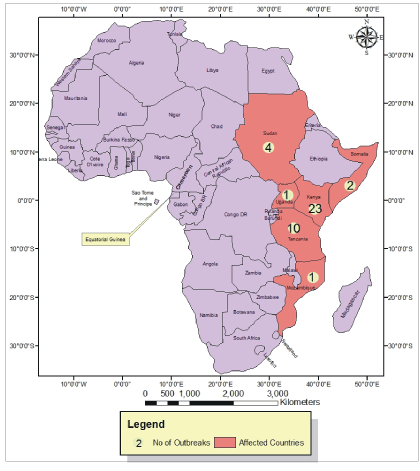
Figure 1: Map of African indicating frequencies of major RVF outbreaks in eastern African countries over the past century (1912- 2010). Numbers of outbreaks in specific countries are indicated in the yellow spheres.


Marycelin Mandu Baba1* Mayomi Ikusemoran2
1Department of Medical Laboratory Science, College of Medical Sciences, Nigeria*Corresponding author: Marycelin Mandu Baba, Department of Medical Laboratory Science, College of Medical Sciences,University of Maiduguri, P.M.B. 1069, Maiduguri, Borno State, Nigeria, Tel: +2348023812573; E-mail: marycelinb@yahoo.com
Objectives: Rift Valley Fever virus (RVFV) is capable of spreading from endemic environments to vulnerable ecologies. The threats RVFV poses to the global public health and food security informed the proposed framework for outbreak prevention.
Method: We reviewed all published, peer-reviewed literature, country reports, and relevant library database for information.
Results: RVF epizootics/epidemics have occurred in Kenya (1910-2007), Tanzania (1930-2007), Sudan (1973-2010) and Somalia (1997- 2007) with varied frequencies and magnitudes. The undeniable role of ecology in the species diversity and distribution of RVFV vectors and the selection pressure it exerts on primary or secondary vectors during outbreaks at a given locality and time is highlighted. In spite of prediction lead period of 2-6 months for the 2006-2008 outbreaks, RVF induced human deaths were estimated at 230, 158, 144 and 51 in Sudan, Kenya, Tanzania and Somali respectively. The morbidity and mortality of livestock did not only disrupt the livelihoods, markets, and the meat industry of the people but also induced ban on livestock slaughter locally as well as International trade bans on the exportation of live animals from the Horn of Africa. Thus the coordinated inter- and intra-sectoral outbreak responses and disease mitigation strategies engaged to contain theses outbreaks had integral noticeable challenges.
Conclusion: Appropriate and timely implementation of the proposed phase disease mitigation strategies would enforce the judicious use of scarce resources, ensure food security and drive behavioral change and promote appropriate vector control.
Rift Valley Fever; Outbreak; Ecology; Vectors; Eastern Africa
Rift Valley fever (RVF) is a mosquito-borne viral and zoonotic disease caused by RVF virus (RVFV), a member of the genus Phlebovirus, family Bunyaviridae. The name ‘Rift Valley fever virus’ was derived from the Great Rift Valley of Kenya, where it was first reported and characterized in 1912 [1] but first described in 1930 [2]. In the 1900s, the understanding of the RVF epizootics in terms of its epidemiology, diagnostic capability, treatment of the disease, genetic evolution of the virus was limited and outbreak investigations and containment was grossly inadequate. Thus, RVF then was grossly underreported, underestimated, misidentified and mismanaged. These challenges paved ways for many subsequent episodes of RVF epizootic/epidemics which occurred in 4-15 year cycles in association with flooding above normal rainfall in eastern African countries [3]. In animals, RVF induces congenital abnormalities [4], abortion and neonatal mortality in animals [5]. In human, RVF can present as an uncomplicated acute febrile illness as well as other complications such as hemorrhagic disease, meningoencephalitis, renal failure, and blindness [6-8]. The ability of RVFV to induce vertical transmission from infected pregnant women reflects its potential for still birth and/or congenital abnormalities in the unborn fetus [9,10].
