
Figure 1: Examples of health promotion images in municipalities based on “Healthy Japan 21” [11].


Tomoko Tachibana1* Hiroshi Mizushima2
1Chief Senior Researcher, National Institute of Public Health, Center for Public Health Informatics, 2-3-6 Minami, Wako city, Saitama prefecture 351-0197, Japan*Corresponding author: Tomoko Tachibana, National Institute of Public Health, Center for Public Health Informatics, 2-3-6 Minami, Wako city, Japan, Tel: +81-48-458-6206; E-mail: tachibana.t.aa@niph.go.jp
Objectives: What the review set out to determine “health” in a care-focused mature society.
Design: Review on the evidence-based public health policies in Japan.
Data Sources: Ministry of Health, Labour, and Welfare in Japan.
Eligibility Criteria: Next Generation Healthcare Foundation Law
Results: In Japan, evidence-based public health is promoted for lifestyle diseases, and evidence such as survival rates of cancer is useful not only for healthcare providers and policymakers but also for cancer patients in executing the right to self-determination in promoting health. Meanwhile, evidence about long-term outcomes of trauma in Japan is overwhelmingly lacking, although the incidence of trauma is estimated to be comparable to that of neoplasms in the 2014 national patient survey. We have proposed reviewing health and welfare policies for people with disabilities from the viewpoint of longitudinal epidemiological studies that understand disease conditions from the perspectives of ordinary citizens by redefining the prognoses of trauma as “the outcomes of acquired disability.” To realize this review in a care-focused society we focus on the Clinical Efficacy database of patients visiting medical institutions, and intend to develop a disability registry toward the additional definition of “health” in a matured society, that is, including “health of the people with disabilities.”
Conclusions: In care-focused mature societies, considering the disease burden and various other social, physical, and psychological problems, maintaining the patient’s quality of life, enabling his/her control over his/her own life, offering opportunity for independent functioning, and fostering his/her self-actualization should be included in the definition of health.
Evidence-based health and welfare policy for people with disabilities; Clinical Efficacy database; Disability registry; Prognoses of trauma; Definition of health
The 2010 Global Burden of Diseases, Injuries, and Risk Factors Study (GBD)-a joint study by the World Health Organization (WHO) and seven institutions from Japan, the US, and the UK-showed that, “with medical and developmental advancement, food shortage has been resolved, the number of deaths has decreased, and the world population has notably aged, while many people are living with burden from ‘mental illness, chronic pain, and trauma’ and risk factors such as ‘obesity and lack of exercise’”[1]. Furthermore, in the past 20 years (1990-2010), analyses of injuries or illnesses causing death and disabilities using disabilityadjusted life years presented the following evidence: “the main factor of the global disease burden was deaths of children under five years old, but presently, majority of the factors are musculoskeletal disorders, mental illnesses, trauma, etc., and such burden increases as people live longer” [2]. Many countries are facing such changes in disease structure, and, as noninfectious diseases have now become a global threat [3], transition in the medical and social security system from focusing on “cure” to “support” is desired.
Japan is aging faster than the rest of the world is, and we must respond to a decreasing birthrate and an aging population. Japan’s new vision for health care measures is to further develop and lead the world as a maturing nation (“Japan Vision: Healthcare 2035”) [4,5]. “Japan Vision: Healthcare 2035” aims to achieve a paradigm shift toward “care-centered healthcare,” “quality improvement,” “patient-centered values,” “discipline by concerned parties” and “integration” by 2035 [6].
On prevention of “trauma,” the authors propose the application of the concept of health promotion and disease prevention and present a fundamental review for understanding trauma medical care for the promotion of healthcare and welfare measures for people with physical disabilities (Table 1) [7].
| Definition of “primary, secondary, and tertiary” prevention of “trauma” | cf. Definition of “primary, secondary, and tertiary” prevention for “health promotion and disease prevention” | |
| Primary prevention | To prevent the occurrence of injuries due to traffic accidents, tumble-falls, and collapses (=injury) | To improve one’s lifestyle and promote health, to prevent lifestyle-related diseases, etc. |
| Secondary prevention | Early transportation and life-saving care, emergency medical care, acute injury care, early detection of sequelae, and early treatment |
Health examinations, etc., for early detection and early treatment |
| Tertiary prevention | To prevent the functional, psychological, and social degradation of quality of life for sequelae and disability and to promote social reintegration and resumption of school, work, and everyday life | Care required after disease onset, maintenance, and recovery of function |
Table 1: Definition of “primary, secondary, and tertiary” prevention for “trauma” and “health promotion and disease prevention.”
