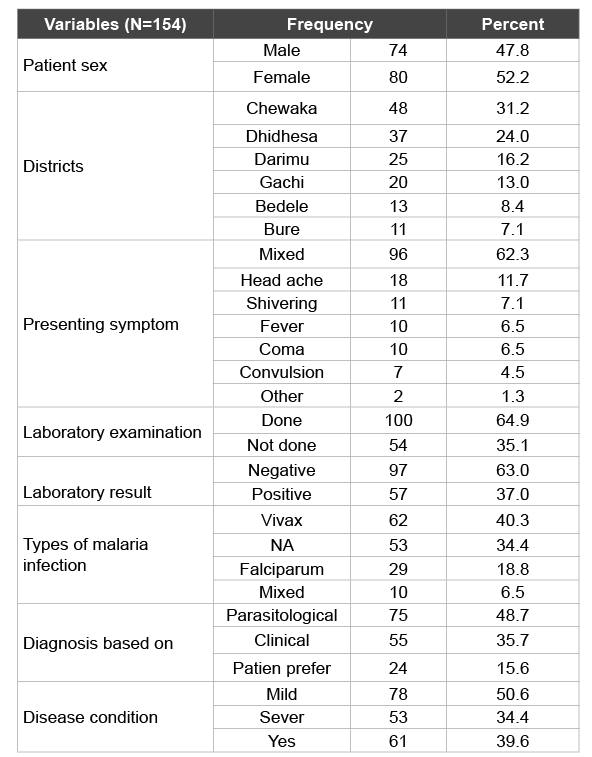
Table 1: Back ground information of study area districts of Ilu Aba Bora zone during study period

Walbek Asefa1 Sileshi Dubale2*
1Department of Bio-medical, Faculty of Health Sciences, Mettu University, Mettu Ethiopia*Corresponding author: Sileshi Dubale, Department of Pharmacy, Faculty of Health Sciences, Mettu University, Mettu Ethiopia, E-mail: sileshi.dubale@gmail.com
Background: Effective and safe drugs should be prescribed, dispensed and used rationally. In much of the tropics drug resistance to malaria is ever increasing. Then, malaria should be treated appropriately.
Objective: Evaluating the utilization pattern of anti-malarial drug in selected Ilu Aba Bora zone district, Oromiya region, south west Ethiopia.
Methods: Prospective cross-sectional study was conducted. Health care worker and Patient was selected using stratified random sampling technique in each malarious area of Ilu Ababor zone districts. Data was compiled and analyzed by using Statistical package for Social Sciences software (SPSS) version 16.0. The explanatory factors were calculated using multiple logistic regressions. The Odd ratio of anti-malarial drug miss utilization was calculated using total number of anti-malarial drug used as the denominator. Statistical significance was defined at a level of 0.05 and data was described with a confidence interval of 95%.
Results: The most prevalent type of malarial case was plasmodium vivax (40.3%), Artemeteren+Lumefantrine (Qoartem®) (42.9%) were the most prescribed for the patients. About 46.8% of prescription was prescribed out of national malarial treatment guide-line protocol. The most significant associated factors for anti-malarial miss utilization were educational level of the prescribers, profession of the dispensers, prescriber working experiences.
Conclusion: New anti-malaria drug on the market in Ethiopia, Qoartem® was exposed to miss utilization and it is the signal for development of drug resistance.
Malaria; Drugs; Use patterns; Health facilities
Malaria is an important cause of death especially in tropical countries. Malaria control requires an integrate approach, including prevention and prompt treatment with effective antimalarial drugs. The objective of treating uncomplicated malaria is to cure the infection as rapidly as possible. This prevents progression to severe disease, and additional morbidity associated with treatment failure. In treatment evaluations, it is necessary to follow patients for sufficient time to appropriately assess cures. The public health goal of treatment is to reduce transmission of the infection to others, i.e. to reduce the infectious reservoir and to prevent the emergence and spread of resistance to antimalarial medicines. The main determinant of antimalarial treatment policy is the therapeutic efficacy of the antimalarial medicines in use. Therapeutic efficacy monitoring involves the assessment of clinical and parasitological outcomes of treatment over at least 28 days following the start of adequate treatment to monitor for the reappearance of parasites in the blood. Reappearance of the same genotype indicates reduced parasite sensitivity to the treatment drug. Antimalarial treatment should be assessed on the basis of parasitological cure rates. The duration of post-treatment follow-up is based on the elimination half-life of the antimalarial medicine being evaluated. The current recommended duration of follow-up is a minimum of 28 days for all antimalarial medicines, while it is extended for longer periods of time depending on elimination half-life. When possible, blood or plasma levels of the antimalarial should also be measured in prospective assessments so that drug resistance can be distinguished from treatment failures due to inadequate drug exposure [1-3].
