Introduction
Recently, over a 4-month period on an American Indian reservation, 11 suicides were completed among children ranging in age from 11 to 17 years old. Local clinic staff reported the occurrence of up to 20 suicide attempts each week in their catchment area of approximately 20,000 residents in as many square miles. The gravity of the conditions among this minority is widely underappreciated by mainstream health care professionals. And while tireless efforts to manage and reverse these circumstances continue, far more is needed and our hope is to promote change first through greater understanding.
Depression and hopelessness permeate such communities, and the causal factors are deeply engrained and intricately complex. They include persistent unemployment, poverty, poor education, family dysfunction, addiction, numerous medical comorbidities, deficient health care, and historic unresolved grief. American Indians have a long history of oppression, exploitation, and trauma which has remained unresolved. Contemporary American Indians continue to experience the consequences of cultural genocide; the incidence of depression and suicide, homicide, child abuse and domestic violence, and addiction are tragically elevated. Government and non-profit programs have only been marginally effective, and local programs fight to contain what is considered an epidemic. Increasing awareness and redirecting efforts is essential to effect change and reverse this life-threatening emotional anguish.
Discrepancies in Wellness and Health Care
In 2009, the rate of suicide among American Indian adolescents and young adults, ages 15-34, was 2.5 times higher than the overall national average for that age group (31 per 100,000 versus 12.2 per 100,000) making suicide the second leading cause of death among adolescent and young adult American Indians [1]. In a 2006 national survey, it was found that among U.S. males over the age of 18 who listed a single race, American Indians (including Native Alaskans) had the highest rate of “a serious psychological stress” (25.9%) and the highest rate of a major depressive episodes (12.1%) within the preceding year [2]. A 2013 study by Ehlers et al. examined the disproportionately high rate of traumatic events among American Indians. They found that out of 309 participants, approximately 94% experienced traumatic events in their lifetime (74% unexpected death, 66% injury/assault, 49% non-injurious crime, 45% witnessing trauma, 36% natural disaster, 22% sexual abuse, 1% military combat) [3]. They concluded that post traumatic stress disorder (PTSD) symptoms as well as experiencing assaultive trauma was moderately heritable (30-50%), a finding supported by previous studies suggesting that genetic factors can account for 30% of PTSD symptom variance and can also influence trauma exposure [4]. Additionally, a correlation was found between substance abuse categories (alcohol, marijuana, and stimulant dependence) and antisocial personality disorder/conduct disorder, and a correlation between mood disorders and PTSD [3]. These findings are consistent with numerous studies associating depressive illness as a sequela of trauma (US Department of Veterans Affairs; National Center for PTSD) [5,6]. Furthermore, The Depression and Bipolar Support Alliance report that not only those who directly experience traumatic events, but those who hear about them, may develop a depressive illness.
Mental health concerns within American Indian communities are far from a new issue. Reports exist from the early 1970’s citing how the health and welfare of these communities were neglected by the federal government [7]. Despite education, awareness, and legislation promising the provision of health/mental health care by the government to the tribal communities [8], rates of depression, suicide, and other diseases remained at much higher levels than the general US population. To illustrate some of the persisting health discrepancies, based on data published between 2006 and 2014, age-adjusted mortality rates for death due to alcohol use, chronic liver disease, diabetes, unintentional injury, suicide, homicide and influenza are all higher in the American Indian population than the general population (Figure 1). An additional 2007 study by Tann et al. [9] found that American Indians/Native Alaskans are at elevated risk for the independent and combined presence of alcohol abuse, depression, and diabetes with an odds ratio of 12.5.
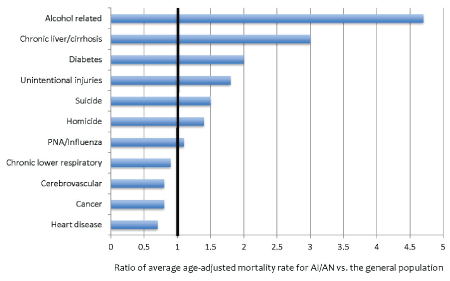
Figure 1: Ratio of average age-adjusted mortality rates for selected high-impact illnesses for American Indians/Native Alaskans vs. general population. Data published by multiple sources between 2006 and 2014 were used to calculate the ratio of mortality rates for the general non-Hispanic white population versus American Indians/Native Alaskans [5-8]. The mortality rates for the general population were adjusted to 1, as indicated by heavy black line.
