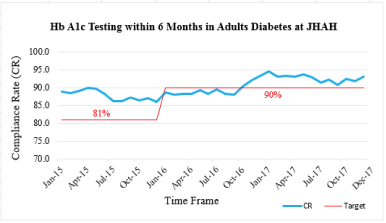
Figure 1: (HbA1c testing within 6 months) Run chart illustrates a quality improvement in process measure performance against the target during the last 3 years at JHAH.


Huda H Al Sayed Ahmed1* Saeed Yami1 Ameera Al Eid1 Sahar Ashraf1 Wala Muslem1 Jalal Al Alwan1 Kanaani Kanaan2 Sarhan Ahlam3
1Department of Quality and Patient Safety, Johns Hopkins Aramco Healthcare (JHAH), Saudi Arabia*Corresponding author: Huda H Al Sayed Ahmed, PhD, CHQO, Department of Quality and Patient Safety/Healthcare Quality Analytics Division, Johns Hopkins Aramco Healthcare (JHAH), Saudi Arabia, E-mail: huda.alsayedahmed@jhah.com
Introduction: Diabetes Mellitus (DM) is a complex health problem. That there is an ongoing increase pattern of DM with a ten-fold in the past three eras in Saudi Arabia. Reducing this rate, through assessing the quality of diabetes care, standardized and effective Quality Improvement (QI) performance measures are highly needed. Johns Hopkins Aramco Healthcare; JHAH revisits QI process yearly evaluating clinical needs on the key processes. It constructs a strategic plan that guarantees the desired patient outcomes and thus satisfaction. Herein, we want to describe the “Diabetes QI Practice and Performance; DQIPP” in JHAH, to share experience and quality of healthcare performance.
Material and Methods: An approximate average of 15000 diabetes seen yearly in JHAH collected from Diabetic registry during the last 3 years. HbA1c testing within 6 months used as a process Key Performance Indicator (KPI), whereas “HbA1c ≥ 9.0%” used for poorly controlled diabetes as an outcome KPI.
Results: Data analysis showed a significant improvement in compliance rate of both KPI measures against the set targets within JHAH, with a p value of ˂0.05.
Conclusions: Working as collaborative healthcare providers to improve care management, control of diabetes and prevent the devastating complications via targeting the high-risk groups. This can impressively expand the efficiency of QI interventions and achieve a better healthcare.
Diabetes mellitus; Diabetes quality improvement practice and performance; HbA1c; Key performance indicator
Diabetes Mellitus (DM) is a global complex health problem. It is a group of metabolic disorders which result in hyperglycemia over an extended period of time [1]. DM is caused by pancreatic islets β-cells defect that subsequently result in reduction of insulin secretion, insulin action, or both [2,3]. DM symptoms include polyuria, polydipsia, and polyphagia in the advanced cases, this concur with weight loss, and blurry vision. The abiding long-lasting complications of DM might enclose retinopathy with potential blindness, nephropathy that drives to renal failure, peripheral neuropathy which jeopardy foot ulcers or amputations [2,3]. In addition to gastrointestinal, genitourinary, and cardiovascular malfunction or dysfunction. DM is often accompanied by Hypertension and defective lipoprotein metabolism as well [3]. All of which lead unfortunately to noteworthy morbidity/mortality, reduced quality of life, thereafter the cost and the health care resource utilization [2,4]. Fortunately, massive study researches have clearly established numerous effective treatment protocols and quality performance practices that can extensively reduce or even prevent this burden [4]. There are three major types of DM, with two broad categories. Type 1 DM referred to as “Insulin-Dependent Diabetes Mellitus” (IDDM). Type 2 DM accounts for about 90-95% of all cases and known as “Non-Insulin Dependent Diabetes Mellitus” (NIDDM). The third type is Gestational Diabetes mellitus (GDM) that occurs when non-diabetic pregnant women develop Hyperglycemia that resolves after delivery [2,3].