Malaria is a complex disease that varies widely in epidemiology and clinical manifestation in different parts of the world. This variability is the result of factors such as the species of malaria parasites that occur in a given area, their susceptibility to commonly used or available antimalarial drugs, the distribution and efficiency of mosquito vectors, climate and other environmental conditions and the behavior and level of acquired immunity of the exposed human populations In particular, young children, pregnant women, and non-immune visitors to malarious areas are at greatest risk of severe or fatal illness. Many malaria control strategies exist, but none are appropriate and affordable in all contexts. Malaria control and prevention efforts need to be designed for the specific environment in which they will be used and need to take into account the local epidemiology of malaria and the level of available resources and political will. The principal aim of drug utilization research is to facilitate the rational use of drugs in populations. It can be used in the application of quality indicators to patterns. This general indicator can be applied at different levels (e.g. individual prescriber, group of prescribers, hospitals, and region or county) to obtain a rough estimate of the quality of prescribing dispensing and community utilization [4,5].
The limited information available on drug use throughout the world indicated that drugs are not optimally used which leads to in appropriate use. This inappropriate use has serious patient harm and economic consequences for individuals, community and for the success of national health care system. Rational prescription pattern and providing correct information during dispensing is inviolable for proper utilization of drugs. In much of tropics, drug resistance malaria is increasing in distribution, frequency and intensity. There is a growing belief among scientists that, to prevent resistance, malaria, should be treated with drug combination. Hence, in-expensive, safe drugs and ultimately vaccines are needed to combat malaria [6-8].
Approximately 52 million people (68%) live in malaria risk areas in Ethiopia, primarily at altitudes below 2,000 meters. Malaria is mainly seasonal with unstable transmission in the highland fringe areas and of relatively longer transmission duration in lowland areas, river basins and valleys. Historically, there have been an estimated 10 million clinical malaria cases annually. Since 2006, however, cases have reduced substantially. Ethiopia is also one of the most malaria epidemic-prone countries in Africa. Rates of morbidity and mortality increase dramatically (i.e. 3-5 fold) during epidemics. Since 2005, Ethiopia has scaled-up one of the largest and most ambitious malaria control programs in Africa, designed to support the country’s Health Sector Development Plan (HSDP), Ensuring prompt and effective treatment will prevent most cases of uncomplicated malaria from progressing to severe and fatal illness. To avoid this progression, treatment must begin as soon as possible, generally within 24 hours after symptom onset. Effective malaria treatment requires improved diagnosis of malaria, well-trained health workers in both the public and private health sectors; and, constant availability of highly efficacious medicines as close to the patient as possible to ensure prompt access. Communities should be aware of the importance of seeking early diagnosis and treatment and adhering to prescribed drug regimens for malaria. Best practices in malaria control require the regular updating of malaria treatment guidelines and their dissemination to all tiers of the health care delivery system and a sound monitoring and supervision system [7-10].
Despite the different efforts to increase public awareness regarding use of anti-malarial drugs there is still irrational prescribing, dispensing, and use the drug. If drug-use pattern of anti-malarias is not monitored, there is possibility of early emergence of resistance to the highly effective antimalarial drugs presently in use. Therefore appropriate drug utilization studies are important tools to evaluate whether drugs are properly utilized at all levels in the chain of drug use. Then the primary purpose of this study was to assess ant-malarial drug utilization patterns and factors affecting rational drug use in malarious areas of Ilu Aba Bor districts, South West Ethiopia.
