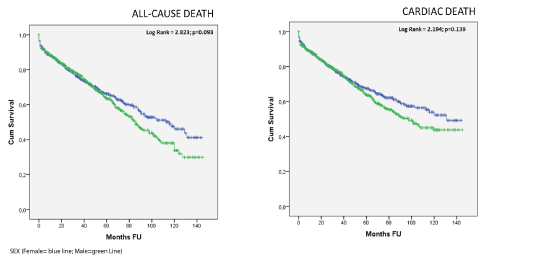
Figure 1: Kaplan-Meier curves according to sex for all-cause death (panel A) and cardiac death (panel B)


Gaetano Tanzilli1 Alessio Arrivi2 Valeria Raparelli3 Giovanni Truscelli1 Nicola Viceconte1 Nicolò Sperduti4 Alessandra Tanzilli1 Stefania Basili4 Marcello Dominici2 Enrico Mangieri1*
1Department of Cardiovascular, Respiratory, Nephrologic, Anaesthesiologic and Geriatric Sciences, Sapienza University of Rome, Rome, Italy*Corresponding author: Enrico Mangieri, Associate Professor in Cardiology, Department of Cardiovascular, Respiratory, Nephrologic, Anaesthesiologic and Geriatric Sciences, Sapienza University of Rome, Viale del Policlinico 155, 00161 Rome, Italy, Tel: +3906499772661; E-mail: enrico.mangieri@uniroma1.it
Background: Women with ischemic heart disease (IHD) typically present less severe coronary artery atherosclerosis. Despite that, as compared with men, women maintain a worse outcome. This female susceptibility seems to be mainly related to older age of clinical presentation and heavier risk factors burden.
Purpose: To investigate whether sex differences exist in the real-world management and clinical outcome of elderly patients with suspected IHD.
Methods: Retrospective analysis of IHD elderly (≥ 80 years) patients undergoing coronary angiography for acute coronary syndrome (ACS) or stable angina (SA). Management strategy, including invasive revascularization or a conservative medical approach, and outcome were evaluated.
Results: A total of 1420 (41% women; mean age: 83.1 ± 2.8) IHD patients referring for ACS (43%) and SA (57%) were analyzed. Men more likely accessed for SA (59.6% vs 52.5%, p<0.001) whereas ACS was the most frequent reason for angiography in women (28.8% vs 21.5%, p<0.001). No significant sex differences in the burden of obstructive epicardial disease were observed in both ACS and SA patients. No sex disparities in antiplatelet therapy, specifically clopidogrel, were detected. Compared with SA men patients, female ones received more likely a conservative therapy (p=0.049). After a median (IQR) follow-up time of 39.0 (16-71) months, a total of 514 (36%) patients died. No sex differences in cardiac death (p=0.139) was observed. Nevertheless, the Kaplan Meier curves showed a trend in lower all-cause mortality in female group (p=0.093).
Conclusions: In the very elderly population, an invasive strategy is superior to a conservative one in terms of survival rate. However, a dilution of the efficacy occurs with increasing age and comorbidities, and for male patients the benefit of the invasive strategy is not clear. Prospective studies are warranted to evaluate the net benefit of an invasive or a conservative approach in older population.
Ischemic heart disease; Elderly; Percutaneous coronary intervention; Sex
Aging is the underlying mechanism of atherosclerotic arterial disease and the elderly population constitutes a rapidly increasing subgroup of patients presenting with ischemic heart disease (IHD) [1].
The prevalence of cardiovascular disease (CVD), including coronary heart disease, heart failure, stroke, and hypertension in men and women 80 years of age and older has been reported at 84.7% and 85.9%, respectively [2]. Compared with younger counterparts, obstructive coronary artery disease (CAD) is often more diffuse and severe anatomically in the elderly population. Such complex anatomy along with the large territory of jeopardized myocardium makes the choice of optimal treatment strategy pivotal for risk reduction. In this context, the recent temporal trend shows declining in mortality along with an increase in myocardial reperfusion rate [2]. Despite that, as compared with men, women maintain a worse outcome. This female susceptibility, irrespective of less extent of coronary atherosclerotic involvement, seems to be mainly related to the older age of clinical presentation, mainly with atypical symptoms, and heavier risk factors burden [3,4].
