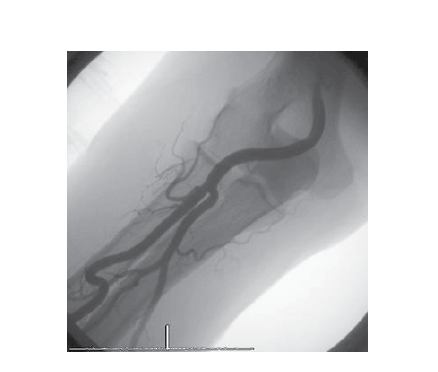
Figure 1: Tortuous radial artery.


Debabrata Dash*
SL Raheja Hospital, Mumbai, India*Corresponding author: Debabrata Dash, Senior Consultant Interventional Cardiologist, SL Raheja Hospital, Mumbai, India, Tel: +91-9833928466; Fax: +91-22-2444-2486; E-mail: dr_dash2003@yahoo.com
Cardiac catheterization via the transradial approach has become the “gold standard” in many centres because it allows quite early ambulation, decrease in bleeding and vascular access site complications. The growing experience has led to an understanding of the anatomical variants leading to technical difficulties and complications that can result from the transradial approach. The purpose of the present manuscript is to review these issues with practical preventive strategies and specific treatment.
Cardiac catheterization; Transradial approach; Complications
Following the report of the transradial (TR) approach for coronary angiography by Campeau in 1989 [1], the technique was extended to percutaneous coronary intervention (PCI) by Kiemeneij and Laarman since 1993 [2]. The reported advantages of the TR approach as compared to transfemoral technique include decreased bleeding and vascular access site complications [3,4], improved patient satisfaction, decreased length of stay and improved economic outlook [5-7]. From this perspective TR approach might be “gold standard” for PCI. However, it requires specific skill set and significant learning curve. In addition, radial artery spasm, arterial puncture failure, vascular anomalies, and failure to reach the ascending aorta are the obstacles that could impede regular use of this approach. This paper will review the anatomical variations and problems encountered during TR catheterization, prevention strategies and methods of treatment.
Tortuosity of radial artery is usually is recognized by difficulty in advancing the wire. It is most commonly seen in elderly smallframed women. It’s incidence is 2 to 6.1% in different angiographic and ultrasonographic studies [8]. In different studies, different definitions of tortuosity (presence of a bend or angulation of more than 45º to 90º ) have been used. But, more the angulation and less diameter, the procedure becomes increasingly difficult due to more chance of spasm (Figure 1). If radial artery (RA) is small and tortuosity segment is long, it should be crossed with a 0.025” or 0.032” J shaped hydrophilic guidewire or a 0.014” soft-tip coronary wire. A catheter should be negotiated over the wire using slow corkscrew movements. Direct push of the catheter should be avoided to prevent reactive spasm. Spasm in tortuous RA is a complex situation which may respond to repeat dose of spasmolytic cocktail. The balloonassisted technique (BAT) should be reserved for most difficult situations [9].

Figure 1: Tortuous radial artery.
It is an anatomical variation in which RA is palpable, but prevents insertion of sheath. Interventionists should adopt femoral or contralateral TR approach. It is associated with large radio-carpal artery in 0.1% cases. Puncture of radio-carpal artery is difficult due to its superficial nature and the artery should be held between two fingers because of its tendency to roll.
Various options are available for wire selection and fluoroscopic control when catheter is advanced from the radial artery to the ascending aorta. The 0.035” J-tip radiofocus wire with hydrophilic coating is the easiest to navigate, but may lead to perforation if not done under fluoroscopic guidance. However, the ordinary 0.035” J-tip spring wire presents no risk of perforation and is not easy to get across. When wire or catheter cannot be advanced, additional force should not be applied and angiographic evaluation of the area should be done to identify possible variations like radio-ulnar loop, a high radial artery take-off, a tortuous brachial artery, or an arterial lusoria (right retro-esophageal subclavian artery).