In addition to, and contributing to, the discrepancies in physical and mental health, is the dramatic difference in rates of poverty and unemployment among the American Indian demographic. According to census data collected between 2007 and 2011, American Indians as a whole have a poverty rate of approximately 27.0%, 12.2 points above the concurrent national rate of 14.7; and when broken down by state, American Indian populations have a poverty rate of 30% or more in Arizona, Maine, Minnesota, Montana, Nebraska, New Mexico, North Dakota, South Dakota and Utah. In some communities, the poverty rate is 50.9% (Rapid City, S.D.) [10]. and while the entire nation is still recovering from a major recession, unemployment rates remain markedly higher for American Indians throughout the country (Table 1) [11].
| |
Native American |
White |
Native American-to- White Ratio |
| Alaska |
11.7% |
5.5% |
2.1 |
Midwest
(AK, IL, IN, IA, MI, MN, MO, OH, WI) |
16.8% |
7.0% |
2.4 |
Northern Plains
(ID, MT, NNE, ND, SD, WY) |
15.0% |
4.6% |
3.3 |
Northeast
(CT, DE, DC, ME, MD, MA, NH, NJ,
NY, PA, RI, VT) |
8.3% |
7.1% |
1.2 |
| Southern Plains (KS, OK, TX) |
6.8% |
5.7% |
1.2 |
Southeast
(AL, FL, GA, KY, LA, MS, NC, SC, TN, VA, WV) |
11.5% |
6.4% |
1.8 |
Southwest
(AZ, CO, NV, NM, UT) |
15.0% |
6.9% |
2.2 |
West
(CA, HI, OR, WA) |
10.8% |
8.5% |
1.3 |
Table 1: Native American unemployment rates compared to non-Hispanic Whites by region for the first half of 2013. Adapted from Austin, 2013
Contributing Factors
Several factors, both past and present, have contributed to the failure of the mental health system in native communities. It is first helpful to discuss why outreach programs aimed at eliminating health disparities in general have failed to produce improved health of their target communities. We will then discuss factors that are particularly relevant in the case of mental health among American Indians.
Due to a paucity of studies specifically looking at the cultural competency of outreach programs in American Indian communities, we have expanded our research to include other cultures to better illustrate related concerns. Reviewing the literature reveals several reoccurring themes as to why well-meaning, global outreach efforts are unsuccessful despite the fact that these programs can be aimed at seemingly vastly different target groups. Basically, these themes include 1) deficient resources and financial support, 2) dissatisfaction and general mistrust of outsiders and Western medicine, 3) practices that lack cultural competency, 4) perceived or real discrimination towards individuals who seek help, and 5) a misguided sense that doing something is better than doing nothing. Quality healthcare comes at a cost that is unfortunately unattainable to many families and individuals; however, allocating more government funds towards healthcare is often not a feasible solution. The remaining four themes represent barriers that can be overcome by outreach organizations and can allow these programs to make the largest impact with the resources available.
Outreach programs can only begin to be successful if the target population is willing to seek the treatment provided. Many individuals decline to utilize the resources available because they are weary or unsatisfied with the care being provided or with the providers themselves. In a 2012 study of four sites in Southeast Asia providing neonatal care, the authors opine many families opt to not deliver their children at their local hospital because their faith in local traditional therapies is greater than contemporary treatment [12]. This in part reflects the reality that the neonatal care provided at these facilities often fails to produce more favorable outcomes. In a study of fixed and outreach health services provided by the government in rural Bangladesh, the strongest predictor of a patient’s overall satisfaction rating was whether they felt respect and compassion from the provider [13]. Other studies also cite lack of provider politeness and respect being a barrier to patient utilization of services [14,15]. Another significant barrier is the vast shortage of mental health providers among middle-income countries, including American Indian communities. Perhaps more importantly, the majority of individuals with depression in middle-income countries receive inadequate treatment with only approximately 15-24% of individuals receiving appropriate treatment in 12 months (World Health Organization 2016: http://www.who.int/ mediacentre/factsheets/fs369/en/). These findings highlight the need to understand patient expectations, being aware different cultures may have different expectations, and the ability to balance meeting expectations and psychosocial needs with meeting the clients’ medical needs [13].