To date, data from trials exclusively enrolling elderly patients are scarce and the management of elderly patients with IHD is essentially addressed by subgroup analyses from major trials. Furthermore, the proportion of such patients in ACS clinical trials is much lower (10%) than that seen in everyday clinical practice, where around 35% of ACS patients are aged ≥ 75 years [5]. As a consequence, a significant knowledge gap persists and the treatment opportunities may be underappreciated. Moreover, few data from randomized trials have addressed the question of the existence of gender difference in affecting management and outcomes in the very elderly population.
The aim of the present analysis is to investigate whether sex differences exist in the management of unselected population with suspected CAD, aged 80 years or older, undergoing diagnostic coronary angiography eventually followed by elective procedures or primary intervention as invasive therapy strategy. Moreover, we assessed the independent predictors of all-cause mortality and cardiac mortality in this peculiar cohort of frail patients.
From January 2004 to January 2011, 1420 out of 2350 consecutive patients with suspected CAD, aged 80 years or older, undergoing diagnostic coronary angiography followed by elective procedures or primary interventions coronary procedure were considered for the enrollment in the present analysis. The complete availability of clinical and angiographic records was mandatory for the inclusion of patients in the analysis. Patients were recruited from the Department of the Heart and Great Vessels Attilio Reale, SAPIENZA-University of Rome and Department of Interventional Cardiology, Santa Maria University Hospital, Terni.
Octogenarians patients accessed to the catheterization lab for acute coronary syndrome (ACS) or stable angina (SA). The revascularization strategy, conservative or invasive, was determined by interventional cardiologists and cardiac surgeons, on the basis of hemodynamic conditions, lesion characteristics, vessel size, the presence of comorbidities, quality of arterial and/or venous conduits for grafting, and patient and/or referring physician preferences. In all cases, the selected revascularization approach (i.e. angioplasty with or without stent implantation and coronary artery bypass graft) seemed suitable to guarantee complete revascularization.
Clinical, anthropometric, angiographic and procedural data were collected in each patient at the moment of the diagnostic angiography. Information with regard to the clinical status at the latest clinical followup available was collected by clinical visits, telephone interviews or referring physicians. Cardiovascular risk factors were defined as follows: hypertension, diabetes mellitus, and/or dyslipidemia [6]. Family history was considered significant, if a first-degree relative younger than 55-year-old (male) or 65-year-old (female) suffered premature CVD [6].
Pharmacological therapy at baseline was optimized according to guidelines for antihypertensive agents, antithrombotics and statins treatment. In particular, antiplatelet therapy was administered according to revascularization strategy and to the type of stent implanted. Both hypertension and dyslipidemia were categorized as treated conditions.
Myocardial infarction was defined based on the definition extracted from Thygesen et al. [7]. ST-segment elevation myocardial infarction (STEMI) was defined as ST-segment elevation or left bundle branch block on initial ECG and elevation of cardiac markers. Non-ST-segment elevation myocardial infarction (NSTEMI) was defined in case of angina symptoms and/or ECG changes and elevated cardiac markers. Unstable angina (UA) was diagnosed in presence of angina symptoms and/or ECG changes and normal values of cardiac markers. On the other hand, stable angina was defined in presence of angina symptoms with stress tests inducible myocardial ischemia
During follow-up observation, major adverse outcomes were defined. Death was classified as cardiac when it resulted from an acute myocardial infarction, sudden death, and death due to heart failure.
All-cause death included all death events occurred during follow-up. Cardiac and overall death was analyzed cumulatively at latest clinical follow-up available. All events were recorded and adjudicated by two blinded cardiologists (MD and AA).
Continuous variables were reported as mean ± SD or as median and interquartile range (IQR) as appropriate. Comparisons between groups of continuous variables were performed by t-test or Mann-Whitney U test. Categorical variables, reported as counts and percentages, were compared by Chi-square test or Fisher’s exact test when cell count was less than five.