RVFV can spread from endemic environments to vulnerable ecologies [5,11] posing serious threats to the global public health and food security especially in Sub-Saharan African with low resilience to economic and environmental challenges. Although diagnostics, surveillance, and availability of effective animal vaccine have significantly improved in recent times, the persistence of RVF outbreaks in eastern African countries has raised serious concern. Additionally, the classification of RVFV as a potential bio-/agro-terrorism agent [12,13], its enormous socio-economic impacts and public health importance require more collaborative and multidisciplinary approach to prevent its reoccurrence and /or reduce its socio-economic impact if it recurs. This review highlights the public health importance of RVF, the trend of RVF outbreaks occurrence in eastern African countries from 1910-2016 and the role of ecology on the selection pressure for primary and secondary vectors of RVFV. We also examined the limitations in the investigations and responses to these outbreaks in eastern Africa between 1910 and 2010. Additionally, we present the enormous socio-economic impact of RFV on both animal and human health and we propose an adjusted framework for mitigation against future RVF outbreaks.
All published, peer-reviewed literature, published country reports, and the World Health Organization (WHO) library database were reviewed using the search terms ‘RVF outbreaks’, ‘RVFV and ecology’, ‘vectors of RVF’, vectors of RVF and ecology’, ‘epidemiology of RVF, ‘RVFV and climate’, ‘RVF in East Africa’, ‘Prediction of RVF outbreaks, ‘genetics of RVF and ‘economic estimates of RVF’. We searched for publications available in English as of September 12th 2016 in MEDLINE, EMBASE, Agora and WHO Hinari electronic databases as well as ProMED-mail posts. We also examined abstracts presented at international forums for information on RVF in eastern Africa from 1900s to 2016. More than 200 published English articles were reviewed, assuming that reports in other languages would not change the conclusions of this article.
In 1910, 1912 and 1913, RVF-like disease that was acute and fatal among lambs occurred in a farm at Nakuru district in Rift Valley Fever Province in Kenya [14] Figures 1 and 2. Aside from subsequent sporadic RVF outbreaks, a highly contagious RVF epizootic resulting in prenatal mortalities and abortion in livestock occurred in a farm within the Rift Valley Fever Province (Kenya) in 1930 during which the disease was described for the first time [2]. The extension of the disease to the laboratory workers who investigated the outbreaks [14] revealed the zoonotic nature of the disease. Characteristically, once RVFV is introduced into vulnerable ecologies, it becomes endemic/enzootic, rendering the area risk prone to periodic outbreaks with the potential to spread further into non-endemic ecologies with favorable conditions [5,11] (Figures 2, 3, and 4). For instance, localized RVF outbreaks in 1912-1913 at Nakuru district spread to five other districts in the same Province in 1931 and 1936 [11] (Figure 2). Tanzania witnessed epizootics in 1930 and 1947 [15-17] (Figure 3). The first and second national RVF epizootic hit Kenya in 1951 [18] and 1955 affecting 8 out of sixty-nine (12%) districts including Nakuru where the initial outbreaks occurred in 1910-1913. Only one district affected in that outbreak borders with Nakuru. In 1957, RVF outbreak occurred in Tanzania, none in Kenya but both countries witnessed localized epizootics in 1960. In Kenya, national epizootics occurred bi-monthly between 1961 and 1964 affecting twenty –two out of sixty-nine districts across six provinces. Notably, all the districts that were involved in 1951 and 1955 epizootics were also affected [11]. In 1960 and 1963, Tanzania witnessed other episodes of RVF epizootics [5,16].

Figure 1: Map of African indicating frequencies of major RVF outbreaks in eastern African countries over the past century (1912- 2010). Numbers of outbreaks in specific countries are indicated in the yellow spheres.