Radial artery loops represent redundancy in the vessel that may be present since birth or develops due to aging process. The reported incidence is around 0.8 to 2.3%, but when present it gives greatest challenge to the operator as it is associated with TR failure rate of 17% to 37% [8,10,11]. Larger the diameter of the loop and smaller the caliber of the artery, it is more difficult to negotiate. Alpha loop in antero-posterior (AP) view is mistaken for small aneurysm. In most cases it is associated with the persistence of remnant vessel which is too small to permit passage of a catheter even if the guide wire enters into it (Figure 2). Sometimes oblique angiographic views are required to define the exact anatomy. Other radial loops include S loop, proximal and distal omega loops (Figure 3). Some of these loops are very complex and require conversion to femoral or contralateral TR approach. Some of the solutions for crossing these are downsizing of guide catheter, use of 0.035” hydrophilic wire technique (Figure 4), downsizing the guidewire to 0.025”, the use of 0.014” coronary wire (Figure 5), coronary buddy wire technique and exchange with 0.035” J-tip spring wire, and also with low profile balloon support. The tip of the guidewire should be shaped to the angle of loop to facilitate crossing. Once the guidewire crosses the loop and it is parked as high as possible, the catheter is negotiated over it. In case of resistance, the operator can try pushing the catheter as far as possible into the loop, keeping the wire tip as high as possible (i.e., high brachial, axillary, or subclavian region) and pulling the entire assembly back. This maneuver opens up the loop and facilitates the advancement of the catheter. If the catheter is partly inside the loop, but has not crossed entirely, then the thin guidewire is exchanged for the standard 0.035” guidewire to provide extra support. A supper stiff guidewire is avoided unless the loop has been crossed and catheter tip is well into higher segment. BAT should be tried in case of failure of negotiation of a catheter through 360ºloop [9].
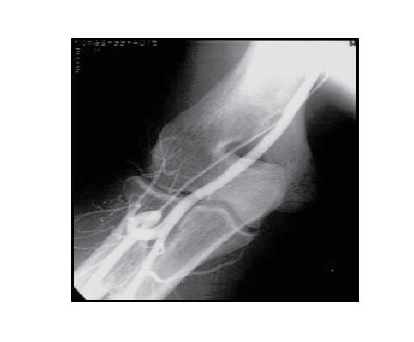
Figure 2: Alpha Loop with recurrent radial artery.
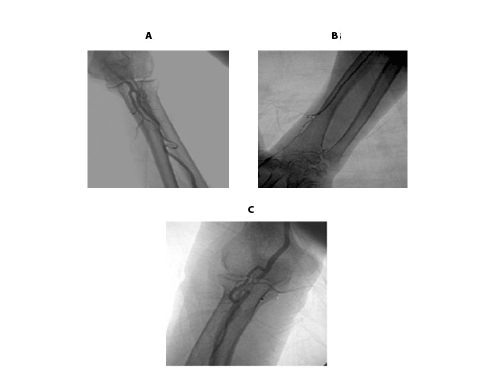
Figure 3:
A. S radial loop.
B. Proximal omega loop.
C. Distal omega loop.
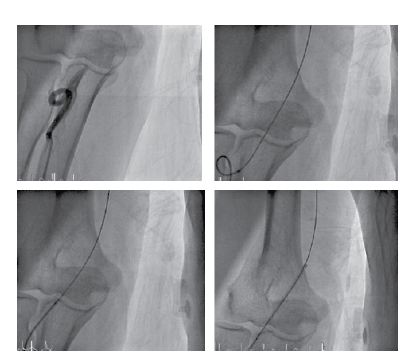
Figure 4: Overcoming of radial alpha loop with 0.034’’ hydrophilic wire.
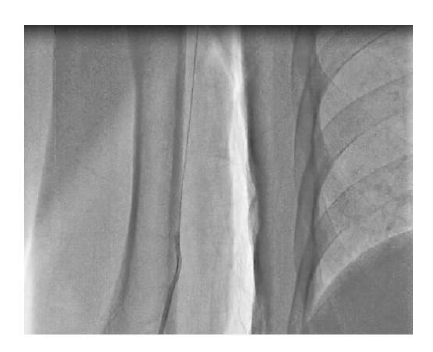
Figure 5: 0.014’’ Coronary angioplasty wire technique in negotiating the radial loop.