Cumulative event curves were generated with the Kaplan-Meier method. Log-rank test was performed to analyze differences in survival distributors between subgroups. Univariate and multivariate Cox models were used to assess clinically relevant factors’ effect on the endpoints. The Cox proportional hazards regression model included all variables with a p<0.10. A forward stepwise model selection procedure based on the AIC was used to select the best multivariate regression model.
A two-sided p value <0.05 was considered as statistically significant. All analyses were performed using SPSS v. 22 (IBM, NY, USA).
One-thousand-four-hundred-twenty patients (59% men) undergoing percutaneous coronary intervention (PCI) were analyzed. In the 43% (n=615) of cases, ACS was the reason for PCI, while eight-hundred-five patients were studied for stable angina.
Table 1 reported the clinical characteristics of octogenarians at baseline according to sex. Women undergoing PCI were significantly older, with a low BSA, more frequently affected by hypertension, diabetes, and dyslipidemia comparing to men. In the 9% of cases, females’ patients had a concomitant cardiac valvular disease. For women, NSTEMI or STEMI were the more frequent reasons for undergoing angiography comparing with men that reported more often stable angina. Women with STEMI underwent to primary PCI more frequently than men. Moreover, in the case of UA and NSTEMI, women were more frequently undergone elective angiography comparing with men.
| Variables | Men (N=837) | Women (N=583) | P |
| Age, mean ± SD | 82.8 ± 2.6 | 83.6 ± 3.0 | <0.0001 |
| Age classes, n (%) | |||
| 80-84 years | 648 (77.4) | 395 (67.7) | 0.00021 |
| 85-89 years | 170 (20.3) | 165 (28.3) | |
| ≥ 90 years | 19 (2.3) | 23 (4.0) | |
| BMI, (kg/m2) mean ± SD | 25.8 ± 3.4 | 25.9 ± 4.4 | 0.662711 |
| BSA,(m2) mean ± SD | 1.83 ± 0,14 | 1.66 ± 0.15 | <0.001 |
| Vascular Access, n (%) | |||
| Radial | 546 (65.2) | 353 (60.6) | 0.11989 |
| Femoral | 249 (31.1) | 199 (34.1) | |
| From radial to femoral | 31 (3.7) | 31 (5.3) | |
| Familial history of CVD, n (%) | 201 (24.0) | 156 (26.8) | 0.24102 |
| Hypertension, n (%) | 558 (66.7) | 429 (73.6) | 0.00534 |
| Smoking Habit, n (%) | 543 (64.9) | 102 (17.5) | <0.00001 |
| Diabetes, n (%) | 222 (26.5) | 198 (34.0) | 0.00252 |
| Treatment of diabetes, n (%) | N=222 | N=198 | |
| Diet | 25 (11.3) | 14 (7.1) | 0.1574 |
| Oral | 135 (60.8) | 114 (57.6) | |
| Insulin | 57 (25.7) | 68 (34.3) | |
| Combined | 5 (2.2) | 2 (1.0) | |
| Dyslipidemia, n (%) | 309 (36.9) | 245 (42.0) | 0.05230 |
| CKD§, n (%) | 143 (17.1) | 81 (13.9) | 0.10461 |
| Concomitant Valvulopathy, n (%) | 39 (4.7) | 48 (8.2) | 0.00574 |
| Type of valvulopathy | |||
| Aortic insufficiency | 3 (0.4) | 4 (0.7) | 0.04260 |
| Aortic Stenosis | 27 (3.2) | 27 (4.7) | |
| Mitral insufficiency | 9 (1.1) | 16 (2.8) | |
| Combined | 0 (0.0) | 1 (0.2) | |
| Access to cath. lab, n (%) | |||
| SA | 499 (59.6) | 306 (52.5) | 0.00397 |
| UA | 158 (18.9) | 109 (18.8) | |
| NSTEMI | 146 (17.4) | 124 (21.3) | |
| STEMI | 34 (4.1) | 44 (7.6) | |
| Timing of PCI, n (%) | |||
| Primary for STEMI | 55 (6.5) | 51 (8.7) | 0.00340 |
| Rescue for STEMI | 8 (1.0) | 17 (2.9) | |
| Early invasive for NSTEMI/UA | 275 (32.9) | 209 (35.9) | |
| Elective for SA | 499 (59.6) | 306 (52.5) | |
| Previous MI, n (%) | 124 (14.8) | 70 (12.0) | 0.5250 |
Table 1: Clinical Characteristics of study population according to sex (n=1420)
BMI: body mass index; BSA: body surface area; CKD: chronic kidney disease; CVD: cardiovascular disease; MI: myocardial infarction; NSTEMI: no ST elevation myocardial infarction; PCI: percutaneous coronary interventions; UA: unstable angina; SA: stable angina; STEMI: ST elevation myocardial infarction;
§CKD defined by creatinine levels ≥ 1.5 mg/dl.
