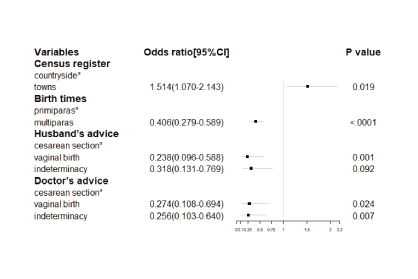
Figure 1: Multi-factors analysis.


Dihui Hu Longfei Li Xiaoni Zhong
Chongqing Medical University, Yuzhong District, Chongqing, China*Corresponding author: Xiaoni Zhong, Chongqing Medical University, Yuzhong District, Chongqing, China, E-mail: zhongxiaoni@cqmu.edu.cn
Background: The abnormally high cesarean section rate results from complex factors, it is an urgent issue in medical field. The purpose of this study is to provide the evidence for the formulation of policies to reduce cesarean section rate from the social aspect of pregnant women themselves and people around them.
Methods: This study conducted a follow-up survey of women entering the perinatal period in four districts and counties of Chongqing, explored the relationship between demography, pregnancy maternal history, behavioral medical characteristics, crowd’s willingness (advice) and final birth outcomes.
Results: The study showed that Chinese towns had a higher cesarean section rate than in rural areas; primiparas had a higher cesarean section rate; pregnant women are more likely to choose what their husbands or doctors recommend.
Conclusions: The study suggests that China should develop medical services in rural and urban areas in a balanced manner, popularize the knowledge of childbirth, more education pregnant women and the surrounding people (especially their spouses) to treat cesarean section correctly, strengthen the management of doctors, establish relevant system, and standardize the behavior makes it strictly according to the associated medical indications of cesarean section surgery.
Cesarean section, that is, birth by surgical operation, it is usually required when vaginal birth may threaten the lives or health of mothers and newborns [1]. With the development of medical and health services, the use of cesarean section has been more and more widely, and a survey conducted in 121 countries showed that the global cesarean section rate increased by 12.4% from 1990 to 2014 [2]. In terms of physiology, cesarean section can avoid postpartum urinary incontinence [3], reduce the maternal and fetal unexplained or unexpected mortality [4,5]; Psychologically, cesarean section in a way can ease the fear and anxiety during women’s birth. However, relevant studies have shown that excessive use of cesarean section does not bring more benefits to the life and health of mothers and fetuses [6-8]. In 2015, World Health Organization (WHO) pointed out that cesarean section rate should be controlled between 10% and 15% [9]. According to Hall et al., [10] the maternal mortality rate of cesarean section is about 9 times higher than that of vaginal birth, and postoperative recovery time of cesarean section is longer, which may cause complications such as tearing and massive hemorrhage [11,12]. Inappropriate cesarean section can have a serious impact on the lungs of newborns, such as respiratory distress [13]. The West China School of Medicine, Sichuan University collected and analyzed 7 million birth data from 2012 to 2016 in China, and found that the cesarean section rate in China was 41.1%, which was far beyond the range regulated by WHO. The data of Chongqing Health Information Center showed that the cesarean section rate in Chongqing was more over 40% in 2015. The abnormally high rate of cesarean section has become an urgent issue in the field of public health. To this end, from June 2018 to January 2019, 817 pregnant women (>28 weeks) without indications of cesarean section were enrolled in the study cohort, investigated the demography, pregnancy maternal history, behavioral medical characteristics, and Crowd’s willingness (advice), and explored the relationship between them and the final birth outcomes. The purpose of this study was to provide the evidence for the policy of reducing cesarean section rate from the social level of pregnant women themselves and surrounding people, popularize the knowledge of childbirth, guide the society to treat and use cesarean section correctly.
In this study, 817 perinatal women (> 28 weeks) were selected as subjects from June 2018 to January 2019. According to the regional economic situation in Chongqing, China, maternal and child health care centers were randomly selected from four districts and counties including Yubei District, Jiangjin District, Dianjiang County and Yunyang County (Economic situation: Yubei District >Jiangjin District >Dianjiang County >Yunyang County). Before involving in this study, all subjects were screened according to criteria as followed:
Inclusion criteria: Signed informed consent; the first pregnancy test fitted the basic pregnancy conditions; willing to accept follow-up arrangements under guidance; willing to take part in the questionnaire during the whole pregnancy.