High origin of RA is rarely diagnosed as it really causes a problem if the artery is of sufficient caliber. The presence of atheromatous lesion is a rarity at this level. In majority of cases, the RA takes-off from brachial, and rarely from the axillary artery. The RA is rarely underdeveloped in this scenario. If the operator experiences unexpected resistance in the mid part of brachial artery after inserting the catheter, or find that torque transmission is impossible once the catheter is into the ascending aorta, this type of anatomical variation may be well culprit. As a counter measure, downsizing the guide catheter would probably allow better manipulation. If it fails, the interventionist should adopt contralateral TR or femoral approach.
The arteria lusoria or retro-esophageal right subclavian artery (RORSA) generally arises from the distal and posterior margin of the horizontal part of the aortic arch at its junction with the descending aorta, less frequently from the proximal descending aorta, and thus the catheter is preferentially oriented towards descending aorta. It is encountered in 0.4 to 2% in right TR approach [12-15]. It is generally not a problem while adopting left TR approach. In AP view, the catheter in the RORSA at its origin is oriented more towards the left than usual and engages the ascending aorta with a peculiar angulation (Figure 6). For diagnostic procedures, selective catheterization of left coronary artery (LCA) is easier with left Judkins (JL), internal mammary artery (IMA) and TIG catheters. For right coronary artery (RCA), the standard right Judkins (JR) catheter is the best followed by an Amplatz right (AR). For interventions in the left coronary system, an extra back up guide catheter is the first choice followed by an Amplatz left (AL) or a wider JL catheter (Figure 7). AR catheter is the first choice for right coronary interventions. JR or AL catheters may be used in case of failure. It is preferable to perform all catheter exchanges using a long exchange 0.035” wire [11].
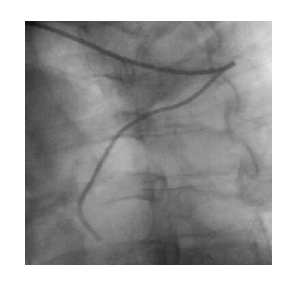
Figure 6: Left anterior oblique projection revealing the characteristic angle L of the catheter in arterial lusoria.
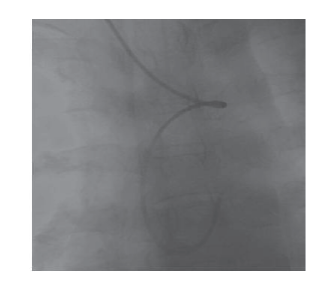
Figure 7: A loop was made using 0.25’’ Terumo to enter the ascending aorta with 6F EBU guide catheter in arteria lusoria-left anterior descending artery.
Both the catheters and guidewire should be withdrawn together as an assembly if they enter into descending aorta repeatedly. After asking the patient to take a deep breath, a 0.035” standard guidewire is pushed gently after patient takes deep breath. The catheter is then negotiated into the ascending aorta once the guidewire enter into it. If the guidewire remains in the descending aorta, the guide catheter is replaced with 5-F IMA diagnostic catheter and is placed in the descending aorta over the guidewire. Then previous maneuver is repeated which usually leads to successful entry into the ascending aorta. If IMA catheter fails, a 5-F Simmons-1 catheter can be used to enter the ascending aorta. If 0.035” standard guidewire repeatedly slips into the descending aorta, it should be replaced with 0.032” or a 0.025” hydrophilic guidewire that facilitates entry into ascending aorta even through challenging anatomy.
Once the standard 0.035” guidewire or the hydrophilic guidewire enters into the ascending aorta, it is replaced with a 0.035” super stiff guidewire and a loop is made. The catheter is slowly negotiated over this so that the assembly (catheter and guidewire) can traverse the aortic loop. By slowly pulling the guidewire slightly inside the mouth of the catheter and then pulling the assembly back facilitates cannulating the LCA. For cannulation of RCA, a slow and gentle clockwise rotation of the assembly is done.
There are many side branches at this level and it is very important to monitor progression of the wire with fluoroscopy to prevent its entry into mammary or vertebral artery. Manipulation of the wire and catheter with a deep inspiration generally allows easy access to the ascending aorta. Subclavian loops, either congenital or acquired, are more often observed in elderly, obese patients, and patients with hypertension. These could be 90º or Z shaped or very complex as depicted (Figure 8). Crossing could be facilitated by deep breathing combined with the use of 0.035” hydrophilic wire exchanged with 0.035” super stiff wire, parallel wire technique and the BAT [9].