When the study population was split according to the presence of ACS, sex gender disparities persist.
Angiographic data are reported in table 2 for ACS patients and in table 3 for SA.
| Variables | Men (N=338) | Women (N=277) | P |
| Epicardial Coronary Angiographic Data | |||
| Normal or non epicardial occlusive disease | 22 (6.5) | 28 (10.1) | 0.055 |
| One-vessel disease | 96 (28.4) | 92 (33.2) | |
| Two-vessel disease | 69 (20.4) | 61 (22.0) | |
| Three-vessel disease or left main | 151 (44.7) | 96 (34.7) | |
| Site of coronary lesion, n (%) | |||
| Right coronary artery | 26 (7.7) | 15 (5.4) | 0.2081 |
| Left anterior descending artery or Left circumflex artery |
108 (31.9) | 99 (35.7) | |
| Both | 180 (53.2) | 134 (48.4) | |
| Therapy strategy, n (%) | |||
| Conservative | 127 (37.6) | 109 (39.3) | 0.47746 |
| Invasive PCI | 198 (58.6) | 162 (58.5) | |
| Invasive CABG | 13 (3.8) | 6 (2.2) | |
| PCI Revascularization therapy | |||
| NO | 140 (41.4) | 115 (41.5) | 0.38162 |
| PCI on Right Coronary Artery | 132 (39.0) | 26 (9.4) | |
| PCI on Left Coronary Artery | 132 (39.0) | 111 (40.1) | |
| PCI on Both | 22 (6.6) | 25 (9.0) | |
| PCI with stent implantation (≤ 2) | 172 (83.5) | 144 (87.3) | 0.3089 |
| Stent Implanted, n (%) | |||
| BMS | 87 (25.7) | 79 (28.5) | 0.4396 |
| DES | 110 (32.5) | 81 (29.2) | 0.3785 |
| Management STEMI, n (%) | |||
| Primary PCI for STEMI | 26 (76.5) | 27 (61.4) | 0.11797 |
| Rescue PCI for STEMI | 8 (23.5) | 17 (38.6) | |
Table 2: Procedural data of patients with Acute Coronary Syndrome (n=615) according to sex.
BMS: bare metal stent; CABG: Coronary Artery Bypass Graft; DES: drug-eluting stent; PCI: percutaneous coronary intervention; STEMI: ST elevation myocardial infarction.