[Tachibana et al. [7] has been revised] (in Japanese)
In Japan, as a measure against “‘obesity and lack of exercise’, which are risk factors for disease burden.” “Healthy Japan 21” promotes taking steps against lifestyle diseases such as diabetes, cardiovascular disease, cancer, and so on. Especially, as steps against “cancer,” the leading cause of death in Japan, the “Cancer Control Act” was established in 2006 and promotes the implementation of primary, secondary, and tertiary comprehensive prevention measures in addition to “Healthy Japan 21” as a part of Evidence-Based Public Health (EBPH). The information necessary for EBPH on cancer countermeasures is gathered based on the Cancer Control Act through the “National Cancer Registry” system started in 2016 [8]. All data from those diagnosed with cancer in Japan are collected and stored in this database. These data are compiled and disease, prevalence, and survival rate data for each site are published as “cancer statistics” along with demographic mortality data [9].
For “whom and how” are such cancer statistics useful? [10] First, municipalities and experts on cancer care use such data for quality management and improvement of cancer screening and other services provided. Second, such data are used as evidence for planning regional medical policies and national cancer countermeasures. Third, the data benefit “‘all citizens performing health promotion activities’, including those diagnosed with cancer.” For example, “cancer survival rate” is necessary for “people who are performing health promotion activities to prevent cancer (=primary prevention)” as well as for “those diagnosed with cancer (=cancer patients)” to select treatment and self-determine future health promotion activities (=tertiary prevention) (Figure 1) [11]. To calculate reliable survival rates, a highly precise prognosis survey is crucial.
.
Figure 1: Examples of health promotion images in municipalities based on “Healthy Japan 21” [11].
In Japan, health policies for “chronic pain, and trauma,” previously indicated as “disease burden” are mostly limited to “responses by experts from each field of medicine.” In the field of healthcare and welfare, other than for “abuse,” policies are limited to measures against sequelae and disabilities resulting from “trauma” and are implemented as “efforts for each type of disability.”
In Japan, since the 1960s, the number of injuries and deaths from traffic-related trauma has increased rapidly while the rate of emergency care has increased. With such changes, the estimated number of “those with sequelae and acquired disabilities from trauma” has increased, making it a social issue (Figure 2) [12-14]. Therefore, a preventive approach for traumas came to be promoted by departments other than the public health department, including 1) “measures against traffic accidents and prevention of injuries” by the National Police Agency and Ministry of Land, Infrastructure, Transport and Tourism and 2) “early transportation and emergency medical care” by the Fire and Disaster Management Agency and medical institutions.
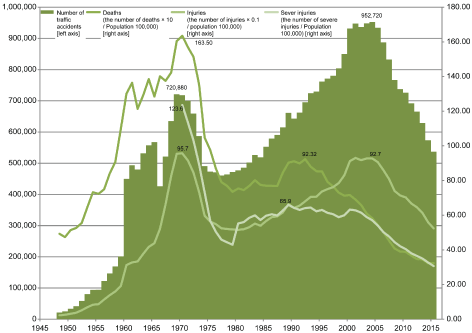
Figure 2: “Occurrence of traffic accidents.”
According to Japan’s epidemiological statistics on trauma, in the 2014 patient survey conducted by the Ministry of Health, Labor and Welfare that reported the estimated number of patients for each category of injuries and illnesses to have received treatment in all medical facilities in Japan (Table 2, Supplement 1), we cannot find major differences in “onsets” between diseases caused by “XIX External causes such as injuries, poisoning, and others” and “II Neoplasm.” Presently, epidemiological statistics on trauma are limited to “patient registration at the onset of injuries and illnesses” and collection, accumulation, and use of “‘qualitative and quantitative preventive epidemiological data for evaluation of intervention effects’ and ‘care and needs for each stage’ in healthcare, medical and nursing care, and welfare associated with long-term prognosis of trauma.” As such, information on “type of sequelae, complications, secondary diseases, and disabilities that may affect patients after treatment of acute-phase trauma” or “type and degree of intervention needed for such conditions” in each region are notably insufficient in Japan (Table 2) [15,16].