Outreach providers and treatments that lack cultural competency often fail to produce successful outcomes. In recent years there has been a strong movement advocating the development of culturally conscious and community-based therapies [16-19]. Culturally conscious and community-based programs have several benefits worth discussing. In communities where colonization is a part of the community’s history, as such is the case among many indigenous groups, a community-based approach could help restore self-sufficiency, dignity, and pride in their heritage and community [19]. It is important to consider the impact of transgenerational grief or ‘historical trauma’; that is, the collective psychological and emotional damage occurring over a lifetime, and often over generations, arising from traumatic experiences affecting an entire group of individuals or communities [20]. The term was originally coined to describe the experience of children of Holocaust survivors, but has since been applied to other victims of genocide and communities subjected to oppression and abuse. It is a useful framework to understand the prevalence of substance abuse and depression among American Indians [16,19,20]. Awareness that historical trauma may play a significant role in a patient’s condition - or a community epidemic - aids in the development and implementation of a treatment program that better addresses the core issues and supports the strength and health of the community and of the individual.
Additionally, even when historical trauma is absent or more indirectly related, programs designed with cultural awareness will always be more relevant and influence the effectiveness of the intervention. As discussed above, an individual’s culture can affect their expectations for treatment, and programs that meet the patient’s expectations are more likely to be trusted and utilized. Further, taking into consideration culturally specific risk factors can improve outcomes, as exampled by the success of culturally adapted treatment and prevention of substance abuse among Latin American youth [21]. Finally, culturally sensitive programs should utilize local practitioners and integrate community beliefs. Working with local providers builds trust, better meets the clients’ expectations, improves the long-term sustainability of the program, improves community independence, and helps restore pride and dignity [17, 19]. Many treatments offered through traditional medicine practitioners are available at a lower cost than conventional treatments, some of which, such as St. John’s wort, have been shown to have comparable efficacy to SSRIs in the treatment of depression [22]. Practitioners of traditional and complementary medicine among lower income communities can help ameliorate the shortage of mental health providers in those communities. Although there are differences in etiologic understanding and implementation of treatments of mental health disorders between conventional western, traditional and complementary practitioners, collaboration across disciplines can appropriately provide effective and adequate care while balancing issues of access [23]. One major problem with community and culturally based interventions, however, is that many currently lack empirical evidence supporting their utility and effectiveness, leading researchers and providers to fall back on more mainstream, “West-is-best” methods [16] which is why there has been a recent surge of support for community-based participatory research (CBPR). CBPR, designed specifically in response to health disparities, “focuses on relationships between academic and community partners, with principles of co-learning, mutual benefit, and long-term commitment and incorporates community theories, participation, and practices into research efforts” [17]. CBPR integrates the benefits of culturally conscious treatment with the need for empirical data that will hopefully result in programs that are culturally sensitive, evidence based, and sustainablebenefitting the community as a whole.
Discrimination towards individuals that seek care, whether real or perceived, can particularly be a problem in mental health treatment. In many cultures, including “main-stream” American culture, stigma and negative stereotypes surrounding mental illness and substance abuse continue to exist. This “double stigma,” causes people of an ethnic or cultural minority with a psychiatric condition to experience the burden of discrimination from two angles: discrimination for being a member of an ethnic minority and discrimination for having a mental illness [24]. Therefore, these individuals will avoid receiving mental health treatment to avoid further discrimination. Understanding the basis for prejudice toward individuals with mental illness, which can be unique in different cultures, can help in the creation of programs that address the specific bias and take advantage of cultural and community values [21]. Discrimination and prejudice is not only a problem in the community at large, it can come from healthcare providers. And while it is more common within the context of mental illness, it can also affect those seeking medical care. Patients who perceived prejudice from their health care provider had worse mental health; specifically, perceived discrimination was strongly correlated with depressive symptoms [15,25]. Discrimination and feeling disrespected can also lead to resistance in seeking or utilizing care [12- 14]. Along with other fundamental issues, short-term community service trips (which will be discussed further) can result in unintentional discrimination, often arising from miscommunication or a lack of cultural competency among volunteers [14,26].