Study was conducted in malarious area of, Illu Aba Bora Zone, Oromiya Region, and South West Ethiopia at health facility level.
A cross-sectional prospective study was conducted to assess antimalarial drug prescription practices at health facility level.
Data collection instrument format that comprises patient information such as, age, Weight, malaria type, and drug data like dose, frequency, and duration of administration was used to collect data.
To evaluate the data collection instrument for its validity, reliabilities and consistency a pilot study was done on 5% of study. Training was given for data collectors and the data collected was checked for the completeness, accuracy, by the principal investigator every day and correction was made soon if any fault done.
All the data was entered, compiled and analyzed by using version 16.0 statistical software packages. Frequencies of descriptive statists were presented by using percentages and table. Logistic regression analysis was performed to assess the relation of each cause of drug miss use. The explanatory factors included patient factors health facility or health professionals related factors was calculated using multiple logistic regression. Statistical significance was defined at a level of 0.05 and data was described with a confidence interval of 95%.
Letter was written by University research review board to Zonal health department and to each malarious area districts and community willingness also asked.
Totally, 154 antimalarial drug treatments were observed. From these 52.2% (80) of them were Female and 47.8% (74) of them were male. The drug utilization was observed in six Ilu Ababor Zone Districts. Chewaka were the most district among high prevalence malarial infection observed 31.2% (40). Dhidhesa 24.0% (37) and Darimu16.2% (25) was the second and the third districts among malaria case observed. About 62.3% (96) of Malaria cases were presented with mixed sign and symptoms and the other cases were mostly presented with head ache 11.7% (18) and shivering 7.1% (11). From cases visited health facilities for malarial treatment, for 64.9% (100) of them, laboratory examination was done and 63.0% (97) of the result were negative. From 37.0% (57) positive results, the most prevalent type of malarial case was plasmodium vivax 40.3% (62). Among patients visited the health facilities 14.9% (23) were presented with complicated disease condition and 39.6% (61) cases were re-visited the health facilities within 4th and 14th days with similar cases. 35.75% (55) of the diagnosis were based on clinical and 15.6% (24) based on patient report and prefer and the rest 48% (75) were based on parasitological diagnosis (Table 1).

Table 1: Back ground information of study area districts of Ilu Aba Bora zone during study period
Regarding the drugs prescribed for the patients visited the health facilities during the study period, Artemeteren+Lumefantrine (Qoartem® ) 42.9% (66) were the most drug prescribed drug for patients. Chiloroquine 40.9% (63) and Quinine 8.3% (13) was the second and the third drugs prescribed for the patients respectively (Figure 1).
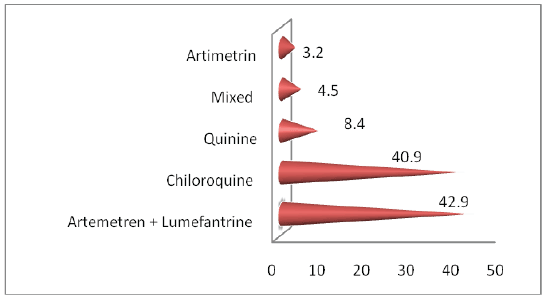
Figure 1: Types of anti-malarial drug prescribed for patients in malarious area of Ilu Aba Bora zone districts during study periods
Table 2 showed that, the patterns of prescribing practices of anti-malaria drugs in Ilu Aba Bor malaria districts. According to this table, from all prescriptions, for most of patients patient name 89% (137), patient age 82.5% (127) drug frequency 84.4% (130) were written on the prescription paper. For most of patients 88.3% (136) the patient weight were not written on the prescription paper. From 90.3% (139) of the drug dose written on the prescription paper, only 58.4% (90) of the drug dose were normal. But 70.8% (109) of frequency written on the prescription paper were correct. From the total prescribed drugs, only for 32.5% (50) patients the first dose was given at health facility level. Regarding the overall prescribing practice, about 46.8% (72) prescriptions were prescribed out of national malarial treatment guide-line protocol (Table 2).