| (Unit: 1,000 people) | October 2014 | |||||||
| Disease classification | Hospitalization | Outpatient | ||||||
| Total | Hospital | General clinic | Total | Hospital | General clinic | Dental clinic | ||
| Total | 1,318.8 | 1,273.0 | 45.8 | 7,238.4 | 1,641.9 | 4,233.0 | 1,363.4 | |
| I | Infectious and parasitic diseases | 20.7 | 20.3 | 0.4 | 173.3 | 41.7 | 131.6 | ・ |
| Tuberculosis (repeated) | 3.4 | 3.4 | 0.0 | 1.7 | 1.5 | 0.2 | ・ | |
| Viral hepatitis (repeated) | 1.4 | 1.3 | 0.1 | 28.3 | 14.0 | 14.3 | ・ | |
| II | Neoplasm | 144.9 | 143.2 | 1.7 | 231.6 | 187.3 | 44.3 | ・ |
| Malignant neoplasm (repeated) | 129.4 | 127.9 | 1.5 | 171.4 | 146.5 | 24.8 | ・ | |
| Gastric malignant neoplasm (repeated) | 13.5 | 13.4 | 0.2 | 19.2 | 14.9 | 4.3 | ・ | |
| Colorectal malignant neoplasm (repeated) | 18.9 | 18.7 | 0.3 | 28.0 | 22.9 | 5.1 | ・ | |
| Hepatic and intrahepatic bile duct malignant neoplasm (repeated) | 6.9 | 6.8 | 0.1 | 5.5 | 4.5 | 1.0 | ・ | |
| Tracheal, bronchial, and pulmonary malignant neoplasm (repeated) | 18.8 | 18.7 | 0.1 | 16.1 | 14.3 | 1.8 | ・ | |
| Breast malignant neoplasm (repeated) | 5.4 | 5.3 | 0.1 | 24.3 | 21.5 | 2.8 | ・ | |
| III | Blood and hematopoietic diseases and immune system disorders | 6.3 | 6.1 | 0.2 | 21.6 | 10.4 | 11.2 | ・ |
| IV | Endocrine, nutritional, and metabolic diseases | 33.0 | 31.6 | 1.3 | 437.0 | 131.9 | 305.1 | ・ |
| Diabetes (repeated) | 20.9 | 20.0 | 1.0 | 222.3 | 77.6 | 144.7 | ・ | |
| Hyperlipidemia (repeated) | 0.3 | 0.2 | 0.1 | 143.7 | 21.7 | 122.1 | ・ | |
| V | Mental and behavioral disorders | 265.5 | 264.3 | 1.3 | 257.7 | 110.9 | 146.9 | ・ |
| Vascular problems and dementia of unknown cause (repeated) | 29.8 | 29.3 | 0.5 | 11.9 | 3.6 | 8.3 | ・ | |
| Schizophrenia, schizotypal disorder, and delusional disorder (repeated) | 165.8 | 165.6 | 0.1 | 69.7 | 44.7 | 25.0 | ・ | |
| Mood disorder (including bipolar disorder) (repeated) | 28.8 | 28.4 | 0.4 | 83.4 | 27.3 | 56.1 | ・ | |
| VI | Nervous system diseases | 122.2 | 119.5 | 2.7 | 173.0 | 69.3 | 103.7 | ・ |
| Alzheimer’s disease (repeated) | 47.0 | 45.8 | 1.2 | 45.1 | 14.1 | 30.9 | ・ | |
| VII | Eye and appendage diseases | 11.5 | 10.2 | 1.3 | 337.9 | 56.9 | 280.9 | ・ |
| VIII | Ear and mastoid process diseases | 2.5 | 2.4 | 0.1 | 100.5 | 15.2 | 85.3 | ・ |
| IX | Cardiovascular diseases | 240.1 | 230.4 | 9.7 | 933.0 | 236.3 | 696.7 | ・ |
| Hypertensive diseases (repeated) | 6.4 | 4.8 | 1.6 | 671.4 | 104.6 | 566.8 | ・ | |
| Heart disease (excluding hypertension) (repeated) | 59.9 | 57.4 | 2.5 | 133.9 | 68.2 | 65.7 | ・ | |
| Cerebrovascular disease (repeated) | 159.4 | 154.9 | 4.6 | 94.0 | 44.7 | 49.2 | ・ | |
| X | Respiratory system disease | 90.7 | 88.1 | 2.6 | 668.4 | 91.6 | 576.8 | ・ |
| Pneumonia (repeated) | 34.6 | 33.3 | 1.3 | 8.2 | 3.9 | 4.3 | ・ | |
| Chronic obstructive pulmonary disease (repeated) | 7.9 | 7.6 | 0.4 | 22.0 | 8.8 | 13.3 | ・ | |
| Asthma (repeated) | 3.8 | 3.6 | 0.2 | 127.6 | 23.7 | 103.9 | ・ | |
| XI | Digestive system diseases | 65.9 | 63.9 | 2.0 | 1,310.0 | 115.9 | 174.4 | 1,019.6 |
| Dental caries (repeated) | 0.1 | 0.1 | 0.0 | 283.6 | 3.4 | 3.3 | 276.8 | |