| Variables | Men (N=499) | Women (N=306) | P |
| Epicardial Coronary angiographic data, n (%) | |||
| Normal | 109 (21.8) | 63 (20.6) | 0.6625 |
| One-vessel disease | 156 (31.3) | 90 (29.4) | |
| Two-vessel disease | 87 (17.4) | 64 (20.9) | |
| Three-vessel disease or left main | 147 (29.5) | 89 (29.1) | |
| Site of coronary lesion, n (%) | |||
| Right coronary artery | 41 (8.2) | 16 (5.2) | 0.26647 |
| Left anterior descending artery or Left circumflex artery | 160 (32.1) | 94 (30.7) | |
| Both | 187 (37.5) | 131 (42.8) | |
| Therapy strategy, n (%) | |||
| Conservative | 249 (49.9) | 169 (55.2) | 0.04902 |
| Invasive PCI | 223 (44.5) | 130 (42.5) | |
| Invasive CABG | 28 (5.6) | 7 (2.3) | |
| Revascularization therapy, n (%) | |||
| PCI on Right Coronary Artery | 44 (19.7) | 23 (17.7) | 0.62359 |
| PCI on Left Coronary Artery | 160 (71.7) | 91 (70.0) | |
| PCI on Both | 19 (8.6) | 16 (12.3) | |
| PCI with stent implantation (≤ 2), n (%) |
202 (87) | 114 (86) | 0.7148 |
| Stent Implanted, n (%) | |||
| BMS | 75 (15.0) | 43 (14.5) | 0.7034 |
| DES | 147 (29.4) | 86 (28.1) | 0.6808 |
Table 3: Procedural data of patients with Stable Angina (n=805) according to sex
BMS: bare metal stent; CABG: Coronary Artery Bypass Graft; DES: drug-eluting stent; PCI: percutaneous coronary intervention; STEMI: ST elevation myocardial infarction.
Survival analysis: After a median [IQR] follow-up time of 39.0 (IQR: 16-71) months a total of 514 (36%) patients died: 24 (2.2%) cardiac deaths, 54 (5.0%) all-cause death events were recorded. Table 4 reports baseline demographic and clinical characteristics of patients who experience the clinical outcomes.
| Variables | ALIVE PATIENTS (N=906) | DIED PATIENTS (N=514) | P |
| Sex female, n (%) | 386 (42.6) | 197 (38.3) | 0.11530 |
| Age, years, mean ± SD | 83.1 ± 2.7 | 83.1 ± 2.9 | 0.86446 |
| Age classes, n (%) | |||
| ≤ 85 years | 748 (83.6) | 427 (83.0) | 0.8057 |
| >85 years | 158 (17.4) | 87 (17.0) | |
| BMI, (kg/m2) mean ± SD | 25.8 ± 3.9 | 25.7 ± 3.8 | 0.31345 |
| Abnormal nutritional State, n (%) | 589 (65.0) | 309 (60.1) | 0.06603 |
| BSA, (m2) mean ± SD | 1.76 ± 0,17 | 1.76 ± 0.17 | 0.9922 |
| Femoral Vascular Access, n (%) | 281 (31.0) | 240 (46.7) | <0.0001 |
| Familial history of CVD, n (%) | 236 (26.0) | 121 (23.5) | 0.29519 |
| Hypertension, n (%) | 649 (71.6) | 338 (65.8) | 0.02084 |
| Smoking Habit, n (%) | 401 (44.3) | 244 (47.5) | 0.24295 |
| Diabetes, n (%) | 242 (26.7) | 168 (34.6) | 0.00168 |
| Dyslipidemia, n (%) | 374 (41.3) | 180 (35.0) | 0.02011 |
| CKD§, n (%) | 125 (13.8) | 99 (19.3) | 0.00664 |
| Reasons for angiography, n (%) | |||
| Stable Angina | 533 (59) | 272 (53) | 0.03073 |
| Acute Coronary syndrome | 373 (41) | 242 (47) | |
| Coronary vessel lesions | |||
| Normal epicardial arteries or non-occlusive disease | 168 (18.5) | 54 (10.5) | <0.0001 |
| One-vessel disease | 307 (33.9) | 127 (24.7) | |
| Two-vessel disease | 174 (19.2) | 107 (20.8) | |
| Three-vessel disease or left main | 257 (28.4) | 226 (44.0) | |
| Invasive PCI, n (%) | 476 (52.5) | 237(46.1) | 0.01987 |
| Conservative therapy, n (%) | 403 (44.5) | 252 (49.0) | 0.09865 |
| Previous MI, n (%) | 140 (15.4) | 107 (20.8) | 0.01038 |
Table 4: Baseline Characteristics According to Survival
BMI: body mass index; BSA: body surface area; CKD: chronic kidney disease; CVD: cardiovascular disease; MI: myocardial infarction; NSTEMI: no
ST elevation myocardial infarction; PCI: percutaneous coronary interventions; UA: unstable angina; SA: stable angina; STEMI: ST elevation myocardial
infarction;
§CKD defined by creatinine levels ≥ 1.5 mg/dl.
