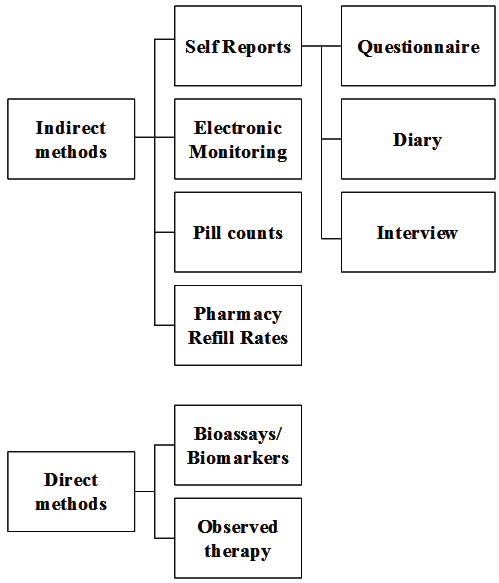
Figure 1: Categorization of the methods for adherence quantification.


Konstantina Tsianou1 Nikolaos Giannakeas2 Markos G Tsipouras2 Alexandros T Tzallas2* Alexandros Skamnelos3 Dimitrios K Christodoulou3 Jan Bureš4 Jiri Vlcek1 Epameinondas V Tsianos3,5
1Department of Social and Clinical Pharmacy, Faculty of Pharmacy, Charles University in Prague, Hradec Kralove, Czech Republic*Corresponding author: Alexandros T Tzallas, Department of Computer Engineering, Faculty of Technological Applications, Technological Educational Institute of Epirus, GR47100 Arta, Greece, Tel: 306932643071; E-mail: tzallas@teiep.gr
Aim: This work presents an extensive comparative study for the use of the Belief about Medicine Questionnaire (BMQ), in order to assess the beliefs of patients into their prescribed medication. The multifactorial nature of patient medication adherence as well as, several compliance improvement strategies are initially examined. According to literature review, most commonly used method for measuring the positions of patients for their drug therapy employs self-organized questionnaires. The current review focuses on studies where BMQ is employed, in several chronic conditions, investigating the beliefs of patients about the necessity of drugs and concerns about their use. The current study aims to examine medical fields that BMQ could be useful for the prediction and avoidance of non-compliance effects, which affect the quality of life of the patient.
Methods: Patient medication beliefs play a significant role in chronic diseases, where long time medication is required. A variety of studies have been presented in the literature, either focusing on specific chronic conditions or investigating generally the assessment of patient medication beliefs in mixed datasets. Most of the studies, present statistical analysis in questionnaire results, regarding the validity of BMQ itself or the performance of socioclinical findings about patients’ beliefs. Statistical results from several works are extensively presented and discussed, regarding BMQ validity, as well as factors such as the chronic condition, the patient age, the prescribed number of drugs per day etc.
Conclusions: BMQ has been extensively employed to measure the beliefs about medicine in several chronic conditions and has been reported to correlate with objective medication adherence assessment. However, beliefs among different patient populations can significantly vary.
Patient medication beliefs; Drug compliance; Belief about Medicine Questionnaire
The significant role of the patients’ adherence to their prescribed medication is extensively investigated in several research studies, regarding the lack of diseases control and the quality of life (QoL) of patients. In terms of healthcare, medication adherence represents the extent that patients follow the advice of healthcare professionals regarding their medication and disease management [1]. Typically, about 50% of patients present low adherence to the prescribed medication treatment [2,3]. The main aim of the studies is the effect of the non-compliance of patients that follow a specific drug medication for their diseases.
The quantification of patient medication adherence can be performed either directly or indirectly (Figure 1). There are two direct methods to measure the compliance of the patients to their medication [4]:

Figure 1: Categorization of the methods for adherence quantification.