| Gingivitis and periodontal disease (repeated) | 0.2 | 0.2 | - | 444.7 | 9.5 | 7.1 | 428.2 | |
| Liver disease (repeated) | 8.0 | 7.7 | 0.3 | 32.6 | 12.1 | 20.5 | ・ | |
| XII | Skin and subcutaneous tissue diseases | 10.9 | 10.5 | 0.4 | 286.9 | 47.7 | 239.3 | ・ |
| XIII | Musculoskeletal system and connective tissue diseases | 69.9 | 64.4 | 5.5 | 877.8 | 180.6 | 697.2 | ・ |
| XIV | Renal, urinary, and reproductive system diseases | 46.9 | 44.0 | 2.9 | 283.1 | 112.6 | 170.5 | ・ |
| Chronic renal failure (repeated) | 24.1 | 21.7 | 2.4 | 107.3 | 47.2 | 60.1 | ・ | |
| XV | Pregnancy, childbirth, and puerperium | 18.4 | 14.2 | 4.3 | 14.5 | 6.7 | 7.8 | ・ |
| XVI | Perinatal period diseases | 6.7 | 6.4 | 0.3 | 2.9 | 2.4 | 0.5 | ・ |
| XVII | Congenital anomaly, deformation, and chromosomal abnormality | 5.8 | 5.7 | 0.0 | 14.3 | 9.0 | 5.3 | ・ |
| XVIII | Not classified under any other category based on symptoms, signs, abnormal clinical findings, and abnormal findings | 16.0 | 15.0 | 1.0 | 76.9 | 38.2 | 38.7 | ・ |
| XIX | External causes such as injuries, poisoning, and others | 131.3 | 124.5 | 6.8 | 306.5 | 102.5 | 201.2 | 2.7 |
| Broken bones (repeated) | 91.4 | 86.4 | 5.0 | 92.0 | 39.9 | 52.1 | ・ | |
| XXI | Factors that affect health conditions and use of healthcare services | 9.7 | 8.3 | 1.3 | 731.7 | 74.9 | 315.8 | 341.1 |
Table 2: 2014 patient survey: Estimated number of patients for each type of facility for each category of injuries and illnesses* [15,16].
The estimated number of patients for each category of injury and illness to have received treatment in all medical facilities in Japan on the survey data is presented in Table 2 (unit [1,000], % of the total): 144.9 (11.0%) “Hospitalizations” and 231.6 (3.2%) “Outpatients” for “II Neoplasm,” and 131.3 (10.0%) “Hospitalizations” and 306.5 (4.2%) “Outpatients” for “XIX External causes such as injuries, poisoning, and others.” Diseases caused by “XIX External causes such as injuries, poisoning, and others” are similar to “II Neoplasm.”
The patient survey was implemented each year as a one-day survey based on medical records of patients. However, since 1984, the contents were improved, the number of participants was increased to enable regional representation, and the survey frequency was reduced to once every three years; it was implemented with the survey of medical facilities.
This was a specifically designated day for each medical facility (between Tuesdays and Thursdays) in October of each survey year. As for clinics, since 2005, Thursdays were excluded as many clinics are closed then, and Tuesdays, Wednesdays, and Fridays were selected. For discharged patients, this date was designated as one month between September 1 and 30 of each survey year.
The methods noted by the manager of each medical facility.
Ministry of Health, Labour and Welfare, prefecture, health centers, medical facilities, cities with healthcare centers, and special zones.
Injuries and illnesses in this survey are classified using “The International Classification of Diseases-10” (ICD-10; 2003) by the WHO.