Indeed, Kingdom of Saudi Arabia (KSA) is the second highest DM ranking in the Middle East, and is the seventh at a world level, as reported in 2015 by the World Health Organization (WHO). It is estimated that there is an ongoing proliferation pattern of DM with a ten-fold increase in the past three eras in KSA [5]. A Ministry of Health report published in 2017 expected that the cases will exceed 3 folds by 2030 worldwide [6]. These findings go with the 2015 report of the International Diabetes Federation (IDF) [7]. Nevertheless, the maximal prevalence of DM overall occur in the Middle East and North Africa where the economic development is really rapid [6]. Actually, most diabetes is obese which by itself causes some degree of insulin resistance. Obesity is the major risk factor associated with increasing the DM prevalence in KSA [8]. Alongside the regional barriers to modify or interfere to enhance active and healthy lifestyles in order to limit the obesity phenomena, this risk factor together with other DM complications are potentially preventable and subsequently promoting wellbeing is ultimately warranted [8,9].
DM is being an important target for quality improvement as the care of the poorly controlled diabetes is costly. This is frequently indicated by numerous governmental and quality agencies such as AHRQ; Agency for Healthcare Research and Quality [8]. All the quality improvement efforts and strategies attempt to shrink the gap between current health care processes or outcomes and those built on evidence-based practice [10]. With anticipated DM high incidence rate worldwide, healthcare enterprise works hard in magnifying the efficiency of DM medical care via influencing patient behavior and lifestyle setting [10]. Obviously, selecting a quality control standard requires social commitment to implement [11]. Both inappropriate health care and/or poor control would possibly result in serious complications and thus precocious mortality [2].
The Quality Improvement (QI) targets should serve the “triple aim” of better care for better health with a lower cost in DM. These targets could include an organizational structure change of the healthcare team through using multidisciplinary professionals [12]. Important success factors to accomplish this goal exist in a cooperative teamwork as stated by Peterson A, et al. [13] in their case study. Another important quality target is at patient’s level that is basically through improving diabetes education programs [12]. Within endocrinology, most of the assigned “diabetic care quality improvement measurements” have focused mainly on process and outcomes measures [14].
A common process QI metric for diabetes is meeting glycated hemoglobin (HbA1c) acceptable threshold [12]. The American College of Physicians (ACP) published a set of guidelines that support the goal of controlling HbA1c for type 2 DM patients [11]. The clinicians should reassess HbA1c level and the treatment protocol based on benefits and harms equipoise [15]. Undoubtedly, prescribing an intensive and expensive pharmaceutical treatment for diabetic patients with elevated HbA1c level may not be profitable for governmental sectors or desired by the patient [11]. However, improving the quality of care is best accomplished by aiming on the high-risk DM subgroups with HbA1c ≥ 9.0% as apriority for QI resources, especially for type 2 diabetes and else presence of other co-morbidity factors [11,15].
Researches showed that despite the decline in HbA1c as a QI target measure, a considerable volume of patients do not meet the target for other measures like BP, LDL Cholesterol and non-smoking status [16]. Therefore, diabetes care and management should not be optimal to glycemic control. It should extend beyond that to imply observing the adherence to preventive care procedures and screening for early complications [12,16]. Not only that, a modification of the patient’s life style is valid quality targets that enlighten the efficiency of quality improvement programs. Research studies have reported the effect of physical exercises, following healthy diet and not smoking on improving Quality of Life (QoL) in diabetic patients. Keerthi GS, et al. [17] study concluded that “Yoga Therapy” along with diabetes standard treatment significantly improved QoL scale compared to standard treatment alone. It is also important to recognize the depression as a risk co-factor for not adhering to medical advises and hence medical noncompliance and poorer outcome. A research evidence of strong association is suggested by DiMatteo MR, et al. [18] study, in comparison with non-depressed patients with an odds ratio of 3 times. Another example is shown in Ojo O, et al. [19] review study, he illustrated that a diet with Low-Glycemic Index (LGI) lead to a significant improvement (p <0.05) in HbA1c level related with a Higher Glycemic Index (HGI) diet in type 2 diabetes [19].