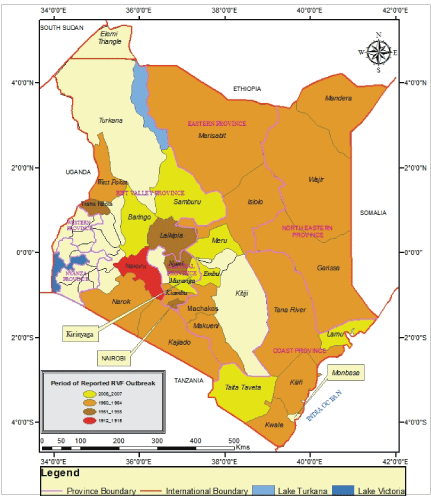
Figure 2: Map of Kenya indicating the Periods and Districts where RVF outbreaks were reported
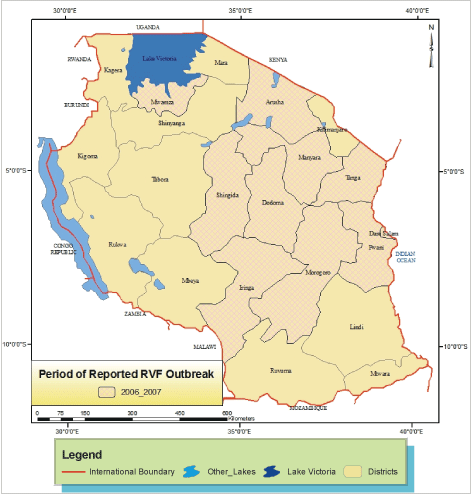
Figure 3: Map of Tanzania indicating the Periods and Districts where RVF outbreaks were reported
Twelve of the previously affected districts in Kenya had RVF epizootics in 1967-1968 [19,20], three in 1970-1971, eleven in 1977-1978, eight in 1981, nine in 1983 and nine in 1989-1991 [11,16]. Between 1973 and 1976, RVF epizootics/ epidemic hit Sudan affecting six districts (Northern Province) [21] (Figure 4) and Northern Tanzania in 1977-1978 [15]. Kenya experienced isolated localized epizootics in 1965 during which two previously affected districts were involved [11,22]. In 1968, both Kenya [11] and Tanzania [5] had RVF epizootics and in 1969 RVF outbreak in Kenya involved two previously affected districts. Between 1985 and 1988 RVF outbreaks reoccurred in Kenya involving two previously affected districts [11].
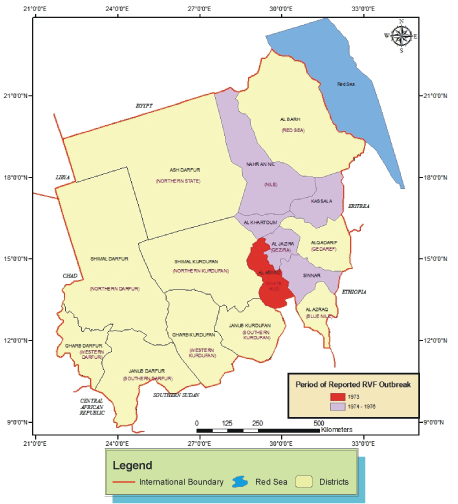
Figure 4: Map of Sudan indicating the Period and Districts where RVF outbreaks were reported
Other national epizootics/epidemic hit 22 of 27 (81%) of the previously affected districts in Kenya, unspecified districts in Tanzania and Somalia resulting in high rates of spontaneous abortions and 70% mortality in livestock in 1997-1998 [11,23,24]. Two localized epizootic reoccurred in Kenya, each affecting one of the previously affected district in 1999 and 2000 [11]. In 2006-2007 the most extensive national epizootics/ epidemics occurred simultaneously again in Kenya, Somalia, and Tanzania [25,16,17]. In Kenya, 33 of 69 districts were affected but 15 of the 33 districts experienced RVF activity for the first time [11,24,2]. Notably, nine of the previously affected district in Kenya reported no RVF case during the 2006-2007 outbreaks. In Somalia and Tanzania, five and ten regions respectively were affected [16]. Eight States in Sudan witnessed yet another intensive national epizootic/epidemic in 2007- 2008 [9,24,26,27]. Contrary to 2007-2008 RVF outbreaks, no detail was reported on the localized epizootic/epidemic that reoccurred in Sudan in 2010 [28]. Surprisingly, RVF epizootic/epidemic suddenly hit Kabale district, 350 kilometers west of the capital, Kampala, Uganda, in March 2016 involving 11 suspected cases (two confirmed and for deaths).The detailed information on that outbreak was not reported at the time of this review[29,30].