Apart from direct methods, four different indirect methods have been proposed and investigation in the literature:
The multifactorial nature of medication adherence in chronic disease patients, could explain a variety of reasons that patients fail to adhere to their maintenance medication [5]. Medication adherence can be influenced by disease (chronic, asymptomatic, requiring different strategies to reach the goal); medicine cost, information about their harm (syndrome of leaflet), dosage scheme and rearing skills with administration; strategy of treatment (polypharmacotherapy, treatment of acute and chronic phase), experience and skills of individuals (motor activity, good vision, understanding of process of minimization of risk, cognitive aspects, etc.); patient-physician (or another health care worker focusing on pharmacotherapy) relationship and understanding each other. The main factors that affect patient compliance include:
Especially in chronic diseases, the consequences of non-compliance to the prescribed medication could cause lack of disease control and affect the QoL of patients. Most of remission cases present clinical recurrence after several months, due to non-adherence of patient to the maintenance medication [6].
Several strategies have been proposed to improve the patient medication adherence. In practice, common approaches attempt to improve the dose regimen using reminders, specific pill-boxes or simplifying the dosing. However, these approaches address the cases where low adherence is due to involuntary medication dose skipping and do not address drug disallowance due to other factors (e.g. low opinion about medication). Thus, most of research studies for medication adherence improvement focus on the education of the patient for understanding:
Better understating and knowledge about the above factors improves the beliefs of the patient regarding his medication and thus affects the drug compliance. Even demonstration tools, which illustrate photographic documentation about the disease, could be beneficial [7]. In this direction Elkjaer et al. [8-10] developed a web-based educational tool, where patients improve their ability to self-initiate treatment and increase the level of disease-specific knowledge. Also, Nigro et al. [11] investigated the correlation between non-adherence and psychiatric disorders, proposing preventive psychiatric interventions.
Apart from the important role of the compliance to the patient health, increasing the medication adherence could be beneficial for the costs of health providers. Luga AO et al. [12] presented recent developments in the investigation of compliance, emphasizing to the impact of medication adherence or non-adherence on healthcare costs, in the US health system. The study denotes the magnitude of the non-adherence problem and related costs, with an extensive discussion of the underlying mechanisms of non-adherence impact on costs. Employing the Medication Possession Ratio (MPR) and the Proportion of Days Covered (PDC) metrics, the authors estimate the impact of non-adherence on health care costs in several chronic diseases, such as diabetes and asthma. MPR is calculated as the total number of days supplied, divided by the number of days between the first and last refills; while PDC is calculated as the total number of days supplied during an interval, divided by the total number of days during that interval.
Employing self-administered questionnaires for the clarification of several factors about the disease process, beliefs and preferences of the patients or their QoL, is a common practice for physicians. Statistical findings highlight a number of physical aspects for the treatment progress regarding personal beliefs, concerns or lifestyle. Quantification of patients’ compliance to their prescribed medication also employs several self-administered questionnaires [13]. Each questionnaire attempts to measure patient medication adherence from a different point of view. The questioners that are more frequently used focus on a specific disease regarding its symptoms, medication, psychological factors, QoL of the patient and the knowledge of the patient about the disease. Below, a summary of the most well-known questionnaires for compliance quantification is presented. There are several general health scales and questionnaires to measure the medication adherence of patient regardless of the disease, as well as there are several questionnaires for specific diseases.
A general health scale, which could be employed for the quantification of patient medication adherence is the Medication Adherence Report Scale (MARS) [14]. MARS is a combination of two other scales, the Drug Attitude Inventory (DAI) [15] and the Medication Adherence Questionnaire (MAQ) [16], consisting of 10 selected items (Table 1). Although, MARS has been employed mainly in the Psychiatric field, the findings of its analysis could be extremely useful to quantify patient compliance.
