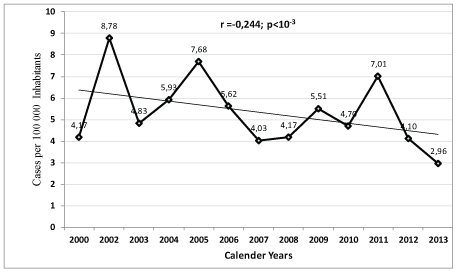
Figure 1: Trend of crude incidence rate/105 Inh of pericarditis: from 2000 to 2013 in Monastir population (Tunisia)


Asma Sriha Belguith1* Ikram Toumi2 Ines Bouanene1 Manel Ben Fredj1 Hela Abroug1 Arwa Ben Salah1 Sana El Mhamdi1 Aymen El Hraiech3 Zohra Dridi3 Majed Hassine3 Afifa Abdelkafi Koubaa2 Khaldoun Ben Hamda3 Habib Gamra3 Faouzi Maatouk3 Mohamed Soltani1
1Department of Epidemiology and Preventive Medicine, University Hospital of Monastir, Tunisia*Corresponding author: Asma Sriha Belguith, Department of Epidemiology and Preventive Medicine, University Hospital of Monastir, Tunisia, Tel: +216 97238022; E-mail: belguith_asma@yahoo.fr
Objective: We aimed at estimating the standardized incidence rate (SIR) of hospitalizations for acute pericarditis (HAP) in Monastir governorate.
Methods: We have enrolled a prospective study including all patients residents of Monastir, newly diagnosed with AP, admitted in cardiology departments between 2000 and 2013 (2001 not included). Data was collected from the regional register of Monastir hospital morbidity. The HAP crude incidence rate (CIR) was calculated based on the Tunisian population statistics, expressed per 105 inhabitants. The age-standardized incidence Rate (SIR) was calculated using the world standard population.
Results: During study period, 333 patients have been newly admitted for AP. The mean age was 53 (IQR: 39-65) years and sex ratio was 0.85. CIR was 5.22 per 105 inh with a strong positive correlation between age and CIR (r=0.892, p=0.000). We have notified a negative trend of CIR (r=-0.244, p=0.000) from 2000 to 2013.The SIR was 7.41 PY being 7.32 in men and 7.49 in women (p=0.139). HAP lethality was 2.1% being 3.0% in elderly. Hospitalizations for AP represented 1.26% of all cardiology admissions (95%, CI: 1.13-1.39). The median length of hospital stay was 8 days (IQR: 4-14).
Conclusion: we have notified a significant decrease in incidence of HAP, further to epidemiological transition in developing country, lethality is being considerable yet.
Acute Pericarditis; Inpatients; Incidence; Epidemiological Transition; Tunisia
Acute Pericarditis (AP) is the most frequent form of pericardial disease encountered in clinical practice [1] and it is relatively common cause of chest pain since it is diagnosed in approximately 5% of patients who have non ischemic chest pain in emergency departments [2,3]. Although AP has generally a brief and benign course after treatment by non steroidal anti-inflammatory drugs (NSAIDs), it can lead to significant morbidity as well as potentially life threatening complications such as cardiac tamponnade and pericardial constriction [3,4]. While viral or idiopathic pericarditis is responsible for the majority of AP cases in Europe and the USA [5], tuberculosis is the most common cause of pericarditis in developing countries [6,7].
Several studies have reported on diagnosis, etiologies and management of AP. Especially, Imazio and colleagues have greatly described the triage and the management of acute and recurrent pericarditis through series of carefully designed prospective investigations [1,3,5,8-12]. However few epidemiological reports on AP have been published [10,12]. In Tunisia, there are no official epidemiological data on AP. This study aims to estimate the incidence rate of hospitalizations for AP (HAP) in Monastir city (Tunisia).
The Hospital Monastir register is an ongoing survey initiated in 1990 [13]. Monastir University Hospital is a public health institution with two cardiology departments applying high cardiologic expertise and provide medical care according to international standards. Monastir is a center coastal city, with an average temperatures fluctuating from 17 in January to 33°C in August.
Newly AP diagnosed, residents in Monastir governorate, and hospitalized in the university hospital of Monastir between 2000 and 2013, encoded according to CIM 10 as I30, have been selected (2001 was not included for data capture problems). Patients aged less than 14 years were managed by the pediatric department.
