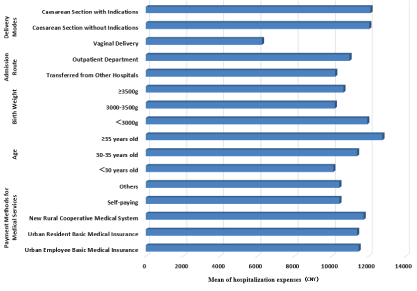
Figure 1: Bar chart of hospitalization expenses for different characteristics.


Ting Zhang1,2,3 Zhong Xiaoni1,2,3* Zhang Yingying1
1School of public health and management, Chongqing Medical University, China*Corresponding author: Zhong Xiaoni, Professor, Supervisor, Department of Epidemiology and Health Statistics, School of Public Health and
Management, Chongqing Medical University,Chongqing, China, Tel: 13308368059; E-mail: 1932352920@qq.com
Objective: To understand the structure and influencing factors of hospitalization costs of pregnant women by analyzing the data collected from a tertiary teaching hospital in China.
Methods: According to the medical records of all pregnant women who had delivery in this hospital from 2014-2016, we divided them into different groups and analyzed the basic information of pregnant women; hospitalization costs structure as well as its influencing factors.
Results: The median hospitalization costs for pregnant women who had caesarean section, with or without indications, are 11483.94 yuan and 11109.15 yuan respectively, and the median length of stay of them are both 4 days, about twice as much as that of pregnant women who had vaginal delivery with median costs 5865.24 yuan and length of stay 2 days. According to multi-factor analysis, length of stay, different delivery modes, age and payment methods are main influencing factors of hospitalization costs.
Conclusions: This study highlights the critical need to reduce the rate of caesarean section without indication. To this end, caesarean section should be done only when there is a medical indication, which can not only improve maternal and perinatal outcomes, but also make medical costs more reasonable.
Delivery modes; Hospitalization costs; Influencing factors
Recent years have seen the rising rates of caesarean section worldwide, especially in China. Of rates of caesarean section in Asian countries, China ranked the highest with a rate of caesarean section of 46.2%, which was much higher than 10%- 15% recommended by WHO, according to a WHO survey in Asia in 2010 [1]. Social factors, or caesarean section without medical indications, had contributed to a worldwide increase in the rate of caesarean section [2]. The rapid increase in the rate of caesarean section did not necessarily bring improvement in maternal and perinatal health, and had placed financial burden on both individual and society.
By systematically analyzing the relevant data of pregnant women from 2014 to 2016 in a tertiary teaching hospital, the purpose of this study is to, on the one hand, analyze the hospitalization costs structure of pregnant women and its influencing factors, so as to provide guidance for the control of medical costs, and to, on the other hand, find out the problems within and put forward some possible advices for strengthening the management on medical expenses and services, and for a better use of the limited health resources.
According to the International Classification of Disease-10 codes(ICD-10), the data of all pregnant women from 2014- 2016 in the tertiary teaching hospital, whose disease codes were started with “O”, which represents diseases related to pregnancy, childbirth and the puerperium, were initially collected. Of the obtained data, pregnancy with abortive outcomes started with “O0” in disease coding, threatened abortion (hemorrhage specified as due to threatened abortion) started with “O20”, excessive vomiting in pregnancy started with “O21”, and complications predominantly related to the puerperium started with “O85-O92” were excluded. From the processed data, cases of 15631 women with singleton pregnancies, whose codes, according to ICD-9-CM, represent obstetrical conditions and were started with “72-74” and with “75”, were included in the study [3]. 3397 of the total cases were vaginal delivery, 3814 were caesarean section without medical indications and 8420 were caesarean section with medical indications. The data of these pregnant women included information such as demographic characteristics, payment methods for medical services, admission route and hospitalization costs. The hospitalization costs consist of costs in general medical services, diagnosis, treatment and rehabilitation, traditional Chinese medicine, western medicine, blood and related products, consumable items and other things.
With data of pregnant women collected from Hospital Information System (HIS), SAS 9.2 was applied to conduct statistical analysis. Rates and ratios were used in descriptive statistics. Wilcoxon Rank Sum (WRS) test and Multiple Linear Regression (MLR) analysis were applied in univariate analysis and in multivariate analysis respectively with α = 0.05(two-sided test).