Majorly, climate determines the geographic and temporal distribution of the arthropod vector; characteristics of arthropod life cycles; dispersal patterns of associated arboviruses; the evolution of arboviruses; and the efficiency with which they are transmitted from arthropods to vertebrate hosts [31]. The impact of rainfall on the presence, absence, size and persistence of breeding sites for disease vectors depends upon local evaporation rates, soil type, the slope of the terrain and the proximity of large bodies of water (e.g. rivers, lakes, ponds) while the wind has a significant effect upon vector distribution [32]. Increased temperature accelerates the metabolic rate increases biting rates and frequency of blood feeding leading to enhanced egg production as well as increase in population size of vectors. However, the extremely high temperature is positively detrimental to disease vectors [32]. Consequently, the temperature may also affect the geographical range or distribution of vectors since this tends to be determined by the minimum and maximum temperature as well as humidity. High relative humidity favors most metabolic processes in vectors for their prolong survival while low humidity tends to decrease their daily survival rate due to dehydration. In some cases, it may also cause an increase in the blood feeding rate, in an attempt to compensate for the high levels of water loss due to dehydration. It is postulated that global climate change and extreme weather events will create the necessary conditions for RVF to expand its geographical range northward and cross the Mediterranean and Arabian seas [33]. We speculate that climate change may select for adaptive changes in RVFV in the new environment that may also influence its host range, virulence, pathogenicity, and/or transmission efficacy. For instance, the emergence of RVF in regions in Egypt (1977) [34] and Arabian Peninsula [35] (reported to have been imported from East Africa), tended to be associated with greater virulence in humans than what had been historically observed in East Africa [36]. Conversely, the association of RVF outbreaks with El Niño/Southern Oscillation (ENSO) related climate anomalies through a combination of satellite measurements of elevated sea-surface temperatures (SSTs) and subsequent elevated rainfall and satellite-derived normalized difference vegetation index (NDVI) data aided successful prediction of 2006-2007 RVF outbreaks in the Horn of Africa [37]. That prediction algorithm provided a lead period of 2-6 months of warning to allow adequate outbreak response activities and disease mitigation implementation [37].
Unlike the majority of arboviruses that adapt to a narrow range of vectors, RVFV infects a wide range of vectors such as mosquitoes (Aedes, Culex and Anopheles), flies and ticks [38]. Interestingly different species of vectors play different roles in sustaining the transmission of the RVFV [39] in an environment. Repeated intersect between competent vector and vertebrate host populations drive arboviral amplification rapidly to epidemic levels within a permissive environment [40]. The cause and magnitude of arboviral disease outbreaks are largely determined by a complex of factors and interaction between these factors [41]. These factors extend beyond the biology and ecology of the vector and virus to include the immunity and resilience of the host, standard of sanitation, quality of housing, poverty, accessibility, and quality of health care, movement of people and animals, level of education and awareness of the disease [41,42]. Disease vectors have particular environmental requirements in respect to temperature, rainfall and precipitation [24]. RVFV has a large number of potentially competent mosquito vectors which include Aedes species Culex species, Mansonia species Anopheles species [43-47]. Whilst Aedes species are considered as the reservoir vector, Culex [42], Mansonia, Anopheles was incriminated as the amplifying vectors during previous RVF outbreaks [37]. RVFV may influence the behavior of vectors in such a way that enhances transmission rates [42], but not necessarily the selection of primary or secondary vectors during outbreaks. For instance, during the 1997-98 and 2006/07 RVF outbreaks, different vectors served as primary and secondary vectors at Garissa, Kenya (an epicenter in 1997-98 and 2006/2007 Rift Valley fever epidemics/epizootics). Anopheles coustani, Mansonia (Mn) Africana (Theobald), and Mansonia uniformis (Theobald) were implicated as the primary vectors in the 1997-98 while Aedes (Neomelaniconion) mcintoshi (Theobald), Aedes Ochraceus and Aedes Sudanensis served as primary vectors during the 2006/2007 [4]. Notably, Garissa is a semi -arid zone well-endowed with numerous and well-defined dambo (depression of the soil surface), sluggish streams and rice fields [38,44]. Interestingly, Mansonia uniformis and Mansonia Africana which prefer the swampy, folded areas or water bodies containing emergent vegetation for breeding served as the primary vectors of RVFV in Baringo during 2006-07 RVF outbreaks [44]. Culex pipiens were incriminated as the primary and secondary vectors during RVF outbreaks in Egypt (1977) and Kenya (2006-2007) [44] respectively. This implies that Garissa and Baringo and Egypt with different ecosystems have different vectors that were incriminated with Rift Valley fever epizootics/epidemics as primary or secondary.