In addition to service trips by doctors and trained healthcare professionals, e.g. Doctors without Borders, the recent past has seen an increase in service trips by medical students, pre-med students, and an increase in organizations specializing in service-based tourism known as “voluntourism” or “responsible tourism”. There is often a notion among these well-intentioned but minimally trained, or completely untrained, volunteers that doing something is better than doing nothing; however, for several reasons, this is not always the reality [14]. Too often it is the case that these short-term medical outreach service trips focus on the symptoms without understanding or attempting to fix the root of the problem. This leads to short-term “band-aid” solutions that do not have a significant long-term effect [14,26]. Short-term service trips often fail to integrate local perspectives, exacerbate dependency by not employing or involving locals even when they are skilled, hinder the progress of established efforts or favor completion over quality and sustainable work, reinforce conceptualizations of “the other” for both locals and volunteers, and perpetuate misunderstandings of poverty [27]. Additionally, the mere presence of volunteers is a potential burden on the hosting community and its resources [14]. For example, the tremendous influx of relief workers and volunteers following the 2010 earthquake in Haiti resulted in a shortage of basic supplies such as water and fuel, making it unavailable to those they were trying to help and in some cases hindering the delivery of additional aid [28].
Barriers
While many of the issues with outreach programs discussed thus far apply to the problem of mental health in American Indian communities, some unique and specific factors merit consideration. American Indians represent the smallest minority group in the United States, comprising only 1.5% of the nation’s population [29]. At the same time, American Indians comprise the most diverse minority, with more than 500 federally recognized tribes [30,31]. The combination of being a small yet culturally diverse population makes conducting studies with an adequate sample size difficult. Calculating accurate rates of occurrence or efficacy of treatment methods and programs is therefore difficult. As an example of the differences that exist between American Indian communities and how it effects health outcomes, Rieckmann et al. [32] found significant differences between an urban and rural population of American Indians enrolled in substance abuse treatment programs; the urban population had higher rates of unemployment, drug use disorders, and history of abuse, whereas the rural population had higher rates of serious medical problems and other mental health issues.
It is also important to acknowledge the impact of a culturally informed mental health diagnosis. A majority of health/mental health care providers utilize the Diagnostic and Statistical Manual (DSM) for the assessment and classification of mental illness. Additionally, many insurance companies require a DSM diagnosis code for the purposes of billing. However, the DSM is considered culture bound (notably Euro-American). Current diagnosis and assessment guidelines may not be culturally compatible with the American Indian conceptualization of mental (and spiritual) wellbeing [33]. As a very basic example, many American Indian languages do not include words for “depressed” or “anxious” [34].
Understanding this issue is as much a study of history and political science as it is psychology. Historical trauma is an important factor when considering the epidemic of suicide, depression and substance abuse plaguing American Indians. Scholars of this subject have focused on three elements that have been especially important in creating and perpetuating this trauma: colonization, residential education, and forced assimilation. In her 2010 article, McLeigh et al. [19] explores how specific government policies and common practices across history, such as the introduction of European diseases and alcohol, forced migration, boarding schools devaluing native traditions, language, and identity, government bans on native spiritual/religious practices, and massacres of American Indians have all contributed to the increased risk of depression, stress, substance abuse, child maltreatment, and domestic violence that is seen today. Native communities continue to carry a general attitude of distrust toward western culture, including western medicine, and the United States government.
Government Policy: Past, Present, and Moving Forward
Given the practical obstacles as well as the cultural and historical elements mentioned above, the prevalence of mental health issues in American Indian communities is explicable. However, while the historical trauma cannot be easily reversed, there is a great deal more that can be done to restore health, strength and pride within these communities. Historically, the United States government has been exploitative to American Indians, and it is believed that the antecedents of the mental health problems experienced by American Indian today can be traced to social and political injustices. It can therefore be argued that it is the ethical duty of the government to promote and support solutions [19]. Legally, the government has the obligation to provide care and to protect the rights and resources of American Indians people as part of the terms of treaties negotiated in the early 1800’s. However, the Bureau of Indian Affairs (BIA), which is responsible for upholding this obligation, historically has been less than effective. Legislators representing western states with American Indian populations have been charged with usurping American Indian land and resources above protecting the American Indian people [35]. Since the 1800’s, various presidential administrations have fluctuated in their sympathies towards American Indians, but the general trend has been one of less than satisfactory services and care.