In the total 15631 deliveries of pregnant women, there were 3397 vaginal deliveries (21.73%) and 12234 caesarean sections (78.27%) including 3814 caesarean sections without medical indications (24.40%) and 8420 caesarean sections with medical indications (53.87%). In caesarean section with indications, there was no statistical difference between caesarean section with absolute indications (including fetal disease, breech, umbilical cord around the neck, placental abruption, placenta praevia, prolonged pregnancy, etc.) and section with relative indications (including uterine scar, twin pregnancy, etc.). Table 1 and table 2 show that pregnant women with different delivery modes were mainly aged below 30; the proportion of newborns whose weight were 3500g or more than 3500g delivered by caesarean section without indications was higher than that of newborns delivered vaginally or by caesarean section with indications; Among pregnant women with different modes of delivery, the proportion of those admitted from outpatient department was the largest; median length of stay of pregnant women who had caesarean section with or without indications was longer than that of pregnant women who had vaginal delivery.
| Features | Delivery modes | ||||||
| Vaginal Delivery (3397) | Caesarean Section without Indications (3814) | Caesarean Section with Indications (8420) | |||||
| n | % | n | % | n | % | ||
| Payment | Urban Employee Basic Medical Insurance | 782 | 23.02 | 624 | 16.36 | 2684 | 31.88 |
| Methods for Medical Services | Urban Resident Basic Medical Insurance | 367 | 10.8 | 474 | 12.43 | 1053 | 12.51 |
| New Rural Cooperative Medical System | 23 | 0.68 | 27 | 0.71 | 60 | 0.71 | |
| Self-paying | 737 | 21.7 | 830 | 21.76 | 1820 | 21.62 | |
| Others | 1488 | 43.8 | 1859 | 48.74 | 2803 | 33.29 | |
| Age | <30 | 2473 | 72.8 | 2050 | 53.75 | 4407 | 52.34 |
| 30-35 | 760 | 22.37 | 1229 | 32.22 | 2730 | 32.42 | |
| ≥35 | 164 | 4.83 | 535 | 14.03 | 1283 | 15.24 | |
| Birth Weight | <3000 | 804 | 23.67 | 807 | 21.16 | 2832 | 33.63 |
| 3000-3500 | 1631 | 48.01 | 1581 | 41.45 | 3029 | 35.97 | |
| ≥3500 | 962 | 28.32 | 1426 | 37.39 | 2559 | 30.39 | |
| Admission Route* | Transferred from Other Hospitals | 993 | 29.25 | 562 | 14.75 | 1400 | 16.65 |
| Outpatient Department | 2402 | 70.75 | 3248 | 85.25 | 7009 | 83.35 | |
Table 1: Basic information of Pregnant Women with Different Delivery Methods.
| Delivery Modes | Mean ± Standard deviation | Median | Maximum | Minimum |
| Vaginal Delivery | 2.42 ± 1.34 | 2 | 16 | 1 |
| Caesarean Section without Indications | 4.26 ± 1.74 | 4 | 39 | 1 |
| Caesarean Section with Indications | 4.53 ± 3.18 | 4 | 86 | 1 |
Table 2: Length of Stay of Pregnant Women with Different Delivery Modes.
Table 3 shows that different payment methods result in the similar hospitalization costs. Pregnant women aged ≥ 35 and aged 30-35 had a slightly higher hospitalization costs than that of the pregnant women aged <30. In terms of birth weight, Hospitalization costs of the group <3000g and the group ≥ 3500g are slightly higher than that of the group 3000-3500g. Hospitalization costs of pregnant women admitted from outpatient department are higher than that of pregnant women transferred from other hospitals. The hospitalization costs of pregnant women who had caesarean section with or without indications are twice as much as that of pregnant women who had vaginal delivery. See figure 1.