Taking into consideration that poorly controlled diabetics account for the majority of retinopathy; blindness, cardiovascular disease and End-Stage of Renal Disease (ESRD) [11]. Several systematic reviews analyzed the impact of effective education, self-management training, emotional support, coping strategies, and appropriate interventions which help patients and their families to better understand diabetes [10]. The current guidelines desire for a tighter control that requires a continuous education and actively communicating this to health care providers and patients. A “physician-driven quality improvement” program has been incorporated into the National Diabetes Quality Improvement Alliance (NDQIA), which includes diabetes caring organizations in the US [20]. Certainly, to assess the quality of diabetes care, standardized performance measures are highly needed. The American Diabetes Association; ADA has developed a set of “Diabetes Quality Improvement Program Measures” that has approved to be utilized in the “Healthcare Effectiveness Data and Information Set” (HEDIS). These measures were thereafter been accepted for assessment of quality performance Medicare and Medicaid healthcare plans. Moreover, the ADA clinical practice recommendations are intended to provide the proper care, treatment guidelines and tools for quality care evaluation [16-23].
Our healthcare center at (Johns Hopkins Aramco Healthcare; JHAH-KSA) is a tertiary healthcare system, where organizational learning and continuous improvement is the culture, as it strives to provide a climate of patient safety. JHAH constructs a strategic plan that guarantees the desired patient outcomes and thus satisfaction, with full consideration to organizational efficiency. In this article, we intended to describe the “Diabetes Quality Improvement Practice and Performance (DQIPP)” in our institute. In addition, we pursue to benchmark the quality of our medical practice’s performance, share our experience, Excellency and successful stories from QI point of view.
An Ethical approval was obtained from the Institutional Review Board at John Hopkins Aramco Healthcare Center (JHAH) before proceeding the project.
The Professional Practice Committee (PPC) at JHAH is responsible for ensuring the medical care in diabetes that is the standard of care. It is a multidisciplinary expert team comprised of internist physician, diabetes educator, endocrine case manager and qualified dietitian. The main role of the PPC is to follow the updated ADA quality measures to guarantee the best of care for diabetic patients in term of treatment and control (Table 1) [21,24,25]. In JHAH, all the prediabetes cases are referred to the diabetes educator who will instruct them of how to monitor their Glucose level, Blood Pressure (BP) and Body Mass Index (BMI) within normal ranges. The diabetes educator in collaboration with dietitian will also assess the diabetic patients to retain their ideal HbA1c at < 7% (53 mmol/L), teach them on correct using of glucometer, adjusting insulin dose if needed and order them to test for HbA1c every 6 months (or at least twice a year). The poorly controlled diabetes, whom HbA1c ≥ 9.0% (75 mmol/L), they are monitored to do the laboratory tests including HbA1c (quarterly), LDL-Cholesterol, kidney function test (i.e. renal panel including serum creatinine, creatinine clearance, Blood Urea Nitrogen (BUN), Glomerular Filtration Rate (GFR) and liver function test (i.e. hepatic panel including liver enzymes , albumin and bilirubin). In addition, they will be assessed by a case manager who will closely monitor their Fasting Blood Sugar (FBS), 2 hours Postprandial Blood Sugar (2h PP), BMI and other co-morbidity cofactors.
| QI Measures | Recommended Value |
| Glycated Hemoglobin (HbA1c) | <7.0% (53 mmol/mol) |
| Pre-prandial Capillary Plasma Glucose | 80-130 mg/dL (4.4-7.2 mmol/L) |
| 2 Hours Postprandial Glucose (2h PP) | <180 mg/dL (10.0 mmol/L) |
| Blood Pressure (BP) | <140/90 mmHg |
| LDL Cholesterol (LDL-C) | <70 mg/dL |
Table 1: ADA Glycemic recommendations for “non-pregnant” Diabetes adults [42].