[Excerpt from “1.Estimated number of patients and Table” “2.Estimated number of patients for each type of facility for each category of injury and illness” in the “2014 patient survey,” edited by the authors.]
For 2025 as a goal, in Japan, an “integrated community care system” consisting of two concepts-community-based [17] and integrated care [18] is being promoted. In a mature care-centered society, the need for highly precise information on “prognosis of trauma” for “those experiencing trauma (=trauma patients)” in “selecting treatment and rehabilitation measures to minimize sequelae and disabilities and for self-determination of future plans” is probably similar to the cancer statistics available for cancer patients.
Trauma could also “be a cause of acquired disabilities (=midlife disability).” If we consider “acquired disabilities as ‘the course and outcome of injuries and illnesses such as trauma’,” disabilities can be re-evaluated as “the subject of public health approach” in an epidemiological longitudinal study. In the past, healthcare and welfare measures for people with physical disabilities have been examined through cross-sectional studies.
On the timing of medical care and welfare service interventions. However, a longitudinal study will provide an “understanding of diseases from the perspective of concerned parties as survivors.” In Japan, it is now important to discuss ways to value primary, secondary, and tertiary preventive medical approaches for “trauma.”
We have proposed to review the medical care for “trauma” to foster the promotion of healthcare and welfare measures for people with physical disabilities (Table 1) [7,19,20]. In mature societies with improved medical standards, including Japan, by viewing trauma care as “medical care for ‘a health hazard that could cause and impact the degree of disability,’ depending on the intervention effect on prognosis,” “tertiary prevention” of traumas could be enhanced (Figure 3). Thus, while searching for possibilities of implementing a collaborative database project on the longterm prognosis course of trauma in Japan, [20] we searched for a concrete, evidence-based measure to change the healthcare and welfare activities for people with physical disabilities. Based on these results, in the next chapter, we will switch our viewpoint to that of healthcare and welfare measures for people with physical disabilities to comprehensively review the connection to trauma care and introduce studies presently progressing toward the “development of a regional model” on healthcare and welfare measures for people with physical disabilities.
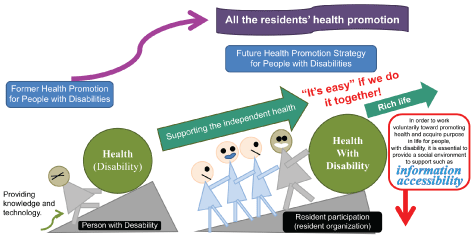
Figure 3: Image of an “environment that supports health” for people with disabilities.
In Japan, the Basic Act for People with Disabilities defines “people with disabilities” as those “who have physical, cognitive, psychological (including developmental) disabilities, or other mental or physical dysfunctions (referred to collectively below as “disabilities”) and whose daily and/or social lives are significantly and continuously restricted by these disabilities and/or by social barriers” [21]. The total number of people with disabilities in Japan, as of March 2015, was 7.879 million people, which is approximately 6.2% of the total population. With the aging of the society, this number has been increasing steadily in addition to the number of people with disabilities who live in their own homes and/ or attend day-care centers.
In Japan, all citizens are guaranteed access to necessary medical treatment by the National Health Insurance System (=universal health coverage) [22]. However, due to the low birth rate and societal aging, difficulties related to the state of public finance continue, and, therefore, it is necessary to invest the scarce resources efficiently. To help achieve this, the present author focused on “clinical efficacy information” as part of the movement toward a sustainable health policy for people with disabilities. “Clinical efficacy information,” according to the Japanese Ministry of Health, Labor and Welfare, promotes and coordinates the maintenance and organization of patient information related to the diagnosis, treatment process, treatment efficacy, and so on, of patients examined and/or treated at all medical institutions in Japan. These data are being collected, analyzed, and published nationwide and are being maintained as a database to improve the quality of medical treatment [23,24]. It is encouraged to structure the database based on injuries/diseases [25-27], and progress is currently being made on examining the links between and the efficient operation of each Clinical Efficacy database [28,29]. However, the bulk of each Clinical Efficacy database consists of the registry information of patients examined and/or treated at medical institutions, classified by disease/injury (referred to below as the “Medical Treatment database”). To evaluate the clinical efficacy of such databases, it is important to assess the outcomes through a follow-up study, but it is currently difficult to make a satisfactory assessment of outcome information.