Figure 1: Bar chart of hospitalization expenses for different characteristics.
| Features | Overall Hospitalization Costs(CNY) | |||||
| n | Mean ± standard deviation | Median | Maximum | Minimum | ||
| Urban Employee Basic Medical Insurance | 4090 | 11472.84 ± 7446.21 | 10632.38 | 216624.19 | 1977.01 | |
| Payment Methods for Medical Services | Urban Resident Basic Medical Insurance | 1894 | 11393.05 ± 8470.56 | 10474.96 | 211991.44 | 3273.54 |
| New Rural Cooperative Medical System | 110 | 11743.24 ± 7700.23 | 10651.22 | 59423.53 | 3133.95 | |
| Self-paying | 3387 | 10428.76 ± 5470.01 | 10288.92 | 92456.22 | 1178.75 | |
| Others | 6150 | 10423.97 ± 5659.76 | 10392.54 | 258697.91 | 2141.69 | |
| Age | <30 years old | 8930 | 10101.49 ± 6112.13 | 9989.77 | 216624.19 | 1977.01 |
| 30-35 years old | 4719 | 11387.7 ± 5954.79 | 10957.28 | 118947.95 | 1178.75 | |
| ≥ 35 years old | 1982 | 12754.21 ± 8897.16 | 11723.65 | 258697.91 | 2141.69 | |
| Birth Weight | <3000g | 4443 | 11936.79 ± 9867.78 | 10692.25 | 258697.91 | 1178.75 |
| 3000-3500 g | 6241 | 10180.1 ± 5077.36 | 10192.32 | 216624.19 | 3268.38 | |
| ≥ 3500 g | 4947 | 10643.73 ± 3750.81 | 10609.76 | 56085.43 | 2141.69 | |
| Admission Route | Transferred from Other Hospitals | 2955 | 10201.17 ± 9282.21 | 9487.06 | 258697.91 | 2371.6 |
| Outpatient Department | 12659 | 10971.96 ± 5723.36 | 10607.23 | 216624.19 | 1178.75 | |
| Delivery Modes | Vaginal Delivery | 3397 | 6262.89 ± 1693.38 | 5865.24 | 34312.88 | 1178.75 |
| Caesarean Section without Indications | 3814 | 12047.17 ± 3065.89 | 11483.94 | 52512.18 | 4687.67 | |
| Caesarean Section with Indications | 8420 | 12114.11 ± 7973.55 | 11109.15 | 258697.91 | 2051.63 | |
Table 3: Hospitalization Costs of Pregnant Women in Different Groups.
Concerning to the hospitalization costs structure of different modes of delivery, for pregnant women of vaginal delivery, the proportion of costs on diagnosis, treatment, general medical services and consumable items are 32.84%, 26.21%, 14.62% and 13.25% respectively. For caesarean section without indications, the proportion of hospitalization costs on consumable items, diagnosis, general medical services, and treatment are 33.18%, 19.46%, 16.96% and 16.75% respectively. As for caesarean section with indications, the proportion of costs on consumable items, diagnosis, treatment and general medical services are 29.78%, 21.23%, 16.44% and 16.29%. Costs on consumable items accounts for the largest proportion in both caesarean section without indications and caesarean section with indications, 33.18% and 29.78% respectively, followed by costs on diagnosis 19.46% and 21.23% respectively. For pregnant women of vaginal delivery, costs on diagnosis accounts for the largest proportion 32.84%, followed by costs on treatment 26.21%. See table 4 and figure 2.
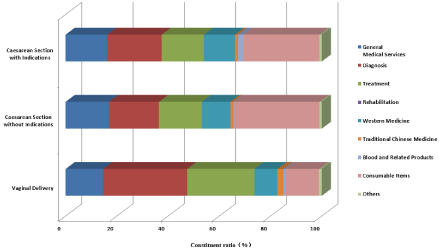
Figure 2: Percentage chart of hospitalization expenses in different delivery modes.
| Delivery Modes | General Medical Services | Diagnosis | Treatment | Rehabilitation | Western Medicine | Traditional Chinese Medicine | Blood and Related Products | Consumable Items | Others |
| Vaginal Delivery | 14.62 | 32.84 | 26.21 | 0.01 | 8.96 | 2.45 | 0.58 | 13.25 | 1.08 |
| Caesarean Section without Indications | 16.96 | 19.46 | 16.75 | 0.00 | 11.14 | 1.21 | 0.41 | 33.18 | 0.89 |
| Caesarean Section with Indications | 16.29 | 21.23 | 16.44 | 0.03 | 12.13 | 1.21 | 2.03 | 29.78 | 0.86 |
Table 4: Hospitalization Costs Structure of Pregnant Women with Different Delivery Modes. (unit: % )
Multiple Linear Regression (MLR) analysis was conducted with payment methods, age, admission route, different delivery modes, and length of stay as independent variables and hospitalization costs as dependent variables (Value can be seen in table 5. Stepwise method was applied to select the independent variables to use in the MLR with α = 0.05 and variables were excluded as the P-value was 0.1). It is found that payment methods, age, different delivery modes and length of stay were influencing factors of hospitalization costs.