Analysis of mosquito host choices has revealed that attraction and engorgement rates of flood water Aedes were at least three-fold higher for cattle than goat or sheep [49-52]. Similarly, the attraction of most Culex spp. to cow was higher than either sheep or goat but the engorgement rate was comparatively lower because of its preferential feeding on birds than mammals [53,54]. It is not yet clear whether the major determinants of primary or secondary vectors of RVFV at different vulnerable ecologies are environmental factors (vegetation, climate rainfall) or composition, abundance and availability of different vertebrate hosts or unknown factors. Overall, the ecosystem significantly plays an undeniable role in the distribution, and species diversity of disease vectors. We speculate that ecology exerts selection pressure on the primary or secondary vectors of RVFV outbreaks at a given locality and time.
RVF induced impact aggravated previous economically impoverished countries in Sub-Sahara Africa. The number of human deaths due to RVF rose from 1 (1912-1988) to 1068 (1998-2016) (Table 1). The impact of these deaths on the families, communities, country and the region was unquantifiable. RVF outbreaks did not only devastate animal producers but other service providers within the livestock supply chain and other parts of the larger economy. Where human RVF victims survived, neurological and visual complications which are likely to be lifelong, attracted considerable economic impact due to a loss in disability-adjusted life years estimated to fall between 353-11,958 and 188-6,530 for 2005 [55]. The morbidity and mortality of livestock bruised the pride, prestige and self-importance of livestock owners [56] and induced ban on livestock slaughter locally [57] threatening the livelihoods of those who depended on livestock products and related activities for labor opportunities [58]. Imposition of International trade bans on the exportation of live animals from the Horn of Africa for three years devastated economic impacts especially the rural communities. In Tanzania, trade ban led to an economic loss estimated at the cost of US$ 352,750 excluding the incomes of rural livestock producers, animal handlers, city animal fees, inspectors’ fees. Consequently, funds (US$3.84 million) for basic amenities like education, health, food, and shelter [59-61] was mobilized to contain the outbreaks [43]. Such fund was quite substantial for a low and impoverished countries [61, 62].