Nevertheless, some progress has been made since the original formation of the Bureau of Indian Affairs. Two major pieces of legislation represent the core of American Indian healthcare policy: the Snyder Act and the Indian Health Care Improvement Act (IHCA) [36]. Together, the Snyder Act of 1921 and IHCA of 1976 authorize the appropriation of federal funding for American Indian health care, education, and social services [36,37]. Recently, as part of the Patient Protection and Affordable Care Act, the Obama administration reinstated, amended, and permanently reauthorized the IHCA in 2010 [38]. Currently the federal agency most responsible for the provision of health/behavioral health care to American Indians is the Indian Health Services (IHS), a division of the U.S. Department of Health and Human Services. Like the BIA before it, the IHS has received criticism for not truly providing the highest level of care [35]. The persistently high rates of depression, suicide and mental health issues among American Indians are evidence that the programs currently in place are grossly deficient.
Research Outcomes
Because of the challenges of conducting research in American Indian communities, the number of studies and data is limited. In 2012, two reviews were published summarizing the results of work concerning the treatment of mental health in American Indian populations. Carter et al. [31] highlight the difficulty of evaluating results due to insufficient sample size and they are hesitant to make claims that any of the tested treatments were successful. The Urban Indian Health Institute, a division of the Seattle Indian Health Board, provides a literature review, and the authors identify eight common themes identifying areas in which the current mental health system is failing and provide recommendations for each [33]: “These themes included: 1) focusing on family and community, 2) incorporating traditional knowledge and practices into care, 3) emphasizing active skills building, 4) integrating and linking prevention and treatment care systems, 5) expanding cultural competency of both providers and health care systems as a whole, 6) developing flexible provider-patient relationships with adaptive treatment approaches, 7) implementing environmental and structural changes to affect surrounding conditions, and 8) developing policies and systems, and advocating for adequate funding to improve health care and economic opportunities for AI/AN people”. Some of these themes have been echoed by the work of other scholars who additionally advocate for a culturally relevant and “rights-based approach” [19,31] and emphasize the need for programs and organizations that encourage and support the growth and increased access to health services from within American Indian communities.
Community-based Programs
Several programs, both federally and privately funded, have been formed in response to a call for a more culturally relevant, community, and rights based approach to mental health care for American Indians. Here we provide examples of such organizations.
Health Professions Recruitment Program for Indians (HPRPI)
HPRPI is a program overseen by the department of IHS with the major objective of identifying individuals within the American Indian community with an interest in the health professions and to encourage and assist them in enrolling in professional schools or training programs [39]. This includes helping them complete any postsecondary education required for enrollment and publicizing sources of financial aid available for American Indians enrolled in such healthcare training programs. The IHS offers a wide range of assistance programs to accomplish its objective such as scholarships, an extern program, loan repayment and deferment support, and recruitment activities. For the 2008 fiscal year, the IHS had a total program budget of $47,283,364 [40]. This budget included 337 individual scholarships averaging $47,114 each. Scholarship recipients also receive aid from the Scholar Placement program, which helped find full-time clinical positions within the IHS system for 61% of scholars within 90 days of graduation. A sample survey of 1,500 IHS Scholars revealed an average retention rate of 6.13 years, almost four years above and beyond the required 2.21 years of service. Additionally in 2008, the Extern Program funded a total of 133 health professional pre-graduate and preparatory students providing them with the opportunity to gain clinical experience with IHS and Tribal health professionals in their chosen discipline. They also had the added benefit of working at sites to which they may wish to apply for permanent positions after completing their health professions training.
American Indians Into Medicine (INMED) Grant
INMED is a funding opportunity for educational institutions provided by IHS (as authorized by the IHCIA, 25 U.S.C § 1616g (a)). The mission of INMED is “to augment the number of Indian health professionals serving Indians by encouraging Indians to enter the health professions and removing the multiple barriers to their entrance into the IHS and private practice among Indians” [41]. For the 2010 fiscal year, INMED provided two grants for the amount of $170,000 each.
One of the two grants in 2010 was awarded to the University of New Mexico Center for American Indian Health (CNAH-INMED). The CNAH-INMED describes its program as adopting a “systematic approach to health improvement,” as presented by the Healthy People 2010 “Healthy People in Healthy Communities” model [42]. The objectives of this program include focusing on community outreach to increase exposure at the secondary school level and the recruitment and retention of American Indian students, in part by increasing the number of educational, cultural, and social opportunities for this population on campus, but also to form partnerships with tribal schools with the hope of providing a smooth transition into the health profession programs.