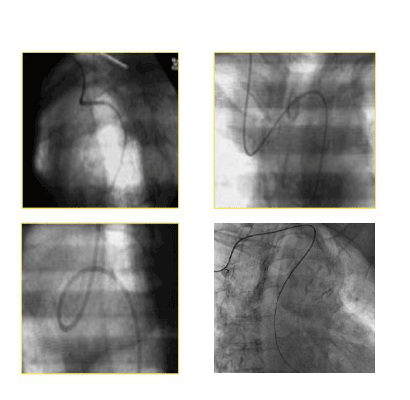
Figure 8: Negotiation of subclavian loops using 0.035 inch extra-stiff guidewire.
Knowledge of complications encountered during TR approach, their preventive strategies and methods of treatment are sin qua non of any TR program (Table 1).
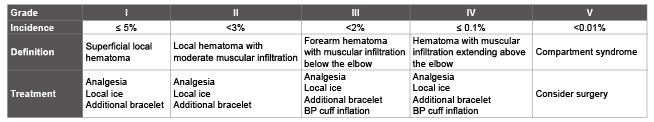
Table 1: The Effect of Kolkolis in reducing Blood Pressure along a duration (n=62)
Radial artery spasm (RAS) remains one of the major challenges of this approach and is the most common causes of procedural failure [16,17]. The reported incidence of RAS varies from 5% to 30% [16,18,19] with most recent literature reported spasm in 10% of cases. Predictors of spasm include younger age, female gender, diabetes, smaller wrist circumference and lower body weight, multiple catheter exchanges, larger sheath size and operator inexperience [16,19]. The vessel has a prominent medial layer largely dominated by α-1 adenoreceptor function [20]. Thus increased levels of circulating catecholamines are a cause of radial artery spasm. Pain from RAS increases vasomotor tone resulting in further spasm. In current practice, local anaesthesia and adequate sedation to control anxiety, careful puncture technique, antispasmodic “cocktails” and hydrophilic-coated sheaths are mainstay of RAS prevention (Figure 8) [19]. A preventive approach would improve procedural success and decrease procedure duration [18]. Intraarterial (IA) administration of antispasmodic medications has been shown to decrease the incidence of RAS (Figure 9) [21-23]. Calcium channel blockers, nitrates, local anaesthetics (e.g., lidicaine) and α-antagonists are most common medications [24] used for this purpose.
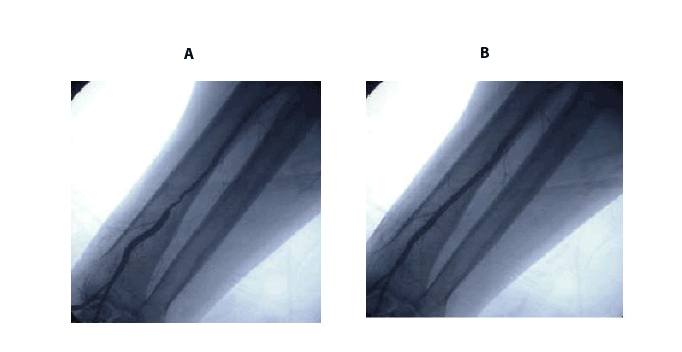
Figure 9:A. Radial artery spasm.