Exclusion criteria: had a history of cesarean section; unfitted the medical indications of cesarean section; the researchers believed that the follow-up or assessment of volunteers might be affected; those who were unable or unwilling to provide informed consent or failed to comply with the test requirements.
In this study, dependent variable were final birth outcome (cesarean section or natural birth), independent variables mainly included demography (age, nationality, census registration, education, occupation, monthly income and insurance), pregnancy maternal history (pregnancy times, birth times, spontaneous abortion history, induced abortion history and family history), behavioral medical characteristics (childbirth knowledge, family care, independence, social support, anxiety, depression and stress), and crowd’s willingness(advice) (pregnant woman’s willingness, advices from husbands, parents, parents-in-law, friends and doctors).
General questionnaires were used in the study of behavioral medical characteristics such as family care, independence, social support, anxiety of women, and so on. The independence questionnaire in The Sixteen Personality Factor Questionnaire (16PF, which was completed by American Professor R.B. Catttell and others) was used and the independence was divided into < 8, 8-18 and ≥ 18 according to the actual situation of Chinese women [14-16]; Family APGAR Index(APGAR, designed by doctor Smilkstein, from University of Washington in Seattle, US) was used and family care level was divided into 0-3, 4-6 and 7-10 [16,17]; Pregnancy stress scale (invented by Zhanghui Chen [18] and others) was used, pregnancy stress was divided into no stress(0), mild stress(0.01-1), moderate or severe stress (>1) with the reference of Yingli Pan and others’ [19] methods; Hamilton Anxiety Scale [20] (HAMA, designed by Hamilton in 1995) was used and anxiety was divided into no anxiety (<7) and anxiety ( ≥ 7) [16]; Self-Rating Depression Scale (SDS, invented by Zung) was used to measure depression [21], it was divided into no depression (≤ 53) and depression (>53) [16,22,23] according to the actual situation of Chinese women. The degree of social support refers to the scale of Social support compiled by Shui-yuan Xiao [24] in 1994, and was divided according to the median score; scale of childbirth knowledge was made according to the relevant literature [25] and combined with clinical knowledge, the median score was used as the cut-off point.
In this study, Epidata 3.1 was used to double-input the data, and SAS 9.4 was used to analyze the data. There were two steps for data analysis: first, single-factor analysis was performed by using Person χ2 to study the relationship between the birth mode and demography, pregnancy maternal history, behavioral medicine and crowd’ willingness (α=0.05); then the significant variables of single-factor analysis (p<0.05) were used to carry out multi-factors logistic stepwise regression with the inclusion criteria of 0.05 and the exclusion criteria of 0.10 to screen out the factors related to the mode of birth.
The effective data of follow-up survey was 672 cases, the effective rate was 82.25%. The psychological scales involved in the questionnaire were general scales and had good reliability and validity.
The study of demographic characteristics (Table 1) showed that there was a significant connection between census registration and cesarean section, and the cesarean section rate of urban residents was 39.62%, which was significantly higher than that of rural residents (p<0.0122). In this survey, the age distribution of the subjects was between 16 and 44 (25.87 ± 4.35), and there was no significant connection between age, nationality, education, income, and insurance condition and cesarean section (P>0.05).