Data including 205451 hospitalizations, during the period study, was collected in the regional register of hospital morbidity, implanted at the Department of Preventive Medicine and Epidemiology [13]. The socio-demographic variables recorded were age, gender, and residence delegation. We identified hospitalization characteristics (department, length of stay, number of episodes).
Data was verified, Adjusted on patients, Monastir inhabitants, and analyzed using Statistical Package for Social Science (SPSS), software version 21.0. The crude incidence and mortality rates (CIR, CMR) of HAP were calculated based on the Tunisian INS population and expressed per 105 Inh [14,15]. The age-standardized incidence and mortality Rates (SIR, SMR) per 105 person-years (PY) were calculated among the world standard population according to WHO statement 2013. We have estimated the number of annual new AP cases in Tunisia by weighing the demographic distribution of the inhabitants of Monastir against those of all of Tunisia. Distribution normality of continuous variables was verified by the KS test. Non-normally distributed continuous variables (length of stay) were presented as median value and inter-quartile range (IQR). Appropriate tests were used and p-Values of b 0.05were considered. The trends were performed using the correlation test of Pearson (r).
Three hundred and thirty three patients have been hospitalized for infective AP. We noted a mean of 26 new cases per year in Monastir governorate. We estimated 521 to be the number of annual new HAP in Tunisia. Median age was 53 (IQR: 39-65) years, being 49 (IQR: 36-61.75) years in men and 57 (IQR: 40.25-70) years in women (p=0.002). Sexratio was 0.85. The CIR was 5.22 cases/year/ 105 Inh. It was higher among patients aged more than 60 years (24.8 /105Inh) compared to younger (p=0.000). A significant positive and very high correlation was noted between age and CIR/105 Inh (r=0.892, p=0.000). The SIR per 105 PY was 7.41, being 7.32 in men and 7.49 in women (p=0.139). Eight patients died whose five aged more than 60 years. AP lethality was 2.1% being 3.0% in elderly. Age-SMR was 0.17 per 105 PY, being 0.24 in men and 0.19 in women (p=0.8) (Table 1).
| HAP Cases | p | CIR/105 Inh | r* (p) | Age-SIR/105 PY | Lethality n (%) | CMR/105 inh | Age-SMR/105 PY | |
| 2000-2013 (unless 2001) | 333 | 5.22 | 7.41 | 7 (2.1) | 0.11 | 0.17 | ||
| Age (n=331) | ||||||||
| 24 | 42 | 0.000 | 1.39 | 1 (2.4) | 0.03 | |||
| 25-39 | 39 | 2.51 | 1 (2.6) | 0.06 | ||||
| 40-59 | 116 | 9.24 | 1 (0.9) | 0.07 | ||||
| ≥ 60 | 134 | 24.85 | 4 (3.0) | 0.74 | ||||
| 0.892 (0.000) | ||||||||
| Gender (n=333) | ||||||||
| Men | 153 | 0.139 | 4.73 | 7.32 | 4 (2.6)* | 0.12 | 0.24 | |
| Women | 180 | 5.73 | 7.49 | 3 (1.6)* | 0.09 | 0.19 |
Table 1: Crude and standardized incidence rates, crude and standardized mortality rates of patients hospitalized for acute pericarditis in Monastir (Tunisia) from 2000 to 2013.
The CIR was the highest in 2002 with 8.78 cases /year /105 Inh. A significant and negative, decrease of AP cases was notified from 2000 to 2013 (r= -0.244, p=0.000) (Figure 1).

Figure 1: Trend of crude incidence rate/105 Inh of pericarditis: from 2000 to 2013 in Monastir population (Tunisia)
Over 13 years, cardiology services have recruited 28911 admissions, among them 366 HAP. Prevalence was 1.22% [95% CI: 1.13-1.39%] being 2.5% among patients aged less than 20 years. This prevalence decreased with increasing age until 0.59% in patients aged 60 years or older. The proportion of decrease was estimated at 56.7% per 15 years increase in age. Among pediatric age, the AP prevalence was significantly higher in boys (5%) than in girls (0.69%) (p=0.000). The median hospital length of stay was 8 days (IQR: 4-14), it was higher among women (9 days (IQR: 5-17)). Readmission occurred in 28 of 333 patients (8.4%) (Table 2). It was equivalent in men (n=13) and women (n=15).