Asniya
Asniya is a non-profit organization founded in 1995 through Harvard Medical School. Its mission is to bring medical knowledge and opportunities to American Indian children and adolescents. Dynamic, animated, and interactive lessons are presented to these students on diverse medical and health topics, providing basic, practical knowledge and increasing medical sophistication” [43]. In addition to its more explicit mission, Asniya maintains the implicit goal of instilling a greater sense of self-worth, confidence, and empowerment within its students through their interaction with the Asniya health profession interns. The student/intern relationship is intended to be one of reciprocal teaching and appreciation, with the hope of promoting positive change and growth both in the American Indian students as well as the Asniya interns.
The John and Sophie Ottens Foundation
The John and Sophie Ottens Foundation was founded with the goal of supporting the education of American Indians from the four-corner states (Arizona, Utah, New Mexico, and Colorado) promoting careers as healthcare professionals, teachers, and social workers [44]. The Arizonabased non-profit organization provides financial support to individuals through grants and scholarships and to universities by providing funding for programming. Some examples of projects supported by the Ottens Foundation are The Four Directions Summer Research Program (FDSRP), the John and Sophie Ottens Foundation American Indian Student Research Awards at Northern Arizona University and the Colorado State University’s American Indian Cultural Center (NACC).
The FDSRP is a research opportunity at Harvard Medical School and Brigham and Women’s Hospital that was founded by American Indian students attending Harvard Medical School with the mission of preparing undergraduates to be leaders in future careers as health care providers [44]. Since its inaugural year in 1994, the FDSRP has given 150 students representing 75 American Indian tribes the opportunity to shadow doctors, conduct research, and network with an array of health care professionals at Harvard Medical School. Alumni of the FDSRP have gone onto careers in research, medicine, public health and policy.
The John and Sophie Ottens Foundation American Indian Student Research Awards provide a students with a wide range of research opportunities, a chance to work one-on-one with a Northern Arizona University (NAU) faculty mentor, and provides the students with up to $8,000 to assist with college expenses [45]. This scholarship helps NAU toward its goal recruiting and retaining American Indian students and providing them with quality fellowship and research opportunities, all in an effort to make NAU “the nation’s leading university serving American Indians”. For the 2011-2012 academic years, the NACC at Colorado State University received a $58,000 donation from the Ottens Foundation to help fulfill its mission “to ensure a successful educational experience for students by providing support and services related to recruitment, retention, graduation, and community outreach. The office embraces and encourages a supportive environment based on the traditions and cultures of American Indian peoples” [46]. Since 2007, NACC has received more than $100,000 from the Ottens Foundation, which the NACC has used to help cover the costs of the tutoring and mentoring provided by the center, the All Nations Leadership Retreat (designed to enhance cultural awareness and personal development) and the K-12 STEM outreach program (involving student and faculty volunteers promoting science education at several local reservation schools), and to help maintain core facilities such as the center’s computer lab and library.
Conclusion
While American Indian culture is extraordinarily rich, the history has been tragic, and the abundance of mental health issues is a reflection of this devastating past. Despite ongoing efforts of interventions, legislation and community based good will, the rates of mental health illness and suicide within American Indian communities has escalated to emergency status. Organizations such as INMED, Asniya and the Ottens Foundation that foster mentoring and support American Indian entrance into the health care arena are positive steps towards fostering culturally sensitive care that may be embraced in these communities. However, as we move forward, there will be a continuing need for outcomes studies validating the effectiveness of programs cited above, to determine whether the services they provide will improve metrics such as numbers of American Indians enrolling and completing degrees in the health professions, numbers of practicing native clinicians in communities, attitudes and views of the health care system and its practitioners, numbers of American Indians utilizing health services, and perhaps most important, whether the methods of treatment are reducing rates of depression, suicide, and other mental illness among American Indians. Future efforts should consider the reasons other health outreach initiatives have failed and avoid repeating those mistakes. Another step toward the ultimate goal of providing better care is educating the mental and public health provider community on the severity of the situation and provide culturally competent community based continuing education and training.. With increased knowledge, mindfulness, and compassion, the attitude and actions of health care professionals, even if distant from any native community, can influence concerted movement towards improved health care and will ultimately contribute to reversing the attrition.