| MAQ 1 | Do you ever forget to take your medicine? |
| MAQ 2 | Are you careless at times about taking your medicine? |
| MAQ 3 | When you feel better, do you sometimes stop taking your medicine? |
| MAQ 4 | Sometimes if you feel worse when you take your medicine, do you stop taking it? |
| DAI 6 | I take my medication when I am sick |
| DAI 8 | It is unnatural for my mind and body to be controlled by medication |
| DAI 9 | My thoughts are clearer on medication |
| DAI 10 | By staying on medication I can prevent getting sick |
| DAI 2 | I feel weird, like a ‘zombie’, on medication |
| DAI 5 | Medication makes me feel tired and sluggish |
Table 1: Medication Adherence Rating Scale (MARS)
MAQ: Medication Adherence Questionnaire; DAI: Drug Attitude Inventory
Another general scale is the Trust in Physician [17], which focuses on the relation between the patient and the physician. After several versions of the scale a five-point response scale is employed, reducing a large number of items into 11, to exclude any redundant information, and make the questionnaire more comfortable (Table 2). There are three dimensions of trust: a) confidence in physician skills and knowledge b) physician dependability, c) and finally the confidentiality of information given by the physician.
| Item | Score |
| I doubt that my doctor really cares about me as a person. † | 1-5 |
| My doctor is usually considerate of my needs and puts them fi | 1-5 |
| I trust my doctor so much that I always try to follow his/her advice. | 1-5 |
| If my doctor tells me something is so, then it must be true. | 1-5 |
| I sometimes distrust my doctor’s opinion and would like a second one.† | 1-5 |
| I trust my doctor’s judgement about my medical care. | 1-5 |
| I feel my doctor does not do everything he/she should for my medical care.† | 1-5 |
| I trust my doctor to put my medical needs above all other considerations when treating my medical problems. | 1-5 |
| My doctor is a real expert in taking care of medical problems like mine. | 1-5 |
| I trust my doctor to tell me if a mistake was made about my treatment. | 1-5 |
| I sometimes worry that my doctor may not keep the information we discuss totally private | 1-5 |
Table 2: Trust in Physician Scale
Five-point response scale: 1-totally disagree; 2-disagree; 3-neutral; 4-agree; 5-totally agree
†Reverse-scored items
Hospital Anxiety and Depression Scale (HADS) [18] consists of two sets of items, which are related to the anxiety and the depression of the patient (Table 3). Indirectly, HADS could be employed to extract the compliant of patients to their medication.
| Relate to anxiety | Relate to depression |
| I feel tense or wound up (0-3) | I still enjoy the things I used to enjoy (0-3) |
| I get a sort of frightened feeling as if something bad is about to happen (0-3) | I can laugh and see the funny side of things (0-3) |
| Worrying thoughts go through my mind (0-3) | I feel cheerful (0-3) |
| I can sit at ease and feel relaxed (0-3) | I feel as if I am slowed down (0-3) |
| I get a sort of frightened feeling like butterflies in the stomach (0-3) | I have lost interest in my appearance (0-3) |
| I feel restless and have to be on the move (0-3) | I look forward with enjoyment to things (0-3) |
| I get sudden feelings of panic (0-3) | I can enjoy a good book or radio or TV program (0-3) |
Table 3: Hospital Anxiety and Depression Scale (HADS)
The Work Productivity and Activity Impairment Questionnaire (WPAI) was created as a patient-reported assessment of the amount of absenteeism, presenteeism and daily activity impairment attributable to general health (WPAI:GH). Since sometimes it is more effective to employ disease-specific questionnaires, WPAI has been modified for specific health problems (WPAI:SHP) [19]. The WPAI:GH and the WPAI:SHP were created simultaneously and are based on the same template, but in the GH version the subject is instructed to respond with reference to general health status while in the SHP version, the subject responds with reference to a specified health problem, disease or condition.
Apart from general scales, questionnaires for specific field have also been presented in the literature. For example, several specific field questionnaires refer to Inflammatory Bowel Diseases (IBD). Such self-organized questionnaire is the Crohn Colitis Knowledge Score (CCKNOW) presented by Eaden et al. [13], the Short Inflammatory Bowel Disease Questionnaire [20] (Short - IBDQ), and the simplified clinical colitis activity index (SCCAI) [21].