| Prevalence of hospitalizations in Cardiology services: % |
354 /28911$=1.22 | |
| In men | 1.01 | |
| ≤ 14 years | 4.29* | |
| 15-29 years | 5.34 | |
| 30-44 years | 2.61 | |
| ≥ 45 years | 0.70 | |
| In women | 1.47 | |
| ≤ 14 years | 0.69* | |
| 15-29 years | 5.19 | |
| 30-44 years | 2.09 | |
| ≥ 45 years | 1.27 | |
| Input mode: N; % | ||
| Outpatient | 118 | 32.2 |
| Emergency | 248 | 67.8 |
| Length of stay: M; IQR | ||
| All | 8 | 4-14 |
| Men | 6 | 3-11£ |
| Women | 9 | 5-17£ |
| Number of hospitalizations: N; % | ||
| 1 | 305 | 94.8 |
| 2 | 24 | 4.0 |
| ≥ 3 (13 hospitalizations) | 4 | 1.2 |
Table 2: Description of hospitalizations for Pericarditis (n=366).
In our study, we described the epidemiology and trends of HAP from 2000 to 2013 in a university hospital in Tunisia. This work falls within an array of articles describing the hospital morbidity in this hospital using its regional register. The SIR was 7.41 per 105 PY. AP lethality was 2.1%. HAP represented 1.22% of all cardiology departments [95% CI: 1.13-1.39%]. The median hospital length of stay was 8 days (IQR: 4-14).
For results, the CIR in our study was 5.22 cases/year/1055 Inh, and SIR was 7.41 per 105 PY. It was similar to a retrospective study including hospitalized and non hospitalized AP, wherein the incidence was 7.4/105 Inh [16] and to a national US study in which Kumar et al. estimated a CIR of 5.75/105 Inh [17]. Our values were higher than those described by Kito et al. [18] with a SIR of 3.32/105 Inh. Authors, explained this low SIR to the exclusion of regional hospitals. CIR was lower that described in a prospective observational cohort study involving two general hospitals from an Italian urban area by Imazio et al. [5] (27.7 cases/year/105 Inh). The variability of CIR and SIR can be explained by the inclusion criteria (HAP and non-hospitalized AP). In fact Our data have underrepresented patients with low-risk features that may be treated without admission. Delon et al. [19] determined that 27% of all patients diagnosed for AP in the emergency room were hospitalized. In addition, we highlight that many clinically silent cases of AP were under diagnosed and misdiagnosed [20], following to difficulty of diagnosis and distinction between pericarditis from myocardial infarction [3]. Therefore AP is detected in several autopsy series (1 to 6%) [10]. Over our study period, there was a negative trend in AP hospitalizations (r= -0.244, p=0.000). Several factors may be responsible for this decrease. It’s due to the communicable diseases decrease, the most common cause of pericarditis in developing countries [13,21] as was noted for the decline of rheumatic heart disease [14]. Our finding is in agreement with the recent US study that reported a significant decline in HAP rates from 6.6 to 5.4/105 Inh from 2003 to 2012 [17]. In Sub-Saharian Africa, the incidence of AP is increasing in response to HIV epidemic which has drag along an increase in all extra-pulmonary tuberculosis forms including pericardial localization [7,22].
The median age of 53 years (IQR: 39-65) in our population was comparable to that reported by Nilay in USA (53.5 years) [17] and that reported by Kyto in Finland (52 years) [18]. CIR was higher among the population aged 60 years and over with 24.8/105 Inh compared to younger (p=0.000). Younger patients tend to have lower incidence of HAP which is consistent with another study [18]. There was no statistically significant sex difference in HAP (p=0.139). Previous studies revealed conflicting results regarding sex differences in the HAP incidence. According to Imazio, there is no specific gender predisposition to pericarditis, although female gender has been reported as a possible risk factor [12] while several others researches have reported a men predominance in HAP [17- 19,21,23]. Men predominance was explained in literature by sex hormone differences and especially by the anti-inflammatory effects of oestrogen and the pro-inflammatory role of testosterone in the pericardial tissue [18,24]. According to Laufer-Perl et al. [24], men predominance may have been due to under-diagnosis of AP among women. In fact, it is possible that women having chest pain seek medical attention less frequently [25].