Nevertheless, diabetes patients are subjected to annual foot and eye examination as a control measure. Optimizing of lifestyle and self-management education is a fundamental aspect in diabetes care. Promoting body exercise/physical activity, heart healthy diet, and smoking cessation counseling are routine components of the diabetes medical care plan in JHAH. Moreover, Aspirin is recommended as a secondary prevention for those with a history of atherosclerotic cardiovascular disease or for those ≥ 45 years old with at least one additional major risk factor. Chronic pediatric diabetics are extensively assessed through pediatric clinicians; same is for gestational diabetics who will be exposed to a comprehensive obstetrician control plan.
Herein, we intended to share our Diabetes Quality Improvement Practice and Performance (DQIPP) in our institute. JHAH is using “HbA1c is testing within 6 months” as a process measure since 2015 [26-29]. Whereas “HbA1c test of ≥ 9.0%” for poorly controlled adult diabetes is used as an outcome measure since April 2016. We collected the data from diabetes registry in SAP system (electronically generated) during the last 3 years. We define the “HbA1c testing within 6 months” measure as the percentage of diabetic patients having a face to face visit in primary care, endocrinology or diabetic teaching center during a reported month that have a documented HbA1c test on the of the encounter or within the previous 6 months [24]. At least 90% of patients have to do HbA1c lab test within 6 months, and the equation used is as follows:
\[\frac{{Number\,of\,Diabetic\,patients\,with\,HbAc\,test\,done\,(within\,the\,last\,months)}}{{Total\,Number\,of\,Diabetic\,patients\,with\,the\,last\,encounter\,visit\,during\,a\,month}}\]
Meanwhile, the definition of the outcome measure “HbA1c test of ≥ 9.0%” for poorly controlled adult diabetes is the percentage of adult diabetic patients (aged 18 to 75 years) with Type 1 or 2, who had an appointment within the last 2 years and with latest HbA1c test of ≥ 9.0%. If the diabetes quality improvement program is performing well, then patients with HbA1c test of ≥ 9.0% should not exceed 20% of all registered diabetes at the same period. The equation used is as follows:
\[\frac{{Number\,of\,eligible\,Diabetic\,patients\,with\,HbA1c \ge 9.0\% }}{{Total\,Number\,of\,adult\,Diabetic\,patients\,that\,had\,a\,provider\,visit\,within\,the\,last\,years}}\]
SPSS software v.20 (IBM Corp., Armonk, NY, USA) was used to perform the required statistical analysis. Data analysis revealed that around 15000 diabetic cases is seen in JHAH facility yearly. The demographic characteristic of the Diabetic patients are summarized in Table 2.
| Age | % |
| (˂18 years) | 1.6 |
| ( ≥ 18 to 75 years) | 98.4 |
| Sex | % |
| Male | 52.4 |
| Female | 47.6 |
| DM Type | % |
| DM Type 1 | 4.0 |
| DM Type 2 | 95.4 |
| DM (Other) | 0.6 |
| Nationality | % |
| Saudi Nationality | 84.9 |
| Other Nationalities | 15.1 |
Table 2: Demographic Characteristics of the Diabetic cases in Saudi Population at JHAH during the period 2015 to 2017.
Analyzing the performance of quality improvement practice at JHAH throughout the last 3 years showed that a gradual improvement in both the process and the outcome QI established measures. “HbA1c test to be performed within 6 months or twice a year” Key Performance Indicator (KPI) illustrated a significant improvement in compliance rate from 87.8% in 2015 to 89.3% in 2016 and up to 92.7% in 2017 against a predetermined target value of ≥ 81%, ≥ 90%, ≥ 90% in 2015, 2016 and 2017 respectively, with a p value of 0.000052 (Figure 1).

Figure 1: (HbA1c testing within 6 months) Run chart illustrates a quality improvement in process measure performance against the target during the last 3 years at JHAH.