Beliefs about Medicine Questionnaire (BMQ) [22], in one of the most commonly used self-organized scale to assess the beliefs of chronic patients in their prescribed medication. The main innovation of BMQ is the direct quantification of the beliefs of patients about the drugs and their use, which is a significant factor that affects the compliance of the patients to their prescribed medication.
The aim of BMQ [22] is the assessment of the broad range of beliefs about specific and general medication. Thus, the questionnaire is divided into two scales, with each of them being divided into two subscales (Table 4). First scale concerns the belief of patients about their prescribed medication, while in the second one patients are inquired for their opinion generally about medicines and their use. More specifically the two scales of BMQ are:
| BMQ-Specific | The BMQ-General |
| Without my medicines I would be very ill (1-5) | Medicines do more harm than good (1-5) |
| My life would be impossible without my medicines (1-5) | All medicines are poisons (1-5) |
| My health, at present, depends on my medicines (1-5) | Most medicines are addictive (1-5) |
| My health in the future will depend on my medicines (1-5) | People who take medicines should stop their treatment for a while every now and again (1-5) |
| My medicines protect me from becoming worse (1-5) | Natural remedies are safer than medicines (1-5) |
| I sometimes worry about becoming too dependent on my medicines (1-5) | Doctors use too many medicines (1-5) |
| My medicines disrupt my life (1-5) | If doctors had more time with patients they would prescribe fewer medicines (1-5) |
| My medicines are a mystery to me (1-5) | Doctors place too much trust on medicines (1-5) |
| Having to take medicines worries me (1-5) | |
| I sometimes worry about long-term effects of my medicines (1-5) | |
| These medicines give me unpleasant side effects (1-5) |
Table 4: Belief about Medicine Questionnaire (BMQ)
BMQ is a self-administer questionnaire, which focuses directly to the beliefs and concerns of the patients about the use and efficacy of medicines. It can be used to a wide range of diseases, where prescribed medication is required. Several studies have been already presented in the literature that uses BMQ for the patients’ medication beliefs assessment. Most of these studies employ mixed datasets, in terms of the diseases. Initial studies by Horne et al. [22,23] use data from several chronic diseases, such as asthma, diabetes and psychiatric conditions from hospital clinics, and cardiac, general medical and renal (haemodialysis recipients) from inpatients; these where chosen to reflect a variety of disease and treatment characteristics. Datasets from several chronic diseases have been employed from several research groups [24-30]. Marbdy et al. [31] presented a study with a total unconditional sample, where the participants are selected using only thee inclusion criteria: a) to understand the Swedish language, b) to be over 18 years old, and c) to take a queue number to a specific prescription counter for Swedish pharmacies. As a result, this sample holds none limitation about the disease of the patient.
BMQ in asthma: Apart from the studies which included mixed datasets, several studies were based in homogenous samples. The adherence to the medication for asthma patients has been investigated from different research groups [32-34]. Menckeberg et al. [34] investigated whether beliefs about inhale corticosteroid relate to medication adherence objectively measured by prescription refill records. They concluded that patients’ beliefs about inhaled corticosteroids correlate not only with medication adherence by self-report but also with a more objective measure of medication adherence calculated by pharmacy dispensing records.
BMQ in HIV: Both Horne et al. [35] and Gaucher et al. [36] analyzed the BMQ records for the behavior of HIV patients in highly active antiretroviral therapy (HAART). It is common sense that adherence to medical regimens is extremely important for HIV patients. The results of the above studies revealed that medication adherence and patients’ beliefs about treatment, satisfaction with treatment, confidence in the physician and duration of treatment and illness are significantly correlated. It also revealed that Specific-Necessity and Specific-Concerns factors of BMQ could be useful for understanding patient perspectives of HAART and predict medication adherence.