In our study, HAP represented 1.22% of all cardiology hospitalizations it was higher than that reported in a previous study (0.2%) [18]. AP prevalence decreased with age rising. This is consistent with the finding of the Finnish study that estimated a prevalence of HAP around 4% in young aged between 16 and 20 years, the proportion decreasing by estimated 51% per 10 years increase in age attaining 0.02% in patients aged more than 84 years [18]. The most patients with idiopathic pericarditis have a benign course after treatment by NSAIDs [4,10], not all patients need to be hospitalized. While in the 2004 European Society of Cardiology (ESC) guidelines, hospitalization and cause search were recommended in all patients with pericarditis [26], the recent 2015 ESC guidelines recommended that hospitalization should be restricted to patients with at least one predictor of poor prognosis and to those which the clinical presentation may suggest an underlying etiology. On the other hands, patients without these features can be managed as outpatients with empiric NSAIDs and a short-term follow up after 1 week to assess the response to treatment. In fact, in an observational study, Imazio et al. [6] selected 254 out of 300 (84.7%) patients as low-risk cases to be treated as outpatients, and reported that there were no serious complications in a mean followup of 38 months [8,27]. This triage may allow a cost-effective approach reducing the admissions and diagnostic investigations. Hospitalization in AP aims to determine the etiology, to start treatment and observe for complications particularly pericardial effusion and cardiac tamponnade [10]. In our study, the median length of hospital stay was 8 days (IQR: 4-14) which is higher than that reported by Kyto (5 days) [18] and that reported by Nilay (4-5.1 days) [17]. In a multicenter study focusing on hospitalizations for idiopathic pericarditis and pericardial effusion among children, the median length of hospital stay was only 3 days (IQR: 2-4) [28-33]. Recurrent pericarditis characterized by a recurrence of symptoms after a documented first episode of AP and a symptom-free interval of at least 4-6 weeks [6]. It is one of the most troublesome complications of AP [9]. Tonini et al. [2] found that the risk of recurrence was higher for women and for patients who do not respond to initial treatment with NSAIDs. In our study, readmissions for AP occurred in 28 of 333 patients (8.4%). They could be underestimated by the absence of the inclusion of outpatient data managed in the emergency room. The in-hospital lethality rate of 2.1%, in our study, was higher than that reported in previous studies [17,18]. Kyto et al. [18] found that increasing age and severe co-infections (pneumonia or septicemia) are associated with greater in-hospital mortality in AP.
Our study has some limitations. First, it focused on HAP and did not include any data pertaining to AP care in outpatient settings or emergency departments as such it may underestimate the overall AP incidence rate. Second, it was an analysis drawn from a register database. This implies a lack of information on potential comorbidities and on medication. Lastly, the nature of our data allowed us to only examine in-hospital mortality related to AP. Despite these limitations, to our knowledge this is the first study to evaluate incidence, prevalence and trends of HAP among a sample of Tunisian population and it fills an important gap in knowledge of the HAP epidemiology in a developing countries.
In conclusion, epidemiological data on HAP are scarce. This study was able to document HAP incidence of 7.41/105 Inh in Monastir city. There was a significant decrease in AP hospitalizations over the study period. We have been able to demonstrate that pericarditis is in regression following the evolution of the health system in Tunisia and the improvement of the quality of life of citizens. Yet further studies focusing on outpatients AP epidemiology are needed.
The authors have nothing to disclose concerning this manuscript.
No financial support was provided for the conduct of the research and the preparation of this paper.
The study was conducted under good clinical practice conditions and according to the ethical standards collections. Each patient in the study is assigned a unique identifying code and all documents labeled accordingly to maintain anonymity
Download Provisional PDF Here
Article Type: Research Article
Citation: Belguith AS, Toumi I, Bouanene I, Fredj MB, Abroug H, et al. (2017) Hospitalization for Acute Pericarditis in a Developing Country: Incidence and Trend (2000-2013). J Epidemiol Public Health Rev 2(4): doi http://dx.doi.org/10.16966/2471-8211.146
Copyright: © 2017 Belguith AS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access