| Outbreaks | Year of occurrence | Country | State/Provinc/ County | Type of diagnostic test used | Estimated no of cases in human | No. of confirmed cases in human ( Deaths) | Source of information |
| RVFl (Epizootic) |
1912-1915 | Kenya | Nakuru | Unknown | Unknown | none | [11] |
| RVF n | 1930 | Kenya, Marura, Ndabibi, Ol Magogo, and Njoro | Nakuru, Naivasha, | Virus isolation | None | None | [2] |
| RVF n | 1936 | Kenya, Marura, Ndabibi, Ol Magogo, and Njoro | Nakuru, Naivasha, | Virus isolation | None | None | [11] |
| RVF n | 1951 | Kenya | Nakuru, Trans Nzoia, Uasin Gishu and Laikipia districts in Rift Valley province, Thika, Nyeri and Maragwa districts in Central province, and Nairobi Metropolitan district in Nairobi province |
unknown | None | None | [3,18] |
| RVF n | 1955 | Kenya | Nakuru, Trans Nzoia, Uasin Gishu and Laikipia districts in Rift Valley province, Thika, Nyeri and Maragwa districts in Central province, and Nairobi Metropolitan district in Nairobi province |
Unknown | None | None | [11] |
| RVFl (Epizootic) |
1960 | Kenya | Nakuru | Unknown | None | None | [11] |
| RVF n | 1961 | Kenya | Districts listed above and Narok, Kajiado, and West Pokot districts in Rift Valley province; Garissa, Wajir, and Mandera districts in Northeastern province; Isiolo, Marsabit, Machakos, and Makueni districts in Eastern province ; Kwale, Kilifi, and Tana River districts in Coast province; and Kiambu district in Central province. |
unknown | None | None | [11] |
| RVF n | 1964 | Kenya | province; and Kiambu district in Central province | unknown | None | None | [11] |
| RVFl (Epizootic) |
1965 | Kenya | 2 of the previously affected districts (not specified) |
unknown | None | None | [11] |
| RVFl (Epizootic) |
1969 | Kenya | 2 of the previously affected districts (not specified) |
unknown | None | None | [11] |
| RVF n | 1967-1968 | Kenya | 12 of the previously affected districts (not specified) |
Virus isolation and serology | None | None | [11, 19, 20] |
| RVF n | 1970-1971 | Kenya | 3 of the previously affected districts (not specified) |
unknown | None | None | [11] |
| RVF n | 1977-1978 | Kenya | 11 of the above districts (not specified) |
unknown | None | None | [11] |
| RVF n | 1981 | Kenya | 8 of the previously affected districts (not specified) |
Unknown | None | None | [11] |
| RVF n | 1983 | Kenya | 9 of the previously affected districts (not specified) |
Unknown | None | None | [11] |
| RVFl (Epizootic) |
1985-1986 | Kenya | 1 of the previously affected districts (not specified) |
Unknown | None | None | [11] |
| RVFl (Epizootic) |
1987-1988 | Kenya | 1 of the previously affected districts (not specified) |
Unknown | None | None | [11] |
| RVF n | 1989-91 | Kenya | 9 of the previously affected districts (not specified) |
Virus isolation and serology | None | None | [19,20] |
| RVF n | 1997-98 | Kenya, | 22 of the 27 previously affected districts (not specified) Somalia and Tanzania | Virus isolation, RT-PCR and serology |
89,000 | 0(478) | [23,24] |
| RVFl (Epizootic) |
1999 | Kenya | 1 of the previously affected districts (not specified) |
Unknown | None | None | [11] |
| RVFl (Epizootic /epidemic) |
2002 | Kenya | 1 of the previously affected districts (not specified) |
Unknown | None | None | [11] |
|
RVF n (epidemics) |
2006-2007 | Kenya | All the previously affected districts except 9 and new 15 districts : Baringo, Samburu, Kirinyaga, Murang’a, Taita- Taveta, Lamu, Malindi, Kitui, Meru South, Meru Mbeere Central, Meru North, Mwingi, Moyale, Embu, and |
Virus isolation, RT-PCR and Serology |
75,000 |
700 (158), CFR = 22.6% |
[11,17,24] |
| RVF | 2008 | Mozambique | Alaotra Mangoro, Analamanga, Itasy, Vakinakaratra and Anosy Regions. | unknown | unknown | 412 (17), CFR=4.1% | http://www. mdtravelhealth. com/ destinations/ africa/ mozambique. php |
| RVF (epidemics) |
2006-2007 | Somalia | Lower Juba Gedo Hiran, Middle Juba, Middle Shabelle, Lower Shabelle regions. | unknown | 30,000 | 114(51), CFR=45% | [17,24] |
| RVF (epidemics) |
1973 | Sudan | Nile, Khartoum, Kassala, El Gezira, Sennar, and White Nile) | Virus isolation | Unknown | Unknown | [21] |
|
RVF (Epizootics/ epidemics) |
2007-2008 | Sudan | White Nile, Sennar, El-Gazira, Sennar (near White Nile and Blue Nile Rivers) River Nile, Khartounm and Kassala States |
Serology | 75,000 | 747(230), CRF=30.8% | [24] |
| RVF (epizootics/ epidemics) |
2010 | Sudan | El Gezira | unknown | unknown | 100 (unknown) | [28] |
| RVF | 1930,1947,1957, 1960, 1963, 1968 |
Tanzania | Unknown | Unknown | Unknown | None | [16] |
In Kenya, the estimated RVF-induced losses were over US$32 million [63]. In Garissa and Ijara districts, losses due to livestock mortality were over US $9.3 million [51] and loss due to reduction in milk production at Garissa was valued at US $77,000. Idling of the Garissa and Mwingi slaughterhouses resulted in losses estimated at US $2,917 and US $812 per month, respectively while each of the two slaughterhouses in Nairobi lost between US $17,000-US $22,000 in direct revenue [57]. Traders, whose livestock trading typically represents about 60-80% of their income, were forced to rely on their past savings in a way that crippled the financial capital to resume trading activities even after the outbreak [57].