| Characteristic | Vaginal birth (N=430) | Cesarean section (N=242) | P value |
| Age | 0.3306 | ||
| non-advanced maternal age (<35) | 412(64.48) | 227(35.52) | |
| advanced maternal age (≥ 35) | 18(54.55) | 15(45.45) | |
| Nationality | 0.2507 | ||
| Han | 419(63.68) | 239(36.32) | |
| Minority | 11(78.57) | 3(21.43) | |
| Census register | 0.0122 | ||
| Towns | 253(60.38) | 166(39.62) | |
| Countryside | 177(69.96) | 76(30.04) | |
| Education | 0.3842 | ||
| Middle school and below | 141(67.79) | 67(32.21) | |
| High school/vocational high school/technical secondary school | 126(62.69) | 75(37.31) | |
| Junior college/undergraduate | 163(61.98) | 100(38.02) | |
| and above | |||
| Occupation | 0.6955 | ||
| Government departments and institution employees | 73(66.36) | 37(33.64) | |
| Enterprise staffs (private/foreign companies etc.) | 77(61.60) | 48(38.40) | |
| Self-employed | 34(58.62) | 24(41.38) | |
| Farmers/housewives/unemployed or waiting for employment | 246(64.91) | 133(35.09) | |
| Monthly income | 0.76 | ||
| ≤ 5000 | 291(64.96) | 157(35.04) | |
| 5001-10000 | 110(62.15) | 67(37.85) | |
| >10000 | 29(61.70) | 18(38.30) | |
| Insurance | 0.5963 | ||
| Doesn’t have (at own expense) | 176(65.19) | 94(34.81) | |
| Have | 254(63.18) | 148(36.82) |
Table 1: Relation between Demographic Characteristics and Cesarean Section.
The study of pregnancy maternal history (Table 2) showed that the cesarean section rate of primiparas was 40.28%, and that of multiparas was 24.35%. The rate of cesarean section in primiparas was significantly higher than that in multiparas, there was relativity between parity and cesarean section (P<0.0001). There was no relativity between gravidity, spontaneous abortion, induced abortion, family history and cesarean section (P>0.05).
| Characteristic | Vaginal birth (N=430) |
Cesarean section (N=242) |
P value |
| Pregnancy times | 0.0693 | ||
| First pregnancy | 182(60.26) | 120(39.74) | |
| Non first pregnancy | 248(67.03) | 122(32.97) | |
| Birth times | <.0001 | ||
| Primiparas (0 time) | 256(57.92) | 186(42.08) | |
| Multiparas (>0 time) | 174(75.65) | 56(24.35) | |
| History of spontaneous abortion |
0.2213 | ||
| Yes | 28(56.00) | 22(44.00) | |
| No | 402(64.63) | 220(35.37) | |
| History of Induced abortion |
0.7129 | ||
| Yes | 145(63.04) | 85(36.96) | |
| No | 285(64.48) | 157(35.52) | |
| Family history | 0.5775 | ||
| Yes | 19(59.38) | 13(40.63) | |
| No | 411(64.22) | 229(35.78) |
Table 2: Relation between pregnancy maternal history and cesarean section.
The study of behavioral medical characteristics included childbirth knowledge, family care, social support, independence, pregnancy stress, anxiety and depression. This survey (Table 3) showed that there was no relativity between different behavioral medical characteristics and cesarean section (P>0.05) in women entering perinatal period (>28 weeks).
| Characteristic | Vaginal birth (N=430) | Cesarean section (N=232) | P value |
| Childbirth knowledge | 0.2102 | ||
| ≤ P50(≤ 23) | 229(61.89) | 141(38.11) | |
| >P50(>23) | 201(66.56) | 101(33.34) | |
| Family care | 0.3992 | ||
| Low score (0-3分) | 17(65.38) | 9(34.62) | |
| In-between (4-6分) | 112(68.29) | 52(31.71) | |
| High score (7-10) | 301(62.45) | 181(37.55) | |
| Independence | 0.2162 | ||
| Low score (<8) | 13(48.15) | 14(51.85) | |
| In-between (8-18) | 413(64.63) | 226(35.37) | |
| High score (≥18) | 4(66.67) | 2(33.33) | |
| Pregnancy stress | 0.31 | ||
| No stress (0) | 36(58.06) | 26(41.94) | |
| Mild stress (0.01-1) | 350(65.42) | 185(34.58) | |
| Moderate /severe stress (>1) | 44(58.67) | 31(41.33) | |
| Anxiety | 0.6198 | ||
| Without anxiety (<7) | 266(64.72) | 145(35.28) | |
| With anxiety (≥7) | 164(62.84) | 97(37.16) | |
| Depression | 0.3568 | ||
| Without depression (≤53) | 428(64.17) | 239(35.83) | |
| With depression (>53) | 2(40.00) | 3(60.00) | |
| Social support | 0.2307 | ||
| ≤P50(≤37) | 248(65.96) | 128(34.04) | |
| >P50(>37) | 182(61.49) | 114(38.51) |
Table 3: Relation between different behavioral medical characteristics and cesarean section.