B. Normal of radial spasm after intrararterial nitrates and dilatiazem.
A cocktail composed of nitroglycerin 200 μg and verapamil 5 mg reduces RAS significantly as compared to placebo [22]. Verapamil 2.5 mg compared to phentolamine 2.5 mg is more efficacious in RAS prevention [25]. Adding verapamil 1.25 mg to nitroglycerin 100 μg does not reduce RAS significantly as compared to nitroglycerine alone [26]. Some have called for caution when using verapamil in patients with left ventricular dysfunction [27]. In another study, addition of nitroglycerin 100 μg, nitroprusside 100 μg, or both to a basic cocktail (unfractionated heparin 2500 U, lidocaine 20 mg, diltiazem 5 mg) did not show any benefit in RAS prevention [23]. Nicorandil 4 mg is equally effective in RAS prevention as compared to a cocktail composed of a small dose of verapamil 100 μg and nitroglycerin 200 μg [27]. Nicardipine is a second-generation dihydropyridine calcium antagonist that does not intrinsically decrease myocardial contractility or influence AV conduction and is useful in patients with depressed left ventricular function and bradycardia. Combination of both nitroglycerine (200 μg) and nicardipine (200 μg) has shown more powerful radial artery dilatation effect. While there is no consensus on the exact regimen or dose, the routine use of a “cocktail” containing a calcium channel blocker with or without a nitrate is an effective modality in decreasing the occurrence of RAS.
Hydrophilic-coated sheaths have been shown in various studies to decrease the incidence of RAS and improve patient comfort during sheath insertion and removal [16,28-30]. Sheath length, in spite of coating, does not have any significant effect on RAS reduction [16]. Once severe spasm occurs, it can be managed with repeated doses of IA vasodilators, increased analgesia and sedation. Deep sedation with propofol, axillary nerve block, or even general anaesthesia has been employed to allow sheath removal [31,32]. The operator should take utmost care not to forcibly remove equipment should resistance occur as this may cause transaction or eversion endarectomy of the radial artery [33].
Radial artery occlusion (RAO) after TR procedure is a well recognized complication occurring in 2% to 10% of patients [34]. It may be related to prolonged cannulation, small diameter of the radial artery, ratio of the radial artery diameter to sheath outer diameter, and inadequate anticoagulation during cannulation [34-37]. Other factors predictive of RAO could be low body weight, advanced age, female gender, and prolonged occlusive pressure while achieving hemostasis. It can be documented by abnormal Barbeau’s test, visible obstruction on two-dimensional ultrasound or absence of Doppler flow distal to puncture site. It is usually asymptomatic and benign. The presence of radial artery pulse does not rule out RAO due to the presence of collateral circulation though palmar arches which is an extremely protective mechanism. Although some operators emphasize the importance of normal Barbeau’s test [38], also referred to as the modified Allen’s test, this is controversial. However, patients with an abnormal modified Allen’s test demonstrate early evidence of hand ischemia with RAO compared to patients with a normal study [39]. Even if there exits case report of significant hand ischemia following TR intervention, RAO is usually clinically quiescent [40]. However, its presence makes repeat radial access difficult [41]. RAO is supposed to be thrombotic process the incidence of which is significantly reduced with adequate anticoagulation with UFH [34,42]. Its incidence decreased from 71% to 4.3% with the use of 5000 units UFH [42]. It can be administered intravenously (IV) or through IA with similar efficacy [43], because of burning sensation in the intraarterial (IA) route, some operators may choose the IV route in view of similar outocomes with regard to RAO [43]. Bivaluridin could be effective in preventing RAO in patients undergoing ad hoc PCI [44].
Catheter size is an important predictor of post-procedure RAO. Saito et al. [45] demonstrated that a ratio of the inner diameter of the radial artery to the sheath’s outer diameter of less than 1.0 predicts severe flow reduction after TR intervention. Use of a smaller size sheath and/or guide catheter may prevent RAO.
A strategy of “patent hemostasis” guided by plethysmography or mean arterial pressure (MAP) with use of a hemostasis device allowing adjustable levels of compression appears to reduce the incidence of RAO [46].
Even if it is usually asymptomatic, RAO may limit future TR catheterization. Low-molecular weight heparin has been found to resolve symptoms when RAO is symptomatic [47]. The patient suffering from hand ischemia could be treated with angioplasty [40]. Finally transient (1-h) ulnar compression has been described recently to recanalize acute RAO [48].
Hematoma is usually apparent during TR procedures due to the superficial course of radial artery. It rarely requires blood transfusion. TR approach does not impact non-access site bleeding that is more a function of patient and anticoagulation regimen [49]. Bertrand described a classification scheme of hematoma with Grade I and II being related to puncture site issues and Grade III and IV related to intramuscular bleeding [50] (Table 2).
Hydrophilic coated sheath reduces local hematoma non significantly as compared to uncoated sheath in one study [16].