BMQ in diabetes: Diabetes patient samples are analyzed by Aikens and Piette [37] to reveal patient beliefs about antihyperglycemic and antihypertensive treatment and medication underuse. The authors also examined diabetes in another point of view, such as the patients’ beliefs about their medication necessity and potential harmfulness in an economically distressed community. According to their findings, diabetic patients with low health literacy are concerned about medication harmfulness, which is in turn associated with medication underuse and higher blood pressure. To enhance medication adherence and outcomes, interventions should address patients’ underlying concerns about potential adverse treatment effects and focus on both cultural factors and health literacy. Another study for diabetes chronic condition presented by Fall et al. [38], where the French translation of BMQ is validated.
BMQ in autoimmune diseases: The role of patient medication adherence in therapies for autoimmune diseases is extremely significant, due to the fact that insufficient medication could lead to irreversible disorders. Kumar et al. [39], Treharne et al. [40], Betegnie et al. [41] employed the BMQ to measure the beliefs about medication in patients with rheumatoid arthritis and systemic lupus erythematosus, while Neame and Hammond [42] investigated which factors are related to medication beliefs about rheumatoid arthritis, and whether these beliefs influence medication adherence. All these studies concluded that most people with rheumatoid arthritis have positive beliefs about the necessity of their medication. However, levels of concern are high and associate with helplessness and non-adherence. The Beliefs about Medicines Questionnaire may identify people at risk of poor medication adherence and provide a focus for patients to discuss their beliefs, providing opportunities to improve medication adherence.
BMQ in gastro-oesophageal reflux: Gastro-oesophageal reflux disease (GORD) causes some of the most frequently seen symptoms in both primary and secondary care; between 20% and 30% of a ‘Western’ adult population experience heartburn and/or reflux intermittently [43]. Treatment of GORD includes a range of options, both medical and surgical. The simplest is self-administered antacids with advice to alter lifestyle factors such as dietary modification, smoking cessation and weight reduction. The role of surgery has traditionally been confined to the treatment of those with severe symptoms not responding to medication in appropriate dosage and medically fit for surgery. Grant et al. [35] focus on the effectiveness and cost-effectiveness of minimal access surgery amongst people with gastro-oesophageal reflux disease. Relative clinical effectiveness was assessed by a randomized trial (with parallel non-randomized preference groups) comparing a laparoscopic surgery based policy with a continued medical management policy. The economic evaluation compared the cost-effectiveness of the two management policies in order to identify the most efficient provision of future care and describe the resource impact that various policies for fund application would have on the NHS. For the above purpose a combination of BMQ and Beliefs about Surgery Questionnaire (BSQ) has been employed in 810 patients. Amongst patients requiring long-term medication to control symptoms of GORD, surgical management significantly increases general and reflux specific health-related quality of life measures, at least up to 12 months after surgery.
BMQ after liver transplantation: Medication adherence of patient after liver transplantation is measured by O’Carroll et al. [44]. Liver transplant recipients have diverse histories, ranging from an impulsive paracetamol overdose, to long-term alcoholic cirrhosis, to the autoimmune disorder primary biliary cirrhosis. However, regardless of cause, lifelong adherence to immunosuppressant medication is essential for the survival of each recipient. Non-adherence rates within the transplant population have been reported as ranging from 20 to 50%. Four different questionnaires have been employed in this study, including the BMQ. The results indicated that low self-reported patient medication adherence was related to greater concerns regarding the potential adverse effects of medication, and a stronger belief that medicines in general are harmful.
BMQ in inflammatory bowel disease: Crohn‘s Disease (CD) and Ulcerative Colitis are typical example of chronic diseases where patient treatment requires a long-life medication. Lots of studies in literature measure the beliefs about medication of IBD patients using BMQ [45]. Dongen et al. [46] validated their own developed questionnaire, using the results of BMQ in order to measure the beliefs of IBD patients in treatment with enema. Another study [47] attempts to correlate non-adherence to 5-ASA therapy in UC patients, between BMQ findings and urine analysis. The obtained results yield serious suspicions about the efficiency of selfreport methods and report difficulties of accurately assessing medication compliance. Significant conclusions have drawn by Fu et al. [48] for attitude of adolescents patients who attended transition clinics. According to the study, transition patients have a stronger belief that medicine is necessary for their quality of life. In 2009, Horne et al. [49] presented an extensive study to assess patients’ attitudes to maintenance for IBD. This study reveals that the way in which patients judge their personal need for maintenance relative to their concerns about maintenance, can be a significant barrier to medication adherence.