A study of crowd’s willingness(advice) (Table 4) showed that the rate of women who were willing to choose cesarean section (54.84%) were significantly higher than those who chose natural or unspecified birth mode (31.16%, 39.93%) (p=0.0058); the rate of cesarean section suggested by Husband (p=0.0003), parents (p=0.0154), inlaws (p=0.0017), friends (p=0.0357) and doctors (p=0.0006) was significantly higher than that of women who deliver naturally or in an unspecified manner. There was relativity between crowd’s willingness (advice) and the outcome of childbirth.
| Characteristic | Vaginal birth (N=430) |
Cesarean section (N=242) | P value |
| Pregnant woman’s willingness | 0.0058 | ||
| Vaginal birth | 243(68.84) | 110(31.16) | |
| Cesarean section | 14(45.16) | 17(54.84) | |
| Unclear | 173(60.07) | 115(39.93) | |
| Husband’s advice | 0.0003 | ||
| Vaginal birth | 186(68.63) | 85(31.37) | |
| Cesarean section | 9(31.03) | 20(68.97) | |
| Unspecific | 235(63.17) | 137(36.83) | |
| Parent’s advice | 0.0154 | ||
| Vaginal birth | 240(67.23) | 117(32.77) | |
| Cesarean section | 6(35.29) | 11(64.71) | |
| Indeterminacy | 184(61.74) | 114(38.26) | |
| Parent-in-law’s advice | 0.0017 | ||
| Vaginal birth | 207(68.77) | 94(31.23) | |
| Cesarean section | 5(29.41) | 12(70.59) | |
| Indeterminacy | 218(61.58) | 136(38.42) | |
| Friend’s advice | 0.0357 | ||
| Vaginal birth | 193(67.01) | 95(32.99) | |
| Cesarean section | 12(42.86) | 16(57.14) | |
| Indeterminacy | 225(63.20) | 131(36.80) | |
| Doctor’s advice | 0.0006 | ||
| Vaginal birth | 183(67.03) | 90(32.97) | |
| Cesarean section | 8(29.63) | 19(70.37) | |
| Indeterminacy | 239(64.25) | 133(35.75) |
Table 4: Relation between different crowd’s willingness (advice) and cesarean section.
The results of a multi-factors survey (Figure 1) showed that when the dependent variable was the outcome of the birth (0 for vaginal birth and 1 for cesarean section), according to the test level of α = 0.05, census registration, parity, husband and doctor’s advice is related to the outcome of childbirth. The odds ratio of cesarean section in towns was 1.514 times higher than that in rural areas (P=0.0192, OR=1.514, 95% CI: 1.070-2.143); the rate of cesarean section was 0.406 times higher than that of primiparas (p<0.0001, OR=0.406, 95% CI: 0.279-0.589); the husband’s advice of vaginal birth was 0.238 times higher than cesarean section (P=0.0013, OR=0.238, 95% CI: 0.096-0.588); doctor’ advice of vaginal birth and indeterminacy mode was 0.274 times and 0.256 times higher than that of cesarean section (p=0.0241, OR=0.274, 95% CI: 0.108-0.694; p=0.0066, OR=0.256, 95% CI: 0.103-0.640).

Figure 1: Multi-factors analysis.
Among the 672 pregnant women in the follow-up survey, the final outcome of cesarean section was 242, the rate of cesarean section as high as 36.01%, which was consistent with the current situation of China’s cesarean section rate survey. According to Li et al., in 2014, the cesarean section rates in Jilin, Beijing and Shanghai were 62%, 43% and 52% [26]. According to Liang et al. (2018), data from more than 6 million newborns in 438 large hospitals showed that the overall cesarean section rate in Chinese hospitals was 41% [14].