Table 2: Patterns of prescribing practice of anti-malarial drug in selected malarious area of Ilu Aba Bora Districts during study periods
Regarding additional supportive practices of prescribers besides prescribing of antimalarial drugs, for 80.5% (124) of patient’s additional drugs were prescribed. 38.3% (57) of them were anti-pain, antibiotics 21.4% (33) and anti-fever 14% (22) were the second and the third categories of additional drugs prescribed together with anti-malarial drugs respectively. But for 19.5% (30) of the patients only anti-malarial drugs were prescribed. The advices given together with prescribing of the drugs also listed in table 3.
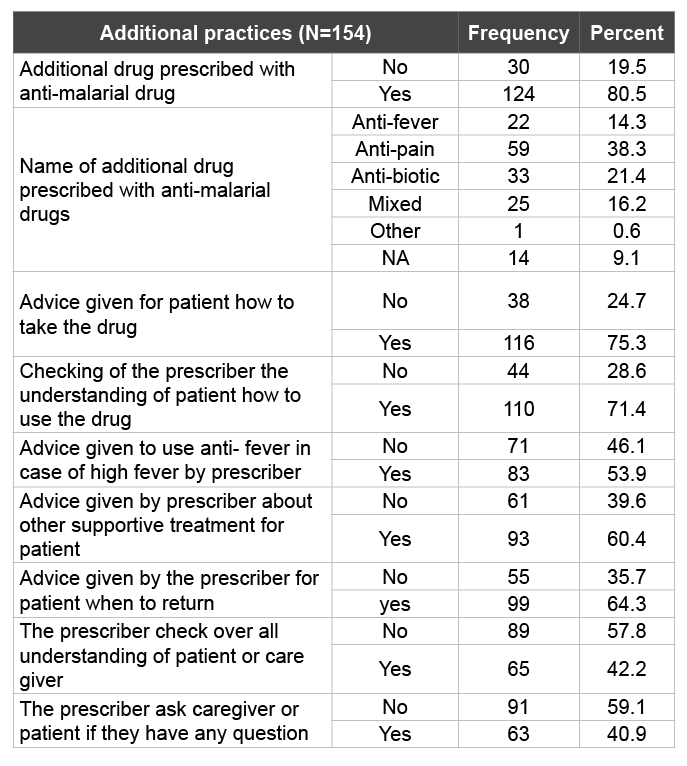
Table 3: Additional practices rather than prescribing anti-malarial drugs to support malarial treatment in selected malarious area of Ilu Aba Bora Districts during study periods
From cumulative over all utilization of anti-malarial drugs, 44.8% (69) were irrationally or incorrectly used, the left were correctly used (Figure 2).
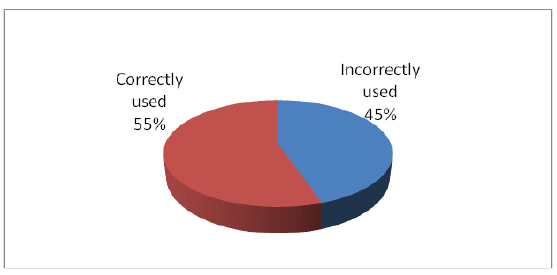
Figure 2: The cumulative over all utilization of the drug among the prescribers and patent/care giver (community level) in selected malarious area of Ilu Aba Bora Districts during study
The most significant associated factors for anti-malarial miss utilization in Ilu Aba Bora six malaria districts were educational level of the prescribers, profession of the dispensers, prescriber working experiences and status of the health facilities. Health facility level, profession of the prescribers also contributed for miss utilization of anti-malaria drugs. But sites of health facilities whether it is in Rural or Urban did not have such significant on drug utilization during the study period. For each patients or care givers the outcomes were whether the drug was prescribed according to national anti-malarial drug treatment guide line or not. Educational level of the prescribers (p-values=0.002), profession of the dispensers (p-value=0.0001), prescribers working experience (p-value=0.0001) and the status of the health facilities (p-value=0.016) were highly associated with anti-malarial drug miss-utilization in Ilu Aba Bor during study period.