BMQ in other chronic conditions: Some other chronic conditions have been investigated in the literature such as cardiovascular disease, mental disorder, heamophilia, hypertension and patients after stroke events. Viktil et al. [50] presents a study for patients from an outpatient clinic which suffers from chronic cardiovascular diseases. According their conclusion about the one-third of patients had strong concerns for their medication, although cardiac conditions present high mortality. Especially, in Psychiatric patient medication adherence plays significant role for the patient himself, as well as for his environment. Thus, several studies have been present in the literature, where the beliefs of patient about their medication have been analyzed [51-53].The study presented by Russel et al. [54] investigates the belief of patient about the necessity of antidepressants. The medication beliefs of patients with Haemophilia [55] and hypertension [56] have also been quantified by Llewellyn et al. [55] and Ross et al. [56] respectively. Finally, two other studies [57,58], assess the multidimensional effect of stroke-event and necessity beliefs on their medication adherence to stroke prevention medication.
The achievements of the Beliefs about Medicine Questionnaire have been approved due to the attempts for translations in several languages. Since the beliefs of peoples are strongly related to their culture, as well as the diverse variety of demographic, psychosocial, and economic factors, it was meaningful to investigate the behavior of the patients in different countries. The first translation presented by Beléndez et al. [24] in Spanish, where diabetic patients have been participated. Cuevas et al. [52] and Torderas et al. [31] revalidated the Spanish translation for Psychiatric disorders and Asthma treatment respectively. BMQ have been translated also in Arabic [30,61], Swedish [31], French [36], Japanese [27], German [28], Italian [29], Portuguese [59] and Czech [60]. Finally, Komninos et al. [26] presented a translation and adaptation in Greek language, in order to validate the BMQ it in primary patients in Greece. Table 5 shows a variety of studies, which employed translations of BMQ.
Work |
Disease | Language Translation |
| Alhalaiqa et al. 2014 [30] | Chronic Diseases | Arabic |
| Beléndez et al. 2007 [24] | Diabetes, Chronic Diseases | Spanish |
| Cuevas et al. 2011 [52] | Psychiatric Outpatients | Spanish |
| Marbdy et al. 2007 [31] | Pharmacy clients | Swedish |
| Fall et al. 2014 [38] | Diabetes type2, HIV | French |
| Komninos et al. 2012 [26] | Chronic Diseases | Greek |
| Lihara et al. 2010 [27] | Chronic (Liver, GI, Nervous system) | Japanese |
| Mahler et al. 2012 [28] | Chronic Diseases | German |
| Salgado et al. 2013 [59] | Chronic Diseases | Portuguese |
| Tibaldi et al. 2009 [29] | Chronic (cardiac, asthma, diabetes, depression) | Italian |
| Tordera et al. 2008 [33] | Asthma | Spanish |
| Matoulkova et al. 2013 [60] | Chronic (diabetes, hypertension, rheumatic disease) | Czech |
Table 5: Works with translated BMQ
According to the literature review, BMQ it is a useful tool mostly for chronic conditions, where long-time medication is needed. In such cases, the internal validity of the questionnaire presents high reliability, according to the Cronbach’s α. The number of studies per chronic condition, combined with the presented reliability, could be a simple indication of how valuable the questionnaire is, for each condition. Apart from the studies with mixed datasets, IBDs, Asthma and mental disorder have mostly been investigated. Specifically, in most of IBDs studies, beliefs groups have been extracted, presenting percentage values of subjects, which are categorized as accepting, skeptical, ambivalent and indifferent. Accessing these results a valuable conclusion could be the small number of skeptical patients. Focusing on the results for medication adherence (accepting patients), it seems that the nature of choric condition is not the only dominant factor, since the number of accepting patients varies among different populations.
