Keywords
CMV enteritis; CMV enteritis post CABG; CMV enteritis in immunocompetent patient
Introduction
Despite improvements in surgical technique and perfusion technology,
the incidence and mortality from gastrointestinal (GI) complications
following cardiac surgery are reported to be up to 3.1% and 39% respectively
[1,2]. One of the GI complications is Cytomegalovirus (CMV) induced
bowel ischaemia. Symptoms and signs include abdominal pain, watery or
bloody diarrhoea, per rectum bleeding, obstruction, perforation and fistula
formation [3]. The severity and outcome of CMV enteritis depend on the
host’s immune status. Risk factors include acquired immune deficiency
syndrome (AIDS), organ recipients, immunosuppression, haematological
malignancies or chemotherapy [3-5]. While a case of CMV colitis has
been reported in a post coronary artery bypass grafting (CABG) patient
previously [5], this is the first histologically proven case of CMV small
bowel ischemia in a patient who was neither immunosuppressed nor on
steroid therapy preoperatively.
Case Report
In 2013, a 65 year old male presented with crescendo angina and a
delayed diagnosis of non-ST-elevation myocardial infarction (NSTEMI)
was made. Coronary angiogram showed triple vessel disease and ejection
fraction of 20%. Magnetic resonance imaging demonstrated some
myocardial reversibility. His past medical history included myocardial
infarction, hypertension, atrial fibrillation, and bowel polyps. One
month after admission, he underwent three-vessel CABG and MAZE
procedure. His three-vessel CABG was done without aortic crossclamp
and cardioplegic arrest to minimize the risk of ischaemia: the left internal
mammary artery was grafted to the left anterior descending artery, the
obtuse marginal and posterior descending artery then had venous grafts
fashioned. An intra-aortic balloon pump was inserted preoperatively.
His post-operative period was complicated: initially his chest was left
open because of the difficulty to be weaned off cardiopulmonary bypass
(CPB). As the heart appeared swollen with poor function, the patient
was placed on renal replacement therapy and once the oedema subsided
the chest was closed five days later. He underwent re-sternotomy with
evacuation of hematoma on day 16. A combination of low cardiac output
states, lower and upper GI bleeding requiring transfusions and multiple
infections meant on day 21 he was still intubated, ventilated and requiring
large amount of inotropes.
An oesophago-gastroduodenoscopy on day 21 and 29 showed erosive
gastritis. Discrete superficial prepyloric erosions were treated with
adrenaline and haemorrhagic gastritis managed with argon plasma
coagulation. Acute abdominal signs and symptoms, progressive from
day 21 to 34 ultimately culminated in abdominal distension, absent
bowel sounds and dialysis resistant lactate acidosis. Despite abdominal
CT showing dilated small bowel loops without a transition point or
features of ischemia, on day 34 he underwent laparotomy, resection of
an 82 cm length of necrotic, ulcerated and perforated small bowel and
ileostomy.
Subsequent to histopathology confirming CMV enteritis (Figure 1),
serologic tests were performed for CMV, Hepatitis (Hep) C and B and
Human immunodeficiency virus (HIV). Quantitative CMV Polymerase
Chain Reaction showed a result of 109000 IU/ml and 6 weeks later CMV
immunoglobulin IgM was negative but CMV IgG positive (>250 AU/ml).
Hep C PCR detected no viral load while HIV1 and HIV2 antibodies, p24
antigen, Hep C virus antibody, Hep B surface antigen and Hep B surface
antibody were all negative. He remained in ICU for 75 days and spent 56
days on a normal ward before discharge.
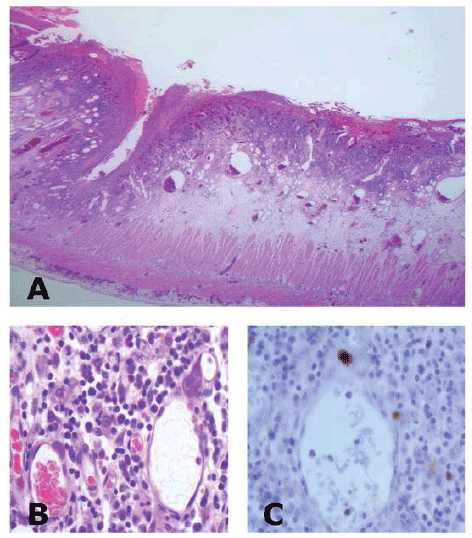
Figure 1: CMV enteritis histology
A- Extensive mucosal ulceration including a fissure ulcer (4X H&E).
B- Multiple CMV intranuclear inclusions seen within endothelial cells
(40X H&E).
C- Immunohistochemistry highlighting a CMV intranuclear inclusions.
Conclusion and Discussion
A MEDLINE literature search of relevant papers failed to identify
any other histologically proven case of post CABG CMV enteritis in a
patient who was immunocompetent and not on steroids preoperatively.
In one case, CMV colitis was attributed to concomitant use of long term
steroids for polymyalgia [5]. Another case, diagnosed on colonoscopy one
month after elective mitral and aortic valve replacement and CABG, does
not provide any information on the patient’s immune status or his/her
complications during intensive care unit (ICU) stay [2]. CMV disease is
often due to the reactivation of latent disease in immunosuppressed and
in up to 36% critically ill immunocompetent patients [6]. This reactivation
is thought to be due the dysfunction of cellular immune system which
causes shifting of T Helper 1 to T Helper 2 response or immune paralysis
[7]. In our case, CMV reactivation is thus likely to be due to the stormy
postoperative recovery.
Reports suggest improved survival rates can be achieved with early
diagnosis, aggressive antiviral therapy [5] and, if indicated, early surgical
intervention [8]. However, since patients likely to have GI complications
of CMV are sedated and ventilated post cardiac surgery, clinical
assessment and early diagnosis are a challenge. Indeed, in our case CMV
enteritis was diagnosed on histology after laparotomy and small bowel
resection. Consequently, we suggest firstly to consider CMV enteritis in
immunocompetent patients who have complicated ICU stay and signs and
symptoms such as abdominal pain, watery or bloody diarrhoea, bleeding
or obstruction; and secondly to have a high index of suspicion for CMV
enteritis in patients who are on steroids preoperatively.
Presentation
Presented at WSCTS, Edinburgh, 19-22 September 2015.
Download Provisional PDF Here
Article Information
Article Type: Case Report
Citation: Mbarushimana S, Farooqui A,
Ervine A, Parissis H (2016) A Novel Case of
Immunocompetent Cytomegalovirus enteritis
after Cardiac Surgery. J Hear Health 2(3): doi
http://dx.doi.org/10.16966/2379-769X.127
Copyright: © 2016 Simon Mbarushimana, et al.
This is an open-access article distributed under the
terms of the Creative Commons Attribution License,
which permits unrestricted use, distribution, and
reproduction in any medium, provided the original
author and source are credited.
Publication history:
Received date: 04 May 2016
Accepted date: 25
May 2016
Published date: 30 May 2016