Radial artery perforation is a rare complication but can lead to severe forearm hematoma if not treated promptly. Its reported incidence is 1% [51]. Forceful manipulation of the guidewire and catheters in elderly and hypertensive patient leads to perforation. Anatomical variations like tortuosity, radial loops, a high radial take-off and short ascending aorta increase the risk of perforation [52]. It should be suspected when there is resistance to guidewire navigation as well as with the patient’s complaint of pain. Usually radial artery perforation could be effectively managed without switching over to an alternate access site [53]. Several series have reported the safety of continuing the procedure either with use of a long sheath [52], guiding catheter [53] or prolonged (5 min) peripheral balloon inflation [54] to seal the perforation.
A compartment syndrome is rare but the most dreaded complication of radial artery hemorrhage, with an incidence reported be 0.004% in a large series [55]. Even a small volume of bleeding in the arm can lead to catastrophe given the limited free space in lower arm as compared to upper thigh. The diagnosis is based on the symptoms of acute forearm pain, swelling and tumefaction with disturbances in distal sensitivity and distal pallor. Direct measurement of compartment pressure confirms the syndrome while diagnosis is principally a clinical one [56]. Access site bleeding and hematoma, perforation or radial artery laceration could be common inciting factors for compartment syndrome. Most perforations are due to aggressive guidewire manipulation or excessive anticoagulation. It may not be detected during procedure because of temporary tamponade by the catheter shaft; as such it often manifests postprocedurally as a forearm hematoma. Conservative measures such as arm elevation, ice application and blood pressure cuff inflation may prevent progression of hematoma to compartment syndrome. However, emergency fasciotomy is required once elevated compartment pressures are documented.
Eversion of the radial artery has been reported with sheath removal after severe RAS. The interventionist must employ various therapies to counter the vasospasm, including sedation and local and systemic delivery of antispasm medication.
Catheter entrapment occurs due to severe RAS or aggressive torquing of the catheter. Aggressive antispasm therapy and general anaeasthesia allows the catheter removal. If entrapment is due to kinking or tortuosity, undoing the kink with fluoroscopic guidance or negotiating a wire to straighten the tortuous segment almost always allows catheter removal [24].
This is a rare complication with an incidence of less than 0.1% as reported in one series [57]. It presents with pulsatile swelling with or without tenderness several days to weeks after the procedure. It is caused by penetrating injury of the arterial wall during cannulation with resultant hemorrhage and hematoma and is associated with multiple puncture attempts and aggressive anticoagulation therapy. Diagnosis is usually confirmed with Doppler ultrasound. Pseudoaneurysm is successfully treated with prolonged compression, is indicated if identified soon after the procedure. However, thrombin injection and surgical correction may be required in some cases.
There are reports showing an association between hydrophilic sheaths and granulomatous foreign body reaction at the access site. These sterile granulomas, often confused with infected pseudoaneurysm, results in unnecessary surgery. Typically occurring 2 to 3 weeks after the procedure, these are most likely owing to the sheath coating. These granulomas are self-limiting and are managed conservatively unless and until symptomatic [58].
Rarely prolonged aggressive haemostatic compression at the access site may lead to vascular and/or neurologic complications, including persistent pain. There may be a chronic regional pain syndrome characterized by hand swelling, allodynia, paresthesia, and the limited range of motion of interphalangeal, metacarpophalangeal, and wrist joints [59]. Sympathetic blockade, analgesics and physical therapy are potential management options.
The feasibility and safety of TR approach adopted by interventionists is supported by robust data. However, these exits many real and perceived barriers for the operators to switch into this approach. The ability to recognize and troubleshoot anatomical variations and various complications unique to TR approach is fundamental in avoiding unnecessary morbidity and mortality. The field has undergone rapid transformation and would likely to improve further with experience, equipment modifications and pharmacological treatment. TR access offers the operators a unique opportunity to provide optimal care with reduced risk.
Download Provisional PDF Here
Article Type: Review Article
Citation: Dash D (2016) Troubleshooting in Transradial Catheterization: The Lessons Learnt so Far. J Hear Health 2(3): doi http://dx.doi. org/10.16966/2379-769X.126
Copyright: © 2016 Dash D. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access