No differences in mortality were found according to sex. Significantly higher rates of all events considered were found for patients receiving femoral vascular access, diabetics, with chronic kidney disease, with a three-vessel disease, presenting with an ACS and with a previous history of MI. Survived patients had more commonly treated hypertension, treated dyslipidemia, stable angina, a lower coronary impairment.
No sex differences in all-cause mortality and cardiac death were observed along the follow-up. Nevertheless, the KM curves showed a trend in better prognosis in female group (Figure 1).

Figure 1: Kaplan-Meier curves according to sex for all-cause death (panel A) and cardiac death (panel B)
Kaplan-Meier curves analysis showed that very elderly patients had a higher risk for occurrence of cardiac death (Log-rank: 7.91, p=0.005), and all-cause death (Log-rank: 5.51, p<0.001) compared to patients with less than 85 years old (Figures 2 and 3, Panels A-B). This difference persists even when the survival analysis was adjusted for revascularization strategy (Log-rank=5,379, p=0.02 and Log-rank=7,573, p=0.006 for allcause death and cardiac death respectively) (Data not shown).
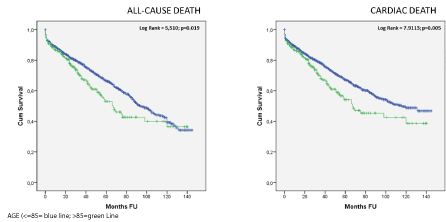
Figure 2: All-cause death (panel A) and cardiac death (panel B) according to age cut-off of 85 years
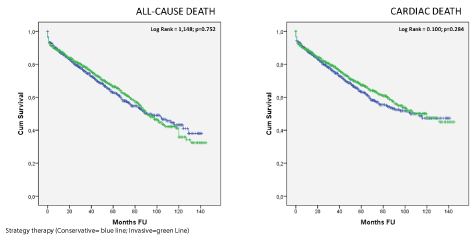
Figure 3: Kaplan-Meier curves according to Treatment Strategy (i.e. conservative vs. intensive) for all-cause death (Panel A) and cardiac death (Panel B).
All-cause mortality: On Cox proportional hazard analysis male sex [Hazard Ratio (HR)= 1.24, 95% Confidence Interval (CI): 1.03-1.48, p= 0.020], age more than 85 years (HR=1.38, 95% CI: 1.09-1.76, p=0.006), presence of diabetes (HR=1.33, 95% CI:1.10-1.59, p=0.002), treated dyslipidemia (HR=0.80, 95% CI:0.77-0.96, p=0.019), CKD (HR=1.43, 95% CI:1.15-1.78, p=0.001), concomitant valvular disease (HR=1.51, 95% CI:1.08-2.11, p=0.014), myocardial infarction clinical presentation (HR=1.32, 95% CI:1.09-1.61, p=0.004), are independent predictors of overall mortality in a model adjusted for nutritional state, vascular femoral access, familiar history of CVD, smoking, treated hypertension, extension of coronary vessel lesions, invasive therapy strategy and CKD.
Cardiac death: On Cox proportional hazard analysis male sex (HR 1.20, 95% CI:1.00-1.46, p=0.050], age more than 85 years (HR=1.43, 95% CI: 1.13-1.81, p=0.003), presence of diabetes (HR=1.36, 95% CI:1.12-1.64, p=0.002), treated dyslipidemia (HR=0.87, 95% CI:0.65- 0.95, p=0.016), CKD (HR=1.40, 95% CI:1.11-1.76, p=0.004), myocardial infarction clinical presentation (HR=1.32, 95% CI:1.09-1.61, p=0.004), are independent predictors of cardiac death in a model adjusted for nutritional state, vascular femoral access, concomitant valvular disease familiar history of CVD, smoking, treated hypertension, extension of coronary vessel lesions, invasive therapy strategy and CKD.