The odds of anti-malarial drug prescribed by health profession having only certificate caused drug miss-use 8.52(95% CI 2.26-32.13) times than anti-malarial drugs prescribed by health profession having first degree and above. Anti-malarial drugs dispensed by other health professionals other than pharmacists exposed to miss-utilization 10(95% CI 4.46-13.36) times than anti-malarial drugs dispensed by pharmacists. The odds of drug prescribed by health professionals having working experience less than two years caused 5.18(95% CI 2.28-11.73) times than drug prescribed health professionals having greater than five years. The odds of the drug prescribed at health posts were exposed to miss-utilization 2.31(95% CI 1.025-5.77) times than anti-malarial drug prescribed at health center and drug prescribed in newer health facilities exposed to miss utilization 2.52(95% CI 1.31-4.85) times drug prescribed in older health centers. Finally since the above mentioned odd ratios did not cross number one it revealed the association was very strong (Table 4).
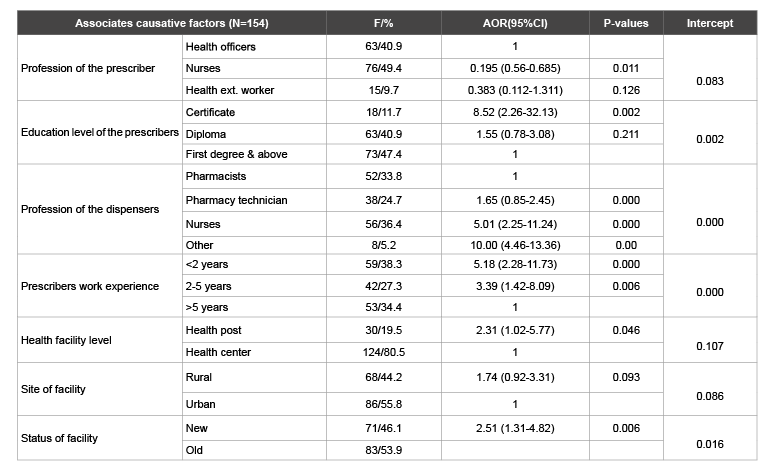
Table 4: Factors affecting antimalarial drug utilization in selected malarious area of Ilu Aba Bora Districts during study
The primary limitation of our study was that the assessment mainly focused only prescription practice and patient interview but no other components of drug utilization like dispensing and drug storage and supply chain management. This may not be used to describe quality indicator. The other limitation was lack of long time follow up to compare and contrasts the outcomes of miss utilization when compared with correctly utilized drug.
Totally 154 anti-malarial drug treatment were observed in six Ilu Aba Bor Zone Districts. Among patients visited the health facilities 14.9% were presented with complicated disease condition and, according to Drug Utilization Study of Anti-Malarial Drugs in Indian Tertiary Care Hospital, 24.26% were complicated case this difference may be due to difference in health facility difference. In India the study were conducted in tertiary Hospital but in our case the study were in the health centers and health posts.
From cases visited health facilities for malarial treatment, for 64.9% of them, laboratory examination was done and 63.0% of the result was negative. During the study period, whether laboratory diagnosis was done or not done, or whether the result was negative or positive for all cases the anti-malarial drug were prescribed this is out of national and international anti-malarial drug treatment guideline, according to the guidelines before prescribing of anti-malarial drug diagnosis should be confirmed and other acute febrile illnesses should be ruled out, un less otherwise the drugs are prone to develop resistance [1,9].
From 37% of positive results, the most prevalent type of malarial case was plasmodium vivax 40.3%. This is quietly different from Indian study. According to Dhara M. Limbachia and his collogues study [5], most of the causative parasite species were Plasmodium falciparum (39.22%), this difference may be due to Geographic and/or epidemiological difference of the two countries [3].