Table 6 summarizes results presented in similar studies. As presented in the table 6, most researchers use Cronbach’s α as a reliability indicator, mainly assessing the internal validity of the BMQ subscales; the values for Necessity subscale range from 0.55 to 0.9, with average value of 0.77, while the values for the Concerns subscale range from 0.51 to 0.85, with 0.71 being the average value. The respective value for the Harm subscale ranges from 0.35 to 0.83, with 0.64 average value, and finally the value for the Overuse subscale ranges from 0.3 to 0.69, with 0.69 being the average value. It is clear that Necessity subscale presents the higher reliability, especially compared to Harm subscale; although these two subscales include the same number of items, there is a significant difference in their reliability.
Table 6: Results presented in similar studies
† calculated from Fig. 2 of [34], *P<0.0500, **P<0.0100, ***P<0.0050, ****P<0.0010, *****
Several researchers reported statistically significant correlation among patients’ age and at least one of the subscales, however it is not easy to draw a general conclusion since the majority of the presented works do not implicitly state findings related to significant or non-significant correlations with age. Furthermore, all values reveal moderate to weak correlations (for P<0.05), being in the range of [-0.29, 0.45] for Necessity and [-0.25, 0.23] for Concerns, while for Harm and Overuse subscales only one significant correlation has been reported for each, being 0.23 and 0.23, respectively. The same applies with the “number of medicines per day” variable; several researches reported statistical significant weak to moderate correlations among “number of medicines per day” variable and at least one of the subscales, being in the range of [0.06, 0.52] for Necessity and [0.20, 0.28] for Concerns, for Harm subscale only one researcher reported significant correlation, being 0.212, while no significant correlation with Overuse subscale has been reported.
Belief groups calculation based on BMQ General subscales is a procedure that is gaining strength as an analysis tool in recent studies. Belief groups analysis results reported from researchers are presented in figure 2. The reported results present a large variation in the percentages for all belief groups, with Accepting percentage being in the range of [16%, 67%], Ambivalent in the range of [21%, 42%], Indifferent in the range of [4%, 41%] and Skeptical in the range of [4%, 19%]. This could be partially explained from the differences among the medical conditions/disease of the patient population under study. However, even in studies for the same disease (there are 3 IBD related studies in figure 2), the differences are substantial.
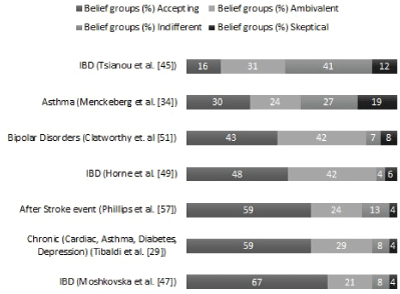
Figure 2: Belief Groups analysis results reported in the literature.
BMQ has been a valuable tool for measuring the beliefs about medicines of patients from various chronic conditions. Furthermore, several researchers have emphasized the strong correlation between patients’ beliefs about drugs and their medication adherence, thus (a) showing an easy and effective way to indirectly predict the medication adherence, and (b) providing an efficient method to improve the medication adherence by cultivating to the patients, positive beliefs about their medicines.
The authors declare that they have no conflict of interest.
This article does not contain any studies with human participants or animals performed by any of the authors.
Download Provisional PDF Here
Article Type: Research Article
Citation: Tsianou K, Giannakeas N, Tsipouras MG, Tzallas AT, Skamnelos A, et al. (2017) Accessing Patient Views about Medication in Chronic Conditions using the Beliefs about Medicine Questionnaire (BMQ): A Review Study. J Drug Res Dev 3(2): doi http://dx.doi.org/10.16966/2470-1009.130
Copyright: © 2017 Tsianou K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access