In terms of demography, the cesarean section rate in urban areas is higher than that in rural areas. This may be related to China specific urban and rural differences. Liang et al., in the decisive factors of cesarean section, pointed out that the rate of cesarean section in Chinese cities was higher than that in rural areas, however there is no analysis of the specific reasons [14]. Yue et al. mentioned in detail in the study were that the differences of cesarean section rates between urban and rural areas in China are mainly influenced by social and iatrogenic factors [27]. The social factor is mainly the rising consciousness of legal protection of pregnant women and their families in urban areas, but they do not have a comprehensive understanding of harm degree of cesarean section. Once pregnant women or their families put forward this will, it is very difficult for doctors to intervene; in addition, the quality of pregnant women’s lives in cities and towns is higher, and their tolerance and endurance to labor pain are lower than those in rural areas [28,29]. The iatrogenic factor lies in a better urban economy level, but people are lack of understanding of childbirth knowledge and more likely to cause a fetal macrosomia; moreover, due to a high level of medical treatment in cities and towns, the abnormal conditions can be quickly detected in the delivery process, thus to ensure the safety, pregnant women and their families will not try to give birth on trial [30-33].
The number of births is also significantly associated with cesarean section. The cesarean section rate of primiparas is much higher than that of multiparas. Because of the experience of delivery, the multiparas have a correct understanding of the pain of vaginal delivery, they treat vaginal delivery as a natural process, and have more confidence in vaginal delivery. However, the primiparas are lack of confidence in vaginal delivery, know little about cesarean section and overestimate the pain in childbirth, and are more prone to fear and anxiety in the face of birth, which leads to overly high cesarean section rate in primiparas. Osis et al. had a similar conclusion in a qualitative interview research [34]. Heinberg et al. pointed out that parturients’ choices won’t increase cesarean section rate under conditions of no complications [35]. Heffner et al. noted that multiparas have a higher cesarean section rate but only when pregnant women are older than 40 and pregnancy week is over 41 [36]. In this study, the respondents were basically under 40 years old and only five pregnant women who were older than 40 were investigated, which explains this contradiction.
The husband’s advice is also positively related to the outcome of the final delivery. In a randomized controlled intervention trial, Sharifirad et al. found that husband’s knowledge and attitude would seriously affect the willingness of pregnant women [37], and the willingness of pregnant women had a positive correlation with cesarean section rate [38]. In our univariate study, there was a positive correlation between the choice of the pregnant women and the final delivery outcome, which was consistent with the study above [39].
Under the premise that all the pregnant women in this followup study had no medical indication of cesarean section, the doctor’s suggestion was closely related to it. Compared with vaginal delivery, cesarean section is more convenient and time-saving [40], generally it only takes 45 minutes to one hour [1]. Vallejos’ survey showed that 35% of obstetricians and gynecologists performed cesarean section for convenience, 17.3% of obstetricians and gynecologists choose cesarean section only to save time. Another reason may be economic benefit [41]. A survey conducted in Guangzhou showed that cesarean sections have higher average hospitalization costs than vaginal birth [42]. Mairead Black and Sohinee Bhattacharya pointed out that even without clinical indications, some obstetricians in China still perform cesarean sections because of economic incentives [43].
The results of this follow-up study shows that the cesarean section rate of pregnant women living in towns is higher than that in rural areas, the rate of cesarean section in primiparas is higher than that in parturients, and both husband and doctor’s advices are positively related to birth outcome, in other words, pregnant women are more likely to choose what their husbands or doctors recommend. This suggests that we should develop medical services in both rural and urban areas in a balanced manner, popularize knowledge about childbirth, educate pregnant women and people around them, especially their spouses, to treat cesarean section correctly, strengthen the management of doctors, establish relevant system, and standardize the behavior to perform cesarean section strictly according to the medical indication of cesarean section.
The authors promised that there were no potential disputes of interest. The study was funded by the national natural science foundation of China for the project (Study on the Public Propagation Model for Generative Mechanism and Regularity of Cesarean Birth Behavior, Project No. 71573027). In addition, we were very grateful to all the medical staff and respondents who participated in this work.
Download Provisional PDF Here
Article Type: RESEARCH ARTICLE
Citation: Hu D, Li L, Zhong X (2019) Cesarean Section in Relation to Demography, Pregnancy Maternal History, Behavioral Medical Characteristics, Crowd’s Willingness (Advice): A Prospective Follow-Up Study. J Epidemiol Public Health Rev 4(1): dx.doi.org/10.16966/2471- 8211.169
Copyright: © 2019 Hu D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access