Drugs prescribed for the patients visited the health facilities during the study period, Artemeteren+Lumefantrine (Qoartem®) (42.9%) were the most drug prescribed for the patients. In Indian tertiary Hospital study during 2012 showed that, Artemisinin Combination Therapy was prescribed for 7.96% patients. Artesunate mono therapy was prescribed in 41.59% patients. This difference was may be difference due to the difference in treatment guideline and or resistance strain patterns of the plasmodium species [1,5]. This study was similar with the study conducted by Appolinary AR Kamuhabwa and his Collogues [11] on Knowledge among drug dispensers and antimalarial drug prescribing practices in public health facilities in Dar es Salaam during the year according to this study, 87% of all prescriptions contained artemether-lumefantrine as the only antimalarial drug.
From 90.3% of the drug dose written on the prescription paper, only 58.4% of the drug doses were normal. This is in line with Dhara M. Limbachia et al. [5] drug utilization study. From the total prescribed drugs, only for 32.5 % patients the first dose were given at health facility level and about 46.8 % prescription were prescribed out of Ethiopian national malarial treatment guide-line protocol and current malarial case management protocols [3,9].
Regarding additional supportive practices of prescribers besides prescribing of antimalarial drugs, for 80.5% of patients additional drugs were prescribed, 38.3% of them were anti-pain, antibiotics 21.4% and antifever 14% were the second and the third categories of additional drugs prescribed together with anti-malarial drugs respectively. This additional therapy was very low according to WHO and national antimalarial drugs guidelines. According to 2010 WHO and 2012 Ethiopian National antimalarial guide line, since fever is a cardinal feature of malaria, and is associated with constitutional symptoms of lassitude, weakness, headache, anorexia and often nausea. Antipyretics should be used if core temperatures >38.5°C Paracetamol and Ibuprofen should be used successfully as an alternative in malaria. Since vomiting also common, in acute malaria and may be severe, antiemetic should be used but there have been no studies of their efficacy in patients with malaria, and no comparisons between different antiemetic compounds [1,3]. But this study was almost similar with the study conducted on Knowledge among drug dispensers and antimalarial drug prescribing practices in public health facilities in Dares Salaam during the year 2013. According to this study, 77.1% contained at least one analgesic, and 26.9% contained at least one antibiotic, indicating unnecessary use of analgesics and antibiotics with antimalarial drugs in public health facilities [11-15].
This study revealed that there were high rate of inappropriate use of anti-malarial drugs. There was the trained of prescribing anti-malarial drug even if there is laboratory examination result were negative. New anti-malaria drug in the in Ethiopia market, Artemeteren+Lumefantrine (Qoartem) was exposed to miss utilization. This indicated that if there is no action is taken to stop this miss utilization, it is the signal of future for development of drug resistance.
Some of patients and/or care givers collected their drug from health facilities did not understand how to use their medication at home. Hence the causes of anti-malarial irrational use were multi factorial both at patient and professional sides. These phenomena was also one dangerous sign for development of anti-malarial drug resistant in the study areas, un less otherwise the preventive mechanism employed to minimize drug miss utilization.
The most significant associated factors for anti-malarial miss utilization were educational level of the prescribers, profession of the dispensers, prescriber of working experiences and status of the health facilities. Then, Intervention should employed by focusing on these main causative areas.
All health facilities at malarious areas of Ilu Aba Bora Zones should assign experienced health professionals to anti-malarial drug prescription practices.
All health centers should employ pharmacists and /or pharmacy technicians for dispensing of drugs and performing of others pharmaceutical managements.
Zonal health office or Regional health Bureau should distribute updated standard treatment guidelines for each health facilities.
Regional Health Bureau and Federal ministry of health should give in service training for health professionals on anti-malarial drug treatment regularly.
Federal ministry of health should distribute material and laboratory chemicals needed for malarial diagnoses and treatment by giving special focuses to malarious areas.
Further advanced studies should be done on anti-malarial drug utilization and on patterns of drug resistance.
The authors declare that they have no competing interests
Download Provisional PDF Here
Article Type: Research Article
Citation: Asefa W, Dubale S (2016) Anti Malaria Drug Utilization Pattern in Selected Malarious Areas of Ilu Aba Bora Zone Health Facilities, Oromiya Regional State, South West Ethiopia. J Drug Res Dev 2(2): doi http://dx.doi.org/10.16966/2470-1009.114
Copyright:© 2016 Asefa W, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access