In this context, a Comprehensive Nursing-Care Insurance database (referred to below as the “Nursing database” [30] is currently being established as one body of information corresponding to “essential outcome information” within the clinical efficacy information to promote effective use of the data. Information related to the use of the Nursing Care Insurance System [31], is brought together in the form of nursingcare receipt data via the National Health Insurance Organization, which is the healthcare billing and payment organization. Subsequently, after anonymization of these data, they are included in the Ministry of Health, Labor and Welfare’s nursing database. However, the Nursing and Medical Treatment databases are managed and run separately, and it is, therefore, necessary to establish a system that links the two. In addition, information included in the Nursing database consists of data about people covered by the Japanese nursing-care insurance system, and, therefore, it is restricted to people aged over 40 years. Thus, the Nursing database does not include information about people who do not have access to the nursing-care insurance system-specifically, those aged below 40 years.
As one achievable outcome information area, the present author proposed the establishment of an Injuries Health and Welfare database. Currently, it is compulsory for local governments to control information related to the health and welfare of people with disabilities, such as information in the “Certification for Persons with Physical Disabilities” (referred to below as “information about people with disabilities”) using a logbook. This is the responsibility of prefectural governors, mayors of cities designated by ordinance, and mayors of core cities [32], but these parties have not yet made full use of such information for purposes such as analysis and evaluation of health policies for people with disabilities. However, in future, to promote the development of more effective and efficient health policies for people with disabilities, it will be necessary to establish an “informational environment” that involves the accumulation and full use of epidemiological data and other such information related to injury-related health and welfare to evaluate policies and design effective interventions. If an Injury Patients database covering both acquired and congenital disorders is established as an Injured/Ill Registry, similar to the Cancer Registry, it should be possible to evaluate, as part of the clinical efficacy information, the outcomes required for the evaluation of intervention efficacy. Therefore, the present author is currently carrying out a study based on a proposal to establish an Injuries/Diseases Medical Treatment, Nursing, Health, and Welfare database, centered on local governments (referred to below as the “study on the Injuries Medical Treatment, Nursing, Health, and Welfare database”; Figure 4).
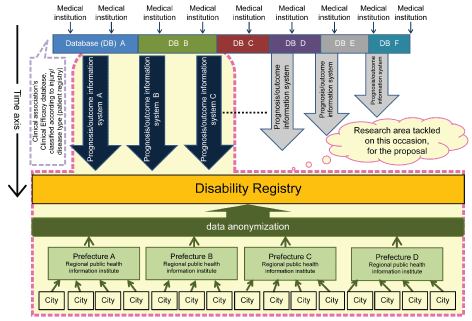
Figure 4: Diagram representing the study on the regional model development of the “Injuries/Diseases Medical Treatment, Nursing, Health, and Welfare DB.”
As part of the study on the Injuries Medical Treatment, Nursing, Health, and Welfare database, the database system component-that is, the “time-series outcome of cross-sectional follow-up in specialized fields” for injuries/diseases, including disability health and welfare information, has been termed in the present manuscript as the “Prognosis/Outcome Information System,” because it is considered that, in general, information included in this Prognosis/Outcome Information System relates to patients and/or other affected parties themselves. Both “prognosis” and “outcome” in this context refer to progression along the temporal axis, but the former indicates a progression from a starting point while and the latter indicates a progression from an intermediate or finishing point. Considering these perspectives, progression that is determined when a physician or other healthcare service provider examines a patient is usually termed as the “outcome.” Thus, it is considered that the data in the Prognosis/ Outcome Information System will be useful for medical care providers and administrative policy planners. On the other hand, with reference to the point of view of the progression required, according to patients and/or other affected parties themselves, there may be an overwhelming demand for prognostic information. In other words, from a patientcentered perspective-that is the desire for creating a better quality of life, notwithstanding various difficulties that may be experienced-the required progression information probably always relates to the prognosis rather than the outcome. For example, if a patient chooses to undergo treatment, it is generally understood that the physician usually provides detailed information about the treatment method and prognosis (Figure 1). Of course, at the initial stage of establishment of the Prognosis/Outcome Information System, much of the information included will be individual outcome information, and most of it is likely to be information that is useful for healthcare service providers and administrative policy planners. However, in the case of, for example, the US Rare Disease Patient Registry, which is equivalent to the Japanese Incurable Disease Registration, the registry is primarily the responsibility of the relevant patients’ association, and the national government merely provides technical support [29]. Further, in the US Rare Disease Patient Registry, registered patient data are anonymized and collected in the Global Rare Disease Patient Registry and Data Repository with registrations made on a single-patient basis, using a Global Unique Identifier (GUID) for each patient, as defined by the National Institutes of Health. Thus, information about a single patient can be pulled out of the database by matching the name with the GUID. In Japan, too, although the Refractory Disease Patient Register is still centered on data entered by the government, professional and academic organizations, and research groups, in recent years, patient’s associations have started getting involved in this process [33].