RVF has no cure but it can be prevented effectively through the use of appropriate and timely administered vaccine to livestock [61,64]. The identified risk epidemiological factors associated with the past RVF outbreaks in eastern Africa ranged from ecological, human practices to genetic evolution of the virus [36]. Whilst diverse ecological factors influenced RVF outbreak frequency, the virus evolution has greatly impacted on its virulence in the hosts [36]. RVFV infect human through direct contact with or handling tissue, tissue fluids and mucous membranes of infected animals or animal products as well as with infectious fomites, small droplets and mosquito bites. Additionally, RVFV infects humans by either inoculation (parenteral route) through a wound from contaminated surgical instruments or contact with broken skin or inhalation of aerosols produced during the slaughter or birthing of infected animals [9]. Currently, Human RVF is managed using supportive therapy [65]. Despite the prediction lead period of 2-6 months for the 2006-2008 outbreaks [37], RVF induced human deaths were estimated at 230, 158, 144 and 51 in Sudan, Kenya, Tanzania and Somali respectively [16,23,56].This implies that the coordinated inter- and intra-sectoral outbreak response and disease mitigation strategies to curb the outbreaks had integral noticeable challenges which include lack of contingency plans [2], late diagnosis, lack of community awareness, weak surveillance in livestock and humans [63], traditional practices and reluctance to travel long distances for medical attention. Additionally, the rapidly changing epidemiology of RVF was not recognized [66] and gaps existed in the suspicion index for healthcare practitioners in respect to clinical symptoms that are not classically associated with the disease. The benefit of RVF prediction lies on maximizing the use of the lead periods to prevent its occurrence. We speculate that with the lead period of 2-6 months, future RVF can be prevented if the proposed appropriate and timely disease prevention and mitigation strategies are properly implemented.
The enormous negative impacts of each RVF outbreak demands new and systematic approaches to prevent or reduce the resultant outcomes if and when it recurs. Our proposed phased approach is based on distinct preparedness and mitigation strategies during inter-epidemic, prediction and outbreak periods. The phased activities consider identified factors that contributed to the occurrence and spread of the disease during past outbreaks.
Activities during the inter-epidemic phase include a well-coordinated multidisciplinary preparedness plans at national and regional levels. Such plans should include assessing the beliefs, attitude and perception of the people on RVF, intensive public awareness campaigns, training of the health workers, assessment of the soil topology/type in each county to identify flood-prone areas [3,67] and the establishment of a systematic and active surveillance system. The use of mobile Phone–based Infectious Disease Surveillance System developed in Sri Lanka may be adopted locally [68]. Supervision of all pastoralists in groups by a Veterinary officer will enhance the capacity of the Veterinary authorities in each country and promote effective communication between them. Enforcing the existing policy on vaccination of animals against RVF in each country and issuance of license for compliant pastoralists will enhance herd immunity against RVF within the community. The establishment of appropriate regulated and well-furnished slaughter facilities in each District/County/Region will facilitate proper ante-mortem and post-mortem meat inspection. The use of mosquito nets, or vector repellent or wearing of protective clothing should be encouraged especially in previously affected areas during the rainy seasons.