At the same time, “HbA1c test of ≥ 9.0%” key performance indicator (KPI) for poorly controlled adult diabetes, including 18 to 75 years old diabetic patients, literally demonstrated an improvement since being implemented to service. The pre-decided target is to have not more than a 20.3% of poorly controlled diabetic patients, and the data analysis confirmed a significant improvement in the service quality since established on April 2016 with compliance rate of 20.5% to 19.2% end of 2017, with a p value of 0.000 (4.5E-61) (Figure 2).
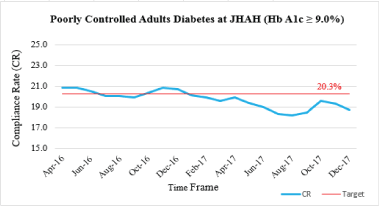
Figure 2: (HbA1c test of ≥ 9.0%) Run chart illustrates a quality improvement outcome measure performance against the target during the last 2 years at JHAH.
In our study, the data are collected from “Diabetes Registry” JHAH data base for the last 2-3 years, since the implementation of diabetes QI measures. “HbA1c testing within the previous 6 months” used as process key performance indicator (KPI), whereas “HbA1c ≥ 9.0% for poorly controlled diabetes” as outcome KPI. A statistical analysis of t-test showed a significant improvement in the Compliance Rate (CR) of both KPI measures against the set targets in our JHAH organization, with a p value of <0.0001. The CR of HbA1c testing within 6 months illustrated improvement against the target value. About 88% of diabetic patients were compliant in 2015 against the target of 81%. In 2016 the target was elevated to 90%, where the CR of our data were almost 89% in 2016 and about 93% in 2017, that reflects the significant improvement in compliance rate. Although more efforts has to be implemented to reach the bench mark (93.5% as of NCQA). As well, the CR of HbA1c ≥ 9.0% for poorly controlled diabetes revealed adherence to improvement versus the target value of about 20%. The analysis showed approximately 20% of our diabetic patient was compliant in 2016 and the proportion was significantly reduced to almost 19%. Fortunately, our performance for this outcome measure is better than the bench mark (27.3% as of NCQA).
Of course, reliance of the glycated hemoglobin (HbA1c) independently to assess the quality of diabetes care is a limitation fence. However, Johns Hopkins Aramco Healthcare selected HbA1c as an organizational KPI; meanwhile it utilizes several other ADA process and outcome measures in monitoring Diabetes healthcare management and control at the primary care unit level.
This article highlights the importance of updating the knowledge and developing the skills of all healthcare professional enrolled in the diabetes care management in order to provide a higher quality of patients care. More effective quality improvement initiatives will help with understanding the nature of the quality problem once having in mind the horrible increased incidence of DM in Saudi Arabia [30-39]. However, governmental support is extremely needed and further development is required to assess Diabetes Quality Program Performance (DQPP) and self-management programs in Saudi Arabia. Throughout this study, we enlightened the potential roles of QI and the effectiveness of QI strategies in diabetes care program. This was emphasized via applying primary prevention and control protocols for diabetic patients more widely [40-42].
Hosting quality improvement measures into healthcare system in Saudi Arabia is definitely of high prominence. Though, interdisciplinary strategies improve management and control of diabetes and prevent devastating complications. This can impressively expand the efficiency of QI interventions and achieve a better healthcare. Nevertheless, mapping the future; achieving better care will lead to better health that will eventually bend the ever‐growing cost curve.
The opinions expressed in this article are those of the author and not necessarily represent the view of Johns Hopkins Aramco Healthcare. I would like to thank my colleagues in Healthcare Quality analytics division, as well as Ms. Zainab Abbas from primary care Division who provided me with the needed assistance and support.
Download Provisional PDF Here
Article Type: RESEARCH ARTICLE
Citation: Ahmed HHAS, Yami S, Al Eid A, Ashrafi S, Muslem W, et al. (2018) Improvement in the Glycated Hemoglobin for Diabetic Patients as a Quality Care Adherence at Johns Hopkins Aramco Healthcare in Saudi Arabia. J Diab Res Ther 4(1): dx.doi.org/10.16966/2380-5544.138
Copyright: © 2018 Ahmed HHAS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access