In 1948, the WHO charter defined “health” as “a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity” [34]. The Japanese translation of this definition has been used in Japan. Subsequently, the WHO proposed the following new definition of health in 1998: “Health is a dynamic state of complete physical, mental, spiritual, and social well-being and not merely the absence of disease or infirmity” [35]. Though the executive board of directors adopted the proposal at a general meeting, this definition was passed without careful deliberation. In Japan, there was no Japanese equivalent for the new “dynamic” and “spiritual” definition by the WHO, and the definition from 1948 continued to be used.
However, the global trend in health has changed greatly since 1948. Huber et al. [36] argued that “the definition of health by the WHO, of complete well-being, does not suit the objective any longer considering the increased number of chronic diseases” and proposed moving the focus on the ability to adapt and self-manage in the face of social, physical, and emotional challenges. People face various social, physical, and mental “challenges” throughout their lives, and, as a result, some may spend the rest of their lives with “disabilities.” Under such circumstances, it is important to shift the “definition of health” to the ability to “adapt and self-manage” in a care-centered mature society. At least, while the traditional definition of “complete well-being” appears to exclude people with disabilities and chronic diseases from the concept of “health,” the proposal by Huber et al. appeared to include these people.
Consequently, the concepts excluded from the “definition of health” do not reflect the health policy of Japan. Considering this aspect, a “definition of health” to stipulate the “target, scope, and direction” of health policy is important for not only developed countries but also other countries worldwide. With health and economic differences between countries, there could be a “unique ‘definition of health’ for each country.” Considering this, we review the discussions in previous sections of this paper and propose that, in Japan’s “care-centered mature society,” the “image of health” that is, the notion that “despite ‘social, physical, and mental challenges’ such as the disabilities acquired from trauma, quality of life can be maintained and that one ‘is able to’ self-manage and aim for “self-actualization” is added to the future “definition of health.”
We attest that we have obtained appropriate permissions and paid any required fees for use of copyright-protected materials.
The Corresponding Author has the right to grant on behalf of all authors and does grant on behalf of all authors, a worldwide license to the Publishers and its licensees in perpetuity, in all forms, formats, and media (whether known now or created in the future), to i) publish, reproduce, distribute, display and store the Contribution, ii) translate the Contribution into other languages, create adaptations, reprints, include within collections and create summaries, extracts and/or, abstracts of the Contribution, iii) create any other derivative work(s) based on the Contribution, iv) to exploit all subsidiary rights in the Contribution, v) the inclusion of electronic links from the Contribution to third party material where-ever it may be located; and, vi) license any third party to do any or all of the above.
Tachibana contributed to the conception of the design of the work, research, collection, analysis, and interpretation of literature data, the writing and major revision of the abstract, approval of the final draft and revising it critically for important intellectual content, and agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. Mizushima contributed evaluation and advice on the overall research and the abstract from the perspective of clinical effect information. Final approval of the version to be published is given by Tachibana.
This study does not need approval of Ethical consideration. All of the objects in this study have been brought to light.
Supported by the 2016 Research on “Effective Methods of Information Support for People with Communication Difficulty.” Research representative: Tomoko Tachibana (H28-Physical/IntellectualGeneral-009), Ministry of Health, Labor and Welfare Grant-in-Aid for Scientific Research-Comprehensive Research on Disability Health and Welfare (Physical/Intellectual Disability).
We have read and understood BMJ policy on declaration of interests and declare that we have no competing interests.
Download Provisional PDF Here
Article Type: Review Article
Citation: Tachibana T, Mizushima H (2017) A Review for Promoting Evidence-based Healthcare and Welfare Policies for People with Disabilities-A Proposed “Definition of Health” for a Care-focused Mature Society. J Epidemiol Public Health Rev 2(6): doi http://dx.doi.org/10.16966/2471-8211.158
Copyright: © 2017 Tachibana T, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access