The major findings of this study, including a large unselected cohort of very elderly patients, all underwent diagnostic coronary angiography followed by elective or primary interventions, are the following: first, compared with men, women presenting with symptoms of myocardial ischemia are older, have a higher rate of traditional risk factors and account for an increased number and proportion of primary PCIs. Second, despite these heavier risk factors burden, reperfusion in women was associated with a better outcome at follow-up. However, a dilution of the efficacy occurred with increasing age and associated comorbidities, and for male patients, the benefit of the invasive strategy was not clear. Third, although in the setting of the stable angina conservative strategy was the more frequent option women had, no sex differences in all-cause mortality and cardiac death were observed over the follow-up. Fourth, no sex disparities in antiplatelet therapy were detected with most patients (80%) with stent treated with aspirin and clopidogrel. Moreover, the long median follow-up allowed us to evaluate the safety profile of long standing medical therapy, specifically clopidogrel, and its role in preventing adverse cardiac events in the very elderly population. Finally, no significant sex differences in the burden of obstructive epicardial disease were observed in both ACS and SA patients. In 52% (ACS, n=371; SA, n=366) of patients, PCI with implantation of one or more stents were performed. Thus, the results of the present study point out the challenge of managing elderly population presenting with myocardial ischemia.
In the next years, along with chronological increase of the population, very elderly patients will more likely be female, more often with a high rate of risk factors, heavier comorbidities, and presenting later in the course of IHD than male counterparts [8].
During the last years, elderly patients have experienced considerable improvements in in-hospital outcomes and these improvements were accompanied by increases in the use of reperfusion therapies. Despite that, women have continued to experience a worse prognosis as compared to men [2,9].
Such female vulnerability, in apparent contrast with widely reported lesser extent of epicardial coronary involvement, has been related to gender differences in clinical presentation, comorbidities, and treatment strategies [10].
Globally, studies conducted largely in men documented a reduction in the risk of adverse cardiac events with a routine interventional strategy. Nevertheless, they suggest the existence of a possible gender difference in the occurrence and extent of benefit of myocardial reperfusion, with a worse outcome in women population. In OASIS 5 women sub-study, a higher risk of mortality at 1-year with an early invasive strategy has been reported. This harm was mainly driven by a higher risk of major bleeding at 30-days with an early invasive strategy [11].
In the ISACS-TC registry [12], 2225 STEMI patients’ ≥ 70 years old (72.8% were ≥ 70 to 79 years old and 27.2% were ≥ 80 years old) were admitted into the network. Primary PCI decreased the unadjusted risk of death both in the elderly (OR: 0.32, 95% CI: 0.24-0.43) and very elderly patients (OR: 0.45, 95% CI 0.30-0.68), without significant difference between groups. The rate of death was two times greater for those patients who did not receive reperfusion. Of note, among others female gender was the only independent factor associated with the lack of use of reperfusion in both groups confirming that sex disparities in treatment persist in the older female population.
The AMIS Plus project [13] by analyzing temporal trends in the treatment and outcomes of older patients with ACS, documented that this cohort of patients has considerable improvements in short-term in-hospital outcomes by increasing the use of guideline-recommended therapies. Furthermore, the increased PCI use was not associated with lower effectiveness to prevent in-hospital death, despite its use in increasingly older (i.e. septua-, octo-, and nonagenarians) and co-morbid patients.