The risk prediction period should attract additional activities including differential diagnosis of febrile illnesses for arboviruses in risk-prone areas, reinforcement of Public awareness through mass/print media and disseminating relevant information to relevant village heads, village elders, constituency and district heads to alert them of the pending outbreak and sharing of ideas on how to prevent the outbreak. Also, warning sign posts should be fixed along the major roads leading into the proposed affected areas to alert visitors about the outbreak. Proper and adequate health education campaigns and social mobilization programs may promote behavioral change to reduce disease spread. Individuals and community should be encouraged to avoid mosquito bites through the use of impregnated mosquito nets, livestock dipping with insecticides or insect repellent. The smoke from burning the leaf headspace of Corymbia citriodora, Ocimum suave and Ostostegia Integrifolia [69] can repel mosquitoes and could be explored in households of affected areas. The adequate use of Personal protective equipment (PPE) in health care settings will avoid possible nosocomial transmissions. Strengthening Inter and intra collaboration between relevant ministries will synergize to contain the spread of the disease in the affected areas and neighboring areas. Mobility of animals/humans to and fro risk prone areas should be regulated, sick animals and human’s quarantined, single needle/ syringes for more than one animal should be avoided during vaccination and abattoir regulations should be re-enforced. A refresher training workshop for health workers from the affected areas and its environs will refresh and update their knowledge and skill on a well-defined case definition for suspected cases, diagnostic capability and disease reporting mechanisms.
Activities during the epidemic phase may include re-enforcing the existing intra and inter sectoral outbreak response mechanism, intensifying the dissemination of health promotion and disease prevention information, using a sensitive and definite case definition to train health workers and during public awareness campaigns. Visiting the affected households and interviewing the victims of the disease may aid identification of epidemiological factors associated with the outbreak for a more cost effective prevention/control [70,71] and referrals to the nearest local health care facilities may be necessary for proper management [71] and further testing. Case-finding efforts should be enhanced by retrospectively reviewing hospital/laboratory/clinic records in government and private hospitals/clinics [70,72]. The local health facility in the affected districts and its environs should be capable of recognizing and diagnosis the disease accurately. Animals in the affected areas should not be vaccinated except those areas surrounding the affected communities and movement of animals and humans to and fro affected areas should be properly regulated to avoid disease spread.
RVF outbreaks have persistently occurred in a cyclical pattern in eastern African countries resulting in significant adverse socio economic impact on health and food security since its discovery in 1912. Vulnerable ecologies are not only risk prone for periodic outbreaks but serve as index foci for future outbreaks in non-endemic environments. Ecology probably exerts selection pressure on the primary and secondary vectors of RVF during outbreaks at a given locality and time. With the prediction lead period of 2-6 months for the 2006-2008 outbreaks, RVF induced human deaths were estimated at 230, 158, 144 and 51 in Sudan, Kenya, Tanzania and Somali respectively. Thus, the integral noticeable challenges in the existing inter- and intra-sectoral outbreak response and disease mitigation strategies demand more stringent, collaborative and effective measures to mitigate future RVF impacts. Considering the identified risk epidemiological factors as well as challenges experienced during the past RVF outbreaks, phased disease mitigation, and outbreak prevention strategies are proposed.
This work was supported by the Institute of International Education for Scholar Rescue Fund (IIE-SRF), the German Academic Exchange Service (DAAD) for granting Marycelin Baba Postdoctoral Fellowship and International Institute for Insect Physiology and Ecology (icipe) for hosting the Fellowship programs. We wish to extend our sincere appreciation to Drs Daniel Masiga and Jandouwe Villinger for their enormous Technical and moral support. Additionally, the technical support of David Makori is highly appreciated.
The authors declare no conflicts of interest.
Download Provisional PDF Here
Article Type: Research Article
Citation: Baba MM, Ikusemoran M (2017) Proposed Systematic Approach to Prevent or Reduce the Resultant Outcomes of RVF Outbreaks: Using the Eastern African Countries Experience Tract. J Epidemiol Public Health Rev 2(2): doi http://dx.doi.org/10.16966/2471-8211.135
Copyright: © 2017 Baba MM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access