| Influencing Factors | Regression Coefficient | Standard Regression Coefficient |
F | P |
| Constant | 3.24988 | 0 | 24.6 | <0.0001 |
| Payment Methods (Compared to Self-paying) | ||||
| Others | 0.20644 | 0.01539 | 1.78 | 0.0759 |
| New Rural Cooperative Medical System | 0.71717 | 0.00915 | 1.37 | 0.172 |
| Urban Resident Basic Medical Insurance | 0.52488 | 0.02614 | 3.36 | 0.0008 |
| Urban Employee Basic Medical Insurance | 0.45748 | 0.03068 | 3.61 | 0.0003 |
| Age (<30:0, 30-34:1, ≥ 35:2) | 0.56371 | 0.06086 | 9.02 | <0.0001 |
| Delivery Modes (Compared to Vaginal Delivery) | ||||
| Caesarean Section without Indications | 3.67506 | 0.24087 | 27.7 | <0.0001 |
| Caesarean Section with Indications | 3.39781 | 0.25848 | 29 | <0.0001 |
| Actual Length of Stay | 1.06512 | 0.439 | 62.8 | <0.0001 |
Table 5: The Results of Generalized Linear Regression Analysis of Hospitalization Costs.
According to the size of standard partial regression coefficient and the results of hypothesis testing by comparison between standard partial regression coefficients, compared to self-paying, the hospitalization costs of urban employee basic medical insurance, urban resident basic medical insurance, new rural cooperative medical system and other payment methods were higher; The hospitalization costs of caesarean section with or without indications were both higher than that of vaginal delivery, with F=27.67, P<0.0001 and F=28.96, P<0.0001 respectively. The length of stay is the most influencing factor of hospitalization costs with standard regression coefficient 0.439, F=62.76 and P<0.0001, followed by different delivery modes. See table 5.
As an obstetric surgery that deals with dystocia and highrisk pregnancy, caesarean section contributes significantly to the safety of high-risk pregnant women and fetus. Several factors, including a fear of pain, the concern for maternal and newborn health, anxiety over vaginal delivery [5], have resulted in a worldwide increase in the rate of caesarean section without medical indications in recent years. Researchers have shown that social factors, instead of medical indications, have now become the major reason for a high rate of caesarean section in China [6-12]. Caesarean section not only adds to the hospitalization costs of the pregnant women, but also serves as a resource drain on the country as a whole. At the same time, it will affect maternal and perinatal health to a certain degree [13]. According to the study, the rate of vaginal delivery in primipara was 21.73%, the rate of caesarean section without indications 24.40%, and the rate of caesarean section with indications 53.87%. The rate of caesarean section without indications was still higher than expectations. The hospitalization costs of pregnant women who had caesarean section in bipara, with or without indications, were twice as much as that of pregnant women who had vaginal delivery, though there was only a slight difference in the median hospitalization costs. Therefore, it is vital to considerably reduce the rate of caesarean section without indications. The univariate and multivariate analysis of the hospitalization costs also shows that the delivery mode is an important factor that influences hospitalization costs. To reduce the rate of caesarean section without indications will, therefore, be the preferred measure to cut down on hospitalization costs. When pregnant women were in hospital, health education during pregnancy for them and their family as well as effective communication between doctors and pregnant women may help build up the expectations of pregnant women towards parturition. By improving midwifery techniques for spontaneous vaginal delivery, developing effective measures on labor pain management and conducting caesarean section when it is medically indicated, the rate of caesarean section without indications can be significantly reduced so as to improve maternal and perinatal health and control the medical costs.
Download Provisional PDF Here
Article Type: RESEARCH ARTICLE
Citation: Zhang T, Zhong X, Zhang Y (2018) An Analysis of the Hospitalization Costs and its Influencing Factors or Different Delivery Modes. J Epidemiol Public Health Rev 3(2): dx.doi. org/10.16966/2471-8211.164
Copyright: © 2018 Zhang T, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access