Taken together, these findings suggested that reperfusion therapy by PCI, along with recommended more effective drugs, in old patients are beneficial, leading to reduced risk mortality. In our study, conservative and invasive strategies were associated with a similar long-term survival for both sexes over the time. Of note, a trend in the better prognosis in terms of survival of the female group has been observed. Nevertheless, the benefits seem to be reduced with increasing age. Kaplan-Meier curves analysis showed that very elderly patients had a higher risk for occurrence of cardiac death (Log-rank: 7.91, p=0.005), and all-cause death (Logrank: 5.51, p<0.001) compared to patients with less than 85 years old. On multivariable analysis, several co-morbidities were found significantly related to older patients and might contribute to the worse outcome. Of notice, although men with stable angina underwent more frequently elective PCI, in our cohort of patients the benefit of such invasive approach was not evident since the analysis was run considering the CAD severity and the strategy of revascularization regardless sex.
The After Eighty study [14] was the first randomized controlled trial to be specifically designed for the very elderly population with NSTEMI and unstable angina, which are frequent causes of hospital admission in this age group. The Authors documented that invasive strategy is superior to a conservative one in terms of a composite outcome including myocardial infarction, need for urgent revascularization, stroke, and death. However, a dilution of the efficacy occurred with increasing age, and for patients older than 90 years the benefit of the invasive strategy was not clear. Importantly, no specific therapeutic interventions are addressed to elderly women making the results of that trial less conclusive for such population.
More recently, the impact of an early invasive strategy on in-hospital survival, as compared with an initial conservative strategy, has been evaluated exclusively in women with the non-ST-elevation acute coronary syndrome in a real-world scenario. The results of that study confirmed the in-hospital mortality benefit of an early invasive strategy in women with non-ST-elevation myocardial infarction and high-risk features [15].
It should be noted, though data is specifically targeted to women, that a large proportion of enrolled patients aged less than 65 years. Thus, it is difficult to translate those results to the older population.
Importantly, in our analysis of contemporary real‐life data, we enrolled all consecutive male and female patients, aged 80 years or older, with suspected IHD and angiographic definition of coronary involvement. So, the strength of the present study includes a large number of very elderly women (41%) from real world scenario powered enough to assess whether sex and gender differences exist in the management of stable and acute coronary syndromes and in the outcome at a long follow-up.
Thus, we may hypothesize that treatment strategy and clinical variable rather than biological gender disparities might have a pivotal role in affecting clinical outcomes.
Despite clinical benefit offered by recommended treatment strategies, mortality rate is high in the present cohort. It is conceivable that the effects of advancing age itself, including morphological changes with blunted cardiac function, increase the risk of mortality in older patients [16].
In the present study, data regarding cardiac functional parameters are lacking and it may determine a confounding effect on estimation of factors predicting mortality.
Therefore, presenting symptoms and time from symptom onset to reperfusion were not recorded. Elderly patients often present with atypical symptoms, causing delay in diagnosis and effective treatment. It results in a worse pre-intervention hemodynamic status that causes higher mortality rates [17,18].
In addition, biochemical markers of periprocedural injury were not assessed. Noteworthy, a meta-analysis from 20 studies over 19-year period, showed a significant correlation between increased mortality and troponin elevation after elective PCI [19].
Finally, no angiographic indexes of myocardial reperfusion enter the statistical analysis. Elderly patients are more likely to have a lower postprocedural myocardial perfusion grade resulting in a reduced ventricular functional recovery that adversely affects the outcome [20,21].
The increasing proportion of elderly in the general population is expected to continue over the next years, suggesting that the need for managing older patients will continue to increase. Our data support the evidence that an invasive strategy including optimal medical treatment along with percutaneous interventions reduces the mortality rate by offering a similar survival improvement for both sexes. Furthermore, the benefit remains unchanged with increasing age. However, these findings must be interpreted with caution and further studies addressed to elderly women are needed to evaluate the relative merits of available reperfusion strategies as well as newer antithrombotic adjunctive therapies.
Download Provisional PDF Here
Article Type: Research Article
Citation: Tanzilli G, Arrivi A, Raparelli V, Truscelli G, Viceconte N, et al. (2017) Outcome of Very Elderly (Octogenarians) Patients with Coronary Artery Disease, All Diagnosed by Coronary Angiography. J Epidemiol Public Health Rev 2(3): doi http://dx.doi.org/10.16966/2471-8211.147
Copyright: © 2017 Tanzilli G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access